Abstract
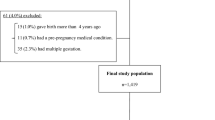
Background Inadequate maternal nutrition is regarded as one of the most important indicators of fetal growth. The aim of this study was to analyze the associated risk of having a small for gestational age (SGA) infant according to the mother’s dairy intake during the first half of pregnancy. Methods A prospective cohort study was performed using 1175 healthy pregnant women selected from the catchment area of Virgen de las Nieves University Hospital, Granada (Spain). SGA was defined as neonates weighing less than the 10th percentile, adjusted for gestational age. Factors associated with SGA were analyzed using logistic regression models. Population attributable fractions of SGA according to dairy intake were estimated. Results Dairy intake among women who gave birth to SGA infants was 513.9, versus 590.3 g/day for women with appropriate size for gestational age infants (P = 0.003). An increased intake of dairy products by 100 g/day during the first half of pregnancy decreased the risk of having a SGA infant by 11.0 %, aOR = 0.89 (0.83, 0.96). A dose–response gradient between dairy intake and SGA was observed. Conclusions An inadequate intake of dairy products is associated with a higher risk of SGA. Our results suggest a possible causal relation between dairy intake during pregnancy and the weight of the newborn, although we cannot discard residual confounding. These results should be further supported by properly designed studies.

Similar content being viewed by others
Abbreviations
- SGA:
-
Small for gestational age
- LGA:
-
Large for gestational age
- AGA:
-
Appropriate size for gestational age
- MET:
-
Metabolic equivalent of task
- aOR:
-
Adjusted odds ratio
- PAF:
-
Population attributable fraction
- DAG:
-
Directed acyclic graph
References
Grisaru-Granovsky, S., Reichman, B., Lerner-Geva, L., et al. (2012). Mortality and morbidity in preterm small-for-gestational-age infants: A population-based study. American Journal of Obstetrics and Gynecology, 206, 150.e1-7.
Werner, E. F., Savitz, D. A., Janevic, T. M., et al. (2012). Mode of delivery and neonatal outcomes in preterm, small-for-gestational-age newborns. Obstetrics and Gynecology, 120, 560–564.
McCowan, L., & Horgan, R. P. (2009). Risk factors for small for gestational age infants. Best Practice and Research Clinical Obstetrics and Gynaecology, 23, 779–793.
Timmermans, S., Steegers-Theunissen, R. P., Vujkovic, M., et al. (2012). The Mediterranean diet and fetal size parameters: The generation R study. British Journal of Nutrition, 108, 1399–1409.
Olausson, H., Goldberg, G. R., Laskey, M. A., et al. (2012). Calcium economy in human pregnancy and lactation. Nutrition Research Reviews, 25, 40–67.
Dietary Reference Intakes (DRI) for the Spanish Population. (2010). Federación Española de Sociedades de Nutrición, Alimentación y Dietética, FESNAD, Vol. 14, pp. 196–197.
Gil A. Leche y derivados lácteos. (2010). In A. Gil Hernández, & M. D. Ruiz López (Eds.), Madrid Tratado de nutrición: Composición y calidad nutritiva de los alimentos [Nutrition treatise: Composition and nutritional quality of foods] (pp. 1–26). Médica Panamericana.
United States department of agriculture (USDA). Tips for pregnant moms (2013). http://www.nal.usda.gov/wicworks/Topics/PregnancyFactSheet.pdf. Accessed February 2013.
Sociedad Española de Nutrición Comunitaria (SENC) y Sociedad Española de Medicina de Familia y Comunitaria (semFYC) (2007). Consejos para una alimentación saludable [Tips for healthy eating]. http://www.semfyc.es/pfw_files/cma/Informacion/modulo/documentos/guia_alimentacion.pdf.
Brantsæter, A. L., Olafsdottir, A. S., Forsum, E., et al. (2012). Does milk and dairy consumption during pregnancy influence fetal growth and infant birthweight? A systematic literature review. Food and Nutrition Research, 56, 1–13.
Dirección General de Salud Pública, Junta de Andalucía. (2006). Manual de atención al embarazo, parto y puerperio [Guidelines for pregnancy, delivery, and puerperium care]. Consejería de Salud, Junta de Andalucía.
Olmedo-Requena, R., Fernández, J. G., Prieto, C. A., et al. (2014). Factors associated with a low adherence to a Mediterranean diet pattern in healthy spanish women before pregnancy. Public Health Nutrition, 17, 648–656.
Amezcua Prieto, C., Olmedo Requena, R., Jiménez Mejías, E., et al. (2013). Changes in leisure time physical activity during pregnancy compared to the prior year. Maternal and Child Health Journal, 17, 632–638.
Martin-Moreno, J., Boyle, P., Gorgojo, L., et al. (1993). Development and validation of a food frequency questionnaire in Spain. International Journal of Epidemiology, 22, 512–519.
Razquin, C., Martínez, J. A., Martinez-Gonzalez, M. A., et al. (2010). A 3-year Mediterranean-style dietary intervention may modulate the association between adiponectin gene variants and body weight change. European Journal of Nutrition, 49, 311–319.
Beunza, J. J., Toledo, E., Hu, F. B., et al. (2010). Adherence to the Mediterranean diet, long-term weight change, and incident overweight or obesity: The seguimiento Universidad de Navarra (SUN) cohort. American Journal of Clinical Nutrition, 92, 1484–1493.
Mataix, J. (2009). Tabla de Composición de Alimentos Españoles [Food composition tables]. Universidad de Granada. Granada, pp 1–555.
Willett, W. (1998). Nutritional epidemiology. New York: Oxford University Press.
Pereira, M. A., Fitzergerald, S. J., Gregg, E. W., et al. (1997). A collection of physical activity questionnaires for health-related research. Medicine and Science in Sports and Exercise, 29, S1–S205.
Ainsworth, B. E., Haskell, W. L., Whitt, M. C., et al. (2000). Compendium of physical activities: An update of activity codes and MET intensities. Medicine and Science in Sports and Exercise, 32, S498–S504.
WHO. (2000) Obesity: Preventing and managing the global epidemic. Joint WHO/FAO expert consultation. WHO Technical Report Series No. 894. Geneva: WHO.
Álvarez-Dardet, C., Alonso, J., & Domingo, A., et al. (1995). La medición de la clase social en ciencias de la salud [Measuring Social Class in Health Sciences]. In Informe de un Grupo de Trabajo de la Sociedad Española de Epidemiología. Barcelona: SG editores, pp. 63–67.
Mora, P., Gobernado, J. A., Pérez-Milán, F., et al. (2010). Estados hipertensivos del embarazo: Resultados perinatales [pregnancy-induced hypertension: Perinatal outcomes]. Clínica e investigación en Ginecología y Obstetricia, 37, 56–62.
Santamaría Lozano, R., Verdú Martín, L., & García López, G. (1998). Tablas españolas de pesos neonatales según edad gestacional [Spanish tables of neonatal weight by gestational age]. Badalona: Artes Gráficas Beatulo.
González González, N. L., González Dávila, E., García Hernández, J. A., et al. (2014). Construction of model for calculating and recording neonatal weight percentiles. Anales de Pediatría (Barcelona), 80, 81–88.
Carrascosa, A., Yeste, D., Copil, A., et al. (2004). Anthropometric growth patterns of preterm and full-term newborns (24–42 weeks’ gestational age) at the Hospital Materno-Infantil Vall d’Hebron (Barcelona, Spain) 1997–2002. Anales de Pediatría (Barcelona), 60, 406–416.
Aulinas, A., Biagetti, B., Vinagre, I., et al. (2013). Gestational diabetes mellitus and maternal ethnicity: High prevalence of fetal macrosomia in non-Caucasian women. Medicina Clinica (Barcelona), 141, 240–245.
Ricart, W., López, J., Mozas, J., et al. (2009). Maternal glucose tolerance status influences the risk of macrosomia in male but not in female fetuses. Journal of Epidemiology and Community Health, 63, 64–68.
Mahadevan, S., Kumaravel, V., & Bharath, R. (2012). Calcium and bone disorders in pregnancy. Indian Journal of Endocrinology and Metabolism, 16, 358–363.
Hoppe, C., Udam, T. R., Lauritzen, L., et al. (2004). Animal protein intake, serum insulin-like growth factor I, and growth in healthy 2.5-y-old Danish children. American Journal of Clinical Nutrition, 80, 447–452.
Zhu, K., Du, X., Cowell, C. T., et al. (2005). Effects of school milk intervention on cortical bone accretion and indicators relevant to bone metabolism in Chinese girls aged 10–12 y in Beijing. American Journal of Clinical Nutrition, 81, 1168–1175.
Heppe, D., van Dam, R., Willemsen, S., et al. (2011). Maternal milk consumption, fetal growth, and the risks of neonatal complications: The generation R study. American Journal of Clinical Nutrition, 94, 501–509.
Xue, F., Willett, W., Rosner, B., et al. (2008). Parental characteristics as predictors of birthweight. Human Reproduction, 23, 168–177.
Olsen, S., Halldorsson, T., Willett, W., et al. (2007). Milk consumption during pregnancy is associated with increased infant size at birth: Prospective cohort study. American Journal of Clinical Nutrition, 86, 1104–1110.
Mannion, C., Gray-Donald, K., & Koski, K. (2006). Association of low intake of milk and vitamin D during pregnancy with decreased birth weight. Canadian Medical Association Journal, 174, 1273–1277.
Mitchell, E. A., Robinson, E., Clark, P. M., et al. (2004). Maternal nutritional risk factors for small for gestational age babies in a developed country: A case-control study. Archives of Disease in Childhood. Fetal and Neonatal Edition, 89, F431–F435.
Moore, V. M., Davies, M. J., Willson, K. J., et al. (2004). Dietary composition of pregnant women is related to size of the baby at birth. Journal of Nutrition, 134, 1820–1826.
Ludvigsson, J. F., & Ludvigsson, J. (2004). Milk consumption during pregnancy and infant birthweight. Acta Paediatrica, 93, 1474–1478.
Hrolfsdottir, L., Rytter, D., Hammer Bech, B., et al. (2013). Maternal milk consumption, birth size and adult height of offspring: A prospective cohort study with 20 years of follow-up. European Journal of Clinical Nutrition, 67, 1036–1041.
WHO. (2012). Metas Globales 2025: Para mejorar la nutrición materna, del lactante y del niño pequeño [Global goals 2025: For the improvement of the maternal, infant and young child]. http://www.who.int/nutrition/topics/nutrition_globaltargets2025/es/index.html Accessed February.
Nayeri, F., Dalili, H., Nili, F., et al. (2013). Risk factors for neonatal mortality among very low birth weight neonates. Acta Medica Iranica, 51, 297–302.
Hebert, J. R., Clemow, L., Pbert, L., et al. (1995). Social desirability bias in dietary self-report may compromise the validity of dietary intake measures. International Journal of Epidemiology, 24, 389–398.
Cuco, G., Fernández-Ballart, J., Sala, J., et al. (2006). Dietary patterns and associated lifestyles in preconception, pregnancy and postpartum. European Journal of Clinical Nutrition, 60, 364–371.
Elwood, P. C., Haley, T. J., Hughes, S. J., et al. (1981). Child growth (0–5 years), and the effect of entitlement to a milk supplement. Archives of Disease in Childhood, 56, 831–835.
Acknowledgments
The authors thank Jean Sanders for improving the use of English in the manuscript. The results of this study are part of Ph.D. work of Rocío Olmedo-Requena. The present study was funded by FIS Scientific Research Project PI 03/1207 and Junta de Andalucía Excellence Project 2005 CTS 942, as well as the Biomedical Research Centre Network for Epidemiology and Public Health (CIBERESP).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors of this paper declare that they have no conflicts of interest.
Rights and permissions
About this article
Cite this article
Olmedo-Requena, R., Amezcua-Prieto, C., Luna-Del-Castillo, J.D. et al. Association Between Low Dairy Intake During Pregnancy and Risk of Small-for-Gestational-Age Infants. Matern Child Health J 20, 1296–1304 (2016). https://doi.org/10.1007/s10995-016-1931-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-016-1931-2