Abstract
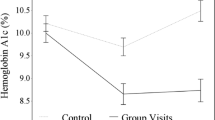
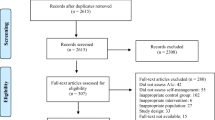
Integrated behavioral healthcare (IBH) is the “standard of care” to address psychosocial factors impacting diabetes outcomes; it is not standard in practice. This longitudinal, retrospective, chart-review examines IBH impact on glycemic control in an adult diabetes clinic. Adults (n = 374) with ≥ 1 behavioral health encounter, ≥ 2 hemoglobin A1c (HbA1c) values, and HbA1c value > 8% at initial IBH visit were included. Mixed effects linear piecewise models examined differences in slope trajectories for 365 days pre- and post-IBH intervention. Pre-intervention slope was not significant (z = − 1.09, p = 0.28). The post-intervention slope was significant (z = − 6.44, p < 0.001), indicating a significant linear decrease in HbA1c values. Results demonstrated that prior to engaging with behavioral health, there was no change in HbA1c. After initial IBH visit, there was a predicted reduction of > 1% in HbA1c over the following year. These results suggest that IBH significantly improves patients’ metabolic status. Next steps for IBH research are offered.


Similar content being viewed by others
References
Alam, R., Sturt, J., Lall, R., & Winkley, K. (2009). An updated meta-analysis to assess the effectiveness of psychological interventions delivered by psychological specialists and generalist clinicians on glycaemic control and on psychological status. Patient Education and Counseling, 75(1), 25–36. https://doi.org/10.1016/j.pec.2008.08.026
American Diabetes Association. (2018). 4. Lifestyle management: Standards of medical care in diabetes—2018. Diabetes Care, 41(Supplement 1), S38–S50. https://doi.org/10.2337/dc18-S004
Anderson, B. J. (2002). Involving family members in diabetes treatment. In B. J. Anderson & R. R. Rubin (Eds.), Practical psychology for diabetes clinicians (2nd ed., pp. 199–207). American Diabetes Association.
Asche, C., LaFleur, J., & Connor, C. (2011). A review of diabetes treatment adherence and the association with clinical and economic outcomes. Clinical Therapeutics, 33(1), 74–109. https://doi.org/10.1016/j.clinthera.2011.01.019
Barry, S. A., Harlan, D. M., Johnson, N., & MacGregor, K. L. (2018). State of behavioral health integration in US diabetes care: How close are we to ADA recommendations? Diabetes Care, 41(7), e115–e116. https://doi.org/10.2337/dc18-0642
Beck, J. (2011). Cognitive behavioral therapy: Basics and beyond (2nd ed.). The Guilford Press.
Blount, A. (2003). Integrated primary care: Organizing the evidence. Family Systems and Health, 21(2), 121–133. https://doi.org/10.1037/1091-7527.21.2.121
Chou, C.-P., Yang, D., Pentz, M. A., & Hser, Y.-I. (2004). Piecewise growth curve modeling approach for longitudinal prevention study. Computational Statistics & Data Analysis, 46, 213–225. https://doi.org/10.1016/S0167-9473(03)00149-X
Chwastiak, L. A., Jackson, S. L., Russo, J., DeKeyser, P., Kiefer, M., Belyeu, B., Mertens, K., Chew, L., & Lin, E. (2017). A collaborative care team to integrate behavioral health care and treatment of poorly-controlled type 2 diabetes in an urban safety net primary care clinic. General Hospital Psychiatry, 44, 10–15. https://doi.org/10.1016/j.genhosppsych.2016.10.005
Cochran, J., & Conn, V. S. (2008). Meta-analysis of quality of life outcomes following diabetes self-management training. The Diabetes Educator, 34(5), 815–823. https://doi.org/10.1177/0145721708323640
Cox, D. J., Gonder-Frederick, L., Polonsky, W., Schlundt, D., Kovatchev, B., & Clarke, W. (2001). Blood glucose awareness training (BGAT-2). Diabetes Care, 24(4), 637–642. https://doi.org/10.2337/diacare.24.4.637
de Groot, M., Golden, S. H., & Wagner, J. (2016). Psychological conditions in adults with diabetes. American Psychologist, 71(7), 552–562. https://doi.org/10.1037/a0040408
Ducat, L., Philipson, L. H., & Anderson, B. J. (2014). The mental health comorbidities of diabetes. JAMA, 312(7), 691–692. https://doi.org/10.1001/jama.2014.8040
Egede, L. E., & Ellis, C. (2010). Diabetes and depression: Global perspectives. Diabetes Research and Clinical Practice, 87(3), 302–312. https://doi.org/10.1016/j.diabres.2010.01.024
Fisher, L., Hessler, D., Glasgow, R. E., Arean, P. A., Masharani, U., Naranjo, D., & Strycker, L. A. (2013). REDEEM: A pragmatic trial to reduce diabetes distress. Diabetes Care, 36(9), 2551–2558. https://doi.org/10.2337/dc12-2493
Fisher, L., Hessler, D., Polonsky, W. H., Masharani, U., Guzman, S., Bowyer, V., Strycker, L., Ahmann, A., Basina, M., Blumer, I., Chloe, C., Kim, S., Peters, A. L., Shumway, M., Weihs, K., & Wu, P. (2018). T1-REDEEM: A randomized controlled trial to reduce diabetes distress among adults with type 1 diabetes. Diabetes Care, 41(9), 1862–1869. https://doi.org/10.2337/dc18-0391
Fisher, L., Hessler, D. M., Polonsky, W. H., & Mullan, J. (2012). When is diabetes distress clinically meaningful? Establishing cut points for the Diabetes Distress Scale. Diabetes Care, 35(2), 259–264. https://doi.org/10.2337/dc11-1572
Flora, D. B. (2008). Specifying piecewise latent trajectory models for longitudinal data. Structural Equation Modeling, 15(3), 513–533. https://doi.org/10.1080/10705510802154349
Glasgow, R. E., Toobert, D. J., & Gillette, C. D. (2001). Psychosocial barriers to diabetes self-management and quality of life. Diabetes Spectrum, 14(1), 33–41. https://doi.org/10.2337/diaspect.14.1.33
Harkness, E., Macdonald, W., Valderas, J., Coventry, P., Gask, L., & Bower, P. (2010). Identifying psychosocial interventions that improve both physical and mental health in patients with diabetes. Diabetes Care, 33(4), 926–930. https://doi.org/10.2337/dc09-1519
Ibrahim, J. G., & Molenberghs, G. (2009). Missing data methods in longitudinal studies: A review. Test (madr), 18(1), 1–43. https://doi.org/10.1007/s11749-009-0138-x
Ismail, K., Winkley, K., & Rabe-Hesketh, S. (2004). Systematic review and meta-analysis of randomised controlled trials of psychological interventions to improve glycaemic control in patients with type 2 diabetes. The Lancet, 363(9421), 1589–1597. https://doi.org/10.1016/S0140-6736(04)16202-8
Katon, W. J., Lin, E. H., Von Korff, M., Ciechanowski, P., Ludman, E. J., Young, B., Peterson, D., Rutter, C. M., McGregor, M., & McCulloch, D. (2010). Collaborative care for patients with depression and chronic illnesses. New England Journal of Medicine, 363(27), 2611–2620. https://doi.org/10.1056/nejmoa1003955
King, D. E., Petrone, A. B., Alcantara, F. M., Elavsky, M. M., Prestoza, M. O., Siebart, J., & Castelli, G. (2019). Outcomes in an interdisciplinary diabetes clinic in rural primary care. Southern Medical Journal, 112(4), 205. https://doi.org/10.14423/smj.0000000000000960
Kohli, N., Hughes, J., Wang, C., Zopluoglu, C., & Davison, M. L. (2015). Fitting a linear–linear piecewise growth mixture model with unknown knots: A comparison of two common approaches to inference. Psychological Methods, 20(2), 259. https://doi.org/10.1037/met0000034
Leichter, S. B., Dreelin, E., & Moore, S. (2004). Integration of clinical psychology in the comprehensive diabetes care team. Clinical Diabetes, 22(3), 129–131. https://doi.org/10.2337/diaclin.22.3.129
Matheson, F. I., Smith, K. L. W., Fasil, G. S., Moineddin, R., Dunn, J. R., & Glazier, R. H. (2014). Physical health and gender as risk factors for usage of services for mental illness. Journal of Epidemiology and Community Health, 68(10), 971–978. https://doi.org/10.1136/jech-2014-203844
Miller, W. R., & Rollnick, S. (2013). Motivational interviewing: Helping people change (3rd ed.). The Guilford Press.
Nansel, T. R., Iannotti, R. J., & Liu, A. (2012). Clinic-integrated behavioral intervention for families of youth with type 1 diabetes: Randomized clinical trial. Pediatrics, 129(4), e866–e873. https://doi.org/10.1542/peds.2011-2858
Peek, C. J., & The National Integration Academy Council. (2013). Lexicon for behavioral health and primary care integration: Concepts and definitions developed by expert consensus. AHRQ Publication No.13-IP001-EF. Rockville, MD: Agency for Healthcare Research and Quality. Retrieved on May 30,2021 from http://integrationacademy.ahrq.gov/sites/default/files/Lexicon.pdf
Prahalad, P., Zaharieva, D. P., Addala, A., New, C., Scheinker, D., Desai, M., Hood, K. K., & Maahs, D. M. (2020). Improving clinical outcomes in newly diagnosed pediatric type 1 diabetes: Teamwork, targets, technology, and tight control—the 4T study. Frontiers in Endocrinology. https://doi.org/10.3389/fendo.2020.00360
Renn, B. N., Feliciano, L., & Segal, D. L. (2011). The bidirectional relationship of depression and diabetes: A systematic review. Clinical Psychology Review, 31(8), 1239–1246. https://doi.org/10.1016/j.cpr.2011.08.001
Steed, L., Cooke, D., & Newman, S. (2003). A systematic review of psychosocial outcomes following education, self-management and psychological interventions in diabetes mellitus. Patient Education and Counseling, 51(1), 5–15. https://doi.org/10.1016/s0738-3991(02)00213-6
Substance Abuse and Mental Health Services Administration. (2017). SAMSHA-HRSA Center for Integrated Health Solutions. Retrieved on May 31, 2021 from https://www.samhsa.gov/integrated-health-solutions
Uchendu, C., & Blake, H. (2017). Effectiveness of cognitive-behavioural therapy on glycaemic control and psychological outcomes in adults with diabetes mellitus: A systematic review and meta-analysis of randomized controlled trials. Diabetic Medicine, 34(3), 328–339. https://doi.org/10.1111/dme.13195
Viana, L. V., Gomes, M. B., Zajdenverg, L., Pavin, E. J., Azevedo, M. J., & Brazilian Type 1 Diabetes Study Group. (2016). Interventions to improve patients’ compliance with therapies aimed at lowering glycated hemoglobin (HbA1c) in type 1 diabetes: Systematic review and meta-analyses of randomized controlled clinical trials of psychological, telecare, and educational interventions. Trials, 17(1), 94. https://doi.org/10.1186/s13063-016-1207-6
Vijayaraghavan, M., Jacobs, E. A., Seligman, H., & Fernandez, A. (2011). The association between housing instability, food insecurity, and diabetes self-efficacy in low income adults. Journal of Healthcare for the Poor and Underserved, 22(4), 1279–1291. https://doi.org/10.1353/hpu.2011.0131
West, D. S., Coulon, S. M., Monroe, C. M., & Wilson, D. K. (2016). Evidence-based lifestyle interventions for obesity and Type 2 diabetes: The look AHEAD intensive lifestyle intervention as exemplar. American Psychologist, 71(7), 614. https://doi.org/10.1037/a0040394
Wild, D., von Maltzahn, R., Brohan, E., Christensen, T., Clauson, P., & Gonder-Frederick, L. (2007). A critical review of the literature on fear of hypoglycemia in diabetes: Implications for diabetes management and patient education. Patient Education and Counseling, 68(1), 10–15. https://doi.org/10.1016/j.pec.2007.05.003
Young-Hyman, D., De Groot, M., Hill-Briggs, F., Gonzalez, J. S., Hood, K., & Peyrot, M. (2016). Psychosocial care for people with diabetes: A position statement of the American Diabetes Association. Diabetes Care, 39(12), 2126–2140. https://doi.org/10.2337/dc16-2053
Funding
Not Applicable.
Author information
Authors and Affiliations
Contributions
KLM conceptualized, wrote, and edited the manuscript; KSD analyzed the data and wrote/edited the manuscript; SAB-M conceptualized the study and edited the manuscript; AGD prepared and analyzed the data and edited the manuscript; MJT conceptualized the study and edited the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
Kristin L. MacGregor, Kelly S. DeMartini, Samantha A. Barry-Menkhaus, Alan G. Derr, and Michael J. Thompson declare that they have no conflict of interest.
Ethical Approval
This research study was conducted retrospectively from data obtained for clinical purposes. We consulted extensively with the IRB of UMass Medical School who determined that our study did not need ethical approval. An IRB official waiver of ethical approval was granted from the IRB of UMass Medical School.
Human and Animal Rights
This retrospective chart review study involving human participants was in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The Institutional Review Board approved this study.
Informed Consent
Not applicable as this was a retrospective chart review study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
MacGregor, K.L., DeMartini, K.S., Barry-Menkhaus, S.A. et al. The Impact of Integrated Behavioral Healthcare on Glycemic Control. J Clin Psychol Med Settings 29, 636–644 (2022). https://doi.org/10.1007/s10880-021-09817-w
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10880-021-09817-w