Abstract
Background
The time-to-isolation (TTI) may be a physiological predictor of durable isolations, and TTI-guided dosing strategies are widely performed in cryoballoon ablation. We sought to investigate the impact of the order of targeting the pulmonary veins (PVs) on the TTI values of left ipsilateral PVs.
Methods
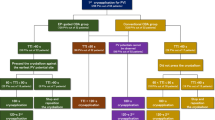
This study included 144 atrial fibrillation patients who underwent PV isolations using 28-mm fourth-generation cryoballoons. In 101 patients, the left superior PV (LSPV) was targeted and followed by the left inferior PV (LIPV) (group 1), and the LIPV was targeted and followed by the LSPV in the remaining 43 (group 2).
Results
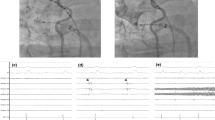
The total LSPV and LIPV freeze durations were 193 ± 60 and 171 ± 40 s, respectively. Real-time PV isolation monitoring was capable in 137 (95.1%) LSPVs and 119 (82.6%) LIPVs and in 112 (77.8%) patients (78 in group 1 and 34 in group 2) in both LSPVs and LIPVs. Among them, the LSPV TTI was significantly longer in group 1 than that in group 2 (54.8 ± 32.1 vs. 34.1 ± 17.3 s, p < 0.0001), while the LIPV TTI was significantly shorter in group 1 than that in group 2 (23.7 ± 11.8 vs. 39.2 ± 19.4 s, p < 0.0001). The ΔTTI ((TTI in LSPV)-(TTI in LIPV)) was significantly greater in group 1 than that in group 2 (31.1 ± 31.4 vs. − 5.0 ± 25.9 s, p < 0.0001). In 5 patients (3 in group 1 and 2 in group 2), initially targeted left PVs were not isolated despite complete vein occlusions, while they were by subsequent applications at the other ipsilateral PVs.
Conclusions
In CB ablation, the order of targeting PVs highly influenced the TTI of the left PVs owing to the presence of electrical connections between left ipsilateral PVs.


Similar content being viewed by others
References
Calkins H, Hindricks G, Cappato R, Kim YH, Saad EB, Aguinaga L, Akar JG, Badhwar V, Brugada J, Camm J, Chen PS, Chen SA, Chung MK, Nielsen JC, Curtis AB, Davies DW, Day JD, d’Avila A, de Groot NMSN, Di Biase L, Duytschaever M, Edgerton JR, Ellenbogen KA, Ellinor PT, Ernst S, Fenelon G, Gerstenfeld EP, Haines DE, Haissaguerre M, Helm RH, Hylek E, Jackman WM, Jalife J, Kalman JM, Kautzner J, Kottkamp H, Kuck KH, Kumagai K, Lee R, Lewalter T, Lindsay BD, Macle L, Mansour M, Marchlinski FE, Michaud GF, Nakagawa H, Natale A, Nattel S, Okumura K, Packer D, Pokushalov E, Reynolds MR, Sanders P, Scanavacca M, Schilling R, Tondo C, Tsao HM, Verma A, Wilber DJ, Yamane T. 2017 HRS/EHRA/ECAS/APHRS/SOLAECE expert consensus statement on catheter and surgical ablation of atrial fibrillation. Heart Rhythm. 2017;14:e275–444.
Kuck KH, Brugada J, Fürnkranz A, Metzner A, Ouyang F, Chun KR, Elvan A, Arentz T, Bestehorn K, Pocock SJ, Albenque JP, Tondo C, FIRE AND ICE Investigators. Cryoballoon or radiofrequency ablation for paroxysmal atrial fibrillation. N Engl J Med. 2016;374:2235–45.
Chun KR, Stich M, Fürnkranz A, Bordignon S, Perrotta L, Dugo D, Bologna F, Schmidt B. Individualized cryoballoon energy pulmonary vein isolation guided by real-time pulmonary vein recordings, the randomized ICE-T trial. Heart Rhythm. 2017;14:495–500.
Aryana A, Kenigsberg DN, Kowalski M, Koo CH, Lim HW, O’Neill PG, Bowers MR, Hokanson RB, Ellenbogen KA, Cryo-DOSING Investigators. Verification of a novel atrial fibrillation cryoablation dosing algorithm guided by time-to-pulmonary vein isolation: results from the Cryo-DOSING Study (Cryoballoon-ablation DOSING based on the assessment of time-to-effect and pulmonary vein isolation guidance). Heart Rhythm. 2017;14:1319–25.
Miyazaki S, Kajiyama T, Watanabe T, Nakamura H, Hachiya H, Tada H, Iesaka Y. Predictors of durable pulmonary vein isolation after second-generation cryoballoon ablation with a single short freeze strategy - different criteria for the best freeze of the 4 individual PVs. Int J Cardiol. 2020;301:96–102.
Miyazaki S, Kajiyama T, Watanabe T, Nakamura H, Hachiya H, Tada H, Iesaka Y. Can the durability of pulmonary vein isolation be predicted by the time-to-isolation in second-generation cryoballoon ablation?: Insight From the Results of Repeat Procedures. Circ Arrhythm Electrophysiol. 2020;13:e008076.
Cabrera JA, Ho SY, Climent V, Fuertes B, Murillo M, Sánchez-Quintana D. Morphological evidence of muscular connections between contiguous pulmonary venous orifices: relevance of the interpulmonary isthmus for catheter ablation in atrial fibrillation. Heart Rhythm. 2009;6:1192–8.
Tritto M, De Ponti R, Zardini M, Spadacini G, Oliveira M, Salerno-Uriarte JA. Electrical connection between pulmonary veins in humans. Evidence after radiofrequency ablation of the venoatrial junction. Circulation. 2001;104:e30–1.
Takahashi A, Iesaka Y, Takahashi Y, Takahashi R, Kobayashi K, Takagi K, Kuboyama O, Nishimori T, Takei H, Amemiya H, Fujiwara H, Hiraoka M. Electrical connections between pulmonary veins: implication for ostial ablation of pulmonary veins in patients with paroxysmal atrial fibrillation. Circulation. 2002;105:2998–3003.
Squara F, Liuba I, Chik W, Santangeli P, Maeda S, Zado ES, Callans D, Marchlinski FE. Electrical connection between ipsilateral pulmonary veins: prevalence and implications for ablation and adenosine testing. Heart Rhythm. 2015;12:275–82.
Miyazaki S, Kajiyama T, Watanabe T, Hada M, Nakamura H, Hachiya H, Tada H, Hirao K, Iesaka Y. Impact of electrical connections between ipsilateral pulmonary veins on the second-generation cryoballoon ablation procedure. J Cardiovasc Electrophysiol. 2019;30:27–31.
Acknowledgements
We thank Mr John Martin for his help in the preparation of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
The study protocol was approved by the hospital’s institutional review board. The study complied with the Declaration of Helsinki.
Informed consent
All patients gave their written informed consent.
Conflict of interest
Dr Miyazaki has received consulting fees and speaker honoraria from Medtronic and belongs to the endowed departments of Medtronic, Boston, Abbott, and Japan Lifeline. The other authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Miyazaki, S., Hasegawa, K., Nodera, M. et al. The impact of electrical connections between left ipsilateral pulmonary veins on the time-to-isolation values in cryoballoon ablation. J Interv Card Electrophysiol 64, 581–586 (2022). https://doi.org/10.1007/s10840-021-01034-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-021-01034-7