Abstract
Purpose
This study was conducted with the purpose of determining whether or not the potential technical advantages of multi-electrode mapping catheters in catheter ablation (CA) of ventricular tachycardia (VT) result in any relevant clinical benefit for VT patients.
Methods
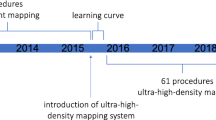
A single-center VT study, having taken place from 2012 to 2014 using a standard 3.5-mm catheter (Thermocool SF® group 1) and from 2014 to 2016 using a 1-mm multi-electrode-mapping catheter (PentaRay® group 2), was conducted. The endpoint was the complete elimination of late potentials (LPs), local abnormal ventricular activities (LAVA), and VT non-inducibility. Follow-up consisted of device interrogation to monitor for VT recurrence.
Results
Out of 74 VT patients aged 64.5 ± 12.0 years (66 male [89.2%], 56 with ICM [75.7%], and 18 with NICM [24.3%)]), 48 patients (64.9%) were investigated in group 1 and 26 (35.1%) in group 2. Using the multi-point acquisition approach, a tendency to require less mapping time (group 1 65.2 ± 37.6 min, group 2 55.6 ± 34.4 min, p ns) was determined. During 12-month follow-up, 57 patients had freedom from VT recurrences (79.2%). The result was insignificant between the groups (38 patients (79.2%) in group 1 and 19 patients (73.1%) in group 2).
Conclusions
In a single-center observational study, both conventional and high-density mapping approaches in VT patients are comparable in terms of procedure duration and outcome. Mapping time when using a multi-electrode catheter seems to have the tendency of being shorter. We should be encouraged to recruit more patients comparing the benefit of different catheter types.





Similar content being viewed by others
Abbreviations
- AT:
-
ablation time
- CA:
-
catheter ablation
- CABG:
-
coronary artery bypass graft
- CRT:
-
cardiac resynchronization therapy
- EAM:
-
electroanatomical mapping
- ECGs:
-
electrocardiograms
- EF:
-
ejection fraction
- FT:
-
fluoroscopy time
- ICD:
-
internal cardioverter defibrillator
- ICM:
-
ischemic cardiomyopathy
- LPs:
-
late potentials
- LAVA:
-
local abnormal ventricular activity
- LV:
-
left ventricle
- MEM:
-
multi-electrode-mapping
- MT:
-
mapping time
- NICM:
-
non-ischemic cardiomyopathy
- NYHA:
-
New York Heart Association
- PBP:
-
point-by-point
- PD:
-
procedure duration
- PVS:
-
programmed ventricular stimulation
- RV:
-
right ventricle
- SHD:
-
structural heart disease
- SR:
-
sinus rhythm
- VT:
-
ventricular tachycardia
- 3D–EAM:
-
three-dimensional electronical mapping
References
Aliot EM, Stevenson WG, Almendral-Garrote JM, Bogun F, Calkins CH, Delacretaz E, Della Bella P, Hindricks G, Jaïs P, Josephson ME, Kautzner J, Kay GN, Kuck KH, Lerman BB, Marchlinski F, Reddy V, Schalij MJ, Schilling R, Soejima K, Wilber D, European Heart Rhythm Association (EHRA) Registered Branch of the European Society of Cardiology (ESC),Heart Rhythm Society (HRS), American College of Cardiology (ACC), American Heart Association (AHA) EHRA/HRS expert consensus on catheter ablation of ventricular arrhythmias: developed in a partnership with the European heart rhythm association (EHRA), a registered branch of the European Society of Cardiology (ESC), and the Heart Rhythm Society (HRS); in collaboration with the American College of Cardiology (ACC) and the American Heart Association (AHA). Heart Rhythm 2009;6:886–933, 6, https://doi.org/10.1016/j.hrthm.2009.04.030.
Haris M. Haqqani, Francis E. Marchlinski, Electrophysiologic substrate underlying postinfarction ventricular tachycardia: characterization and role in catheter ablation. Heart Rhythm, 2009Vol 6, No 8S, August Supplement .
Stevenson WG, Soejima K. Catheter ablation for ventricular tachycardia. Circulation. 2007;115(21):2750–60. https://doi.org/10.1161/CIRCULATIONAHA.106.655720.
Kottkamp H, Wetzel U, Schirdewahn P, Dorszewski A, Gerds-Li JH, Carbucicchio C, et al. Catheter ablation of ventricular tachycardia in remote myocardial infarction: substrate description guiding placement of individual linear lesions targeting noninducibility. J Cardiovasc Electrophysiol. 2003;14(7):675–81. https://doi.org/10.1046/j.1540-8167.2003.02541.x.
Marchlinski FE, Callans DJ, Gottlieb CD, Zado E. Linear ablation lesions for control of unmappable ventricular tachycardia in patients with ischemic and nonischemic cardiomyopathy. Circulation. 2000;101(11):1288–96. https://doi.org/10.1161/01.CIR.101.11.1288.
Arenal A, del Castillo S, Gonzalez-Torrecilla E, Atienza F, Ortiz M, Jimenez J, et al. Tachycardia-related channel in the scar tissue in patients with sustained monomorphic ventricular tachycardias: influence of the voltage scar definition. Circulation. 2004;110(17):2568–74. https://doi.org/10.1161/01.CIR.0000145544.35565.47.
Reddy VY, Neuzil P, Taborsky M, Ruskin JN. Short-term results of substrate mapping and radiofrequency ablation of ischemic ventricular tachycardia using a saline-irrigated catheter. J Am Coll Cardiol. 2003;41(12):2228–36. https://doi.org/10.1016/S0735-1097(03)00492-3.
Soejima K, Stevenson WG, Maisel WH, Sapp JL, Epstein LM. Electrically unexcitable scar mapping based on pacing threshold for identification of the reentry circuit isthmus. Circulation. 2002;106(13):1678–83. https://doi.org/10.1161/01.CIR.0000030187.39852.A7.
Soejima K, Suzuki M, Maisel WH, Brunckhorst CB, Delacretaz E, Blier L, et al. Catheter ablation in patients with multiple and unstable ventricular tachycardias after myocardial infarction: short ablation lines guided by reentry circuit isthmuses and sinus rhythm mapping. Circulation. 2001;104(6):664–9. https://doi.org/10.1161/hc3101.093764.
Stevenson WG, Wilber DJ, Natale A, Jackman WM, Marchlinski FE, Talbert T, et al. Multicenter Thermocool VT Ablation Trial Investigators. Irrigated radiofrequency catheter ablation guided by electroanatomic mapping for recurrent ventricular tachycardia after myocardial infarction: the multicenter thermocool ventricular tachycardia ablation trial. Circulation. 2008;118(25):2773–82.
Tung R, Vaseghi M, Frankel DS, Vergara P, di Biase L, Nagashima K, et al. Freedom from recurrent ventricular tachycardia after catheter ablation is associated with improved survival in patients with structural heart disease: an international VT ablation center collaborative group study FHRS. Heart Rhythm. 2015;12(9):1997–2007. https://doi.org/10.1016/j.hrthm.2015.05.036.
Anter E, Tschabrunn CM, Buxton AE, Josephson ME. High-resolution mapping of Postinfarction reentrant ventricular tachycardia: electrophysiological characterization of the circuit. Circulation. 2016 Jul 26;134(4):314–27. https://doi.org/10.1161/CIRCULATIONAHA.116.021955.
Tschabrunn CM, Roujol S, Dorman NC, Nezafat R, Josephson ME, Anter E. High-Resolution Mapping of Ventricular Scar: Comparison Between Single and Multielectrode Catheters. Circ Arrhythm Electrophysiol. 2016;9(6):e003841. https://doi.org/10.1161/CIRCEP.115.003841.
Yamashita S, Cochet H, Sacher F, et al. Impact of New Technologies and Approaches for Post-Myocardial Infarction Ventricular Tachycardia Ablation During Long-Term Follow-Up. Circ Arrhythm Electrophysiol. 2016;9(7):e003901.
Sosa E, Scanavacca M, d'Avila A, Pilleggi FA. New technique to perform epicardial mapping in the electrophysiology laboratory. J Cardiovasc Electrophysiol. 1996;7(6):531–6. https://doi.org/10.1111/j.1540-8167.1996.tb00559.x.
Kuteszko R, Pytkowski M, Farkowski MM, et al. Utility of automated template matching for the interpretation of pace mapping in patients ablated due to outflow tract ventricular arrhythmias. Europace. 2015;17(9):1428–34. https://doi.org/10.1093/europace/euu392.
Cano O, Hutchinson M, Lin D, Garcia F, Zado E, Bala R, et al. Electroanatomic substrate and ablation outcome for suspected epicardial ventricular tachycardia in left ventricular nonischemic cardiomyopathy. J Am Coll Cardiol. 2009;54(9):799–808. https://doi.org/10.1016/j.jacc.2009.05.032.
Tanner H, Hindricks G, Volkmer M, Furniss S, Kühlkamp V, Lacroix D, de Chillou C, Almendral J, Caponi D, Kuck KH, Kottkamp H. Catheter ablation of recurrent scar-related ventricular tachycardia using electroanatomical mapping and irrigated ablation technology: results of the prospective multicenter Euro-VT-study. J Cardiovasc Electrophysiol. 2010 21(1):47–53. https://doi.org/10.1111/j.1540-8167.2009.01563.x. Epub 2009 Jul 28.
McPherson CA, Rosenfeld LE, Batsford WP. Day-to-day reproducibility of responses to right ventricular programmed electrical stimulation: implications for serial drug testing. Am J Cardiol. 1985;55(6):689–95. https://doi.org/10.1016/0002-9149(85)90138-9.
Acosta J, Penela D, Andreu D, Cabrera M, Carlosena A, Vassanelli F, et al. Multielectrode vs. point-by-point mapping for ventricular tachycardia substrate ablation: a randomized study. Europace. 2017;8:euw406. https://doi.org/10.1093/europace/euw406.
Kapa S, Desjardins B, Callans DJ, Marchlinski FE, Dixit S. Contact electroanatomic mapping derived voltage criteria for characterizing left atrial scar in patients undergoing ablation for atrial fibrillation. J Cardiovasc Electrophysiol201425(10):1044–-1052. https://doi.org/10.1111/jce.12452. Epub 2014 Jun 11.
Anter E, Tschabrunn CM, Josephson ME. High-resolution mapping of scar-related atrial arrhythmias using smaller electrodes with closer interelectrode spacing. Circ Arrhythm Electrophysiol. 2015;8(3):537–45. https://doi.org/10.1161/CIRCEP.114.002737. Epub 2015 Mar 19
Spragg DD, Khurram I, Zimmerman SL, Yarmohammadi H, Barcelon B, Needleman M, et al. Initial experience with magnetic resonance imaging of atrial scar and co-registration with electroanatomic voltage mapping during atrial fibrillation: success and limitations. Heart Rhythm. 2012;9(12):2003–9. https://doi.org/10.1016/j.hrthm.2012.08.039.
Squara F, Frankel DS, Schaller R, Kapa S, Chik WW, Callans DJ, et al. Voltage mapping for delineating inexcitable dense scar in patients undergoing atrial fibrillation ablation: a new end point for enhancing pulmonary vein isolation. Heart Rhythm. 2014;11(11):1904–11. https://doi.org/10.1016/j.hrthm.2014.07.027.
Liang JJ, Elafros MA, Muser D, Pathak RK, Santangeli P, Supple GE, et al. Comparison of left atrial bipolar voltage and scar using multielectrode fast automated mapping versus point-by-point contact Electroanatomic mapping in patients with atrial fibrillation undergoing repeat ablation. J Cardiovasc Electrophysiol. 2017 Mar;28(3):280–8. https://doi.org/10.1111/jce.13151. Epub 2017 Jan 10
Cassidy DM, Vassallo JA, Marchlinski FE, Buxton AE, Untereker WJ, Josephson ME. Endocardial mapping in humans in sinus rhythm with normal left ventricles: activation patterns and characteristics of electrograms. Circulation. 1984;70(1):37–42. https://doi.org/10.1161/01.CIR.70.1.37.
Hutchinson MD, Gerstenfeld EP, Desjardins B, Bala R, Riley MP, Garcia FC, et al. Endocardial unipolar voltagemapping to detect epicardial ventricular tachycardia substrate in patients with nonischemic left ventricular cardiomyopathy. Circ Arrhythm Electrophysiol. 2011;4(1):49–55. https://doi.org/10.1161/CIRCEP.110.959957.
Hsia HH, Callans DJ, Marchlinski FE. Characterization of endocardial electrophysiological substrate in patients with nonischemic cardiomyopathy and monomorphic ventricular tachycardia. Circulation. 2003;108(6):704–10. https://doi.org/10.1161/01.CIR.0000083725.72693.EA.
Marra MP, Leoni L, Bauce B, Corbetti F, Zorzi A, Migliore F, et al. Imaging study of ventricular scar in arrhythmogenic right ventricular cardiomyopathy: comparison of 3D standard electroanatomical voltagemapping and contrast-enhanced cardiac magnetic resonance. Circ Arrhythm Electrophysiol. 2012;5(1):91–100. https://doi.org/10.1161/CIRCEP.111.964635.
Deneke T, Muller KM, Lemke B, Lawo T, Calcum B, Helwing M, et al. Human histopathology of electroanatomic mapping after cooled-tip radiofrequency ablation to treat ventricular tachycardia in remote myocardial infarction. J Cardiovasc Electrophysiol. 2005;16(11):1246–51. https://doi.org/10.1111/j.1540-8167.2005.40826.x.
Perin EC, Silva GV, Sarmento-Leite R, Sousa AL, Howell M, Muthupillai R, et al. Assessing myocardial viability and infarct transmurality with left ventricular electromechanical mapping in patients with stable coronary artery disease: validation by delayed-enhancement magnetic resonance imaging. Circulation. 2002;106(8):957–61. https://doi.org/10.1161/01.CIR.0000026394.01888.18.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The study was approved by the Institutional Committee on Human Research. All patients signed consent forms prior to the ablation procedure.
Rights and permissions
About this article
Cite this article
Maagh, P., Christoph, A., Müller, M.S. et al. Point-by-point versus multisite electrode mapping in VT ablation: does freedom from VT recurrences depend on mapping catheter? An observational study. J Interv Card Electrophysiol 51, 169–181 (2018). https://doi.org/10.1007/s10840-018-0311-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-018-0311-9