Abstract
Purpose
To evaluate the quality of life of glaucoma patients using the Ocular Surface Disease Index (OSDI) questionnaire and their association with dry eye clinical signs.
Methods
The study included patients into three groups. The treated group diagnosed with bilateral open-angle glaucoma and treated with one or more topical medication at least 1 year. The operated group underwent glaucoma surgery without the need for topical medications. The control group entered subjects without ocular diseases or previous surgeries. Dry eye clinical signs were evaluated; noninvasive tear break-up time, Meibomian gland depletion (MGD), and conjunctival hyperemia were measured using the Keratograph 5 M. The total-OSDI (T-OSDI) score was divided into the visual field-OSDI and discomfort-OSDI scores.
Results
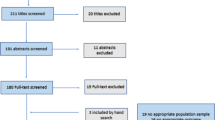
Two hundred and nine subjects participated in this cross-sectional study, 147 using glaucoma medications, 21 patients underwent glaucoma surgery and 41 were controls. The T-OSDI and subscores were higher in glaucoma patients compared with controls (p < 0.05); we found no differences between treated and surgically groups. Correlations were observed between the T-OSDI values and Schirmer test (p = 0.016), ocular surface staining (p < 0.001) and the MGD (p = 0.006). The subscores were associated with the ocular surface staining (VF p = 0.013 and D p = 0.003). In treated patients, the number of drops per day correlates with T-OSDI and subscores (p = 0.017 and p = 0.005).
Conclusion
OSDI scores increased in the glaucoma patients compared to controls without significant changes between treated and surgical patients. OSDI scores were associated to dry eye signs and medication in glaucoma patients.

Similar content being viewed by others
References
Nirmalan PK, Tielsch JM, Katz J et al (2005) Relationship between vision impairment and eye disease to vision-specific quality of life and function in rural India: the Aravind Comprehensive Eye Survey. Investig Ophthalmol Vis Sci 46:2308–2312
Broman AT, Munoz B, Rodriguez J et al (2002) The impact of visual impairment and eye disease on vision-related quality of life in a Mexican-American population: proyecto VER. Investig Ophthalmol Vis Sci 43:3393–3398
Knudtson MD, Klein BE, Klein R et al (2005) Age-related eye disease, quality of life, and functional activity. Arch Ophthalmol 123:807–814. https://doi.org/10.1001/archopht.123.6.807
Takahashi G, Otori Y, Urashima M et al (2016) Evaluation of quality of life in Japanese glaucoma patients and its relationship with visual function. J Glaucoma 25:e150–e156. https://doi.org/10.1097/IJG.0000000000000221
Sun Y, Lin C, Waisbourd M et al (2016) The impact of visual field clusters on performance-based measures and vision-related quality of life in patients with glaucoma. Am J Ophthalmol 163:45–52. https://doi.org/10.1016/j.ajo.2015.12.006
Gracitelli CP, Abe RY, Tatham AJ et al (2015) Association between progressive retinal nerve fiber layer loss and longitudinal change in quality of life in glaucoma. JAMA Ophthalmol 133:384–390. https://doi.org/10.1001/jamaophthalmol.2014.5319
Abe RY, Diniz-Filho A, Costa VP et al (2016) The impact of location of progressive visual field loss on longitudinal changes in quality of life of patients with glaucoma. Ophthalmology 123:552–557. https://doi.org/10.1016/j.ophtha.2015.10.046
Campbell MK, Bush TL, Hale WE (1993) Medical conditions associated with driving cessation in community-dwelling, ambulatory elders. J Gerontol 48:S230–S234
Ramulu PY, West SK, Munoz B et al (2009) Driving cessation and driving limitation in glaucoma: the Salisbury Eye Evaluation Project. Ophthalmology 116:1846–1853. https://doi.org/10.1016/j.ophtha.2009.03.033
Freeman EE, Munoz B, Rubin G, West SK (2007) Visual field loss increases the risk of falls in older adults: the Salisbury eye evaluation. Investig Ophthalmol Vis Sci 48:4445–4450
Lee BL, Wilson MR (2000) Health-related quality of life in patients with cataract and glaucoma. J Glaucoma 9:87–94
Janz NK, Wren PA, Guire KE et al (2007) Fear of blindness in the Collaborative Initial Glaucoma Treatment Study: patterns and correlates over time. Ophthalmology 114:2213–2220
Rossi GCM, Tinelli C, Pasinetti GM et al (2009) Dry eye syndrome-related quality of life in glaucoma patients. Eur J Ophthalmol 19:572–579
Jaenen N, Baudouin C, Pouliquen P et al (2007) Ocular symptoms and signs with preserved and preservative-free glaucoma medications. Eur J Ophthalmol 17:341–349
Cvenkel B, Stunf S, Kirbis IS, Flezar MS (2015) Symptoms and signs of ocular surface disease related to topical medication in patients with glaucoma. Clin Ophthalmol 9:625–631. https://doi.org/10.2147/OPTH.S81247
Leung EW, Medeiros FA, Weinreb RN (2008) Prevalence of ocular surface disease in glaucoma patients. J Glaucoma 17:350–355. https://doi.org/10.1097/IJG.0b013e31815c5f4f
Bron AJ et al (2007) Methodologies to diagnose and monitor dry eye disease: report of the Diagnostic Methodology Subcommittee of the International Dry Eye WorkShop (2007). Ocul Surf 5:108–152
Schiffman RM, Christianson MD, Jacobsen G et al (2000) Reliability and validity of the Ocular Surface Disease Index. Arch Ophthalmol 118:615–621
Mathews PM, Ramulu PY, Friedman DS et al (2013) Evaluation of ocular surface disease in patients with glaucoma. Ophthalmology 120:2241–2248. https://doi.org/10.1016/j.ophtha.2013.03.045
Bron AJ, Evans VE, Smith JA (2003) Grading of corneal and conjunctival staining in the context of other dry eye tests. Cornea 22:640–650
Mengher LS, Pandher KS, Bron AJ (1986) Topical anaesthetic and tear film stability. Acta Ophthalmol 64:79–82
Mengher LS, Bron AJ, Tonge SR, Gilbert DJ (1985) Effect of fluorescein instillation on the pre-corneal tear film stability. Curr Eye Res 4:9–12
Lemij HG, Hoevenaars JG, van der Windt C et al (2015) Patient satisfaction with glaucoma therapy: reality or myth? Clin Ophthalmol 9:785–793. https://doi.org/10.2147/OPTH.S78918
Fechtner RD, Godfrey DG, Budenz D et al (2010) Prevalence of ocular surface complaints in patients with glaucoma using topical intraocular pressure-lowering medications. Cornea 29:618–621. https://doi.org/10.1097/ICO.0b013e3181c325b2
Arita R, Itoh K, Maeda S et al (2012) Effects of long-term topical anti-glaucoma medications on meibomian glands. Graefe’s Arch Clin Exp Ophthalmol 250:1181–1185. https://doi.org/10.1007/s00417-012-1943-6
Arita R, Itoh K, Maeda S et al (2012) Comparison of the long-term effects of various topical antiglaucoma medications on meibomian glands. Cornea 31:1229–1234. https://doi.org/10.1097/ICO.0b013e31823f8e7d
Terai N, Müller-Holz M, Spoerl E, Pillunat LE (2011) Short-term effect of topical antiglaucoma medication on tear-film stability, tear secretion, and corneal sensitivity in healthy subjects. Clin Ophthalmol. https://doi.org/10.2147/OPTH.S18849
Lee SY, Wong TT, Chua J et al (2013) Effect of chronic anti-glaucoma medications and trabeculectomy on tear osmolarity. Eye 27:1142–1150. https://doi.org/10.1038/eye.2013.144
Budenz DL, Hoffman K, Zacchei A (2001) Glaucoma filtering bleb dysesthesia. Am J Ophthalmol 131:626–630
Neves Mendes CR, Hida RY, Kasahara N (2012) Ocular surface changes in eyes with glaucoma filtering blebs. Curr Eye Res 37:309–311. https://doi.org/10.3109/02713683.2011.635400
Sagara H, Iida T, Saito K et al (2012) Conservative treatment for late-onset bleb leaks after trabeculectomy with mitomycin C in patients with ocular surface disease. Clin Ophthalmol 6:1273–1279. https://doi.org/10.2147/OPTH.S33427
Sagara H, Sekiryu T, Noji H et al (2015) Treatment with sodium hyaluronate eye drops in a patient who had early-onset bleb leakage after trabeculectomy with mitomycin C. Int Med Case Rep J 8:301–304. https://doi.org/10.2147/IMCRJ.S95334
Wang X, Lu X, Yang J et al (2016) Evaluation of dry eye and meibomian gland dysfunction in teenagers with myopia through noninvasive keratograph. J Ophthalmol 2016:6761206. https://doi.org/10.1155/2016/6761206
de Paiva CS (2017) Effects of aging in dry eye. Int Ophthalmol Clin 57:47–64. https://doi.org/10.1097/IIO.0000000000000170
Saade CE, Lari HB, Berezina TL et al (2015) Topical glaucoma therapy and ocular surface disease: a prospective, controlled cohort study. Can J Ophthalmol 50:132–136. https://doi.org/10.1016/j.jcjo.2014.11.006
Funding
Supported in part by Instituto de Salud Carlos III, “Red temática de Investigación Cooperativa, RETICS RD12/0034/0013 Enfermedades oculares: “Prevención, detección precoz, tratamiento y rehabilitación de las patologías oculares”. Supported in part by Instituto de Salud Carlos III, Subvenciones de la Acción Estratégica en Salud 2013–2016, del Programa Estatal de Investigación Orientad, Project PI14/00811.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee (Ethic Committee of Clinical Investigation of Navarra) and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
It was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Guarnieri, A., Carnero, E., Bleau, AM. et al. Relationship between OSDI questionnaire and ocular surface changes in glaucomatous patients. Int Ophthalmol 40, 741–751 (2020). https://doi.org/10.1007/s10792-019-01236-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-019-01236-z