Abstract
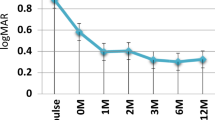
To study the efficacy of systemic steroids (SS) associated with mycophenolate mofetil (MMF) for the control of juxta/sub-foveal uveitic choroidal neovascularization (CNV) unresponsive to the traditional immunosuppressive agents. Patients with juxta/sub-foveal uveitic CNV unresponsive to the traditional immunesuppressive drugs were treated with SS and MMF. The study was designed as a prospective, consecutive, open-label, interventional case series. Visual gain and loss were defined as improving or worsening of two or more lines of best-corrected visual acuity (BCVA), respectively. CNV size outcome was dichotomized as “increased” or “stable/reduced”, if increased >200 μm2, or reduced ≥200 μm2 or not modified by 200 μm2, respectively. Nine cases (12 eyes) have been considered; ages ranged from 27 to 56 years. The mean follow-up time was 18.2 ± 2.9 months (min: 14 months, max: 23 months). At base-line, the mean BCVA was 0.3 ± 0.17, improving up to 0.57 ± 0.25 and to 0.63 ± 0.22 (P < 0.001, paired t-test) at the 6 and 12-month follow-ups, respectively. At the last follow-up, all the patients had stable/improved BCVA (P < 0.0001, Fisher’s exact test) and stable/reduced lesion size (P < 0.0001, Fisher’s exact test). None of the patients complained of any severe adverse event during the treatment. The combination of SS and MMF seems to be a promising strategy in order to control uveitic CNVs unresponsive to the traditional immunosuppressive agents. Further studies are needed to validate the data of this case series.



Similar content being viewed by others
References
Parvan PR, Margo CE (1996) Submacular neovascular membrane and focal granulomatous inflammation. Ophthalmology 103:586–589
Forrester JV, Liversidge J, Dua HS et al (1990) Comparison of clinical experimental uveitis. Curr Eye Res 9:75–84
Okada AA, Wakabayashi T, Kojima E et al (2004) Trans-tenon’s retrobulbar triamcinolone infusion for small choroidal neovascularization. Br J Ophthalmol 88:1097–1098
Flaxel CJ, Owens SL, Mulholland B et al (1998) The use of corticosteroids for choroidal neovascularization in young patients. Eye 12(Pt 2):266–272
Lim JI, Flaxel CJ, LaBree L (2006) Photodynamic therapy for choroidal neovascularisation secondary to inflammatory chorioretinal disease. Ann Acad Med Singap 35(3):198–202
Gerth C, Spital G, Lommatzsch A, Heiligenhaus A, Pauleikhoff D (2006) Photodynamic therapy for choroidal neovascularization in patients with multifocal choroiditis and panuveitis. Eur J Ophthalmol 16(1):111–118
Lit ES, Kim RY, Damico DJ (2001) Surgical removal of subfoveal choroidal neovascularization without removal of posterior hyaloid: a consecutive series in younger patients. Retina 21(4):317–323
Vitale AT, Foster CS (2002) Corticosteroids. In: Foster CS, Vitale AT (eds) Diagnosis and treatment of uveitis. Philadelphia, W.B. Saunders Company, pp 142–158
Ferrante P, Ramsey A, Bunce C, Lightman S (2004) Clinical trial to compare efficacy and side-effects of injection of posterior sub-tenon triamcinolone versus orbital floor methylprednisolone in the management of posterior uveitis. Clin Exp Ophthalmol 32:563–568
Wang JJ, Rochtchina E, Tan AG, Cumming RG, Leeder SR, Mitchell P (2009) Use of inhaled and oral corticosteroids and the long-term risk of cataract. Ophthalmology 116(4):652–657
Neri P, Azuara-Blanco A, Forrester JV (2004) Incidence of glaucoma in patients with uveitis. J Glaucoma 13(6):461–465
Dees C, Arnold JJ, Forrester JV, Dick AD (1998) Immunosuppressive treatment of choroidal neovascularization associated with endogenous posterior uveitis. Arch Ophthalmol 116(11):1456–1461
Enk AH, Knop J (1997) Treatment of pemphigus vulgaris with mycophenolate mofetil. Lancet 350:494
Goldblum R (1993) Therapy of rheumatoid arthritis with mycophenolate mofetil. Clin Exp Rheumatol 11(Suppl 8):S1117–S1119
Spatz S, Rudnicka A, McDonald CJ (1978) Mycophenolic acid in psoriasis. Br J Dermatol 98:429–435
Kilmartin DJ, Forrester JV, Dick AD (1998) Rescue therapy with mycophenolate mofetil in refractory uveitis. Lancet 352:35–36
Thorne JE, Jabs DA, Qazi FA, Nguyen QD, Kempen JH, Dunn JP (2005) Mycophenolate mofetil therapy for inflammatory eye disease. Ophthalmology 112(8):1472–1477
Siepmann K, Huber M, Stübiger N, Deuter C, Zierhut M (2006) Mycophenolate mofetil is a highly effective and safe immunosuppressive agent for the treatment of uveitis. A retrospective analysis of 106 patients. Graefes Arch Clin Exp Ophthalmol 244:788–794
Espinosa-Heidmann D, Suner IJ, Hernandez EP et al (2003) Macrophage depletion diminishes lesion size and severity in experimental choroidal neovascularization. Invest Ophthalmol Vis Sci 44:3586–3592
Reddy VM, Zamora RL, Kaplan HJ (1995) Distribution of growth factors in subfoveal neovascular membranes in age-related macular degeneration and presumed ocular histoplasmosis syndrome. Am J Ophthalmol 120:291–301
Levy J, Shneck M, Klemperer I et al (2005) Punctate inner choroidopathy: resolution after oral steroid treatment and review of the literature. Can J Ophthalmol 40(5):605–608
Dick AD (2005) Are we still reluctant to immunosuppress? Clin Exp Ophthalmol 33(1):1–2
Sollinger HW (1995) US renal transplant mycophenolate mofetil study group. Mycophenolate mofetil for the prevention of acute rejection in primary cadaveric renal allograft recipients. Transplantation 60:225–232
Tricontinental Mycophenolate Mofetil Renal Transplantation Study Group (1996) A blinded, randomized clinical trial of mycophenolate mofetil for the prevention of acute rejection in cadaveric renal transplantation. Transplantation 61:1029–1037
Nowack R, Gobel U, Klooker P, Hergesell O, Andrassy K, van der Wounde FJ (1999) Mycophenolate mofetil for maintenance therapy of Wegener’s granulomatosis and microscopic polyangiitis: a pilot study in 11 patients with renal involvement. J Am Soc Nephrol 10(9):1965–1971
Miehsler W, Reinisch W, Moser G, Gangl A, Vogelsang H (2001) Is mycophenolate mofetil an effective alternative in azathioprine-intolerant patients with chronic active Crohn’s disease? Am J Gastroenterol 96(3):782–787
Benez A, Fierlbeck G (2001) Successful long-term treatment of severe atopic dermatitis with mycophenolate mofetil. Br J Dermatol 144(3):638–639
Disel U, Pavdas S, Dogan A, Gulfiliz G, Yavuz S (2004) Effect of colchicine on cyclosporine nephrotoxicity, reduction of TGF-beta overexpression, apoptosis, and oxidative damage: an experimental animal study. Transplant Proc 36(5):1372–1376
Naesens M, Kuypers DR, Sarwal M (2009) Calcineurin inhibitor nephrotoxicity. Clin J Am Soc Nephrol 4(2):481–508
Yamanaka R, Ogata N, Yamamoto C, Matsushita M, Matsuzaki K, Uyama M, Matsumura M (2002) Expression of transforming growth factor-beta receptors in normal rat retina, experimental choroidal neovascularization. Jpn J Ophthalmol 46(5):525–532
Clancy RM, Buyon JP (2003) Clearance of apoptotic cells: TGF-beta in the balance between inflammation and fibrosis. J Leukoc Biol 74(6):959–960
Shihab FS, Bennett WM, Yi H, Choi SO, Andoh TF (2003) Mycophenolate mofetil ameliorates arteriolopathy and decreases transforming growth factor-beta 1 in chronic cyclosporine nephrotoxicity. Am J Transplant 3(12):1550–1559
Lau CH, Comer M, Lightmen S (2003) Long-term efficacy of mycophenolate mofetil in the control of severe intraocular inflammation. Clin Exp Ophthalmol 31(6):487–491
Allison M, Eugui EM (2000) Mycophenolate mofetil and its mechanism of action. Immunopharmacology 47:85–118
Tran TH, Fardeau C, Terrada C, Ducos De Lahitte G, Bodaghi B, Lehoang P (2008) Intravitreal bevacizumab for refractory choroidal neovascularization (CNV) secondary to uveitis. Graefes Arch Clin Exp Ophthalmol 246(12):1685–1692
Acknowledgments
We thank Miss Barbara Tanucci for her significant help with the statistical analysis.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Neri, P., Manoni, M., Fortuna, C. et al. Association of systemic steroids and mycophenolate mofetil as rescue therapy for uveitic choroidal neovascularization unresponsive to the traditional immunesuppressants: interventional case series. Int Ophthalmol 30, 583–590 (2010). https://doi.org/10.1007/s10792-009-9323-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-009-9323-x