Abstract
Purpose
To investigate the natural course, visual outcome, and risk factors for visual loss after nonarteritic anterior ischemic optic neuropathy (NAION) attack in Chinese patients from a tertiary medical center in Southern Taiwan.
Methods
This is a longitudinal observational study that included sixty NAION patients, who were seen in our neuro-ophthalmology clinic from 2007 to 2016. Records of their ophthalmic history, medical history, best-corrected visual acuity (BCVA), visual field (VF) testing, and optical coherence tomography (OCT) were obtained for analysis.
Results
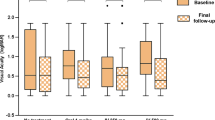
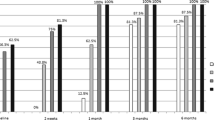
When the first visit was within two weeks after NAION onset, 62% of patients had BCVA of less than 0.1 (logMAR BCVA ≥ 1) and 38% had at least moderate–severe depression (VF grade ≥ 3) on VF on the initial visit. VA stabilized at three months after onset and was predictive of VA at 12 months. Diabetes mellitus was a risk factor associated with VA worsening. Sixty-one percent of patients had BCVA of less than 0.1 at 12 months after onset. VF remained relatively unchanged during the disease, with 41% eyes having VF grade ≥ 3 at 12 months after onset. On OCT, all quadrants of retinal nerve fiber layer thickened initially, returned to the level of the fellow eye at one month, and continued thinning up to 12 months slowly.
Conclusion
In Southern Taiwan, a higher proportion of Chinese patients (over half) presented with severe visual loss during the first two weeks of NAION attack and at 12 months after the onset of NAION as compared to the findings previously reported in Caucasians. Understanding the natural course of NAION in Chinese patients may provide insights toward a possible therapeutic window for NAION treatments in this group of patients.




Similar content being viewed by others
References
Hayreh SS (2013) Ischemic optic neuropathies - where are we now? Graefes Arch Clin Exp Ophthalmol 251(8):1873–1884
Hayreh SS (2009) Ischemic optic neuropathy. Prog Retin Eye Res 28(1):34–62
Johnson LN, Arnold AC (1994) Incidence of nonarteritic and arteritic anterior ischemic optic neuropathy. Population-based study in the state of Missouri and Los Angeles County. California. J Neuroophthalmol 14(1):38–44
Hattenhauer MG, Leavitt JA, Hodge DO, Grill R, Gray DT (1997) Incidence of nonarteritic anterior ischemic optic neuropathy. Am J Ophthalmol 123(1):103–107
Lee YC, Wang JH, Huang TL, Tsai RK (2016) Increased risk of stroke in patients with nonarteritic anterior ischemic optic neuropathy: a nationwide retrospective cohort study. Am J Ophthalmol 170:183–189
Group IONDTR (1996) Characteristics of patients with nonarteritic anterior ischemic optic neuropathy eligible for the Ischemic optic neuropathy decompression trial. Arch Ophthalmol 114(11):1366–1374
Biousse V, Newman NJ (2015) Ischemic optic neuropathies. N Engl J Med 372(25):2428–2436
Hayreh SS, Zimmerman MB (2008) Nonarteritic anterior ischemic optic neuropathy: natural history of visual outcome. Ophthalmology 115(2):298–305
Group IONDTR (2000) Ischemic optic neuropathy decompression trial: twenty-four-month update. Arch Ophthalmol 118(6):793–798
Group IONDTR (1995) Optic nerve decompression surgery for nonarteritic anterior ischemic optic neuropathy (NAION) is not effective and may be harmful. The Ischemic Optic Neuropathy Decompression Trial Research Group. JAMA 273 (8):625–632
Hayreh SS (2004) Posterior ischaemic optic neuropathy: clinical features, pathogenesis, and management. Eye 18(11):1188–1206
Contreras I, Noval S, Rebolleda G, Muñoz-Negrete FJ (2007) Follow-up of nonarteritic anterior ischemic optic neuropathy with optical coherence tomography. Ophthalmology 114(12):2338–2344.e2331
Hayreh SS (1969) Blood supply of the optic nerve head and its role in optic atrophy, glaucoma, and oedema of the optic disc. Br J Ophthalmol 53(11):721–748
Atkins EJ, Bruce BB, Newman NJ, Biousse V (2009) Translation of clinical studies to clinical practice: survey on the treatment of nonarteritic anterior ischemic optic neuropathy. Am J Ophthalmol 148(5):809
Hayreh SS, Zimmerman MB (2008) Nonarteritic anterior ischemic optic neuropathy: clinical characteristics in diabetic patients versus nondiabetic patients. Ophthalmology 115(10):1818–1825
Hayreh SS, Joos KM, Podhajsky PA, Long CR (1994) Systemic diseases associated with nonarteritic anterior ischemic optic neuropathy. Am J Ophthalmol 118(6):766–780
Hayreh SS, Zimmerman MB, Podhajsky P, Alward WLM (1994) Nocturnal arterial hypotension and its role in optic nerve head and ocular ischemic disorders. Am J Ophthalmol 117(5):603–624
Hayreh SS, Podhajsky PA, Zimmerman B (1997) Nonarteritic anterior ischemic optic neuropathy: time of onset of visual loss. Am J Ophthalmol 124(5):641–647
Hayreh SS (1987) Anterior ischemic optic neuropathy. Ophthalmology 94(11):1488–1502
Hayreh SS (2012) Non-arteritic anterior ischemic optic neuropathy versus cerebral ischemic stroke. Graefes Arch Clin Exp Ophthalmol 250(9):1255–1260
Wu Y, Zhou LM, Lou H, Cheng JW, Wei RL (2016) The Association between obstructive sleep apnea and nonarteritic anterior ischemic optic neuropathy: a systematic review and meta-analysis. Curr Eye Res 41(7):987–992
Salomon O, Huna-Baron R, Kurtz S, Steinberg DM, Moisseiev J, Rosenberg N, Yassur I, Vidne O, Zivelin A, Gitel S, Davidson J, Ravid B, Seligsohn U (1999) Analysis of prothrombotic and vascular risk factors in patients with nonarteritic anterior ischemic optic neuropathy. Ophthalmology 106(4):739–742
Arnold AC, Costa RM, Dumitrascu OM (2013) The spectrum of optic disc ischemia in patients younger than 50 years (an Amercian Ophthalmological Society thesis). Trans Am Ophthalmol Soc 111:93–118
Hayreh SS (2001) Blood flow in the optic nerve head and factors that may influence it. Prog Retin Eye Res 20(5):595–624
Lee MS, Grossman D, Arnold AC, Sloan FA (2011) Incidence of nonarteritic anterior ischemic optic neuropathy: increased risk among diabetic patients. Ophthalmology 118(5):959–963
Talks SJ, Chong NHV, Gibson JM, Dodson PM (1995) Fibrinogen, cholesterol and smoking as risk factors for non-arteritic anterior ischaemic optic neuropathy. Eye 9(1):85–88
Acknowledgements
This work was supported by the grant from the Kaohsiung Chang Gung Memorial Hospital and University College of Medicine (CMRPG8F1741; Kaohsiung, Taiwan).
Funding
This study was funded by the grant from the Kaohsiung Chang Gung Memorial Hospital and University College of Medicine (CMRPG8F1741; Kaohsiung, Taiwan).
Author information
Authors and Affiliations
Contributions
All of the authors contributed to study conception and design; HMH, LYCP helped in material preparation, data collection and analysis; HMH contributed to writing the first draft of the manuscript; LYCP helped in reviewing and editing the manuscript; HMH helped in funding acquisition. All authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in the retrospective study involving human participants were in accordance with the ethical standards of the Human Investigation Committee (IRB) of Chang Gung Memorial Hospital and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The Human Investigation Committee (IRB) of Chang Gung Memorial Hospital approved this study (IRB number: 201601055A3.
Informed consent
This retrospective chart review qualifies for exempt status under human subjects regulations and has been approved by the IRB of Chang Gung Memorial Hospital.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Huang, HM., Wu, PC., Kuo, HK. et al. Natural history and visual outcome of nonarteritic anterior ischemic optic neuropathy in Southern Taiwan: a pilot study. Int Ophthalmol 40, 2667–2676 (2020). https://doi.org/10.1007/s10792-020-01448-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-020-01448-8