Abstract
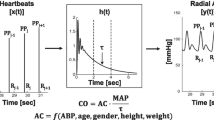
Objective. Three of the us developed a new non-invasive continuous cardiac output (CCO) measurement method utilizing routine clinical monitors based on the pulse-contour analysis combined with pulse wave transit time (PWTT). Using pulmonary artery catheter (CCOpa), we compared this estimated CCO (esCO) with the thermodilution CCO early after cardiac surgery, and tested whether the esCO method has potential of being an alternative measure of CCO. Methods. Thirty-six patients without continued arrhythmias were studied. esCO was computed using electrocardiogram (ECG) monitor, arterial pressure monitor and pulse-oximetry system. Both sets of data (esCO and CCOpa), by averaging the results of the preceding 10 min, were compared at 30-min intervals throughout the 15.8± 3.3 h (S.D.) of study. Bland–Altman plots and correlation analysis were used for statistical comparison. Results. A total of 981 paired sets of data (89.9%) among 1093 measurements were compared in the absence of displacement of either pulse-oximetry or ECG probes and/or inaccurate detection of R wave. The difference between esCO and CCOpa results was −0.06 ± 0.82 L/min (S.D.), and there was a linear correlation between them (r = 0.80, p < 0.0001). The difference between them was 0.00± 0.48 L/min at the first 1 h, which remained unchanged throughout 20 h after the start of measurement. Conclusions. The results demonstrate that esCO has a close correlation with the CCOpa, even though the two methods are not interchangeable. The results suggest that esCO method has potential of being an alternative non-invasive cardiac output trend, unless there are apparent arrhythmias.
Article PDF
Similar content being viewed by others
References
Kouchoukos NT, Sheppard LC, McDonald DA. Estimation of stroke volume in the dog by a pulse contour method. Cir Res 1970; 26: 611–623.
Ochiai R, Takeda J, Hosaka H, Sugo Y, Tanaka R, Soma T. The relationship between modified pulse wave transit time and cardiovascular changes in isoflurane anesthetized dogs. J Clin Monit Comput 1999; 15: 493–501.
Balik M, Pachl J, Hendl J. Effect of the degree of tricuspid regurgitation on cardiac output measurements by thermodilution. Intensive Care Med 2002; 28: 1117–1121.
Yelderman ML, Ramsay MA, Quinn MD, Paulsen AW, McKown, RC, Gillman PH. Continuous thermodilution cardiac output measurement in intensive care unit patients. J Cardiothorac Vasc Anesth 1992; 6: 270–274.
Siegel LC, Hennessy MM, Pearl RG. Delayed time response of the continuous cardiac output pulmonary artery catheter. Anesth Analg 1996; 83: 1173–77.
Lazor MA, Pierce ET, Stanley GD, Cass JL, Halpern EF, Bode RH. Evaluation of the accuracy and response time of Stat-Mode continuous cardiac output. J Cardiothorac Vasc Anesth 1997; 11: 432–436.
Della Rocca G, Costa MG, Pompei L, Coccia C, Pietropaoli P. Continuous and intermittent cardiac output measurement: Pulmonary artery catheter versus aortic transpulmonary technique. Br J Anaesth 2002; 88: 350–356.
Felbinger TW, Reuter DA, Eltzschig HK, Moerstedt K, Gædje O, Goetz AE. Comparison of pulmonary arterial thermodilution and arterial pulse contour analysis: Evaluation of a new algorithm. J Clin Anesth 2002; 14: 296–301.
Zöllner C, Goetz AE, Weis M, Moerstedt K, Pichler B, Lamm P, Kilger E, Haller M. Continuous cardiac output measurements do not agree with conventional bolus thermodilution cardiac output determination. Can J Anesth 2001; 48: 1143–1147.
Le Tulzo Y, Belghith M, Seguin P, Dall’Ava J, Monchi M, Thomas R, Dhainaut JF. Reproducibility of thermodilution cardiac output determination in critically ill patients: Comparison between bolus and continuous method. J Clin Monit 1996; 12: 379–385.
Schmid ER, Schmidlin D, Tornic M, Seifert B. Continuous thermodilution cardiac output: Clinical validation against a reference technique of known accuracy. Intensive Care Med 1999; 25: 166–172.
Yelderman M. Continuous measurement of cardiac output with the use of stochastic system identification techniques. J Clin Monit 1990; 6: 322–332.
Aranda M, Mihm FG, Garrett S, Mihm MN, Pearl RG. Continuous cardiac output catheters. Delay in in vitro response time after controlled flow changes. Anesthesiology 1998; 89: 1592–1955.
Irlbeck M, Forst H, Briegel J, Haller M, Peter K. Continuous measurement of cardiac output with pulse contour analysis. Anaesthesist 1995; 42: 972–976.
Rödig G, Prasser C, Keyl C, Liebold A, Hobbhahn, J. Continuous cardiac output measurement: pulse contour analysis vs. thermodilution technique in cardiac surgical patients. Br J Anaesth 1999; 82: 525–530.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ishihara, H., Okawa, H., Tanabe, K. et al. A New Non-Invasive Continuous Cardiac Output Trend Solely Utilizing Routine Cardiovascular Monitors. J Clin Monit Comput 18, 313–320 (2004). https://doi.org/10.1007/s10877-005-2452-5
Received:
Revised:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/s10877-005-2452-5