Abstract
Recently, chronic osteomyelitis is still a challenging surgical problem. Unfortunately, the traditional clinical method using bone cement loaded antibiotics is restricted due to its non-biodegradability and limited release of antibiotics. Hydroxyapatite is a good adsorbent with good biocompatibility, an ideal bone repair material, and can avert the requirement for the secondary surgical procedure of removal. In this study, nano-hydroxyapatite combined with a polyurethane containing 3% silver (Ag/n-HA/PU) was synthesized, and investigated for its efficacy of treating chronic bone infection with bone defects. To clarify its silver ions release characteristics, the concentration of the Ag+ in the elution was analyzed every day after in vitro deionized water immersion. A chronic osteomyelitis of tibia in rabbit model was established, and 70 New Zealand rabbits were divided into 4 groups, including the blank control group, nano-hydroxyapatite combined with polyurethane (n-HA/PU) implant group, 3% Ag/n-HA/PU group and 10% Ag/n-HA/PU group after debridement. Routine blood tests, radiography, Micro-CT, and histological staining were conducted at 4 days, 3, 6 and 12 weeks post-treatment. The results showed that the released silver from the 3% Ag/n-HA/PU and 10% Ag/n-HA/PU exhibited an initial burst release and followed by a slow controlled release up to 39 days and 42 days respectively. A good repair of bone defects, an appropriate rate of degradation of scaffolds and no significant toxicity were observed in the 3% Ag/n-HA/PU group, indicating the advantages of this novel synthetic scaffold to be a potential option for the treatment of chronic osteomyelitis.

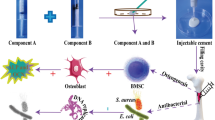
A novel nano-composite, nano-hydroxyapatite combined with a polyurethane containing 3% silver (Ag/n-HA/PU) provide controlled release of Ag+, illustrated by its abilities of biodegradation, antimicrobial activity, and favorable repair of bone defects in the treatment of chronic osteomyelitis.










Similar content being viewed by others
References
Walter G, Kemmerer M, Kappler C, Hoffmann R. Treatment algorithms for chronic osteomyelitis. Dtsch Arztebl Int. 2012;109:257–64.
Beck-Broichsitter BE, Smeets R, Heiland M. Current concepts in pathogenesis of acute and chronic osteomyelitis. Curr Opin Infect Dis. 2015;28:240–5.
Lew DP, Waldvogel FA. Osteomyelitis. Lancet. 2004;364:369–79.
Ellington JK, Harris M, Webb L, Smith B, Smith T, Tan K, et al. Intracellular Staphylococcus aureus: A mechanism for the indolence of osteomyelitis. J Bone Joint Surg Br. 2003;85:918–21.
Norden CW. Lessons learned from animal models of osteomyelitis. Rev Infect Dis. 1988;10:103–10.
Mader JT, Landon GC, Calhoun J. Antimicrobial treatment of osteomyelitis. Clin Orthop Relat Res. 1993;295:87–95.
Haidar R, Der Boghossian A, Atiyeh B. Duration of post-surgical antibiotics in chronic osteomyelitis: empiric or evidence-based? Int J Infect Dis. 2010;14:e752–8.
Inzana JA, Schwarz EM, Kates SL, Awad HA. Biomaterials approaches to treating implant-associated osteomyelitis. Biomaterials. 2016;81:58–71.
Dunne N, Hill J, McAfee P, Todd K, Kirkpatrick R, Tunney M, et al. In vitro study of the efficacy of acrylic bone cement loaded with supplementary amounts of gentamicin: effect on mechanical properties, antibiotic release, and biofilm formation. Acta Orthop. 2007;78:774–85.
Van De Belt H, Neut D, Schenk W, van Horn JR, van der Mei HC, Busscher HJ. Gentamicin release from polymethylmethacrylate bone cements and Staphylococcus aureus biofilm formation. Acta Orthop Scand. 2000;71:625–9.
Zalavras C, Patzakis M, Holtom P. Local antibiotic therapy in the treatment of open fractures and osteomyelitis. Clin Orthop Relat Res. 2004;427:86–93.
Giavaresi G, Bertazzoni Minelli E, Sartori M, Benini A, Della Bora T, Sambri V, et al. Microbiological and pharmacological tests on new antibiotic-loaded PMMA-based composites for the treatment of osteomyelitis. J Orthop Res. 2012;30:348–55.
Cheng H, Li Y, Huo K, Gao B, Xiong W. Long-lasting in vivo and in vitro antibacterial ability of nanostructured titania coating incorporated with silver nanoparticles. J Biomed Mater Res A. 2014;102:3488–99.
Percival SL, Bowler PG, Russell D. Bacterial resistance to silver in wound care. J Hosp Infect. 2005;60:1–7.
Becker RO, Spadaro JA. Treatment of orthopaedic infections with electrically generated silver ions. A preliminary report. J Bone Joint Surg Am. 1978;60:871–81.
Nand S, Sengar GK, Nand S, Jain VK, Gupta TD. Dual use of silver for management of chronic bone infections and infected non-unions. J Indian Med Assoc. 1996;94:91–5.
Mahltig B, Soltmann U, Haase H. Modification of algae with zinc, copper and silver ions for usage as natural composite for antibacterial applications. Mater Sci Eng C Mater Biol Appl. 2013;33:979–83.
Kolmas J, Groszyk E, Kwiatkowska-Różycka D. Substituted hydroxyapatites with antibacterial properties. Biomed Res Int. 2014;2014:178123.
Politano AD, Campbell KT, Rosenberger LH, Sawyer RG. Use of silver in the prevention and treatment of infections: silver review. Surg Infect (Larchmt). 2013;14:8–20.
Guelcher SA. Biodegradable polyurethanes: synthesis and applications in regenerative medicine. Tissue Eng Part B Rev. 2008;14:3–17.
Heo SJ, Kim SE, Wei J, Hyun YT, Yun HS, Kim DH, et al. Fabrication and characterization of novel nano- and micro-HA/PCL composite scaffolds using a modified rapid prototyping process. J Biomed Mater Res A. 2009;89:108–16.
Rau JV, Cacciotti I, Laureti S, Fosca M, Varvaro G, Latini A. Bioactive, nanostructured Si-substituted hydroxyapatite coatings on titanium prepared by pulsed laser deposition. J Biomed Mater Res B Appl Biomater. 2015;103:1621–31.
Bil M, Ryszkowska J, Woźniak P, Kurzydłowski KJ, Lewandowska-Szumieł M. Optimization of the structure of polyurethanes for bone tissue engineering applications. Acta Biomater. 2010;6:2501–10.
McBane JE, Sharifpoor S, Cai K, Labow RS, Santerre JP. Biodegradation and in vivo biocompatibility of a degradable, polar/hydrophobic/ionic polyurethane for tissue engineering applications. Biomaterials. 2011;32:6034–44.
Yang W, Both SK, Zuo Y, Birgani ZT, Habibovic P, Li Y, et al. Biological evaluation of porous aliphatic polyurethane/hydroxyapatite composite scaffolds for bone tissue engineering. J Biomed Mater Res A. 2015;103:2251–9.
Wang Q, Chen C, Liu W, He X, Zhou N, Zhang D, et al. Levofloxacin loaded mesoporous silica microspheres/nano-hydroxyapatite/polyurethane composite scaffold for the treatment of chronic osteomyelitis with bone defects. Sci Rep. 2017;7:41808.
Guo C, Li X, Dong Y. Preparation and characterization of silver/hydroxyapatite nanoparticles. Advanced Materials Research. 2011;311–3:1746–50.
Akiyama T, Miyamoto H, Yonekura Y, Tsukamoto M, Ando Y, Noda I, et al. Silver oxide-containing hydroxyapatite coating has in vivo antibacterial activity in the rat tibia. J Orthop Res. 2013;31:1195–200.
Oh KS, Kim KJ, Jeong YK, Choa YH. Effect of fabrication processes on the antimicrobial properties of silver doped nano-sized HAp. Key Engineering Materials. 2003;240–2:583–6.
Jiang J, Li L, Li K, Li G, You F, Zuo Y, et al. Antibacterial nanohydroxyapatite/polyurethane composite scaffolds with silver phosphate particles for bone regeneration. J Biomater Sci Polym Ed. 2016;27:1584–98.
Gite VV, Kulkarni RD, Hundiwale DG, Kapadi UR. Synthesis and characterisation of polyurethane coatings based on trimer of isophorone diisocyanate (IPDI) and monoglycerides of oils. Surf Coat Int. 2006;89:117–22.
Norden CW. Experimental osteomyelitis. I. A description of the model. J Infect Dis. 1970;122:410–8.
Brennan SA, Ní Fhoghlú C, Devitt BM, O'Mahony FJ, Brabazon D, Walsh A. Silver nanoparticles and their orthopaedic applications. Bone Joint J. 2015;97:582–9.
Gosheger G, Hardes J, Ahrens H, Streitburger A, Buerger H, Erren M, et al. Silver-coated megaendoprostheses in a rabbit model—an analysis of the infection rate and toxicological side effects. Biomaterials. 2004;25:5547–56.
Samani S, Hossainalipour SM, Tamizifar M, Rezaie HR. In vitro antibacterial evaluation of sol-gel-derived Zn-, Ag-, and (Zn+ Ag)-doped hydroxyapatite coatings against methicillin-resistant Staphylococcus aureus. J Biomed Mater Res A. 2013;101:222–30.
Shimazaki T, Miyamoto H, Ando Y, Noda I, Yonekura Y, Kawano S, et al. In vivo antibacterial and silver-releasing properties of novel thermal sprayed silver-containing hydroxyapatite coating. J Biomed Mater Res B Appl Biomater. 2010;92:386–9.
Yonekura Y, Miyamoto H, Shimazaki T, Ando Y, Noda I, Mawatari M, et al. Osteoconductivity of thermal-sprayed silver-containing hydroxyapatite coating in the rat tibia. J Bone Joint Surg Br. 2011;93:644–9.
Eto S, Miyamoto H, Shobuike T, Noda I, Akiyama T, Tsukamoto M, et al. Silver oxide-containing hydroxyapatite coating supports osteoblast function and enhances implant anchorage strength in rat femur. J Orthop Res. 2015;33:1391–7.
Fielding GA, Roy M, Bandyopadhyay A, Bose S. Antibacterial and biological characteristics of silver containing and strontium doped plasma sprayed hydroxyapatite coatings. Acta Biomater. 2012;8:3144–52.
Rihn JA, Kirkpatrick K, Albert TJ. Graft options in posterolateral and posterior interbody lumbar fusion. Spine (Phila Pa 1976). 2010;35:1629–39.
Mao K, Yang Y, Li J, Hao L, Tang P, Wang Z, et al. Investigation of the histology and interfacial bonding between carbonated hydroxyapatite cement and bone. Biomed Mater. 2009;4:045003.
Park SH, Park DS, Shin JW, Kang YG, Kim HK, Yoon TR, et al. Scaffolds for bone tissue engineering fabricated from two different materials by the rapid prototyping technique: PCL versus PLGA. J Mater Sci Mater Med. 2012;23:2671–8.
von Doernberg MC, von Rechenberg B, Bohner M, Grünenfelder S, van Lenthe GH, Müller R, et al. In vivo behavior of calcium phosphate scaffolds with four different pore sizes. Biomaterials. 2006;27:5186–98.
Neut D, van de Belt H, van Horn JR, van der Mei HC, Busscher HJ. Residual gentamicin-release from antibiotic-loaded polymethylmethacrylate beads after 5 years of implantation. Biomaterials. 2003;24:1829–31.
Thian ES, Lim PN, Shi Z, Tay BY, Neoh KG. Silver-doped apatite as a bioactive and an antimicrobial bone material. Key Engineering Materials. 2012;493-4:27–30.
Choi JW, Cho HM, Kwak EK, Kwon TG, Ryoo HM, Jeong YK, et al. Effect of Ag-doped hydroxyapatite as a bone filler for inflamed bone defects. Key Engineering Materials. 2004;254–6:47–50.
Roy M, Fielding GA, Beyenal H, Bandyopadhyay A, Bose S. Mechanical, in vitro antimicrobial, and biological properties of plasma-sprayed silver-doped hydroxyapatite coating. ACS Appl Mater Interfaces. 2012;4:1341–9.
Pepla E, Besharat LK, Palaia G, Tenore G, Migliau G. Nano-hydroxyapatite and its applications in preventive, restorative and regenerative dentistry: a review of literature. Ann Stomatol (Roma). 2014;5:108–14.
Venkatesan J, Kim SK. Nano-hydroxyapatite composite biomaterials for bone tissue engineering–a review. J Biomed Nanotechnol. 2014;10:3124–40.
Acknowledgements
The authors thank Mian Tian (from Department of orthopedic Surgery, The First Affiliated Hospital of Chongqing Medical University) for his help on surgical procedure. They are also grateful to the Infectious Disease Laboratory of The First Affiliated Hospital of Chongqing Medical University for donating bacterial strains.
Funding
This work was supported by the National High Technology Research and Development Program of China (863 Program, 2013AA032203) and the Social Undertakings and Livelihood Security Scientific and Technological Innovation Project of Chongqing China (cstc2017shmsA130022).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethics statement
The study was approved by the animal experiment ethic committee of The First Affiliated Hospital of Chongqing Medical University.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zhang, D., Liu, W., Wu, XD. et al. Efficacy of novel nano-hydroxyapatite/polyurethane composite scaffolds with silver phosphate particles in chronic osteomyelitis. J Mater Sci: Mater Med 30, 59 (2019). https://doi.org/10.1007/s10856-019-6261-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10856-019-6261-7