Abstract
Background
The efficient delivery of radiofrequency (RF) energy through an endocardial ablation catheter is affected by variable tissue contact due to cardiac motion with myocardial contraction and respiration. In addition, many operators intentionally move an ablation catheter during the delivery of radiofrequency energy when targeting specific arrhythmias that require lines of conduction block such as atrial flutter and atrial fibrillation. We sought to characterize and quantify any effects of catheter movement and intermittent ablation catheter contact on lesion characteristics.
Methods
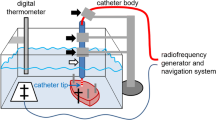
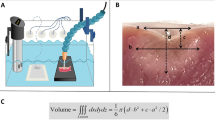
An ex vivo model consisting of recently excised viable bovine myocardium, a circulating saline bath at 37 °C, a submersible load cell, and a deflectable sheath with an ablation catheter was assembled. A stepper motor attached to an ablation catheter apparatus was programmed to simulate linear drag lesions and series of point lesions with variable contact using constant force. Lesion volumes were analyzed using a digital micrometer by measuring depth, max width, depth at max width, and surface width and compared.
Results
The drag lesion was significantly larger than a point-by-point linear lesion using a constant force of 15 g (2,088 ± 122 mm3 vs. 1,595 ± 121.6; p = 0.01) when controlling for RF time and power. For single point lesion assessment, constant contact lesions were significantly larger than lesions created with intermittent contact using the same duration of RF (194 ± 68 mm3 vs. 112.5 ± 53; p = 0.03). There was no significant difference in lesion size between the constant contact at 60 s and 90-s intermittent contact lesions (194 ± 68 mm3 vs.186 ± 69).
Conclusions
In our ex vivo model, externally irrigated radiofrequency catheters produced drag lesion volumes equal to or larger than those created by a point-by-point method. We also found decreased lesion size due to intermittent contact can be overcome by increasing duration of ablation time.




Similar content being viewed by others
References
Nakagawa, H., Yamanashi, W. S., Pitha, J. V., Arruda, M., Wang, X., Ohtomo, K., et al. (1995). Comparison of in vivo tissue temperature profile and lesion geometry for radiofrequency ablation with a saline-irrigated electrode versus temperature control in a canine thigh muscle preparation. Circulation, 91, 2264–2273.
Wood, M. A., Goldberg, S. M., Parvez, B., Pathak, V., Holland, K., Ellenbogen, A. L., et al. (2009). Effect of electrode orientation on lesion sizes produced by irrigated radiofrequency ablation catheters. Journal of Cardiovascular Electrophysiology, 20, 1262–1268.
Thiagalingam, A., D’avila, A., Foley, L., Guerrero, J. L., Lambert, H., Leo, G., et al. (2010). Importance of catheter contact force during irrigated radiofrequency ablation: evaluation in a porcine ex vivo model using a force-sensing catheter. Journal of Cardiovascular Electrophysiology, 21, 806–811.
Shah, D. C., Lambert, H., Nakagawa, H., Langenkamp, A., Aeby, N., & Leo, G. (2010). Area under the real-time contact force curve (force–time integral) predicts radiofrequency lesion size in an in vitro contractile model. Journal of Cardiovascular Electrophysiology, 21, 1038–1043.
Demazumder, D., Mirotznik, M. S., & Schwartzman, D. (2001). Comparison of irrigated electrode designs for radiofrequency ablation of myocardium. Journal of Interventional Cardiac Electrophysiology, 5, 391–400.
Nakagawa, H., Wittkampf, F. H. M., Yamanashi, W. S., Pitha, J. V., Imai, S., Campbell, B., et al. (1998). Inverse relationship between electrode size and lesion size during radiofrequency ablation with active electrode cooling. Circulation, 98, 458–465.
Jaïs, P., Hocini, M., Hsu, L.-F., Sanders, P., Scavee, C., Weerasooriya, R., et al. (2004). Technique and results of linear ablation at the mitral isthmus. Circulation, 110, 2996–3002.
Miyazaki, S., Takahashi, A., Kuwahara, T., Kobori, A., Yokoyama, Y., Nozato, T., et al. (2007). Randomized comparison of the continuous vs point-by-point radiofrequency ablation of the cavotricuspid isthmus for atrial flutter. Circulation Journal, 71, 1922–1926.
Okumura, Y., Johnson, S. B., Bunch, T. J., Henz, B. D., O’brien, C. J., & Packer, D. L. (2008). A systematical analysis of in vivo contact forces on virtual catheter tip/tissue surface contact during cardiac mapping and intervention. Journal of Cardiovascular Electrophysiology, 19, 632–640.
Yokokawa, M., Bhandari, A. K., Tada, H., Suzuki, A., Kawamura, M., Ho, I., et al. (2011). Comparison of the point-by-point versus catheter dragging technique for curative radiofrequency ablation of atrial fibrillation. Pacing and Clinical Electrophysiology, 34, 15–22.
Ernst, S., Ouyang, F., Löber, F., Antz, M., & Kuck, K.-H. (2003). Catheter-induced linear lesions in the left atrium in patients with atrial fibrillation: an electroanatomic study. Journal of the American College of Cardiology, 42, 1271–1282.
van Rensburg, H., Willems, R., Holemans, P., Anné, W., Ector, H., & Heidbüchel, H. (2002). Simultaneous creation and evaluation of linear radiofrequency lesions. Journal of Interventional Cardiac Electrophysiology, 6, 215–224.
Everett, T. H., IV, Lee, K. W., Wilson, E. E., Guerra, J. M., Varosy, P. D., & Olgin, J. E. (2009). Safety profiles and lesion size of different radiofrequency ablation technologies: a comparison of large tip, open and closed irrigation catheters. Journal of Cardiovascular Electrophysiology, 20, 325–335.
Demazumder, D., Mirotznik, M. S., & Schwartzman, D. (2001). Biophysics of radiofrequency ablation using an irrigated electrode. Journal of Interventional Cardiac Electrophysiology, 5, 377–389.
Su, W. W., Johnson, S. B., Jain, M. K., Hall, J., & Packer, D. L. (2005). Creating continuous linear lesions in the atria: a comparison of the multipolar ablation technique versus the conventional drag-and-burn. Journal of Cardiovascular Electrophysiology, 16, 905–911.
McRury, I. D., Panescu, D., Mitchell, M. A., & Haines, D. E. (1997). Nonuniform heating during radiofrequency catheter ablation with long electrodes monitoring the edge effect. Circulation, 96, 4057–4064.
Yokoyama, K., Nakagawa, H., Shah, D. C., Lambert, H., Leo, G., Aeby, N., et al. (2008). Novel contact force sensor incorporated in irrigated radiofrequency ablation catheter predicts lesion size and incidence of steam pop and thrombus. Circulation. Arrhythmia and Electrophysiology, 1, 354–362.
Acknowledgments
The authors thank Bonnie Neltner for assistance in experimental setup and maintenance of the University of Colorado Ablation Biophysics Laboratory.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Olson, M.D., Phreaner, N., Schuller, J.L. et al. Effect of catheter movement and contact during application of radiofrequency energy on ablation lesion characteristics. J Interv Card Electrophysiol 38, 123–129 (2013). https://doi.org/10.1007/s10840-013-9824-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-013-9824-4