Abstract
Introduction
Argentina has a large number of patients with definite diagnosis of X-linked agammaglobulinemia reported in the Latin-American registry. Forty-nine of them were seen in our referral pediatric hospital, between 1987 and 2005.
Results and Discussion
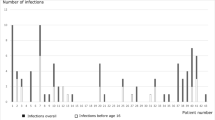
A retrospective study of clinical, laboratory, and molecular data showed that respiratory tract infections were the most frequent initial clinical presentation and the most common among all manifestations prior to diagnosis (69%). Up to diagnosis, we found a high frequency of severe infections (sepsis, 14% and meningitis, 16%) and a high proportion of patients with chronic lung disease. During follow-up, the development of chronic lung disease was significantly related with age at diagnosis and inappropriate treatment.
Conclusion
Although molecular diagnosis has been available in our center for the past 10 years, there is no doubt that awareness for early recognition of immunodeficiency should be improved through broader and more comprehensive education programs emphasizing characteristics of patients with immunodeficiencies.
Similar content being viewed by others
References
Nomura K, Kanegane H, Karasuyama H, Tsukada S, Agematsu K, Murakami G, et al. Genetic defect in human X-linked agammaglobulinemia impedes a maturational evolution of pro-B cells into a latter stage of pre-B cells in the B-cell differentiation pathway. Blood 2000;96:610–7.
Noordzij JG, de Bruin-Versteeg S, Comans-Bitter WM, Hartwig NG, Hendriks RW, de Groot R, et al. Composition of precursor B-cell compartment in bone marrow from patients with X-linked agammaglobulinemia compared with healthy children. Pediatr Res 2002;51:159–68. doi:10.1203/00006450-200202000-00007.
Tsukada S, Saffran DC, Rawlings DJ, Parolini O, Allen RC, Klisak I, Sparkers RS, Kubagawa H, Mohandas T, Quan S, Belmont JW, Cooper MD, Conley ME, Witte ON. Deficient expression of a B cell cytoplasmic tyrosine kinase in human X-linked agammaglobulinemia. Cell 1993;72:279–90. doi:10.1016/0092-8674(93)90667-F.
Vetrie D, Vorechovsky I, Sideras P, Holland J, Davies A, Flinter F, et al. The gene involved in X-linked agammaglobulinemia is a member of the src family of protein tyrosine kinases. Nature 1993;361:226–33. doi:10.1038/361226a0.
Hermaszewski RA, Webster AD. Primary hypogammaglobulinaemia: a survey of clinical manifestations and complications. Q J Med 1993;86:31–42.
Quartier P, Debré M, De Blic J, de Sauverzac R, Sayegh N, Jabado N, et al. Early and prolonged intravenous immunoglobulin replacement therapy in childhood agammaglobulinemia: a retrospective survey of 31 patients. J Pediatr 1999;134:589–96. doi:10.1016/S0022-3476(99)70246-5.
Conley ME, Howard V. Clinical findings leading to the diagnosis of X-linked agammaglobulinemia. J Pediatr 2002;141:566–71. doi:10.1067/mpd.2002.127711.
Plebani A, Soresina A, Rondelli R, Amato GM, Azzari C, Cardinale F, et al. Italian Pediatric Group for XLA-AIEOP. Clinical, immunological, and molecular analysis in a large cohort of patients with X-linked agammaglobulinemia: an Italian multicenter study. Clin Immunol 2002;104:221–30. doi:10.1006/clim.2002.5241.
Moin M, Aghamohammadi A, Farhoudi A, Pourpak Z, Rezaei N, Movahedi M, et al. X-linked agammaglobulinemia: a survey of 33 Iranian patients. Immunol Invest 2004;33:81–93. doi:10.1081/IMM-120027687.
López-Granados E, Pérez de Diego R, Ferreira Cerdán A, Fontán Casariego G, García Rodríguez MC. A genotype–phenotype correlation study in a group of 54 patients with X-linked agammaglobulinemia. J Allergy Clin Immunol 2005;116:690–7. doi:10.1016/j.jaci.2005.04.043.
Winkelstein JA, Marino MC, Lederman HM, Jones SM, Sullivan K, Burks AW, et al. X-linked agammaglobulinemia: report on a United States registry of 201 patients. Medicine (Baltimore) 2006;85:193–202. doi:10.1097/01.md.0000229482.27398.ad.
Leiva LE, Zelazco M, Oleastro M, Carneiro-Sampaio M, Condino-Neto A, Costa-Carvalho BT, Latin American Group for Primary Immunodeficiency Diseases, et al. Primary immunodeficiency diseases in Latin America: the second report of the LAGID registry. J Clin Immunol 2007;27:101–8. doi:10.1007/s10875-006-9052-0.
Ryser O, Morell A, Hitzig WH. Primary immunodeficiencies in Switzerland: first report of the national registry in adults and children. J Clin Immunol 1988;8:479–85. doi:10.1007/BF00916954.
Matamoros Florí N, Mila Llambi J, Español Boren T, Raga Borja S, Fontan Casariego G. Primary immunodeficiency syndrome in Spain: first report of the National Registry in Children and Adults. J Clin Immunol 1997;17:333–9. doi:10.1023/A:1027382916924.
Danielian S, El-Hakeh J, Basílico G, Oleastro M, Rosenzweig S, Feldman G, et al. Bruton tyrosine kinase gene mutations in Argentina. Hum Mutat 2003;21:451–6. doi:10.1002/humu.9131.
Lindvall JM, Blomberg KE, Väliaho J, Vargas L, Heinonen JE, Berglöf A, et al. Bruton’s tyrosine kinase: cell biology, sequence conservation, mutation spectrum, siRNA modifications, and expression profiling. Immunol Rev 2005;203:200–15. doi:10.1111/j.0105-2896.2005.00225.x.
Stiehm ER, Fudenberg HH. Serum levels of immune globulins in health and disease: a survey. Pediatrics 1966;37:715–27.
Author information
Authors and Affiliations
Corresponding author
Additional information
Natalia Basile and Silvia Danielian contributed equally to this work
Rights and permissions
About this article
Cite this article
Basile, N., Danielian, S., Oleastro, M. et al. Clinical and Molecular Analysis of 49 Patients With X-linked Agammaglobulinemia From A Single Center in Argentina. J Clin Immunol 29, 123–129 (2009). https://doi.org/10.1007/s10875-008-9227-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10875-008-9227-y