Abstract
Purpose
To study the differences in protein expression profiles of follicular fluid (FF) between controlled ovarian hyperstimulation (COH) and natural ovulatory cycles.
Methods
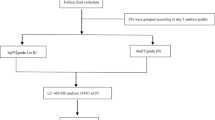
Twelve infertile women undergoing in vitro fertilization and embryo transfer (IVF–ET), with matched clinical information, were retrospectively recruited in the IVF center of our university hospital, including six undergoing COH and another six with natural cycles. FF was sampled from dominant follicles with mature oocytes. Protein expression profiles in each FF sample were analyzed respectively using two-dimensional gel electrophoresis. Differentially expressed proteins were identified using matrix-assisted laser desorption/ionization time-of-flight mass spectrometry (MALDI-TOF MS) and validated by western blotting. Differentially expressed proteins were further analyzed using Ingenuity Pathway Analysis (IPA) software.
Results
Two proteins were downregulated and 11 proteins were upregulated (change ≥1.5-fold, P < 0.05) in the COH group. We identified one down-egulated and seven upregulated proteins using MALDI-TOF MS. Four differentially expressed proteins, including transferrin, complement component C3 (C3), haptoglobin and alpha-1-antitrypsin (AAT), were further validated by rate nephelometry and western blotting analyses. The IPA analysis revealed a significant network involved in the humoral immune and inflammatory responses.
Conclusions
The eight differentially expressed proteins were related to immune and inflammatory responses in the ovary. Our results provide new insights into the influence of COH on follicular (spp) development and IVF outcomes.





Similar content being viewed by others
References
Orisaka M, Tajima K, Tsang BK, Kotsuji F. Oocyte-granulosa-theca cell interactions during preantral follicular development. J Ovarian Res. 2009;2(1):9.
Cheng Y, Kawamura K, Deguchi M, Takae S, Mulders SM, Hsueh AJ. Intraovarian thrombin and activated protein C signaling system regulates steroidogenesis during the periovulatory period. Mol Endocrinol. 2012;26(2):331–40.
Santos MA, Kuijk EW, Macklon NS. The impact of ovarian stimulation for IVF on the developing embryo. Reproduction. 2010;139(1):23–34.
Hammoud I, Vialard F, Bergere M, Albert M, Gomes DM, Adler M, et al. Follicular fluid protein content (FSH, LH, PG4, E2 and AMH) and polar body aneuploidy. J Assist Reprod Genet. 2012;29(10):1123–34.
Fortier AL, Lopes FL, Darricarrere N, Martel J, Trasler JM. Superovulation alters the expression of imprinted genes in the midgestation mouse placenta. Hum Mol Genet. 2008;17(11):1653–65.
Stouder C, Deutsch S, Paoloni-Giacobino A. Superovulation in mice alters the methylation pattern of imprinted genes in the sperm of the offspring. Reprod Toxicol. 2009;28(4):536–41.
Sachs AR, Politch JA, Jackson KV, Racowsky C, Hornstein MD, Ginsburg ES. Factors associated with the formation of triploid zygotes after intracytoplasmic sperm injection. Fertil Steril. 2000;73(6):1109–14.
Zhu YM, Hu XL, Wu YT, Feng C, Huang HF. Assisted Reproductive Technology and Gamete/Embryo-Fetal Origins of Diseases. In: Huang HF, Sheng JZ, editors. Gamete and embryo-fetal origins of adult diseases. Dordrecht: Springer Netherlands; 2014. p. 197.
Wilkins-Huag L. Assisted reproductive technology, congenital malformations, and epigenetic disease. Clin Obstet Gynecol. 2008;51(1):96–105.
Shiota K, Yamada S. Assisted reproductive technologies and birth defects. Congenit Anom (Kyoto). 2005;45(2):39–43.
Chang AS, Moley KH, Wangler M, Feinberg AP, Debaun MR. Association between Beckwith-Wiedemann syndrome and assisted reproductive technology: a case series of 19 patients. Fertil Steril. 2005;83(2):349–54.
Seggers J, Haadsma ML, La Bastide-Van GS, Heineman MJ, Middelburg KJ, Roseboom TJ, et al. Is ovarian hyperstimulation associated with higher blood pressure in 4-year-old IVF offspring? Part I: multivariable regression analysis. Hum Reprod. 2014;29(3):502–9.
Wu YT, Tang L, Cai J, Lu XE, Xu J, Zhu XM, et al. High bone morphogenetic protein-15 level in follicular fluid is associated with high quality oocyte and subsequent embryonic development. Hum Reprod. 2007;22(6):1526–31.
Kushnir MM, Naessen T, Wanggren K, Rockwood AL, Crockett DK, Bergquist J. Protein and steroid profiles in follicular fluid after ovarian hyperstimulation as potential biomarkers of IVF outcome. J Proteome Res. 2012;11(10):5090–100.
Von Wald T, Monisova Y, Hacker MR, Yoo SW, Penzias AS, Reindollar RR, et al. Age-related variations in follicular apolipoproteins may influence human oocyte maturation and fertility potential. Fertil Steril. 2010;93(7):2354–61.
Tyers M, Mann M. From genomics to proteomics. Nature. 2003;422(6928):193–7.
Liu AX, Jin F, Zhang WW, Zhou TH, Zhou CY, Yao WM, et al. Proteomic analysis on the alteration of protein expression in the placental villous tissue of early pregnancy loss. Biol Reprod. 2006;75(3):414–20.
Ahmed N, Barker G, Oliva K, Garfin D, Talmadge K, Georgiou H, et al. An approach to remove albumin for the proteomic analysis of low abundance biomarkers in human serum. Proteomics. 2003;3(10):1980–7.
Gupta N, Shankernarayan NP, Dharmalingam K. Serum proteome of leprosy patients undergoing erythema nodosum leprosum reaction: regulation of expression of the isoforms of haptoglobin. J Proteome Res. 2007;6(9):3669–79.
Liu AX, He WH, Yin LJ, Lv PP, Zhang Y, Sheng JZ, et al. Sustained endoplasmic reticulum stress as a cofactor of oxidative stress in decidual cells from patients with early pregnancy loss. J Clin Endocrinol Metab. 2011;96(3):E493–7.
Swain M, Ross NW. A silver stain protocol for proteins yielding high resolution and transparent background in sodium dodecyl sulfate-polyacrylamide gels. Electrophoresis. 1995;16(6):948–51.
Fahiminiya S, Reynaud K, Labas V, Batard S, Chastant-Maillard S, Gerard N. Steroid hormones content and proteomic analysis of canine follicular fluid during the preovulatory period. Reprod Biol Endocrinol. 2010;8:132.
Hu XL, Feng C, Lin XH, Zhong ZX, Zhu YM, Lv PP, et al. High maternal serum estradiol environment in the first trimester is associated with the increased risk of small-for-gestational-age birth. J Clin Endocrinol Metab. 2014;99:2217–24.
Aanesen A, Nygren KG, Nylund L. Modified natural cycle IVF and mild IVF: a 10 year Swedish experience. Reprod Biomed Online. 2010;20(1):156–62.
Gordon JD, DiMattina M, Reh A, Botes A, Celia G, Payson M. Utilization and success rates of unstimulated in vitro fertilization in the United States: an analysis of the Society for Assisted Reproductive Technology database. Fertil Steril. 2013;100(2):392–5.
Murdoch WJ, Murphy CJ, Van Kirk EA, Shen Y. Mechanisms and pathobiology of ovulation. Soc Reprod Fertil Suppl. 2010;67:189–201.
Orvieto R, Chen R, Ashkenazi J, Ben-Haroush A, Bar J, Fisch B. C-reactive protein levels in patients undergoing controlled ovarian hyperstimulation for IVF cycle. Hum Reprod. 2004;19(2):357–9.
Jarkovska K, Kupcova Skalnikova H, Halada P, Hrabakova R, Moos J, Rezabek K, et al. Development of ovarian hyperstimulation syndrome: interrogation of key proteins and biological processes in human follicular fluid of women undergoing in vitro fertilization. Mol Hum Reprod. 2011;17(11):679–92.
Estes SJ, Ye B, Qiu W, Cramer D, Hornstein MD, Missmer SA. A proteomic analysis of IVF follicular fluid in women < or = 32 years old. Fertil Steril. 2009;92(5):1569–78.
Hanrieder J, Nyakas A, Naessén T, Bergquist J. Proteomic analysis of human follicular fluid using an alternative bottom-up approach. J Proteome Res. 2008;7(1):443–9.
Kim YS, Kim MS, Lee SH, Choi BC, Lim JM, Cha KY, et al. Proteomic analysis of recurrent spontaneous abortion: Identification of an inadequately expressed set of proteins in human follicular fluid. Proteomics. 2006;6(11):3445–54.
Aune B, Høie KE, Oian P, Holst N, Osterud B. Does ovarian stimulation for in-vitro fertilization induce a hypercoagulable state? Hum Reprod. 1991;6(7):925–7.
Andersen CY. Characteristics of human follicular fluid associated with successful conception after in vitro fertilization. J Clin Endocrinol Metab. 1993;77(5):1227–34.
Bianchi L, Gagliardi A, Campanella G, Landi C, Capaldo A, Carleo A, et al. A methodological and functional proteomic approach of human follicular fluid en route for oocyte quality evaluation. J Proteomics. 2013;90:61–76.
Dai G, Lu G. Different protein expression patterns associated with polycystic ovary syndrome in human follicular fluid during controlled ovarian hyperstimulation. Reprod Fertil Dev. 2012;24(7):893–904.
Nagy B, Pulay T, Szarka G, Csomor S. The serum protein content of human follicular fluid and its correlation with the maturity of oocytes. Acta Physiol Hung. 1989;73(1):71–5.
Imoedemhe D, Shaw R. Follicular fluid alpha 1-antitrypsin–correlation with fertilizing capacity of oocytes. Br J Obstet Gynaecol. 1986;93(8):863–8.
Meng QX, Gao HJ, Xu CM, Dong MY, Sheng X, Sheng JZ, et al. Reduced expression and function of aquaporin-3 in mouse metaphase-II oocytes induced by controlled ovarian hyperstimulation were associated with subsequent low fertilization rate. Cell Physiol Biochem. 2008;21(1–3):123–8.
Angelucci S, Ciavardelli D, Di Giuseppe F, Eleuterio E, Sulpizio M, Tiboni GM, et al. Proteome analysis of human follicular fluid. Biochim Biophys Acta. 2006;1764(11):1775–85.
Aleshire SL, Osteen KG, Maxson WS, Entman SS, Bradley CA, Parl FF. Localization of transferrin and its receptor in ovarian follicular cells: morphologic studies in relation to follicular development. Fertil Steril. 1989;51(3):444–9.
Briggs DA, Sharp DJ, Miller D, Gosden RG. Transferrin in the developing ovarian follicle: evidence for de-novo expression by granulosa cells. Mol Hum Reprod. 1999;5(12):1107–14.
Li YD, Zhang ZW, Li WX. Transferrin inhibits aromatase activity of rat granulosa cells in vitro. J Endocrinol. 1991;131(2):245–50.
Kawano Y, Narahara H, Miyamura K, Mifune K, Miyakawa I. Inhibitory effect of transferrin on progesterone production in the granulosa cell of humans in vivo and porcine granulosa cell in vitro. Gynecol Obstet Invest. 1995;40(1):1–4.
Ducolomb Y, Gonzalez-Marquez H, Fierro R, Jimenez I, Casas E, Flores D, et al. Effect of porcine follicular fluid proteins and peptides on oocyte maturation and their subsequent effect on in vitro fertilization. Theriogenology. 2013;79(6):896–904.
Entman SS, Maxson WS, Bradley CA, Osteen K, Webster BW, Vaughn WK, et al. Follicular fluid transferrin levels in preovulatory human follicles. J In Vitro Fert Embryo Transf. 1987;4(2):98–102.
Revelli A, Chiado A, Dalmasso P, Stabile V, Evangelista F, Basso G, et al. “Mild” vs. “long” protocol for controlled ovarian hyperstimulation in patients with expected poor ovarian responsiveness undergoing in vitro fertilization (IVF): a large prospective randomized trial. J Assist Reprod Genet. 2014;31(7):809–15.
von Wolff M, Kollmann Z, Fluck CE, Stute P, Marti U, Weiss B, et al. Gonadotrophin stimulation for in vitro fertilization significantly alters the hormone milieu in follicular fluid: a comparative study between natural cycle IVF and conventional IVF. Hum Reprod. 2014;29(5):1049–57.
Acknowledgments
This work was supported by research grants from the National Science & Technology Pillar Program during the 12th Five-year Plan Period of China (No. 2012BAI32B04) and the Zhejiang Provincial Natural Science Foundation of China (No. LY13H040002).
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
Capsule
To study the effect in the follicular milieu of ovarian stimulation versus no stimulation, we analyzed protein expression profiles of follicular fluid from six women undergoing COH IVF and another six with natural cycles using two-dimensional gel electrophoresis. Eight differentially expressed proteins were identified and related to immune and inflammatory responses in the ovary.
Rights and permissions
About this article
Cite this article
Wu, YT., Wu, Y., Zhang, JY. et al. Preliminary proteomic analysis on the alterations in follicular fluid proteins from women undergoing natural cycles or controlled ovarian hyperstimulation. J Assist Reprod Genet 32, 417–427 (2015). https://doi.org/10.1007/s10815-014-0419-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-014-0419-5