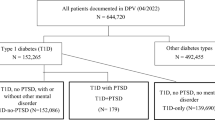
The purpose of this study was to assess the prevalence and correlates of comorbid diabetes and Post-Traumatic Stress disorder(PTSD)and potential relationships between PTSD and diabetes outcomes. Male patients enrolled in a VA primary care database (N = 73,270) were classified as having diabetes from pharmacy records (N = 14,438) and grouped into those with diagnoses of PTSD with depression (N = 649), PTSD-only (N = 480), Depression-only (N = 1696), Other psychiatric diagnosis (N = 736), or No psychiatric diagnosis (N = 10,877) based on the Purpose of Visit diagnoses in the medical record. Outcomes included glycemic control (HbA1c), cholesterol and tryglycerides. Correlates were age, substance use disorder, other psychiatric diagnosis, number of primary care encounters, and medications. The prevalence of comorbid diabetes and PTSD was 8% (n = 1129). Of these, 57% (n = 649) had comorbid depression. Patients with PTSD and depression had higher rates of substance use disorder and higher cholesterol and LDL. Patients with depression had poorer glycemic control. Patients with PTSD and depression weighed more and had higher BMI than patients with neither diagnosis. Thus, male diabetes patients with PTSD and depression may be vulnerable to substance use disorders and to weight/lipid problems that can affect health. Depression is a likely contributor to poor glycemic control. Careful screening for mental health comorbidities is needed for diabetes patients.
Similar content being viewed by others
References
Anderson, R. J., Freedland, K. E., Clouse, R. E., and Lustman, P. J. (2001). The prevalence of comorbid depression in adults with diabetes: A meta-analysis. Diabetes Care 24: 1069–1078.
Anderson, R. J., Grigsby, A. B., Freedland, K. E., de Groot, M., McGill, J. B., Clouse, R. E., and Lustman, P. J. (2002). Anxiety and poor glycemic control: A meta-analytic review of the literature. Int. J. Psychiatry Med. 32: 235–247.
Baker, D. G., Mendenhall, C. L., Simbartl, L. A., Magan, L. K., and Steinberg, J. L. (1997). Relationship between posttraumatic stress disorder and self-reported physical symptoms in Persian Gulf War veterans. Arch. Intern. Med. 157: 2076–2078.
Beckham, J. C., Moore, S. D., Feldman, M. E., Hertzberg, M. A., Kirby, A. C., and Fairbank, J. A. (1998). Health status, somatization and severity of posttraumatic stress disorder in Vietnam combat veterans with posttraumatic stress disorder. Am. J. Psychiatry 155: 1565–1569.
Boscarino, J. A. (2004). Posttraumatic stress disorder and physical illness: Results from clinical and epidemiologic studies. In Yehuda, R., and McEwen, B., (Eds.), (Biobehavioral Stress Response: Protective and Damaging Effects. Annals of the New York Academy of Sciences (vol. 1032, pp. 141–153). New York, NY.
Carnethon, M. R., Kinder, L. S., Fair, J. M., Stafford, R. S., and Fortmann, S. P. (2003). Symptoms of depression as a risk factor of incident diabetes: Findings from the National Health and Nutrition Examination Epidemiologic Follow-up Study, 1971–1992. Am. J. Epidemiol. 158: 416–423.
Centers for Disease Control Vietnam Experience Study (1988). Health status of Vietnam veterans: I. Psychosocial characteristics. JAMA 259: 2701–2707.
Clouse, R. E., Lustman, P. J., Freedland, K. E., Griffith, L. S., McGill, J. B., and Carney, R. M. (2003). Depression and coronary heart disease in women with diabetes. Psychosom. Med. 65: 376–383.
Davidson, J. R. T., Hughes, D., Blazer, D. G., and George, L. K. (1991). Posttraumatic stress disorder in the community: An epidemiological study. Psychol. Med. 21: 713–721.
DeGroot, M., Anderson, R. J., Freedland, K. E., Clouse, R. E., and Lustman, P. J. (2001). Association of depression and diabetes complications: A meta-analysis. Psychosom. Med. 63: 619–630.
Egede, L. E., Nietert, P. J., and Zheng, D. (2005). Depression and all-cause and coronary heart disease mortality among adults with and without diabetes. Diabetes Care 28: 1339–1345.
Fairbank, J. A., Schlenger, W. E., Saigh, P. A., and Davidson, J. R. T. (1995). An epidemiologic profile of post-traumatic stress disorder: Prevalence, comorbidity, and risk factors. In Friedman, M. J., Charney, D. S., and Deutch, A. Y. (Eds.), Neurobiological and Clinical Consequences of Stress; From Normal Adaptation to PTSD (pp. 415–427). Lippincott-Raven, Philadelphia, PA.
Frayne, S. M., Halanych, J. H., Miller, D. R., Wang, F., Lin, H., Pogach, L., Sharansky, E. J., Keane, T. M., Skinner, K. M., Rosen, C. S., and Berkowitz, D. R. (2005). Disparities in diabetes care: Impact of mental illness. Arch. Intern. Med. 165: 2631–2638.
Frayne, S. M., Seaver, M. R., Loveland, S., Christiansen, C. L., Spiro, A. 3rd, Parker, V. A., and Skinner, K. M. (2004). Burden of medical illness in women with depression and posttraumatic stress disorder. Arch. Intern. Med. 164: 1306–1312.
Friedman, M. J., and Schnurr, P. P. (1995). The relationship between trauma, post-traumatic stress disorder, and physical health. In Friedman, M. J., Charney, D. S., and Deutsch, A. Y. (Eds.), Neurobiological and Clinical Consequences of Stress: From Normal Adaptation to PTSD (pp. 507–524). Lippincott-Raven Pub, Philadelphia, PA.
Goodwin, R. D., and Davidson, J. R. (2005). Self-reported diabetes and posttraumatic stress disorder among adults in the community. Prev. Med. 40: 570–574.
Haas, L. B. and Watts, S. A. (2005). Diabetes care in the Veterans Health Administration. Diabetes Spectr 18: 159–162.
Hoge, C. W., Castro, C. A., Messer, S. C., McGurk, D., Cotting, D. I., and Koffman, R. L. (2004). Combat duty in Iraq and Afghanistan, mental health problems, and barriers to care. N. Engl. J. Med. 351: 13–22.
Ironson, G., Wynings, C., Schneiderman, N., Baum, A., Rodriguez, M., Greenwood, D., Benight, C., Antoni, M., LaPerriere, A., Huang, H. S., Klimas, H. S., and Fletcher, M. A. (1997). Posttraumatic stress symptoms, intrusive thoughts, loss, and immune function after Hurricane Andrew. Psychosom Med. 59: 128–141.
Kang, H. K., Natelson, B. H., Mahan, C. M., Lee, K.Y., and Murphy, F. M. (2003). Post-traumatic stress disorder and chronic fatigue syndrome-like illness among Gulf War veterans: A population-base survey of 30,000 veterans. Am. J. Epidemiol. 157: 141–148.
Kang, H. K. and Hyams, K. C. (2005). Mental health care needs among recent war veterans. N. Engl. J. Med. 352: 1289.
Kessler, R. C., Sonnega, A., Bromet, E., Hughes, M., and Nelson, C. B. (1995). Posttraumatic stress disorder in the National Comorbidity Survey. Arch. Gen. Psychiatry 52: 1048–1060.
Kulka, R. A., Schlenger, W. E., Fairbank, J. A., and Weiss, D. (1990). Trauma and the Vietnam War Generation: Report of Findings from the National Vietnam Veterans Readjustment Study. Brunner/Mazel, New York.
Lin, E. H. B., Katon, W., VonKorff, M., Rutter, C., Simon, G. E., Oliver, M.. Ciechanowski, P., Ludman, E.J., Bush, T., and Young, B. (2004). Relationship of depression and diabetes self-care, medication adherence and preventive care. Diabetes Care 27: 2154–2160.
Lustman, P. J., Anderson, R. J., Freedland, K. E., DeGroot, M. K., Carney, R. M., and Clouse, R. E.(2000). Depression and poor glycemic control: A meta-analytic review of the literature. Diabetes Care 23: 934–942.
Musselman, D. L., Betan, E., Larsen, H., and Phillips, L. S. (2003). Relationship of depression to diabetes types 1 and 2: Epidemiology, biology, and treatment. Biol. Psychiatry 54: 317–329.
Ouimette, P., Cronkite, R., Henson, B. R., Prins, A., Gima, K., and Moos, R. H. (2004). Posttraumatic stress disorder and health status among female and male medical patients. J. Trauma. Stress 17: 1–9.
Peyrot, M. and Rubin, R. R. (1997). Levels and risks of depression and anxiety symptomatology among diabetic adults. Diabetes Care 20: 585–590.
Resnick, H. S., Kilpatrick, D. G., Dansky, B. S., Saunders, B. E., and Bedst, C. L. (1993). Prevalence of civilian trauma and posttraumatic stress disorder in a representative national sample of women. J. Consult. Clin. Psychol. 61: 984–991.
Rosenbaum, P. R. and Rubin, D. B. (1983). The central role of the propensity score in observational studies for causal effects. Biometrica 70: 41–55.
Schnurr, P. P., Ford, J. D., Friedman, M. J., Green, B. L., Dain, B. J., and Sengupta, A. (2000). Predictors and outcomes of posttraumatic stress disorder in World War II veterans exposed to mustard gas. J. Consult. Clin. Psychol. 68: 258–268.
Schnurr, P. P. and Jankowski, M. K. (1999). Physical health and post-traumatic stress disorder: Review and synthesis. Semin. Clin. Neuropsychiatry 4: 295–304.
Solomon, Z. (1988). Somatic complaints, stress reaction, and posttraumatic stress disorder: A three-year follow-up study. Behav. Med. 14: 179–185.
Sullivan, G. M. and Gorman, J. M. (2002). Finding a home for post-traumatic stress disorder in biological psychiatry. Is it a disorder of anxiety, mood, stress, or memory? Psychiatr. Clin. N. Am. 25: 463–468.
Thomas, J., Jones, G., Scarinci, I., and Brantley, P. (2003). A descriptive and comparative study of the prevalence of depressive and anxiety disorders in low-income adults with type 2 diabetes and other chronic illnesses. Diabetes Care 26: 2311–2317.
Weisberg, R. B., Bruce, S. E., Machan, J. T., Kessler, R. C., Culpepper, L., and Keller, M. B. (2002). Nonpsychiatric illness among primary care patients with trauma histories and posttraumatic stress disorder. Psychiatr. Serv. 53: 848–854.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Trief, P.M., Ouimette, P., Wade, M. et al. Post-traumatic Stress Disorder and Diabetes: Co-Morbidity and Outcomes in a Male Veterans Sample. J Behav Med 29, 411–418 (2006). https://doi.org/10.1007/s10865-006-9067-2
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10865-006-9067-2