Abstract
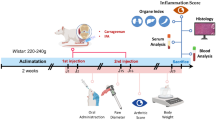
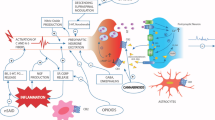
Osteoarthritis (OA) is characterized by cartilage degeneration, subchondral sclerosis, and pain. Cannabinoids have well-established anti-nociceptive properties in animal models of chronic pain. The aim of this study is to evaluate the anti-nociceptive effects of synthetic cannabinoids (WIN-55,212 and HU210) and the cannabinoid-like compound palmitoylethanolamide (PEA) in rat models of OA and to assess the role of cannabinoid receptor 1 (CB1) and the peroxisome proliferator-activated receptor α (PPARα) in mediating these effects. Intra-articular injection of monosodium iodoacetate (MIA) in the knee joint was used as a model of osteoarthritis. The von Frey filament test and weight-bearing difference were used to assess the anti-nociceptive effects of WIN-55,212, HU210, and PEA on MIA-induced OA in rats. Open-field locomotor activity system was used confirm the analgesic effects of those compounds. HU210, WIN55, 212, and PEA in a dose-dependent manner restored the paw withdrawal threshold (PWT) and the weight-bearing difference induced by MIA injection. SR141716A (a CB1 antagonist) significantly reversed the anti-nociceptive effects of all the administered drugs in terms of PWT. However, in terms of weight-bearing difference, SR141716A significantly reduced the anti-nociceptive effect of HU210 but not PEA or WIN55, 212. GW6471 (a PPARα antagonist) significantly reversed the anti-nociceptive effects of PEA but not those of HU210 or WIN55, 212. HU210, WIN55, 212 and PEA significantly restored the MIA-induced reduction in locomotor activity. In conclusions, both CB1 and PPARα receptors are involved in mediating pain in osteoarthritis. Therefore, targeting these receptors may be of great clinical value.






Similar content being viewed by others
References
Adams IB, Martin BR (1996) Cannabis: pharmacology and toxicology in animals and humans. Addiction 91:1585–1614
Akopian AN, Ruparel NB, Jeske NA, Patwardhan A, Hargreaves KM (2009) Role of ionotropic cannabinoid receptors in peripheral antinociception and antihyperalgesia. Trends Pharmacol Sci 30:79–84
Aldossary SA et al (2018) The role of transient receptor potential vanilloid receptor 1 and peroxisome proliferator-activated receptors-α in mediating the antinociceptive effects of palmitoylethanolamine in rats. NeuroReport 30:32–37 (Publish Ahead of Print)
Alsalem M, Altarifi A, Heba K (2016) Role of PPARα and PPARγ in mediating the analgesic properties of ibuprofen in vivo and the effects of dual PPARα/γ activation in inflammatory pain model in the rat. Int J Pharmacol 12:812–820
Blanquart C, Barbier O, Fruchart JC, Staels B, Glineur C (2003) Peroxisome proliferator-activated receptors: regulation of transcriptional activities and roles in inflammation. J Steroid Biochemi Mol Biol 85:267–273
Bocher V, Chinetti G, Fruchart JC, Staels B (2002) Role of the peroxisome proliferator-activated receptors (PPARS) in the regulation of lipids and inflammation control. J de la societe de biologie 196:47–52
Bove SE et al (2003) Weight bearing as a measure of disease progression and efficacy of anti-inflammatory compounds in a model of monosodium iodoacetate-induced osteoarthritis. Osteoarthr Cartil 11:821–830
Cabral GA, Raborn ES, Griffin L, Dennis J, Marciano-Cabral F (2008) CB2 receptors in the brain: role in central immune function. Br J Pharmacol 153:240–251
Chard JA, Tallon D, Dieppe PA (2000) Epidemiology of research into interventions for the treatment of osteoarthritis of the knee joint. Ann Rheum Dis 59:414–418
Clockaerts S, Bastiaansen-Jenniskens YM, Feijt C, Verhaar JA, Somville J, De Clerck LS, Van Osch GJ (2011) Peroxisome proliferator activated receptor alpha activation decreases inflammatory and destructive responses in osteoarthritic cartilage. Osteoarthr cartil 19:895–902
D’Agostino G et al (2009) Central administration of palmitoylethanolamide reduces hyperalgesia in mice via inhibition of NF-kappaB nuclear signalling in dorsal root ganglia. Eur J Pharmacol 613:54–59
Di Cesare Mannelli L, D’Agostino G, Pacini A, Russo R, Zanardelli M, Ghelardini C, Calignano A (2013) Palmitoylethanolamide is a disease-modifying agent in peripheral neuropathy: pain relief and neuroprotection share a PPAR-alpha-mediated mechanism. Mediat Inflamm 2013:328797
Drew LJ, Harris J, Millns PJ, Kendall DA, Chapman V (2000) Activation of spinal cannabinoid 1 receptors inhibits C-fibre driven hyperexcitable neuronal responses and increases [35S]GTPgammaS binding in the dorsal horn of the spinal cord of noninflamed and inflamed rats. Eur J Neurosci 12:2079–2086
Fahmi H, Di Battista JA, Pelletier JP, Mineau F, Ranger P, Martel-Pelletier J (2001) Peroxisome proliferator-activated receptor gamma activators inhibit interleukin-1beta-induced nitric oxide and matrix metalloproteinase 13 production in human chondrocytes. Arthritis Rheum 44:595–607
Felder CC et al (1995) Comparison of the pharmacology and signal transduction of the human cannabinoid CB1 and CB2 receptors. Mol Pharmacol 48:443–450
Hansen HS (2010) Palmitoylethanolamide and other anandamide congeners. Proposed role in the diseased brain. Exp Neurol 224:48–55
Harirforoosh S, Asghar W, Jamali F (2013) Adverse effects of nonsteroidal antiinflammatory drugs: an update of gastrointestinal, cardiovascular and renal complications Journal of pharmacy & pharmaceutical sciences: a publication of the Canadian Society for Pharmaceutical Sciences. Societe canadienne des Sci Pharm 16:821–847
Haywood AR, Hathway GJ, Chapman V (2018) Differential contributions of peripheral and central mechanisms to pain in a rodent model of osteoarthritis. Sci Rep 8:7122
Hohmann AG, Herkenham M (1999) Localization of central cannabinoid CB1 receptor messenger RNA in neuronal subpopulations of rat dorsal root ganglia: a double-label in situ hybridization study. Neuroscience 90:923–931
Huang D, Zhao Q, Liu H, Guo Y, Xu H (2016) PPAR-alpha Agonist WY-14643 Inhibits LPS-Induced Inflammation in Synovial Fibroblasts via NF-kB Pathway. J Mol Neurosci 59:544–553
Huggins JP, Smart TS, Langman S, Taylor L, Young T (2012) An efficient randomised, placebo-controlled clinical trial with the irreversible fatty acid amide hydrolase-1 inhibitor PF-04457845, which modulates endocannabinoids but fails to induce effective analgesia in patients with pain due to osteoarthritis of the knee. Pain 153:1837–1846
Ivanavicius SP, Ball AD, Heapy CG, Westwood FR, Murray F, Read SJ (2007) Structural pathology in a rodent model of osteoarthritis is associated with neuropathic pain: increased expression of ATF-3 and pharmacological characterisation. Pain 128:272–282
Jean-Gilles L et al (2015) Effects of pro-inflammatory cytokines on cannabinoid CB1 and CB2 receptors in immune cells. Acta Physiol (Oxf) 214:63–74
Jiang W, Zhang Y, Xiao L, Van Cleemput J, Ji SP, Bai G, Zhang X (2005) Cannabinoids promote embryonic and adult hippocampus neurogenesis and produce anxiolytic- and antidepressant-like effects. J Clin Investig 115:3104–3116
Kong Y, Wang W, Zhang C, Wu Y, Liu Y, Zhou X (2016) Cannabinoid WIN55,2122 mesylate inhibits ADAMTS4 activity in human osteoarthritic articular chondrocytes by inhibiting expression of syndecan1. Mol Med Rep 13:4569–4576
Lauckner JE, Hille B, Mackie K (2005) The cannabinoid agonist WIN55,212-2 increases intracellular calcium via CB1 receptor coupling to Gq/11 G proteins. Proc Nat Acad Sci USA 102:19144–19149
Lo Verme J, Fu J, Astarita G, La Rana G, Russo R, Calignano A, Piomelli D (2005) The nuclear receptor peroxisome proliferator-activated receptor-alpha mediates the anti-inflammatory actions of palmitoylethanolamide. Mol Pharmacol 67:15–19
LoVerme J et al (2006) Rapid broad-spectrum analgesia through activation of peroxisome proliferator-activated receptor-alpha. J Pharmacol Exp Ther 319:1051–1061
Martin WJ, Coffin PO, Attias E, Balinsky M, Tsou K, Walker JM (1999) Anatomical basis for cannabinoid-induced antinociception as revealed by intracerebral microinjections. Brain Res 822:237–242
Mogil JS (2009) Animal models of pain: progress and challenges Nature reviews. Neuroscience 10:283–294
Muley MM, Krustev E, McDougall JJ (2016) Preclinical Assessment of Inflammatory Pain. CNS Neurosci Ther 22:88–101
O’Brien M, McDougall JJ (2018) Cannabis and joints: scientific evidence for the alleviation of osteoarthritis pain by cannabinoids. Curr Opin Pharmacol 40:104–109
Orita S et al (2011) Pain-related sensory innervation in monoiodoacetate-induced osteoarthritis in rat knees that gradually develops neuronal injury in addition to inflammatory pain. BMC Musculoskelet Disord 12:134
Palazuelos J et al (2009) Microglial CB2 cannabinoid receptors are neuroprotective in Huntington’s disease excitotoxicity. Brain J neurol 132:3152–3164
Patwardhan AM, Jeske NA, Price TJ, Gamper N, Akopian AN, Hargreaves KM (2006) The cannabinoid WIN 55,212-2 inhibits transient receptor potential vanilloid 1 (TRPV1) and evokes peripheral antihyperalgesia via calcineurin. Proc Nat Acad Sci USA 103:11393–11398
Richardson D et al (2008) Characterisation of the cannabinoid receptor system in synovial tissue and fluid in patients with osteoarthritis and rheumatoid arthritis. Arthritis Res Ther 10:R43
Rinaldi-Carmona M et al (1995) Biochemical and pharmacological characterisation of SR141716A, the first potent and selective brain cannabinoid receptor antagonist. Life Sci 56:1941–1947
Sagar DR et al (2010) Tonic modulation of spinal hyperexcitability by the endocannabinoid receptor system in a rat model of osteoarthritis pain. Arthritis Rheum 62:3666–3676
Schuelert N, McDougall JJ (2008) Cannabinoid-mediated antinociception is enhanced in rat osteoarthritic knees. Arthritis Rheum 58:145–153
Schuelert N et al (2010) Paradoxical effects of the cannabinoid CB2 receptor agonist GW405833 on rat osteoarthritic knee joint pain. Osteoarthr Cartil 18:1536–1543
Song ZH, Slowey CA, Hurst DP, Reggio PH (1999) The difference between the CB(1) and CB(2) cannabinoid receptors at position 5.46 is crucial for the selectivity of WIN55212-2 for CB(2). Mol Pharmacol 56:834–840
Stevenson GW et al (2011) Monosodium iodoacetate-induced osteoarthritis produces pain-depressed wheel running in rats: implications for preclinical behavioral assessment of chronic pain. Pharmacol Biochem Behav 98:35–42
Suokas AK, Sagar DR, Mapp PI, Chapman V, Walsh DA (2014) Design, study quality and evidence of analgesic efficacy in studies of drugs in models of OA pain: a systematic review and a meta-analysis. Osteoarthr Cartil 22:1207–1223
Symmons D, Mathers C, Pfleger B (2003) Global burden of osteoarthritis in the year 2000. World Health Organization, Geneva
Uhelski ML, Cain DM, Harding-Rose C, Simone DA (2013) The non-selective cannabinoid receptor agonist WIN 55,212-2 attenuates responses of C-fiber nociceptors in a murine model of cancer pain. Neuroscience 247:84–94
Van Sickle MD et al (2005) Identification and functional characterization of brainstem cannabinoid CB2 receptors. Science (New York) 310:329–332
Wang K, Xu J, Hunter DJ, Ding C (2015) Investigational drugs for the treatment of osteoarthritis. Expert Opin Investig Drugs 24:1539–1556
Wang J, Wang G, Sun GW (2016) Role of PPAα in down-regulating AGE-induced TGF-β and MMP-9 expressions in chondrocytes. Genet Mol Res. https://doi.org/10.4238/gmr.15027963
Wong GY, Gavva NR (2009) Therapeutic potential of vanilloid receptor TRPV1 agonists and antagonists as analgesics: recent advances and setbacks. Brain Res Rev 60:267–277
Acknowledgements
This work was sponsored by the deanship of academic research in The University of Jordan.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Authors declare no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Alsalem, M., Haddad, M., Aldossary, S.A. et al. Role of cannabinoid receptor 1 and the peroxisome proliferator-activated receptor α in mediating anti-nociceptive effects of synthetic cannabinoids and a cannabinoid-like compound. Inflammopharmacol 27, 1131–1142 (2019). https://doi.org/10.1007/s10787-019-00584-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10787-019-00584-7