Abstract
Background
Electrocardiographic conduction abnormalities following transcatheter aortic valve replacement (TAVR) with the Edwards-Sapien valve (ESV) are not uncommon and may be transient. We sought to examine the clinical time-course of conduction abnormalities after TAVR with ESV and determine risk factors for persistent abnormalities.
Methods
In this single-center prospective study, 116 consecutive patients underwent implantation of the ESV after approval by the Food and Drug Administration (FDA). Demographic, clinical, and intra-procedural variables were collected in a registry, including ECGs before, immediately after, and at discharge from hospital. Conduction abnormalities were analyzed including PR interval lengthening, QRS widening, left bundle branch block (LBBB), and high-grade AV block.
Results
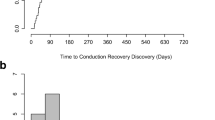
There were 92 patients included in the analysis. A total of 41 new conduction abnormalities were observed in 31 (34 %) patients: 7 new PR prolongation, 14 QRS widening, 14 new LBBB, and 5 high-grade AV block requiring permanent pacemaker. Of the 41 new CAs, 11 (27 %) were transient; of the transient abnormalities, 9 (82 %) resolved within 24 h of the index procedure. Chronic kidney disease was a risk factor for the development of a persistent abnormality and for need for PPM. Antegrade approach was associated with the development of persistent LBBB and persistent QRS widening.
Conclusions
A significant proportion of conduction abnormalities after ESV implantation improved prior to discharge from the hospital, usually within 24 h. CKD is associated with persistence of abnormalities and with need for PPM. Antegrade approach increases risk for new intraventricular conduction delays, including LBBB.






Similar content being viewed by others
Abbreviations
- ECG:
-
Electrocardiogram
- TAVR:
-
Transcatheter aortic valve replacement
- PPM:
-
Permanent pacemaker
- LBBB:
-
Left bundle branch block
- LAFB:
-
Left anterior fascicular block
- POD:
-
Post-operative day
References
Laynez A, Ben-Dor I, Barbash IM, et al. Frequency of conduction disturbances after Edwards SAPIEN percutaneous valve implantation. Am J Cardiol. 2012;110:1164–8.
Roten L, Wenaweser P, Delacretaz E, et al. Incidence and predictors of atrioventricular conduction impairment after transcatheter aortic valve implantation. Am J Cardiol. 2010;106:1473–80.
Gutierrez M, Rodes-Cabau J, Bagur R, et al. Electrocardiographic changes and clinical outcomes after transapical aortic valve implantation. Am Heart J. 2009;158:302–8.
Aktug O, Dohmen G, Brehmer K, et al. Incidence and predictors of left bundle branch block after transcatheter aortic valve implantation. Int J Cardiol. 2012;160:26–30.
Houthuizen P, Van Garsse LA, Poels TT, et al. Left bundle-branch block induced by transcatheter aortic valve implantation increases risk of death. Circulation. 2012;126:720–8.
Sinhal A, Altwegg L, Pasupati S, et al. Atrioventricular block after transcatheter balloon expandable aortic valve implantation. J Am Coll Cardiol Intv. 2008;1:305–9.
Steinberg BA, Harrison JK, Frazier-Mills C, Hughes GC, Piccini JP. Cardiac conduction system disease after transcatheter aortic valve replacement. Am Heart J. 2012;164:664–71.
Leon MB, Smith CR, Mack M, et al. Transcatheter aortic-valve implantation for aortic stenosis in patients who cannot undergo surgery. N Engl J Med. 2010;363:1597–607.
Erkapic D, De Rosa S, Kelava A, Lehmann R, Fichtlscherer S, Hohnloser SH. Risk for permanent pacemaker after transcatheter aortic valve implantation: a comprehensive analysis of the literature. J Cardiovasc Electrophysiol. 2012;23:391–7.
Godino C, Maisano F, Montorfano M, et al. Outcomes after transcatheter aortic valve implantation with both Edwards-SAPIEN and CoreValve devices in a single center: the Milan experience. J Am Coll Cardiol Intv. 2010;3:1110–21.
Bleiziffer S, Ruge H, Horer J, et al. Predictors for new-onset complete heart block after transcatheter aortic valve implantation. J Am Coll Cardiol Intv. 2010;3:524–30.
Godin M, Eltchaninoff H, Furuta A, et al. Frequency of conduction disturbances after transcatheter implantation of an Edwards Sapien aortic valve prosthesis. Am J Cardiol. 2010;106:707–12.
Roten L, Stortecky S, Scarcia F, et al. Atrioventricular conduction after transcatheter aortic valve implantation and surgical aortic valve replacement. J Cardiovasc Electrophysiol. 2012;23:1115–22.
Piazza N, de Jaegere P, Schultz C, Becker AE, Serruys PW, Anderson RH. Anatomy of the aortic valvar complex and its implications for transcatheter implantation of the aortic valve. Circ Cardiovasc Interv. 2008;1:74–81.
Rubin JM, Avanzas P, del Valle R, et al. Atrioventricular conduction disturbance characterization in transcatheter aortic valve implantation with the CoreValve prosthesis. Circ Cardiovasc Interv. 2011;4:280–6.
Urena M, Mok M, Serra V, et al. Predictive factors and long-term clinical consequences of persistent left bundle branch block following transcatheter aortic valve implantation with a balloon-expandable valve. J Am Coll Cardiol. 2012;60:1743–52.
Haworth P, Behan M, Khawaja M, et al. Predictors for permanent pacing after transcatheter aortic valve implantation. Catheter Cardiovasc Interv: Off J Soc Cardiac Angiography Interv. 2010;76:751–6.
Piazza N, Onuma Y, Jesserun E, et al. Early and persistent intraventricular conduction abnormalities and requirements for pacemaking after percutaneous replacement of the aortic valve. J Am Coll Cardiol Intv. 2008;1:310–6.
Houthuizen P, van der Boon RM, Urena M, et al. Occurrence, fate and consequences of ventricular conduction abnormalities after transcatheter aortic valve implantation. EuroIntervention: J EuroPCR Collab Work Group Interv Cardiol Eur Soc Cardiol. 2014;9:1142–50.
Nazif TM, Williams MR, Hahn RT, et al. Clinical implications of new-onset left bundle branch block after transcatheter aortic valve replacement: analysis of the PARTNER experience. Eur Heart J. 2014;35:1599–607.
Nuis RJ, Van Mieghem NM, Schultz CJ, et al. Timing and potential mechanisms of new conduction abnormalities during the implantation of the Medtronic CoreValve System in patients with aortic stenosis. Eur Heart J. 2011;32:2067–74.
Lardizabal JA, O’Neill BP, Desai HV, et al. The transaortic approach for transcatheter aortic valve replacement: initial clinical experience in the United States. J Am Coll Cardiol. 2013;61:2341–5.
Lichtenstein SV, Cheung A, Ye J, et al. Transapical transcatheter aortic valve implantation in humans: initial clinical experience. Circulation. 2006;114:591–6.
Webb JG, Pasupati S, Humphries K, et al. Percutaneous transarterial aortic valve replacement in selected high-risk patients with aortic stenosis. Circulation. 2007;116:755–63.
Walther T, Simon P, Dewey T, et al. Transapical minimally invasive aortic valve implantation: multicenter experience. Circulation. 2007;116:I240–5.
Willems JL, de Medina EO R, Bernard R, et al. Criteria for intraventricular conduction disturbances and pre-excitation. World Health Organizational/International Society and Federation for Cardiology Task Force Ad Hoc. J Am Coll Cardiol. 1985;5:1261–75.
Cohen MG, Singh V, Martinez CA, et al. Transseptal antegrade transcatheter aortic valve replacement for patients with no other access approach—a contemporary experience. Catheter Cardiovasc Interv: Off J Soc Cardiac Angiography Interv. 2013;82:987–93.
Ye J, Cheung A, Lichtenstein SV, et al. Transapical transcatheter aortic valve implantation: follow-up to 3 years. J Thorac Cardiovasc Surg. 2010;139:1107–13. 1113 e1.
Walther T, Schuler G, Borger MA, et al. Transapical aortic valve implantation in 100 consecutive patients: comparison to propensity-matched conventional aortic valve replacement. Eur Heart J. 2010;31:1398–403.
Foley RN, Murray AM, Li S, et al. Chronic kidney disease and the risk for cardiovascular disease, renal replacement, and death in the United States Medicare population, 1998 to 1999. J Am Soc Nephrol: JASN. 2005;16:489–95.
Shamseddin MK, Parfrey PS. Mechanisms of the cardiorenal syndromes. Nat Rev Nephrol. 2009;5:641–9.
Ravani P, Tripepi G, Malberti F, Testa S, Mallamaci F, Zoccali C. Asymmetrical dimethylarginine predicts progression to dialysis and death in patients with chronic kidney disease: a competing risks modeling approach. J Am Soc Nephrol: JASN. 2005;16:2449–55.
Tanawuttiwat T, O’Neill BP, Cohen MG, et al. New-onset atrial fibrillation after aortic valve replacement: comparison of transfemoral, transapical, transaortic, and surgical approaches. J Am Coll Cardiol. 2014;63:1510–9.
Damluji AA, Al-Damluji MS, Marzouka GR, et al. New-onset versus prior history of atrial fibrillation: outcomes from the AFFIRM trial. Am Heart J. 2015;170:156–63. e1.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
None.
Disclosures
All other authors have no conflict of interest.
Additional information
Solomon J. Sager and Abdulla A. Damluji contributed equally to this work.
Rights and permissions
About this article
Cite this article
Sager, S.J., Damluji, A.A., Cohen, J.A. et al. Transient and persistent conduction abnormalities following transcatheter aortic valve replacement with the Edwards-Sapien prosthesis: a comparison between antegrade vs. retrograde approaches. J Interv Card Electrophysiol 47, 143–151 (2016). https://doi.org/10.1007/s10840-016-0145-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-016-0145-2