Abstract
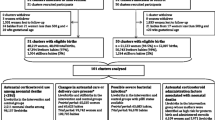
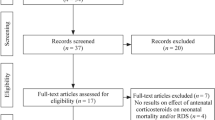
To assess the use of antenatal corticosteroids in clinical circumstances for which both the NIH Guideline and local experts recommend their use and to describe characteristics associated with failure to use recommended antenatal steroids. We convened local experts to adapt the NIH statement by identifying clinical circumstances for which they agree antenatal steroids should always be used. We conducted a retrospective chart review on a cohort study of mothers who delivered premature (24–34 weeks) infants between 2000 and 2002 at three New York City hospitals and investigated the association of failure to treat with antenatal steroids with characteristics of the mother, pregnancy, delivery, and hospital. Twenty percent (101/515) of eligible mothers failed to receive indicated antenatal corticosteroid therapy. Of these, 43% delivered more than 2 h after admission, and 33% delivered more than 4 h after admission, indicating sufficient time to have treated them. Lack of prenatal care, longer gestation, advanced cervical exam, and intact membranes at admission were associated with failure to receive the recommended therapy. Antenatal steroids were under-utilized in our sample. If our results our generalizable, opportunities for quality improvement in the antenatal management of mothers in preterm labor exist.
Similar content being viewed by others
References
Crowley, P. A. (1995). Antenatal corticosteroid therapy: A meta-analysis of the randomized trials, 1972–1994. American Journal of Obstetrics and Gynecology, 173(1), 322–335. doi:10.1016/0002-9378(95)90222-8.
Roberts, D., & Dalziel, S. R. (2006). Antenatal corticosteroids for accelerating fetal lung maturation for women at risk of preterm birth. Cochrane Database of Systematic Reviews, (3). Art. No.: CD004454. doi:10.1002/14651858.CD004454.pub2.
The Effect of Antenatal Steroids for Fetal Maturation on Perinatal Outcomes-Interim Draft Statement. NIH Consens Statement Online 1994 Feb 28–Mar 2 [cited August 4, 2008]. 12(2), 1–24.
Elimian, A., Figueroa, R., Spitzer, A. R., et al. (2003). Antenatal corticosteroids: Are incomplete courses beneficial? Obstetrics and Gynecology, 102(2), 352–355. doi:10.1016/S0029-7844(03)00485-X.
Chien, L. Y., Ohlsson, A., Seshia, M. M., et al. (2002). Variations in antenatal corticosteroid therapy: A persistent problem despite 30 years of evidence. Obstetrics and Gynecology, 99(3), 401–408. doi:10.1016/S0029-7844(01)01732-X.
Sinclair, J. C. (1995). Meta-analysis of randomized controlled trials of antenatal corticosteroid for the prevention of respiratory distress syndrome. American Journal of Obstetrics and Gynecology, 173(1), 335–344. doi:10.1016/0002-9378(95)90223-6. discussion.
New York City Birth and Infant Mortality Trends. New York: New York City Department of Health and Mental Hygiene. 2006 Updated October 31, 2008. Accessed March 15, 2009 at http://www.nyc.gov/html/doh/html/ms/ms-bimt.shtml.
Ohlsson, H., Lindblad, U., Lithman, T., et al. (2005). Understanding adherence to official guidelines on statin prescribing in primary health care––a multi-level methodological approach. European Journal of Clinical Pharmacology, 61(9), 657–665. doi:10.1007/s00228-005-0975-9.
Boyd, E. A. (1998). Bureaucratic authority in the “company of equals” “the interactional management of medical Peer review. American Sociological Review, 63(2), 200–224. doi:10.2307/2657323.
Greco, P. J., & Eisenberg, J. M. (1993). Changing physicians’ practices. The New England Journal of Medicine, 329(17), 1271–1274.
Assessment of Risk Factors for Preterm Birth. (2001). ACOG practice bulletin no. 31. Obstetrics and Gynecology, 98, 709–716.
Murphy, K. E., Reuss, M. L., Leviton, A., et al. (1998). Variation in use of corticosteroids among infants ≤1, 500 g across hospitals in three states. The Journal of Maternal-Fetal Medicine, 7(3), 137–141. doi:10.1002/(SICI)1520-6661(199805/06)7:3<137::AID-MFM7>3.0.CO;2-L.
Wirtschafter, D. D., Danielsen, B. H., Main, E. K., et al. (2006). Promoting antenatal steroid use for fetal maturation: Results from the California perinatal quality care collaborative. The Journal of Pediatrics, 148(5), 606–612. doi:10.1016/j.jpeds.2005.12.058.
Leviton, L. C., Goldenberg, R. L., Baker, C. S., et al. (1999). Methods to encourage the use of antenatal corticosteroid therapy for fetal maturation: A randomized controlled trial. Journal of the American Medical Association, 281(1), 46–52. doi:10.1001/jama.281.1.46.
Wennberg, J. (1999). Understanding geographic variations in health care delivery. The New England Journal of Medicine, 340, 52–53. Jan. 7, No. 1.
Wennberg, J. E., & Barnis, B. A. (1982). Zubkopp. Professional uncertainty and the problem of supplier-induced demand. Social Science and Medicine, 16, 811–824. doi:10.1016/0277-9536(82)90234-9.
Davies, B. L., Stewart, P. J., Sprague, A. E., et al. (1998). Education of women about the prevention of preterm birth. Canadian Journal of Public Health, 89(4), 260–263.
Sprague, A., Stewart, P., Niday, P., et al. (2002). Community education on preterm birth. Does it change practice? Canadian Family Physician Medecin de Famille Canadien, 48(72), 7–734.
Antenatal Corticosteroids Revisited: Repeat Courses. NIH Consens Statement Online 2000 August 17–18; [March 15, 2009]. 17(2), 1–10.
Acknowledgements
Supported by the Agency for Healthcare Research and Quality (PO1 HS10859) the Commonwealth Fund (20030088), and the National Center for Minority Health and Health Disparities (P60 MD00270). The opinions, view, and conclusions expressed in this article are those of the authors and not necessarily those of the Agency for Healthcare Research and Quality or the Commonwealth Fund.
Author information
Authors and Affiliations
Corresponding author
Appendix
Appendix
Management of Prematurity Steering Committee Obstetric Interventions: Antenatal Corticosteroids
Guidelines
-
1.
All women who present in preterm labor with intact membranes between 24 and 34 weeks gestation should receive a course of antenatal corticosteroids.
Exceptions:
-
1.
Patients with contraindications to corticosteroids (e.g. chorioamnionitis)
-
2.
Patients who have already received a course of antenatal corticosteroids
-
3.
Patients for whom antenatal corticosteroid administration is not feasible because immediate delivery is anticipated
-
1.
-
2.
All pregnant women between 24 and 34 weeks gestation who are not in labor but require delivery within 7 days secondary to maternal or infant indications * should receive a course of antenatal corticosteroids.
Exceptions:
-
1.
Patients with contraindications to corticosteroids
-
2.
Patients who have already received a course of antenatal corticosteroids
-
3.
Patients for whom antenatal corticosteroid administration is not feasible because immediate delivery is anticipated
-
1.
-
3.
A single course of antenatal corticosteroids should consist either of betamethasone 12 mg intramuscularly every 24 h for 2 doses or dexamethasone 6 mg intramuscularly every 12 h for 4 doses.
-
4.
All patients with preterm premature rupture of membranes (PPROM) between 24 and 32 weeks gestation should receive a course of antenatal corticosteroids.
Exceptions:
-
1.
Patients with contraindications to corticosteroids
-
2.
Patients who have already received a course of antenatal corticosteroids
-
3.
Patients with documented fetal lung maturity
-
1.
* Examples of maternal and infant indications that may require preterm delivery are preeclampsia, diabetes, intrauterine growth retardation, and hydrops.
Rights and permissions
About this article
Cite this article
Howell, E.A., Stone, J., Kleinman, L.C. et al. Approaching NIH Guideline Recommended Care for Maternal–Infant Health: Clinical Failures to Use Recommended Antenatal Corticosteroids. Matern Child Health J 14, 430–436 (2010). https://doi.org/10.1007/s10995-009-0480-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-009-0480-3