Abstract
Purpose
Conduction disturbances after transcatheter aortic valve replacement (TAVR) requiring pacemaker (PPM) implantation are a known complication and may be reversible. Therefore, we sought to evaluate the incidence and predictors for atrioventricular (AV) conduction recovery after TAVR.
Methods
A single-center, retrospective study of patients undergoing PPM implantation for conduction disorders after TAVR between June 2011 and March 2019. Conduction recovery was defined as ≤ 1% ventricular pacing (VP) on follow-up PPM interrogation.
Results
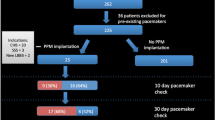
A total of 110 patients (mean age 83.6 ± 6.6 years, 46.8% female) were included. At a median follow-up of 438 days (interquartile range [IQR] 111–760 days), 35 patients (32%) had conduction recovery, with 50% of these occurring within the first 6 months. On multivariate analysis, predictors of conduction recovery include female sex (hazard ratio [HR] 2.5, 95% confidence interval [CI] 1.01–6.4, p = 0.048), non-VP/non-complete heart block rhythm immediately post-TAVR (HR 5.2, 95% CI 1.5–18.1, p = 0.011), normal sinus rhythm 7 days post-TAVR (HR 3.9, 95% CI 1.7–9.2, p = 0.002), and smaller valve size (mm) (HR 0.81, 95% CI 0.7–0.996, p = 0.045). Significant narrowing of the QRS and resolution of new-onset left bundle branch block within 1 month post-TAVR occurred in those with conduction recovery on PPM interrogation.
Conclusions
One-third of patients receiving new PPM implantation have conduction recovery after TAVR, with 50% occurring within the first 6 months. Patient gender, valve size, and rhythm on serial ECGs after TAVR can help identify patients that may recover AV conduction. A conservative approach rather than immediate PPM implantation may be considered in these patients.


Similar content being viewed by others
Abbreviations
- AV:
-
Atrioventricular
- CHB:
-
Complete heart block
- ECG:
-
Electrocardiogram
- LBBB:
-
Left bundle branch block
- LVEF:
-
Left ventricular ejection fraction
- LVOT:
-
Left ventricular outflow tract
- NSR:
-
Normal sinus rhythm
- PPM:
-
Permanent pacemaker
- RBBB:
-
Right bundle branch block
- TAVR:
-
Transcatheter aortic valve replacement
- TTE:
-
Transthoracic echocardiogram
- VP:
-
Ventricular pacing
References
Grover FL, Vemulapalli S, Carroll JD, Edwards FH, Mack MJ, Thourani VH, et al. STS/ACC TVT Registry. 2016 annual report of the Society of Thoracic Surgeons/American College of Cardiology Transcatheter Valve Therapy Registry. J Am Coll Cardiol. 2017;69(10):1215–30. https://doi.org/10.1016/j.jacc.2016.11.033.
Fadahunsi OO, Olowoyeye A, Ukaigwe A, Li Z, Vora AN, Vemulapalli S, et al. Incidence, predictors, and outcomes of permanent pacemaker implantation following transcatheter aortic valve replacement: analysis from the U.S. Society of Thoracic Surgeons/American College of Cardiology TVT Registry. JACC Cardiovasc Interv. 2016;9(21):2189–99. https://doi.org/10.1016/j.jcin.2016.07.026.
Maan A, Refaat MM, Heist EK, Passeri J, Inglessis I, Ptaszek L, et al. Incidence and predictors of pacemaker implantation in patients undergoing transcatheter aortic valve replacement. Pacing Clin Electrophysiol. 2015;38(7):878–86. https://doi.org/10.1111/pace.12653.
Regueiro A, Abdul-Jawad Altisent O, Del Trigo M, Campelo-Parada F, Puri R, Urena M, et al. Impact of new-onset left bundle branch block and periprocedural permanent pacemaker implantation on clinical outcomes in patients undergoing transcatheter aortic valve replacement: a systematic review and meta-analysis. Circ Cardiovasc Interv. 2016;9(5):e003635. https://doi.org/10.1161/CIRCINTERVENTIONS.115.003635.
Khatri PJ, Webb JG, Rodés-Cabau J, Fremes SE, Ruel M, Lau K, et al. Adverse effects associated with transcatheter aortic valve implantation: a meta-analysis of contemporary studies. Ann Intern Med. 2013;158(1):35–46. https://doi.org/10.7326/0003-4819-158-1-201301010-00007.
Aljabbary T, Qiu F, Masih S, Fang J, Elbaz-Greener G, Austin PC, et al. Association of clinical and economic outcomes with permanent pacemaker implantation after transcatheter aortic valve replacement. JAMA Netw Open. 2018;1(1):e180088. https://doi.org/10.1001/jamanetworkopen.2018.0088.
Nazif TM, Dizon JM, Hahn RT, Xu K, Babaliaros V, Douglas PS, et al. PARTNER Publications Office. Predictors and clinical outcomes of permanent pacemaker implantation after transcatheter aortic valve replacement: the PARTNER (Placement of AoRtic TraNscathetER Valves) trial and registry. JACC Cardiovasc Interv. 2015;8(1 Pt A):60–9. https://doi.org/10.1016/j.jcin.2014.07.022.
Smith CR, Leon MB, Mack MJ, Miller DC, Moses JW, Svensson LG, et al. Transcatheter versus surgical aortic-valve replacement in high-risk patients. N Engl J Med. 2011;364(23):2187–98. https://doi.org/10.1056/NEJMoa1103510.
Leon MB, Smith CR, Mack MJ, Makkar RR, Svensson LG, Kodali SK, et al. Transcatheter or surgical aortic-valve replacement in intermediate-risk patients. N Engl J Med. 2016;374(17):1609–20. https://doi.org/10.1056/NEJMoa1514616.
Popma JJ, Adams DH, Reardon MJ, Yakubov SJ, Kleiman NS, Heimansohn D, et al. Transcatheter aortic valve replacement using a self-expanding bioprosthesis in patients with severe aortic stenosis at extreme risk for surgery. J Am Coll Cardiol. 2014;63(19):1972–81. https://doi.org/10.1016/j.jacc.2014.02.556.
Reardon MJ, Van Mieghem NM, Popma JJ, Kleiman NS, Søndergaard L, Mumtaz M, et al. Surgical or transcatheter aortic-valve replacement in intermediate-risk patients. N Engl J Med. 2017;376(14):1321–31. https://doi.org/10.1056/NEJMoa1700456.
Mack MJ, Leon MB, Thourani VH, Makkar R, Kodali SK, Russo M, et al. Transcatheter aortic-valve replacement with a balloon-expandable valve in low-risk patients. N Engl J Med. 2019;380(18):1695–705. https://doi.org/10.1056/NEJMoa1814052.
Popma JJ, Deeb GM, Yakubov SJ, Mumtaz M, Gada H, O’Hair D, et al. Transcatheter aortic-valve replacement with a self-expanding valve in low-risk patients. N Engl J Med. 2019;380(18):1706–15. https://doi.org/10.1056/NEJMoa1816885.
Jilaihawi H, Zhao Z, Du R, Staniloae C, Saric M, Neuburger PJ, et al. Minimizing permanent pacemaker following repositionable self-expanding transcatheter aortic valve replacement. JACC Cardiovasc Interv. 2019;S1936–8798(19):31425–6. https://doi.org/10.1016/j.jcin.2019.05.056.
Rodés-Cabau J, Ellenbogen KA, Krahn AD, Latib A, Mack M, Mittal S, et al. Management of conduction disturbances associated with transcatheter aortic valve replacement: JACC Scientific Expert Panel. J Am Coll Cardiol. 2019;74(8):1086–106. https://doi.org/10.1016/j.jacc.2019.07.014.
Sharma E, Chu AF. Predictors of right ventricular pacing and pacemaker dependence in transcatheter aortic valve replacement patients. J Interv Card Electrophysiol. 2018 Jan;51(1):77–86. https://doi.org/10.1007/s10840-017-0303-1.
Lader JM, Barbhaiya CR, Subnani K, Park D, Aizer A, Holmes D, et al. Factors predicting persistence of AV nodal block in post-TAVR patients following permanent pacemaker implantation. Pacing Clin Electrophysiol. 2019;42:1347–54. https://doi.org/10.1111/pace.13789.
Gaede L, Kim WK, Liebetrau C, Dörr O, Sperzel J, Blumenstein J, et al. Pacemaker implantation after TAVI: predictors of AV block persistence. Clin Res Cardiol. 2018;107(1):60–9. https://doi.org/10.1007/s00392-017-1158-2.
van der Boon RM, Van Mieghem NM, Theuns DA, Nuis RJ, Nauta ST, Serruys PW, et al. Pacemaker dependency after transcatheter aortic valve implantation with the self-expanding Medtronic CoreValve System. Int J Cardiol. 2013;168(2):1269–73. https://doi.org/10.1016/j.ijcard.2012.11.115.
Kaplan RM, Yadlapati A, Cantey EP, Passman RS, Gajjar M, Knight BP, et al. Conduction recovery following pacemaker implantation after transcatheter aortic valve replacement. Pacing Clin Electrophysiol. 2019;42(2):146–52. https://doi.org/10.1111/pace.13579.
Alasti M, Rashid H, Rangasamy K, Kotschet E, Adam D, Alison J, et al. Long-term pacemaker dependency and impact of pacing on mortality following transcatheter aortic valve replacement with the LOTUS valve. Catheter Cardiovasc Interv. 2018;92(4):777–82. https://doi.org/10.1002/ccd.27463.
Simms AD, Hogarth AJ, Hudson EA, Worsnop VL, Blackman DJ, O'Regan DJ, et al. Ongoing requirement for pacing post-transcatheter aortic valve implantation and surgical aortic valve replacement. Interact Cardiovasc Thorac Surg. 2013;17(2):328–33. https://doi.org/10.1093/icvts/ivt175.
Chamandi C, Barbanti M, Munoz-Garcia A, Latib A, Nombela-Franco L, Gutiérrez-Ibanez E, et al. Long-term outcomes in patients with new permanent pacemaker implantation following transcatheter aortic valve replacement. JACC Cardiovasc Interv. 2018;11(3):301–10. https://doi.org/10.1016/j.jcin.2017.10.032.
Urena M, Mok M, Serra V, Dumont E, Nombela-Franco L, DeLarochellière R, et al. Predictive factors and long-term clinical consequences of persistent left bundle branch block following transcatheter aortic valve implantation with a balloon-expandable valve. J Am Coll Cardiol. 2012;60(18):1743–52. https://doi.org/10.1016/j.jacc.2012.07.035.
Brignole M, Auricchio A, Baron-Esquivias G, Bordachar P, Boriani G, Breithardt OA, et al. 2013 ESC Guidelines on cardiac pacing and cardiac resynchronization therapy: the Task Force on cardiac pacing and resynchronization therapy of the European Society of Cardiology (ESC). Developed in collaboration with the European Heart Rhythm Association (EHRA). Eur Heart J. 2013;34(29):2281–329. https://doi.org/10.1093/eurheartj/eht150.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
This study was approved by the Institutional Review Board of Kaiser Permanente Southern California.
Conflict of interest
Dr. Vicken Aharonian is a consultant for Medtronic. The remaining authors have no conflicts of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Phan, D.Q., Goitia, J., Lee, MS. et al. Predictors of conduction recovery after permanent pacemaker implantation following transcatheter aortic valve replacement. J Interv Card Electrophysiol 61, 365–374 (2021). https://doi.org/10.1007/s10840-020-00813-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-020-00813-y