Abstract
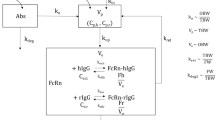
This study investigates the impact of disease on nicotinic acid (NiAc)-induced changes in plasma concentrations of non-esterified fatty acids (NEFA). NiAc was given by constant intravenous infusion to normal Sprague–Dawley and obese Zucker rats, and arterial blood samples were taken for analysis of NiAc, NEFA, insulin and glucose plasma concentrations. The intravenous route was intentionally selected to avoid confounding processes, such as absorption, following extravascular administration. Data were analyzed using nonlinear mixed effects modeling (NONMEM, version VI). The disposition of NiAc in the normal rats was described by a two-compartment model with endogenous synthesis of NiAc and two parallel capacity-limited elimination processes. In the obese rats disposition was described by a one-compartment model with endogenous synthesis of NiAc and one capacity-limited elimination process. The plasma concentration of NiAc drove NEFA (R) turnover via an inhibitory drug-mechanism function acting on the formation of NEFA. NEFA turnover was described by a feedback model with a moderator distributed over a series of transit compartments, where the first compartment (M 1 ) inhibited the formation of R and the last compartment (M N ) stimulated the loss of R. All processes regulating plasma NEFA concentrations were assumed to be captured by the moderator function. Differences in the pharmacodynamic response of the two strains included, in the obese animals, an increased NEFA baseline, diminished rebound and post-rebound oscillation, and a more pronounced slowly developing tolerance during the period of constant drug exposure. The feedback model captured the NiAc-induced changes in NEFA response in both the normal and obese rats. Differences in the parameter estimates between the obese and normal rats included, in the former group, increases in R 0 , k in and p by 44, 41 and 78 %, respectively, and decreases in k out and γ by 64 and 84 %, respectively. The estimates of k tol and IC 50 were similar in both groups. The NiAc–NEFA concentration–response relationship at equilibrium was substantially different in the two groups, being shifted upwards and to the right, and being shallower in the obese rats. The extent of such shifts is important, as they demonstrate the impact of disease at equilibrium and, if ignored, will lead to erroneous dose predictions and, in consequence, poorly designed studies. The proposed models are primarily aimed at screening and selecting candidates with the highest potential of becoming a viable drug in man.









Similar content being viewed by others
References
Ballantyne CM, O’Keefe JH, Gotto AM (2009) Dyslipidemia & atherosclerosis essentials, overview of atherosclerosis and dyslipidemia. Jones and Bartlett, Sudbury
National Cholesterol Education Program (2002) Detection, evaluation and treatment of high blood cholesterol in adults. http://www.nhlbi.nih.gov/guidelines/cholesterol/atp3full.pdf
Grundy SM, Mok HYI, Zech L, Berman M (1981) Influence of nicotinic acid on metabolism of cholesterol and triglycerides in man. J Lipid Res 22(1):24–36
Vega GL, Grundy SM (1994) Lipoprotein responses to treatment with lovastatin, gemfibrozil, and nicotinic acid in normolipidemic patients with hypoalphalipoproteinemia. Arch Intern Med 154(1):73–82
Martin-Jadraque R, Tato F, Mostaza JM, Vega GL, Grundy SM (1996) Effectiveness of low-dose crystalline nicotinic acid in men with low high-density lipoprotein cholesterol levels. Arch Intern Med 156(10):1081–1088
Mostaza JM, Schulz I, Vega GL, Grundy SM (1997) Comparison of pravastatin with crystalline nicotinic acid monotherapy in treatment of combined hyperlipidemia. Am J Cardiol 79(9):1298–1301
Guyton JR, Goldberg AC, Kreisberg RA, Sprecher DL, Superko HR, O’Connor CM (1998) Effectiveness of once-nightly dosing of extended-release niacin alone and in combination for hypercholesterolemia. Am J Cardiol 82(6):737–743
Knopp RH, Alagona P, Davidson M, Goldberg AC, Kafonek SD, Kashyap M, Sprecher D, Superko HR, Jenkins S, Marcovina S (1998) Equivalent efficacy of a time-release form of niacin (Niaspan) given once-a-night versus plain niacin in the management of hyperlipidemia. Metab Clin Exp 47(9):1097–1104
Capuzzi DM, Guyton JR, Morgan JM, Goldberg AC, Kreisberg RA, Brusco OA, Brody J (1998) Efficacy and safety of an extended-release niacin (Niaspan): a long-term study. Am J Cardiol 82(12):74–81
Guyton JR, Blazing MA, Hagar J, Kashyap ML, Knopp RH, McKenney JM, Nash DT, Nash SD (2000) Extended-release niacin vs gemfibrozil for the treatment of low levels of high-density lipoprotein cholesterol. Arch Intern Med 160(8):1177–1184
Carlson LA (1963) Studies on the effect of nicotinic acid on catecholamine stimulated lipolysis in adipose tissue in vitro. Acta Med Scand 173:719–722
Lauring B, Taggart AKP, Tata JR, Dunbar R, Caro L, Cheng K, Chin J, Colletti SL, Cote J, Khalilieh S, Liu J, Luo W, MacLean AA, Peterson LB, Polis AB, Sirah W, Wu T, Liu X, Jin L, Wu K, Boatman PD, Semple G, Behan DP, Connolly DT, Lai E, Wagner JA, Wright SD, Cuffie C, Mitchel YB, Rader DJ, Paolini JF, Waters MG, Plump A (2012) Niacin lipid efficacy is independent of both the niacin receptor GPR109A and free fatty acid suppression. Sci Transl Med 4(148):115–124
Dobbins RL, Shearn SP, Byerly RL, Gao FF, Mahar KM, Napolitano A, Nachbaur GJ, Le Monnier de Gouville AC (2013) GSK256073, a selective agonist of G-protein coupled receptor 109A (GPR109A) reduces serum glucose in subjects with type 2 diabetes mellitus. Diabetes Obes Metab. doi:10.1111/dom.12132
Fulcher GR, Walker M, Catalano C, Agius L, Alberti KGMM (1992) Metabolic effects of suppression of nonesterified fatty acid levels with acipimox in obese NIDDM subjects. Diabetes 41(11):1400–1408
Kumar S, Durrington PN, Bhatnagar D, Laing I (1994) Suppression of non-esterified fatty acids to treat type A insulin resistance syndrome. Lancet 343(8905):1073–1074
Bajaj M, Suraamornkul S, Kashyap S, Cusi K, Mandarino L, DeFronzo RA (2004) Sustained reduction in plasma free fatty acid concentration improves insulin action without altering plasma adipocytokine levels in subjects with strong family history of type 2 diabetes. J Clin Endocrinol Metab 89(9):4649–4655
Worm D, Henriksen JE, Vaag A, Thye-Ronn P, Melander A, Beck-Nielsen H (1994) Pronounced blood glucose-lowering effect of the antilipolytic drug acipimox in noninsulin-dependent diabetes mellitus patients during a 3-day intensified treatment period. J Clin Endocrinol Metab 78(3):717–721
Metcalfe P, Johnston DG, Nosadini R (1981) Metabolic effects of acute and prolonged growth hormone excess in normal and insulin-deficient man. Diabetologia 20(2):123–128
Gill A, Johnston DG, Orskov H (1982) Metabolic interactions of glucagon and cortisol in man—studies with somatostatin. Metab Clin Exp 31(4):305–311
Mittelman SD, Bergman RN (2000) Inhibition of lipolysis causes suppression of endogenous glucose production independent of changes in insulin. Am J Physiol 279(3):630–637
Stralfors P, Bjorgell P, Belfrage P (1984) Hormonal regulation of hormone-sensitive lipase in intact adipocytes: identification of phosphorylated sites and effects on the phosphorylation by lipolytic hormones and insulin. Proc Natl Acad Sci USA 81(11):3317–3321
Frayn KN, Shadid S, Hamlani R, Humphreys SM, Clark ML, Fielding BA, Boland O, Coppack SW (1994) Regulation of fatty acid movement in human adipose tissue in the postabsorptive-to-postprandial transition. Am J Physiol Endocrinol Metab 266(3):308–317
Sadur CN, Eckel RH (1982) Insulin stimulation of adipose tissue lipoprotein lipase. Use of the euglycemic clamp technique. J Clin Invest 69(5):1119–1125
Ahlström C, Peletier LA, Jansson-Löfmark R, Gabrielsson J (2011) Feedback modeling of non-esterified fatty acids in rats after nicotinic acid infusions. J Pharmacokinet Pharmacodyn 38(1):1–24
Ahlström C, Peletier LA, Gabrielsson J (2011) Quantitative analysis of rate and extent of tolerance of biomarkers: application to nicotinic acid-induced changes in non-esterified fatty acids in rats. Eur J Pharm Sci 44(3):250–264
Ahlström C, Peletier LA, Gabrielsson J (2013) Challenge of a mechanistic feedback model describing nicotinic acid-induced changes in non-esterified fatty acids in rats. J Pharmacokinet Pharmacodyn 40(4):497–512
Levy G (1993) Integration of pharmacokinetics, pharmacodynamics and toxicokinetics in rational drug development, the case for preclinical pharmacodynamics. Plenum, New York
Zucker L, Zucker T (1961) Fatty, a new mutation in the rat. J Hered 52:275–278
Shum L, Jusko WJ (1984) Theophylline disposition in obese rats. J Pharmacol Exp Ther 228(2):380–386
Jaber LA, Ducharme MP, Halapy H (1996) The effects of obesity on pharmacokinetics and pharmacodynamics of glipizide in patients with non-insulin-dependent diabetes mellitus. Ther Drug Monit 18(1):6–13
Cheymol G (2000) Effects of obesity on pharmacokinetics: implications for drug therapy. Clin Pharmacokinet 39(3):215–231
Cortinez LI, Anderson BJ, Penna A, Olivares L, Munoz HR, Holford NHG, Struys MMRF, Sepulveda P (2010) Influence of obesity on propofol pharmacokinetics: derivation of a pharmacokinetic model. Br J Anaesth 105(4):448–456
Hanley MJ, Abernethy DR, Greenblatt DJ (2010) Effect of obesity on the pharmacokinetics of drugs in humans. Clin Pharmacokinet 49(2):71–87
Danhof M, Levy G (1984) Kinetics of drug action in disease states. I. Effect of infusion rate on phenobarbital concentrations in serum, brain and cerebrospinal fluid of normal rats at onset of loss of righting reflex. J Pharmacol Exp Ther 229(1):44–50
Rohner-Jeanrenaud F, Proietto J, Ionescu E, Jeanrenaud B (1986) Mechanism of abnormal oral glucose tolerance of genetically obese fa/fa rats. Diabetes 35(12):1350–1355
McCaleb ML, Sredy J (1992) Metabolic abnormalities of the hyperglycemic obese Zucker rat. Metab Clin Exp 41(5):522–525
Zucker LM, Antoniades HN (1972) Insulin and obesity in the Zucker genetically obese rat “fatty”. Endocrinology 90(5):1320–1330
Martin RJ, Wangsness PJ, Gahagan JH (1978) Diurnal changes in serum metabolites and hormones in lean and obese Zucker rats. Horm Metab Res 10(3):187–192
Tannenbaum GS, Lapointe M, Gurd W, Finkelstein JA (1990) Mechanisms of impaired growth hormone secretion in genetically obese Zucker rats: roles of growth hormone-releasing factor and somatostatin. Endocrinology 127(6):3087–3095
Terrettaz J, Assimacopoulos-Jeannet F, Jeanrenaud B (1986) Severe hepatic and peripheral insulin resistance as evidenced by euglycemic clamps in genetically obese fa/fa rats. Endocrinology 118(2):674–678
Eaton RP, Conway M, Schade DS (1976) Endogenous glucagon regulation in genetically hyperlipemic obese rats. Am J Physiol 230(5):1336–1341
Martin RJ, Gahagan JH (1977) The influence of age and fasting on serum hormones in the lean and obese-Zucker rat. Proc Soc Exp Biol Med 154(4):610–614
Popovic V, Popovic P (1960) Permanent cannulation of aorta and vena cava in rats and ground squirrels. J Appl Physiol 15(4):727–728
Isaksson C, Wallenius K, Peletier LA, Toresson H, Gabrielsson J (2009) Turnover modeling of non-esterified fatty acids in rats after multiple intravenous infusions of nicotinic acid. Dose-Response 7(3):247–269
van Schaick EA, Zuideveld KP, Tukker HE, Langemeijer MWE, Ijzerman AP, Danhof M (1998) Metabolic and cardiovascular effects of the adenosine A1 receptor agonist N6-(p-sulfophenyl)adenosine in diabetic Zucker rats: influence of the disease on the selectivity of action. J Pharmacol Exp Ther 287(1):21–30
Bray GA (1977) The Zucker-fatty rat: a review. Fed Proc 36(2):148–153
Schonfeld G, Pfleger B (1971) Overproduction of very low-density lipoproteins by livers of genetically obese rats. Am J Physiol 220(5):1178–1181
Schonfeld G, Felski C, Howald MA (1974) Characterization of the plasma lipoproteins of the genetically obese hyperlipoproteinemic Zucker fatty rat. J Lipid Res 15(5):457–464
Kato R (1977) Drug metabolism under pathological and abnormal physiological states in animals and man. Xenobiotica 7:25–92
Levy G (1977) Pharmacokinetics in renal disease. Am J Med 62(4):461–465
Breimer DD (1987) Pharmacokinetics in liver disease. Pharm Weekbl Sci Ed 9(2):79–84
Frayn KN, Williams CM, Arner P (1996) Are increased plasma non-esterified fatty acid concentrations a risk marker for coronary heart disease and other chronic diseases? Clin Sci 90(4):243–253
Rowland, Tozer (1995) Clinical pharmacokinetics, concepts and applications. Williams and Wilkins, Baltimore
Vaag AA, Beck-Nielsen H (1992) Effects of prolonged acipimox treatment on glucose and lipid metabolism and on in vivo insulin sensitivity in patients with non-insulin dependent diabetes mellitus. Acta Endocrinol (Copenh) 127(4):344–350
Garg A, Grundy SM (1990) Nicotinic acid as therapy for dyslipidemia in non-insulin-dependent diabetes mellitus. J Am Med Assoc 264(6):723–726
Thadani U, Fung HL, Darke AC, Parker JO (1982) Oral isosorbide dinitrate in angina pectoris: comparison of duration of action and dose-response relation during acute and sustained therapy. Am J Cardiol 49(2):411–419
Jamrozik K, Fowler G, Vessey M, Wald N (1984) Placebo controlled trial of nicotine chewing gum in general practice. Br Med J 289(6448):794–797
Parker JO, Fung HL (1984) Transdermal nitroglycerin in angina pectoris. Am J Cardiol 54(6):471–476
Jordan RA, Seth L, Casebolt P (1986) Rapidly developing tolerance to transdermal nitroglycerin in congestive heart failure. Ann Intern Med 104(3):295–298
Elkayam U, Kulick D, McIntosh N (1987) Incidence of early tolerance to hemodynamic effects of continuous infusion of nitroglycerin in patients with coronary artery disease and heart failure. Circulation 76(3):577–584
Porchet HC, Benowitz NL, Sheiner LB (1988) Pharmacodynamic model of tolerance: application to nicotine. J Pharmacol Exp Ther 244(1):231–236
Author information
Authors and Affiliations
Corresponding author
Appendix
Appendix
Steady state response
The steady state values for the response R and the moderators M i (i = 1,…, N) of the feedback model, formulated in Eq. (3) and (4), are given by:
where R ss is the unique solution of the equation:
in which
and R 0 is the baseline response. There is no explicit solution to Eq. (11).
For the obese animals, k cap could not be estimated and was therefore fixed to zero throughout the analysis. Equation (11) can then be simplified and solved for R SS :
Response at baseline
At baseline, I(C p ) = 1, and Eq. (11) can be expressed as:
For the obese animals where k cap = 0, Eq. (14) can then be simplified and solved for R 0 :
For the normal rats k cap is assumed to be small compared to the other terms in Eq. (14), and the baseline can therefore be approximated according to Eq. (15).
Steady state response at IC 50
Assuming that I max = 1, the inhibitory drug mechanism function at IC 50 is equal to 0.5. For the obese rats, Eq. (13) can be expressed as:
If k cap for the normal animals is assumed to be smaller than the other terms in Eq. (11), the steady state response at IC 50 for the normal rats can be approximated by Eq. (16), although this will slightly underestimate the value of R SS .
Steady state response at high NiAc concentrations
As I max = 1, it follows from the definition of I(C p ) (Eq. 2) that \( I(C_{p} ) \to 0 \) as \( C_{p} \to \infty \). This implies that:
For the obese animals where k cap = 0 it follows that:
For the normal animals, the sigmoidicity factor γ is equal to 2.2. At NiAc concentrations higher than 0.5 μmol L−1, \( IC_{50}^{\gamma } \ll C_{p}^{\gamma } \) and I(C p ) ≈ 0. Equation (17) is therefore valid at NiAc concentrations of 0.5 μmol L−1 and higher.
For the obese animals, the sigmoidicity factor γ is equal to 0.35 and \( IC_{50}^{\gamma } \) will then extensively affect I(C p ) at NiAc concentrations far above 1,000 μmol L−1. The steady state response \( R_{SS,obese} \) will therefore not approach zero within a therapeutic concentration interval. The steady state response \( R_{SS,obese} \) at high NiAc concentrations is still described by Eq. (13).
Rights and permissions
About this article
Cite this article
Ahlström, C., Kroon, T., Peletier, L.A. et al. Feedback modeling of non-esterified fatty acids in obese Zucker rats after nicotinic acid infusions. J Pharmacokinet Pharmacodyn 40, 623–638 (2013). https://doi.org/10.1007/s10928-013-9335-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10928-013-9335-z