Abstract
Purpose
The aim of this study was to systematically investigate the potential heating effects of magnetic resonance imaging (MRI) in the presence of epicardial leads, which are connected to a device or abandoned, using a series of in vitro measurements.
Methods
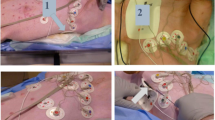
The heating effects of MRI in a 1.5-T scanner were measured at the lead tip in a gel-filled tank. First, a transvenous lead (5086—45 cm, Medtronic) was compared with an epicardial lead (4968—35 cm, Medtronic) with and without connection to an MR-conditional pacemaker. Then, experiments were conducted using various lengths of epicardial leads exposed to MRI.
Results
(1) A temperature rise of + 2.5 °C was observed for the transvenous lead attached to an MRI-conditional pacemaker. The epicardial lead attached to the same pacemaker showed four times higher heating. (2) The transvenous lead without pacemaker showed four times higher heating, and the epicardial lead without pacemaker showed 30 times higher heating. (3) The epicardial lead coiled to 20 cm length without pacemaker showed 9 times higher heating. (4) Experiments with various lengths of epicardial leads showed that the shorter the leads were, the smaller was the heating effect.
Conclusion
Standard clinical MRI investigations may result in pronounced heating at the tip of epicardial electrodes. Epicardial leads, which are not connected to a pacemaker and thus mimicking abandoned leads, may even result in a more pronounced rise in temperature at the lead tip. Therefore, current epicardial pacing systems may carry a substantial risk of inducing thermal damage of the neighboring tissue during MRI scanning.



Similar content being viewed by others
References
Sommer T, Bauer W, Fischbach K, Kolb C, Luechinger R, Wiegand U, et al. MR imaging in patients with cardiac pacemakers and implantable cardioverter defibrillators. Rofo. 2017;189:204–17.
Indik JH, Gimbel JR, Abe H, Alkmim-Teixeira R, Birgersdotter-Green U, Clarke GD, et al. 2017 HRS expert consensus statement on magnetic resonance imaging and radiation exposure in patients with cardiovascular implantable electronic devices. Heart Rhythm. 2017;14:e97–e153.
Vuorinen AM, Pakarinen S, Jaakkola I, Holmström M, Kivistö S, Kaasalainen T. Clinical experience of magnetic resonance imaging in patients with cardiac pacing devices: unrestricted patient population. Acta Radiol 2019;19:284185119830288.
Nazarian S, Hansford R, Rahsepar AA, Weltin V, McVeigh D, Gucuk Ipek E, et al. Safety of magnetic resonance imaging in patients with cardiac devices. N Engl J Med. 2017;377:2555–64.
Shah AD, Morris MA, Hirsh DS, Warnock M, Huang Y, Mollerus M, et al. Magnetic resonance imaging safety in nonconditional pacemaker and defibrillator recipients: a meta-analysis and systematic review. Heart Rhythm. 2018;15:1001–8.
Padmanabhan D, Kella DK, Mehta R, Kapa S, Deshmukh A, Mulpuru S, et al. Safety of magnetic resonance imaging in patients with legacy pacemakers and defibrillators and abandoned leads. Heart Rhythm. 2018;15:228–33.
Pulver AF, Puchalski MD, Bradley DJ, Minich LL, Su JT, Saarel EV, et al. Safety and imaging quality of MRI in pediatric and adult congenital heart disease patients with pacemakers. Pacing Clin Electrophysiol. 2009;32:450–6.
Luechinger R, Zeijlemaker VA, Pedersen EM, Mortensen P, Falk E, Duru, et al. In vivo heating of pacemaker leads during magnetic resonance imaging. Eur Heart J. 2005;26:376–83.
Nordbeck P, Weiss I, Ehses P, Ritter O, Warmuth M, Fidler F, et al. Measuring RF-induced currents inside implants: impact of device configuration on MRI safety of cardiac pacemaker leads. Magn Reson Med. 2009;61:570–8.
Bottomley PA, Redington RW, Edelstein WA, Schenck JF. Estimating radiofrequency power deposition in body NMR imaging. Magn Reson Med. 1985;2:336–49.
Cline H, Mallozzi R, Li Z, McKinnon G, Barber W. Radiofrequency power deposition utilizing thermal imaging. Magn Reson Med. 2004;51:1129–37.
Higgins JV, Gard JJ, Sheldon SH, Espinosa RE, Wood CP, Felmlee JP, et al. Safety and outcomes of magnetic resonance imaging in patients with abandoned pacemaker and defibrillator leads. Pacing Clin Electrophysiol. 2014;37:1284–90.
Langman DA, Goldberg IB, Finn JP, Ennis DB. Pacemaker lead tip heating in abandoned and pacemaker-attached leads at 1.5 tesla MRI. J Magn Reson Imaging. 2011;33:426–31.
Kubus P, Materna O, Gebauer RA, Matejka T, Gebauer R, Tláskal T, et al. Permanent epicardial pacing in children: long-term results and factors modifying outcome. Europace. 2012;14:509–14.
Egbe AC, Huntley GD, Connolly HM, Ammash NM, Deshmukh AJ, Khan AR, et al. Outcomes of cardiac pacing in adult patients after a Fontan operation. Am Heart J. 2017;194:92–8.
Winkler F, Dave H, Weber R, Gass M, Balmer C. Long-term outcome of epicardial implantable cardioverter-defibrillator systems in children: results justify its preference in paediatric patients. Europace. 2018;20:1484–90.
Buiten MS, van der Heijden AC, Klautz RJM, Schalij MJ, van Erven L. Epicardial leads in adult cardiac resynchronization therapy recipients: a study on lead performance, durability, and safety. Heart Rhythm. 2015;12:533–9.
Mellert F, Schneider C, Esmailzadeh B, Balta O, Haushofer M, Schiller W, et al. Implantation of left ventricular epicardial leads in cardiosurgical patients with impaired cardiac function--a worthwhile procedure in concomitant surgical interventions? Thorac Cardiovasc Surg. 2012;60:64–9.
Author information
Authors and Affiliations
Contributions
Christian Balmer: Study concept and study design; data analysis and interpretation, input of pediatric electrophysiology aspects, manuscript draft, and approval of the submitted version.
Matthias Gass: Relevant inputs to study design, critical manuscript revision, and approval of the submitted version.
Hitendu Dave: Relevant inputs to study design, highlighting the surgical aspects, critical manuscript revision, and approval of the submitted version.
Firat Duru: Developing the study protocol, critical manuscript revision, and approval of the submitted version.
Roger Luechinger: Study concept and study design, statistics, data analysis and interpretation, input of technical/engineering aspects, manuscript draft, and approval of the submitted version.
Corresponding author
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Balmer, C., Gass, M., Dave, H. et al. Magnetic resonance imaging of patients with epicardial leads: in vitro evaluation of temperature changes at the lead tip. J Interv Card Electrophysiol 56, 321–326 (2019). https://doi.org/10.1007/s10840-019-00627-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-019-00627-7