Abstract
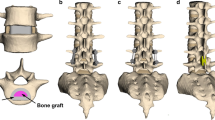
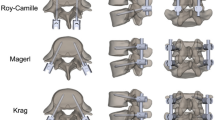
The use of a pedicle screw fixation system with rods made of more compliant materials has become increasingly popular for spine fusion surgery in recent years. The aim of this study was to compare stress responses of the implants in transforaminal lumbar interbody fusion (TLIF) when using flexible and conventional rigid posterior fixation systems. A previously validated intact L1–S1 finite element model was modified to simulate single-level (L4–L5) TLIF with bilateral pedicle screw fixation using two types of connecting rod (rigid and flexible rods). The von Mises stresses in the implants (including TLIF cage, pedicle screws and rods) for the rigid and flexible fixations were analyzed under static and vibration loadings. The results showed that compared with the rigid fixation, the use of flexible fixation decreased the maximum stress in the pedicle screws, but increased the maximum stress in the cage and the ratio of maximum stress in the rods to the yield stress. It was also found that with decreasing diameter of the flexible rod (i.e. increasing flexibility of the rod), the maximum stress was decreased in the pedicle screws but increased in the cage and the rods. The findings imply that compared with the rigid rod, application of the flexible rod in the pedicle screw fixation system for the TLIF might decrease the breakage risk of pedicle screws but increase the risk of cage subsidence and rod breakage. Moreover, flexibility of the rod in the flexible fixation system should be carefully determined.











Similar content being viewed by others
References
Hackenberg L, Halm H, Bullmann V, Vieth V, Schneider M, Liljenqvist U. Transforaminal lumbar interbody fusion: a safe technique with satisfactory three to five year results. Eur Spine J. 2005;14:551–8.
Deng QX, Ou YS, Zhu Y, Zhao ZH, Liu B, Huang Q, et al. Clinical outcomes of two types of cages used in transforaminal lumbar interbody fusion for the treatment of degenerative lumbar diseases: n-HA/PA66 cages versus PEEK cages. J Mater Sci Mater Med. 2016;27:102.
Ambati DV, Wright EK, Lehman RA, Kang DG, Wagner SC, Dmitriev AE. Bilateral pedicle screw fixation provides superior biomechanical stability in transforaminal lumbar interbody fusion: a finite element study. Spine J. 2015;15:1812–22.
Cao YW, Liu FB, Wan SC, Liang Y, Jiang C, Feng ZZ, et al. Biomechanical evaluation of different surgical procedures in single-level transforaminal lumbar interbody fusion in vitro. Clin Biomech. 2017;49:91–5.
Harris BM, Hilibrand AS, Savas PE, Pellegrino A, Vaccaro AR, Siegler S, et al. Transforaminal lumbar interbody fusion-The effect of various instrumentation techniques on the flexibility of the lumbar spine. Spine. 2004;29:E65–70.
Niemeyer TK, Koriller M, Claes L, Kettler A, Werner K, Wilke HJ. In vitro study of biomechanical behavior of anterior and transforaminal lumbar interbody instrumentation techniques. Neurosurgery. 2006;59:1271–6.
Kang KT, Kim HJ, Son J, Yeom JS, Chun HJ. Comparing an instrumented posterior fixation system with rigid and semi-flexible rods using finite element analysis. Int J Precis Eng Manuf. 2015;16:163–70.
Cripton PA, Jain GM, Wittenberg RH, Nolte LP. Load-sharing characteristics of stabilized lumbar spine segments. Spine. 2000;25:170–9.
Jacobs E, Roth AK, Arts JJ, van Rhijn LW, Willems PC. Reduction of intradiscal pressure by the use of polycarbonate-urethane rods as compared to titanium rods in posterior thoracolumbar spinal fixation. J Mater Sci Mater Med. 2017;28:148.
Chen CS, Huang CH, Shih SL. Biomechanical evaluation of a new pedicle screw-based posterior dynamic stabilization device (Awesome Rod System)-finite element analysis. BMC Musculoskelet Disord. 2015;16:81.
Le Cann S, Chaves-Jacob J, Rossi JM, Linares JM, Chabrand P. Tribology of flexible and sliding spinal implants: development of experimental and numerical models. J Biomed Mater Res B Appl Biomater. 2018;106(l):104–11.
Rohlmann A, Nabil Boustani H, Bergmann G, Zander T. Effect of a pedicle-screw-based motion preservation system on lumbar spine biomechanics: a probabilistic finite element study with subsequent sensitivity analysis. J Biomech. 2010;43:2963–9.
Onen MR, Basgul C, Yilmaz I, Ozkaya M, Demir T, Naderi S. Comparison of rigid and semi-rigid instrumentation under acute load on vertebrae treated with posterior lumbar interbody fusion/transforaminal lumbar interbody fusion procedures: an experimental study. Proc Inst Mech Eng H. 2018;232:388–94.
Ahn YH, Chen WM, Lee KY, Park KW, Lee SJ. Comparison of the load-sharing characteristics between pedicle-based dynamic and rigid rod devices. Biomed Mater. 2008;3:044101.
Kim K, Park WM, Kim YH, Lee S. Stress analysis in a pedicle screw fixation system with flexible rods in the lumbar spine. Proc Inst Mech Eng H. 2010;224:477–85.
Kang KT, Koh YG, Son J, Yeom JS, Park JH, Kim HJ. Biomechanical evaluation of pedicle screw fixation system in spinal adjacent levels using polyetheretherketone, carbon-fiber-reinforced polyetheretherketone, and traditional titanium as rod materials. Compos Part B-Eng. 2017;130:248–56.
Kim YS, Zhang HY, Moon BJ, Park KW, Ji KY, Lee WC, et al. Nitinol spring rod dynamic stabilization system and Nitinol memory loops in surgical treatment for lumbar disc disorders: short-term follow up. Neurosurg Focus. 2007;22:E10.
Li C, Liu L, Shi JY, Yan KZ, Shen WZ, Yang ZR. Clinical and biomechanical researches of polyetheretherketone (PEEK) rods for semi-rigid lumbar fusion: a systematic review. Neurosurg Rev. 2018;41:375–89.
Putzier M, Hoff E, Tohtz S, Gross C, Perka C, Strube P. Dynamic stabilization adjacent to single-level fusion: Part II. No clinical benefit for asymptomatic, initially degenerated adjacent segments after 6 years follow-up. Eur Spine. J 2010;19:2181–9.
Fan W, Guo LX. Influence of different frequencies of axial cyclic loading on time-domain vibration response of the lumbar spine: a finite element study. Comput Biol Med. 2017;86:75–81.
Guo LX, Fan W. Dynamic response of the lumbar spine to whole-body vibration under a compressive follower preload. Spine. 2018;43:E143–53.
Fan W, Guo LX. A comparison of the influence of three different lumbarinterbody fusion approaches on stress in the pedicle screwfixation system: finite element static and vibration analyses. Int J Numer Method Biomed Eng. 2019;35:e3162.
Lee CH, Kim YE, Lee HJ, Kim DG, Kim CH. Biomechanical effects of hybrid stabilization on the risk of proximal adjacent-segment degeneration following lumbar spinal fusion using an interspinous device or a pedicle screw-based dynamic fixator. J Neurosurg Spine. 2017;27:643–9.
Jahng TA, Kim YE, Moon KY. Comparison of the biomechanical effect of pedicle-based dynamic stabilization: a study using finite element analysis. Spine J. 2013;13:85–94.
McAfee PC, Weiland DJ, Carlow JJ. Survivorship analysis of pedicle spinal instrumentation. Spine. 1991;16:S422–7.
McLain RF, Sparling E, Benson DR. Early failure of short-segment pedicle instrumentation for thoracolumbar fractures. J Bone Jt Surg Am. 1993;75:162–7.
Oktenoglu T, Erbulut DU, Kiapour A, Ozer AF, Lazoglu I, Kaner T, et al. Pedicle screw-based posterior dynamic stabilisation of the lumbar spine: in vitro cadaver investigation and a finite element study. Comput Methods Biomech Biomed Engin. 2015;18:1252–61.
Schmoelz W, Huber JF, Nydegger T, Dipl-Ing, Claes L, Wilke HJ. Dynamic stabilization of the lumbar spine and its effects on adjacent segments: an in vitro experiment. J Spinal Disord Tech. 2003;16:418–23.
Mummaneni PV, Haid RW, Rodts GE. Lumbar interbody fusion: state-of-the-art technical advances. Invited submission from the Joint Section Meeting on Disorders of the Spine and Peripheral Nerves, March 2004. J Neurosurg. Spine 2004;1:24–30.
Galbusera F, Schmidt H, Wilke HJ. Lumbar interbody fusion: a parametric investigation of a novel cage design with and without posterior instrumentation. Eur Spine J. 2012;21:455–62.
Zhang M, Pu F, Xu LQ, Zhang LL, Yao J, Li DY, et al. Long-term effects of placing one or two cages in instrumented posterior lumbar interbody fusion. Int Orthop. 2016;40:1239–46.
Wade KR, Schollum ML, Robertson PA, Thambyah A, Broom ND. ISSLS Prize Winner: vibration really does disrupt the disc: a microanatomical investigation. Spine. 2016;41:1185–98.
Zeeman ME, Kartha S, Winkelstein BA. Whole-body vibration induces pain and lumbar spinal inflammation responses in the rat that vary with the vibration profile. J Orthop Res. 2016;34:1439–46.
Goel VK, Park H, Kong WZ. Investigation of vibration characteristics of the ligamentous lumbar spine using the finite element approach. J Biomech Eng. 1994;116:377–83.
Wilder DG. On the loading of the human lumbar intervertebral motion segment. Ph.D. Thesis. Burlington, Vermont: University of Vermont; 1985.
Cunningham BW, Sefter JC, Shono Y, McAfee PC. Static and cyclical biomechanical analysis of pedicle screw spinal constructs. Spine. 1993;18:1677–88.
Wittenberg RH, Shea M, Edwards WT, Swartz DE, White AA III, Hayes WC. A biomechanical study of the fatigue characteristics of thoracolumbar fixation implants in a calf spine model. Spine. 1992;17:S121–8.
Pearson HB, Dobbs CJ, Grantham E, Niebur GL, Chappuis JL, Boerckel JD. Intraoperative biomechanics of lumbar pedicle screw loosening following successful arthrodesis. J Orthop Res. 2017;35:2673–81.
Bagby GW. Arthrodesis by the distraction-compression method using a stainless steel implant. Orthopedics. 1988;11:931–4.
Acknowledgements
This work was supported by the Fundamental Research Funds for the Central Universities (N180303030) and the National Natural Science Foundation of China (51875096).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Fan, W., Guo, LX. & Zhao, D. Stress analysis of the implants in transforaminal lumbar interbody fusion under static and vibration loadings: a comparison between pedicle screw fixation system with rigid and flexible rods. J Mater Sci: Mater Med 30, 118 (2019). https://doi.org/10.1007/s10856-019-6320-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10856-019-6320-0