Abstract
Purpose
Kartagener syndrome (KS), also known as visceral inversion-nasosinusitis-bronchiectasis syndrome, or familial bronchiectasis, is an autosomal recessive inherited disease. In this study, through two cases of KS, we aimed to assess the clinical and genetic characteristics of KS caused by DNAH5 mutations.
Methods
The two cases of KS from the same family underwent extensive clinical assessments, with next-generation DNA sequencing and bioinformatics analysis to identify pathogenic genes. In addition, Sanger sequencing was used to verify the pedigrees.
Results
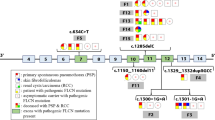
The present study employed a directional capture strategy for hereditary disease screening, which correctly identified the virulence sites in the pedigree, and facilitated the differential diagnosis among multiple genes. Two novel mutations were detected in DNAH5: c.7778C>T (missense mutation) and c.13729G>A (nonsense mutation). They were not found in dbSNP, 1000 Genomes, and ExAC.
Conclusions
These findings demonstrated that new DNAH5 mutations could be used for molecular diagnosis of KS, providing families with genetic counseling and prenatal diagnosis.



Similar content being viewed by others
References
Moore A, Escudier E, Roger G, Tamalet A, Pelosse B, Marlin S, et al. RPGR is mutated in patients with a complex X linked phenotype combining primary ciliary dyskinesia and retinitis pigmentosa. J Med Genet. 2006;43(4):326–33. doi:10.1136/jmg.2005.034868.
Knowles MR, Leigh MW, Ostrowski LE, Huang L, Carson JL, Hazucha MJ, et al. Exome sequencing identifies mutations in CCDC114 as a cause of primary ciliary dyskinesia. Am J Hum Genet. 2013;92(1):99–106. doi:10.1016/j.ajhg.2012.11.003.
Afzelius B, Mossberg B, Bergstrom S. Immotile-cilia syndrome (primary ciliary dyskinesia), including Kartagener syndrome. Metabol Molecul Base Inherit Dis. 1995;3:3943–54.
Kennedy MP, Omran H, Leigh MW, Dell S, Morgan L, Molina PL, et al. Congenital heart disease and other heterotaxic defects in a large cohort of patients with primary ciliary dyskinesia. Circulation. 2007;115(22):2814–21. doi:10.1161/CIRCULATIONAHA.106.649038.
Hogg C, Bush A. Genotyping in primary ciliary dyskinesia: ready for prime time, or a fringe benefit? Thorax. 2012;67(5):377–8. doi:10.1136/thoraxjnl-2011-201320.
O’Roak BJ, Deriziotis P, Lee C, Vives L, Schwartz JJ, Girirajan S, et al. Exome sequencing in sporadic autism spectrum disorders identifies severe de novo mutations. Nat Genet. 2011;43(6):585–9. doi:10.1038/ng.835.
Geremek M, Schoenmaker F, Zietkiewicz E, Pogorzelski A, Diehl S, Wijmenga C, et al. Sequence analysis of 21 genes located in the Kartagener syndrome linkage region on chromosome 15q. Euro J Hum Genet: EJHG. 2008;16(6):688–95. doi:10.1038/ejhg.2008.5.
Djakow J, Svobodova T, Hrach K, Uhlik J, Cinek O, Pohunek P. Effectiveness of sequencing selected exons of DNAH5 and DNAI1 in diagnosis of primary ciliary dyskinesia. Pediatr Pulmonol. 2012;47(9):864–75. doi:10.1002/ppul.22520.
Failly M, Bartoloni L, Letourneau A, Munoz A, Falconnet E, Rossier C, et al. Mutations in DNAH5 account for only 15% of a non-preselected cohort of patients with primary ciliary dyskinesia. J Med Genet. 2009;46(4):281–6. doi:10.1136/jmg.2008.061176.
Fliegauf M, Olbrich H, Horvath J, Wildhaber JH, Zariwala MA, Kennedy M, et al. Mislocalization of DNAH5 and DNAH9 in respiratory cells from patients with primary ciliary dyskinesia. Am J Respir Crit Care Med. 2005;171(12):1343–9. doi:10.1164/rccm.200411-1583OC.
Jorissen M, Willems T, Van der Schueren B, Verbeken E, De Boeck K. Ultrastructural expression of primary ciliary dyskinesia after ciliogenesis in culture. Acta Otorhinolaryngol Belg. 2000;54(3):343–56.
Afzelius BA. A human syndrome caused by immotile cilia. Science. 1976;193(4250):317–9.
Geremek M, Witt M. Primary ciliary dyskinesia: genes, candidate genes and chromosomal regions. J Appl Genet. 2004;45(3):347–61.
Noone PG, Leigh MW, Sannuti A, Minnix SL, Carson JL, Hazucha M, et al. Primary ciliary dyskinesia: diagnostic and phenotypic features. Am J Respir Crit Care Med. 2004;169(4):459–67. doi:10.1164/rccm.200303-365OC.
Halbert SA, Patton DL, Zarutskie PW, Soules MR. Function and structure of cilia in the fallopian tube of an infertile woman with Kartagener’s syndrome. Hum Reprod. 1997;12(1):55–8.
Fischer TJ, McAdams JA, Entis GN, Cotton R, Ghory JE, Ausdenmoore RW. Middle ear ciliary defect in Kartagener’s syndrome. Pediatrics. 1978;62(4):443–5.
Guichard C, Harricane MC, Lafitte JJ, Godard P, Zaegel M, Tack V, et al. Axonemal dynein intermediate-chain gene (DNAI1) mutations result in situs inversus and primary ciliary dyskinesia (Kartagener syndrome). Am J Hum Genet. 2001;68(4):1030–5. doi:10.1086/319511.
Eliasson R, Mossberg B, Camner P, Afzelius BA. The immotile-cilia syndrome. A congenital ciliary abnormality as an etiologic factor in chronic airway infections and male sterility. N Engl J Med. 1977;297(1):1–6. doi:10.1056/NEJM197707072970101.
Hornef N, Olbrich H, Horvath J, Zariwala MA, Fliegauf M, Loges NT, et al. DNAH5 mutations are a common cause of primary ciliary dyskinesia with outer dynein arm defects. Am J Respir Crit Care Med. 2006;174(2):120–6. doi:10.1164/rccm.200601-084OC.
Afzelius BA, Eliasson R. Male and female infertility problems in the immotile-cilia syndrome. Eur J Respir Dis Suppl. 1983;127:144–7.
Munro NC, Currie DC, Lindsay KS, Ryder TA, Rutman A, Dewar A, et al. Fertility in men with primary ciliary dyskinesia presenting with respiratory infection. Thorax. 1994;49(7):684–7.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Research involving human participants
The present study was approved by the Ethics Committee of People’s Hospital. All procedures performed in studies involving human participants were in accordance with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Capsule These findings demonstrated that new DNAH5 mutations could be used for molecular diagnosis of KS, providing families with genetic counseling and prenatal diagnosis.
Rights and permissions
About this article
Cite this article
Xu, X., Gong, P. & Wen, J. Clinical and genetic analysis of a family with Kartagener syndrome caused by novel DNAH5 mutations. J Assist Reprod Genet 34, 275–281 (2017). https://doi.org/10.1007/s10815-016-0849-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-016-0849-3