Abstract
This study evaluated the effectiveness of Bedtime Fading with Response Cost (BFRC) in decreasing sleep disturbances in children with Autism Spectrum Disorder (ASD) using parents as change agents by implementing treatment in the home environment. A non-concurrent multiple baseline design across three participants was used. Results indicate that BFRC was effective in eliminating unwanted co-sleeping, frequent night awakenings, and dependent sleep onset. Secondary improvements include reducing sleep onset latency, bedtime resistance, and disruptive sleep-related behaviors. Follow-up data demonstrate gains were maintained. Parents reported high satisfaction with BFRC and sleep outcomes for their children. This study extends both the practice and science of parent-implemented behavioral interventions as treatment options for children with ASD and co-occurring sleep disturbances.








Similar content being viewed by others
Change history
16 August 2018
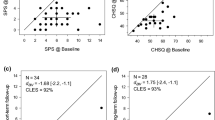
The original version of this article unfortunately contained errors. The errors induced during the production process are corrected. The correct keywords, figures and tables are given below.
References
Adams, H. L., Matson, J. L., & Jang, J. (2014). The relationship between sleep problems and challenging behavior among children and adolescents with autism spectrum disorder. Research in Autism Spectrum Disorders, 8, 1024–1030. https://doi.org/10.1016/j.rasd.2014.05.008.
Aili, K., Astrom-Paulsson, S., Stoetzer, U., Svartengren, M., & Hillert, L. (2017). Reliability of actigraphy and subjective sleep measurements in adults: the design of sleep assessments. Journal of Clinical Sleep Medicine, 13, 39–47. https://doi.org/10.5664/jcsm.6384.
Allen, K. D., Kuhn, B. R., DeHaai, K. A., & Wallace, D. P. (2013). Evaluation of a behavioral treatment package to reduce sleep problems in children with angelman syndrome. Research in Developmental Disabilities, 34, 676–686. https://doi.org/10.1016/j.ridd.2012.10.001.
American Psychiatric Association. (2013). Diagnostic and statistical manual of mental disorders (5th edn.). Arlington, VA: American Psychiatric Publishing.
Anders, T. F., Iosif, A., Schwichtenberg, A. J., Tang, K., & Goodlin-Jones, B. L. (2011). Six month sleep-wake organization and stability in preschool-age children with autism, developmental delay, and typical development. Behavioral Sleep Medicine, 9, 92–106. https://doi.org/10.1080/15402002.2011.557991.
Ashbaugh, R., & Peck, S. M. (1998). Treatment of sleep problems in a toddler: A replication of the faded bedtime with response cost protocol. Journal of Applied Behavior Analysis, 31, 127–129. https://doi.org/10.1901/jaba.1998.31-127.
Bellanger, M. E., Bernier, A., Paquet, J., Simard, V., & Carrier, J. (2013). Validating actigraphy as a measure of sleep for preschool children. Journal of Clinical Sleep Medicine, 9, 701–706. https://doi.org/10.1080/15374416.2015.1079782.
Burke, R. V., Kuhn, B. R., & Peterson, J. L. (2004). Brief report: a ‘storybook’ ending to children’s bedtime problems—the use of a rewarding social story to reduce bedtime resistance and frequent night waking. Journal of Pediatric Psychology, 29, 389–396. https://doi.org/10.1093/jpepsy/jsh042.
Center for Disease Control and Prevention (CDC). (2016). Prevalence and characteristics of autism spectrum disorder among children aged 8 years—autism and developmental disabilities monitoring network, 11 sites, United States, 2012. Morbidity and Mortality Weekly Report. Retrieved from https://www.cdc.gov/mmwr/volumes/65/ss/ss6503a1.htm.
Christodulu, K. V., & Durand, V. M. (2004). Reducing bedtime disturbances and night waking using positive bedtime routines and sleep restriction. Focus on Autism and Other Developmental Disabilities, 19, 130–139. https://doi.org/10.1177/10883576040190030101.
Corkum, P., Tannock, R., Moldofsky, H., Hogg-Johnson, S., & Humphries, T. (2001). Actigraphy and parental ratings of sleep in children with attention-deficit/hyperactivity disorder (ADHD). Sleep, 24, 303–312. https://doi.org/10.1586/ern.11.7.
Crane, D. R., Middleton, K. C., & Bean, R. A. (2000). Establishing criterion scores for the Kansas marital satisfaction scale and the revised dyadic adjustment scale. The American Journal of Family Therapy, 28, 53–60. https://doi.org/10.1080/019261800261815.
DeLeon, I., Fisher, W., & Marhefka, J. (2004). Decreasing self-injurious behavior associated with awakening in a child with autism and developmental delays. Behavioral Interventions, 19, 111–119. https://doi.org/10.1002/bin.154.
Deliens, G., Leproult, R., Schmitz, R., Destrebecqz, A., & Peigneux, P. (2015). Sleep disturbances in autism spectrum disorders. Review Journal of Autism and Developmental Disorders, 2, 343–356. https://doi.org/10.1007/s40489-015-0057-6.
Dominick, K. C., Ornstein Davis, N., Lainhart, J., Tager-Flusberg, H., & Folstein, S. (2007). Atypical behaviors in children with autism and children with a history of language impairment. Research in Developmental Disabilities, 28, 145–162. https://doi.org/10.1016/j.ridd.2006.02.003.
Durand, V. M. (2002). Treating sleep terrors in children with autism. Journal of Positive Behavior Interventions, 4, 66–72. https://doi.org/10.1177/109830070200400201.
Durand, V. M., & Christodulu, K. V. (2004). A description of a sleep restriction program to reduce bedtime disturbances and night waking. Journal of Positive Behavioral Interventions, 6, 83–91. https://doi.org/10.1177/10983007040060020301.
Durand, V. M., Gernert-Dott, P., & Mapstone, E. (1996). Treatment of sleep disorders in children with developmental disabilities. The Journal of the Association for Persons with Severe Handicaps, 21, 114–122. https://doi.org/10.1177/154079699602100302.
Durand, V. M., & Mindell, J. A. (1999). Behavioral intervention for childhood sleep terrors. Behavior Therapy, 30, 705–715.
Fisman, S. N., Wolf, L. C., & Noh, S. (1989). Marital intimacy in parents of exceptional children. Canadian Journal of Psychiatry, 34, 519–525.
Friedman, A., & Luiselli, J. K. (2008). Excessive daytime sleep: Behavioral assessment and intervention in a child with autism. Behavior Modification, 32, 548–555. https://doi.org/10.1177/0145445507312187.
Goldman, S. E., Alder, M. L., Burgess, H. J., Corbett, B. A., Hundley, R., Wofford, D., Fawkes, D. B., Wang, L., Laudenslager, M. L., & Malow, B. A. (2017). Characterizing sleep in adolescents and adults with autism spectrum disorders. Journal of Autism and Developmental Disorders, 47, 1682–1695. https://doi.org/10.1007/s10803-017-3089-1.
Goodlin-Jones, B. L., Tang, K., Liu, J. Y., & Anders, T. F. (2008). Sleep patterns in preschool-age children with autism, developmental delay, and typical development. Journal of the American Academy of Child and Adolescent Psychiatry, 47, 930–938. https://doi.org/10.1097/CHI.0b013e3181799f/c.
Gotham, K., Risi, S., Pickles, A., & Lord, C. (2007). The autism diagnostic observation schedule: Revised algorithms for improved diagnostic validity. Journal of Autism and Developmental Disorders, 37, 613–627. https://doi.org/10.1007/s10803-006-0280-1.
Harvey, M. T., May, M. E., & Kennedy, C. H. (2004). Nonconcurrent multiple baseline design and the evaluation of educational systems. Journal of Behavioral Education, 13, 267–276.
Hirshkowitz, M., Whiton, K., Albert, S. M., Alessi, C., Bruni, O., DonCarlos, L., et al. (2015). National sleep foundation’s sleep time duration recommendations: methodology and results summary. Sleep Health, 1, 40–43. https://doi.org/10.1016/j.sleh.2014.12.010.
Hodge, D., Carollo, T. M., Lewin, M., Hoffman, C. D., & Sweeney, D. P. (2014). Sleep patterns in children with an without autism spectrum disorders: Developmental comparisons. Research in Developmental Disabilities, 35, 1631–1638. https://doi.org/10.1016/j.ridd.2014.03.037.
Hoffman, C. D., Sweeney, D. P., Lopez-Wagner, M. C., Hodge, D., Nam, C. Y., & Botts, B. H. (2008). Children with autism, sleep problems and mothers’ stress. Focus on Autism and Other Disabilities, 23, 155–165. https://doi.org/10.1177/1088357608316271.
Holley, S., Hill, C. M., & Stevenson, J. (2010). A comparison of actigraphy and parental report of sleep habits in typically developing children aged 6 to 11 years. Behavioral Sleep Medicine, 8, 16–27. https://doi.org/10.1080/15402000903425462.
Howlin, P. (1984). A brief report on the elimination of long tern sleeping problems in a 6-year-old autistic boy. Behavioural Psychotherapy, 12, 257–260. https://doi.org/10.1017/S014134730001082X.
Hudson, A., Wilken, P., Jauering, R., & Raddler, G. (1995). Regionally based teams for the treatment of challenging behavior: A three year outcome study. Behavior Change, 12, 209–215. https://doi.org/10.1017/S081348390000406X.
Iglowstein, I., Jenni, O. G., Molinari, L., & Largo, R. H. (2003). Sleep duration from infancy to adolescence: Reference values and generational trends. Pediatrics, 111, 302–307. https://doi.org/10.1542/peds.111.2.302.
Jin, C. S., Hanley, G. P., & Beauliue, L. (2013). An individualized and comprehensive approach to treating sleep problems in young children. Journal of Applied Behavior Analysis, 46, 161–180. https://doi.org/10.1002/jaba.16.
Knight, R. M., & Johnson, C. M. (2014). Using a behavioral treatment package for sleep problems in children with autism spectrum disorders. Child & Family Behavior Therapy, 36, 204–221. https://doi.org/10.1080/07317107.2014.934171.
Krakowiak, P., Goodlin-Jones, B., Hertz-Picciotto, I., Croen, L. A., & Hansen, R. L. (2008). Sleep problems in children with autism spectrum disorders, developmental delays, and typical development: A population-based study. Journal of Sleep Research, 17, 197–206. https://doi.org/10.1111/j.1365-2869.2008.00650.x.
Kurdek, L. A. (2002). Predicting the timing of separation and marital satisfaction: An eight-year prospective longitudinal study. Journal of Marriage and the Family, 64, 163–179. https://doi.org/10.1111/j.1741-3737.2002.00163x.
Kushnir, J., & Sadeh, A. (2013). Correspondence between reported and actigraphic sleep measures in preschool children: The role of a clinical context. Journal of Clinical Sleep Medicine, 9, 1147–1151. https://doi.org/10.5664/jcsm.3154.
Lam, J. C., Mahone, E. M., Mason, T. B., & Scharf, S. M. (2011). Defining the roles of actigraphy and parent logs for assessing sleep variables in preschool children. Behavioral Sleep Medicine, 9, 184–193. https://doi.org/10.1080/15402002.2011.583906.
Levin, A., & Scher, A. (2016). Sleep problems in young children with autism spectrum disorders: A study of parenting stress, mothers’ sleep-related cognitions, and bedtime behaviors. CNS Neuroscience & Therapeutics, 22, 921–927. https://doi.org/10.1111/cns.12651.
Lord, C., Rutter, M., DiLavore, P. C., Risi, S., Gotham, K., & Bishop, S. (2012). Autism diagnostic observation schedule (2nd edn). Torrance, CA: Western Psychological Services.
Malow, B., Adkins, K. W., Reynolds, A., Weiss, S. K., Loh, A., Fawkes, D., et al. (2014). Parent-based sleep education for children with autism spectrum disorders. Journal of Autism and Developmental Disorders, 44, 216–228. https://doi.org/10.1007/s10803-013-1866-z.
Mandell, D. S., Morales, K. H., Marcus, S. C., Stahmer, A. C., Doshi, J., & Polsky, D. E. (2008). Psychotropic medication use among Medicaid-enrolled children with autism spectrum disorder. Pediatrics, 121, 441–448.
Mazurek, M. O., & Sohl, K. (2016). Sleep and behavioral problems in children with autism spectrum disorder. Journal of Autism and Developmental Disorders, 46, 1906–1915. https://doi.org/10.1007/s10803-016-2723-7.
McMahon, R. J., & Forehand, R. L. (2003). Parent’s consumer satisfaction questionnaire. Adapted from helping the noncompliant child (2nd edn.). New York: The Guildford Press.
Meltzer, L. J. (2011). Factors associated with depressive symptoms in parents of children with autism spectrum disorders. Research in Autism Spectrum Disorders, 5, 361–367. https://doi.org/10.1016/j.rasd.2010.05.001.
Meltzer, L. J., Montgomery-Downs, H. E., Insana, S. P., & Walsh, C. M. (2012). Use of actigraphy for assessment in pediatric sleep research. Sleep Medicine Reviews, 16, 463–475. https://doi.org/10.1016/j.smrv.2011.10.002.
Mihaila, I., & Hartley, S. L. (2016). Parental sleep quality and behavior problems of children with autism. Autism. https://doi.org/10.1177/1362361316673570.
Mindell, J. A., & Durand, V. M. (1993). Treatment of childhood sleep disorders: Generalization across disorders and effects on family members. Journal of Pediatric Psychology, 18, 731–750.
Montgomery, P., Stores, G., & Wiggs, L. (2004). The relative efficacy of two brief treatments for sleep problems in young learning disabled (mentally retarded) children: A randomized controlled trial. Archives of Disease in Childhood, 89, 125–130. https://doi.org/10.1136/adc.2002.017202.
Moon, E. C., Corkum, P., & Smith, I. M. (2010). Case study: A case-series evaluation of a behavioral sleep intervention for three children with autism and primary insomnia. Journal of Pediatric Psychology. https://doi.org/10.1093/jpepsy/jsq057.
Owens, J. A., Spirito, A., & McGuinn, M. (2000). The children’s sleep habits questionnaire (CSHQ): Psychometric properties of a survey instrument for school aged children. Sleep, 23, 1043–1051.
Owens, J. A., & Whitmans, M. (2004). Sleep problems. Current Problems in Pediatric & Adolescent Health Care, 34, 154–179.
Patzold, L. M., Richdale, A. L., & Tonge, B. J. (1998). An investigation into sleep characteristics of children with autism and asperger’s disorder. Journal of Paediatrics and Child Health, 34, 528–533.
Piazza, C. C., & Fisher, W. W. (1991a). Bedtime fading in the treatment of pediatric insomnia. Journal of Behavior, Therapy, & Experimental Psychiatry, 22, 53–56. https://doi.org/10.1016/0005-7916(91)90034-3.
Piazza, C. C., & Fisher, W. W. (1991b). A faded bedtime with response cost protocol for treatment of multiple sleep problems in children. Journal of Applied Behavior Analysis, 24, 129–140. https://doi.org/10.1901/jaba.1991.24-129.
Piazza, C. C., Fisher, W. W., & Moser, H. (1991). Behavioral treatment of sleep dysfunction on patients with the rett syndrome. Brain & Development, 13, 232–237.
Piazza, C. C., Fisher, W. W., & Sherer, M. (1997). Treatment of multiple sleep problems in children with developmental disabilities: Faded bedtime with response cost versus bedtime scheduling. Developmental Medicine & Child Neurology, 39, 414–418.
Piazza, C. C., Hagopian, L. P., Hughes, C. R., & Fisher, W. W. (1998). Using chronotherapy to treat severe sleep problems: A case study. American Journal on Mental Retardation, 102, 358–366.
Reed, H. E., McGrew, S. G., Artibee, K., Surdkya, K., Goldman, S. E., Frank, K., Wang, L., & Malow, B. A. (2009). Parent-based sleep education workshops in autism. Journal of Child Neurology, 24, 936–945. https://doi.org/10.1177/0883073808331348.
Reynolds, A. M., & Malow, B. A. (2011). Sleep and autism spectrum disorders. Pediatric Clinics of North America, 58, 685–698. https://doi.org/10.1016/j.pcl.2011.03.009.
Sadeh, A. (2011). The role and validity of actigraphy in sleep medicine: An update. Sleep Medicine Reviews, 15, 259–267.
Sadeh, A., Sharkey, K. M., & Carskadon, M. A. (1994). Activity-based sleep wake identification: An empirical test of methodological issues. Sleep, 17, 201–217.
Schopler, E., Van Bourgondien, M. E., Wellman, G. J., & Love, S. R. (2010). Childhood autism rating scale (2nd edn.). Los Angeles, CA: Western Psychological Services.
Schreck, K. A., & Mulick, J. A. (2000). Parental report of sleep problems in children with autism. Journal of Autism and Developmental Disabilities, 30, 127–135.
Schumm, W. A., Nicholas, C. W., Schectman, K. L., & Grigsby, C. C. (1983). Characteristics of response to the Kansas Marital Satisfaction Scale by a sample of 84 married mothers. Psychological Reports, 53, 567–572.
Spencer, D., Marshall, J., Post, B., Kulakodlu, M., Newschaffer, C., Dennen, T., Azocar, F., & Jain, A. (2013). Psychotropic medication use and polypharmacy in children with autism spectrum disorders. Pediatrics, 138, 833–840.
Tilford, M. J., Payakachat, N., Kuhlthau, K. A., Pyne, J. M., Kovacs, E., Bellando, J., et al. (2015). Treatment for sleep problems in children with autism and caregiver spillover effects. Journal of Autism and Developmental Disorders, 45, 3613–3623. https://doi.org/10.1007/s10803-015-2507-5.
Vollmer, T. R., Sloman, K. N., & St. Peter Pipkin, C. (2008). Practical implications of data reliability and treatment integrity monitoring. Behavior Analysis in Practice, 1, 4–11.
Watson, P. J., & Workman, E. A. (1981). The non-concurrent multiple baseline across-individuals design: An extension of the traditional multiple baseline design. Journal of Behavior Therapy and Experimental Psychiatry, 12, 257–259. https://doi.org/10.1016/0005-7916(81)90055-0.
Weiskop, S., Matthews, J., & Richdale, A. L. (2001). Treatment of sleep problems in a 5-year-old boy with autism using behavioural principles. Autism, 5, 209–221. https://doi.org/10.1177/1362361301005002009.
Weiskop, S., Richdale, A., & Matthews, J. (2005). Behavioural treatment to reduce sleep problems in children with autism or fragile x syndrome. Developmental Medicine & Child Neurology, 47, 94–104. https://doi.org/10.1017/S0012162205000186.
Wiggs, L., & Stores, G. (2004). Sleep patterns and sleep disorders in children with autistic spectrum disorders: Insights using parent report and actigraphy. Developmental Medicine & Child Neurology, 46, 372–380. https://doi.org/10.1017/S0012162204000611.
Wolf, M., Risley, T., & Mees, H. (1964). Application of operant conditioning procedures to the behavior problems of an autistic child. Behavior Research & Therapy, 1, 305–312.
Acknowledgements
We would like to express our deep gratitude to our colleagues and/or professors, especially Keith D. Allen, Ph.D., BCBA-D; William J. Warzak, Ph.D., BCBA-D; and Holly Roberts, Ph.D., for their guidance, encouragement, and helpful critiques of this work. We are extremely grateful to all those who participated.
Author information
Authors and Affiliations
Contributions
SS conceived of the study, participated in its design and coordination, participated in the measurement and data acquisition, performed the data analysis and interpretation, drafted and revised the manuscript and figures, and has given final approval of the version to be published; BK helped conceive the study, participated in its design, data analysis and interpretation, and manuscript revisions. AK participated in the coordination of the study, performed the measurement and data acquisition, and helped with manuscript revisions.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. This article does not contain any studies with animals performed by any of the authors.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Sanberg, S.A., Kuhn, B.R. & Kennedy, A.E. Outcomes of a Behavioral Intervention for Sleep Disturbances in Children with Autism Spectrum Disorder. J Autism Dev Disord 48, 4250–4277 (2018). https://doi.org/10.1007/s10803-018-3644-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10803-018-3644-4