Abstract
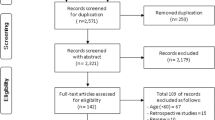
Accidental falls are a leading cause of disability and death in older adults living in urban centers. However, little is known about the consequences of falls in rural communities. We aimed to assess characteristics and risk of falls in community-dwellers aged ≥ 60 years living in rural Ecuador. Of 463 older adults enrolled in the Atahualpa Project, 327 (71%) were included. Multivariate logistic regression models were fitted to assess factors associated with history of falls and risk of future falls. Sensitivity analysis was conducted to determine which component of the Downton fall risk index (DFRI) better predicts risk of future falls. A history of falls was reported by 173 (53%) individuals. Most were related to stumbling due to uneven (non-paved) streets. Only three individuals had bone fractures after the fall. Previous falls were not associated with any of the investigated covariables. The DFRI was positive in 87 (27%) participants, and was associated with age (p < 0.001) and history of stroke (p < 0.001). None of the subjects were taking tranquilizers/sedatives. The most reliable component of the DFRI was the presence of sensory/motor deficits. History of falls in our population is similar to that reported elsewhere. However, the risk of future falls is lower. Such discrepancies are probably because the DFRI does not take into account environmental factors resulting in falls. There were almost no severe complications from falls, which could be partly related to the lack of use of tranquilizers/sedatives.
Similar content being viewed by others
References
Burns, E. R., Stevens, J. A., & Lee, R. (2016). The direct costs of fatal and non-fatal falls among older adults—United States. Journal of Safety Research, 58(9), 99–103.
Del Brutto, O. H., Mera, R. M., Castillo, P. R., & Del Brutto, V. J. (2018). Key findings from the Atahualpa Project: What should be learn? Expert Review of Neurotherapeutics, 18(1), 5–8.
Del Brutto, O. H., Peñaherrera, E., Ochoa, E., Santamaría, M., Zambrano, M., & Del Brutto, V. J. (2014). Door-to-door survey of cardiovascular health, stroke, and ischemic heart disease in rural coastal Ecuador—the Atahualpa Project: Methodology and operational definitions. International Journal of Stroke, 9(4), 367–371.
Lloyd-Jones, D., Hong, Y., Labarthe, F., et al. (2010). Defining and setting national goals for cardiovascular health promotion. The American Heart Association’s strategic impact goal through 2020 and beyond. Circulation, 121(4), 586–613.
Nilsson, M., Eriksson, J., Larsson, B., Odén, A., Johansson, H., & Lorentzon, M. (2016). Fall risk assessment predicts fall-related injury, hip fracture, and head injury in older adults. Journal of the American Geriatrics Society, 64(11), 2242–2250.
Mojtaba, M., Alinaghizadeh, H., & Rydwik, E. (2018). Downton Fall Risk Index during hospitalization is associated with fall-related injuries after discharge: A longitudinal observational study. Journal of Physiotherapy, 64(3), 172–177.
Talbot, L. A., Musiol, R. J., Witham, E. K., & Metter, E. J. (2005). Falls in young, middle-aged and older community-dwelling adults: Perceived causes, environmental factors and injury. BMC Public Health, 5, 86.
Trevisan, C., Crippa, A., Ek, S., et al. (2018). Nutritional status, body mass index, and the risk of falls in community-dwelling older adults: A systematic review and meta-analysis. Journal of the American Medical Directors Association. https://doi.org/10.1016/j.jamda.2018.10.027.
Ambrose, A. F., Paul, G., & Hausdorff, J. M. (2013). Risk factors for falls among older adults: A review of the literature. Maturitas, 75(1), 51–61.
Hausdorff, J. M., Rios, D. A., & Edelberg, H. K. (2001). Gait variability and fall risk in community-living older adults: A 1-year prospective study. Archives of Physical Medicine and Rehabilitation, 82(8), 1050–1056.
Rubenstein, L. Z., & Josephson, K. R. (2002). The epidemiology of falls and syncope. Clinical and Geriatric Medicine, 18(2), 141–158.
Karlsson, M. K., Vonschewelov, T., Karlsson, C., Coster, M., & Rosengen, B. E. (2013). Prevention of falls in the elderly: A review. Scandinavian Journal of Public Health, 41(5), 442–454.
Pereira, S. G., Santos, C. B. D., Doring, M., & Portella, M. R. (2017). Prevalence of household falls in long-lived adults and Association with extrinsic factors. Revista Latino-Americana de Enfermagem, 25, e2900.
Westerlind, B., Ostgren, C. J., Molstad, S., Midlov, P., & Hagg, S. (2018). Use of non-benzodiazepine hypnotics is associated with falls in nursing home residents: A longitudinal cohort study. Aging Clinical and Experimental Research. https://doi.org/10.1007/s40520-018-1056-0.
Del Brutto, O. H., Mera, R. M., Gillman, J., Zambrano, M., & Ha, J. E. (2016). Oily fish intake and cognitive performance in community-dwelling older adults: The Atahualpa Project. Journal of Community Health, 41(1), 82–86.
Choi, E., & Park, Y. (2016). The association between the consumption of fish/shellfish and the risk of osteoporosis in men and postmenopausal women aged 50 years or older. Nutrients, 8(3), 113.
Coughlan, T., & Dockery, F. (2014). Osteoporosis and fracture risk in older people. Clinical Medicine, 14(2), 187–191.
Del Brutto, O. H., Mera, R. M., de la Luz Andrade, M., et al. (2016). Temporal bone thickness and texture are major determinants of the high rate of insonation failures of transcranial Doppler in Amerindians (The Atahualpa Project). Journal of Clinical Ultrasound, 44(1), 55–60.
Funding
This study was partially supported by an unrestricted grant from Universidad Espiritu Santo – Ecuador, Guayaquil, Ecuador.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Del Brutto, O.H., Mera, R.M., Peinado, C.D. et al. Prevalence, Severity, and Risk of Future Falls in Community-Dwelling Older Adults Living in a Rural Community: The Atahualpa Project. J Community Health 44, 487–491 (2019). https://doi.org/10.1007/s10900-019-00664-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10900-019-00664-3