Abstract
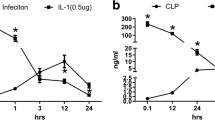
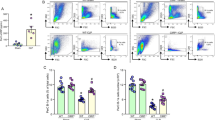
Sepsis continues to be a major healthcare issue with one of the highest mortality rates in intensive care units. Toll-like receptors are pattern recognition receptors that are intricately involved in the pathogenesis of sepsis. TLR3 is a major receptor for double-stranded RNA and is largely associated with immunity to viral infection. In this study, we examined the role of TLR3 priming in the immunopathology of sepsis using cecal-ligation and puncture (CLP) model of sepsis in mice. Mice injected with vehicle or poly(I:C) were subjected to sham or CLP surgery and various parameters of sepsis, including mortality, inflammation, and bacterial clearance were assessed. Poly(I:C) pre-treatment significantly enhanced mortality in mice subjected to CLP. Consistent with this, inflammatory cytokines including TNFα, IL-12p40, IFNγ, and MCP-1 were enhanced both systemically and locally in the poly(I:C)-treated group compared to the vehicle control. In addition, bacterial load was significantly higher in the poly(I:C)-treated septic mice. These changes were associated with reduced macrophage activation (but not neutrophils) in the peritoneal cavity of poly(I:C) pre-treated mice compared to vehicle pre-treatment. Together our results demonstrate that poly(I:C) priming in sepsis is likely to be detrimental to the host due to effects on systemic inflammatory cytokines and bacterial clearance.





Similar content being viewed by others
References
Cavassani, K.A., M. Ishii, H. Wen, and M.A. Schaller. 2008. TLR3 is an endogenous sensor of tissue necrosis during acute inflammatory events. The Journal of Experimental Medicine 205 (11): 2609–2621. https://doi.org/10.1084/jem.20081370.
Coffman, R.L., A. Sher, and R.A. Seder. 2010. Vaccine adjuvants: putting innate immunity to work. Immunity 33 (4): 492–503. https://doi.org/10.1016/j.immuni.2010.10.002.
Davis, Christopher G., Kathy Chang, Dale Osborne, Andrew H. Walton, Sarbani Ghosh, William Michael Dunne, Richard S. Hotchkiss, and Jared T. Muenzer. 2013. TLR3 agonist improves survival to secondary pneumonia in a double injury model. The Journal of Surgical Research 182 (2): 270–276. https://doi.org/10.1016/j.jss.2012.09.039.
Dejager, L., S. Vandevyver, M. Ballegeer, E. Van Wonterghem, L.L. An, J. Riggs, R. Kolbeck, and C. Libert. 2014. Pharmacological inhibition of type I interferon signaling protects mice against lethal sepsis. The Journal of Infectious Diseases 209 (6): 960–970. https://doi.org/10.1093/infdis/jit600.
Deng, T., X. Feng, P. Liu, K. Yan, Y. Chen, and D. Han. 2013. Toll-like receptor 3 activation differentially regulates phagocytosis of bacteria and apoptotic neutrophils by mouse peritoneal macrophages. Immunology and Cell Biology 91 (1): 52–59. https://doi.org/10.1038/icb.2012.45.
Doyle, S.E., R.M. O'Connell, G.A. Miranda, S.A. Vaidya, E.K. Chow, P.T. Liu, S. Suzuki, et al. 2004. Toll-like receptors induce a phagocytic gene program through p38. The Journal of Experimental Medicine 199 (1): 81–90. https://doi.org/10.1084/jem.20031237.
Feterowski, C. 2005. Attenuated pathogenesis of polymicrobial peritonitis in mice after TLR2 agonist pre-treatment involves ST2 up-regulation. International Immunology 17 (8): 1035–1046. https://doi.org/10.1093/intimm/dxh282.
Gao, M., T. Ha, X. Zhang, X. Wang, L. Liu, J. Kalbfleisch, K. Singh, D. Williams, and C. Li. 2013. The toll-like receptor 9 ligand, CpG oligodeoxynucleotide, attenuates cardiac dysfunction in polymicrobial sepsis, involving activation of both phosphoinositide 3 kinase/Akt and extracellular-signal-related kinase signaling. The Journal of Infectious Diseases 207 (9): 1471–1479. https://doi.org/10.1093/infdis/jit036.
Gong, Wei, Erling Hu, Huan Dou, Yuxian Song, Liu Yang, Jianjian Ji, Erguang Li, Renxiang Tan, and Yayi Hou. 2014. A novel 1,2-benzenediamine derivative FC-99 suppresses TLR3 expression and ameliorates disease symptoms in a mouse model of sepsis. British Journal of Pharmacology 171 (21): 4866–4878. https://doi.org/10.1111/bph.12797.
Kelly-Scumpia, K.M., P.O. Scumpia, M.J. Delano, J.S. Weinstein, A.G. Cuenca, J.L. Wynn, and L.L. Moldawer. 2010. Type I interferon signaling in hematopoietic cells is required for survival in mouse polymicrobial sepsis by regulating CXCL10. The Journal of Experimental Medicine 207 (2): 319–326. https://doi.org/10.1084/jem.20091959.
Liu, J.R., X. Han, S.G. Soriano, and K. Yuki. 2014. The role of macrophage 1 antigen in polymicrobial sepsis. Shock 42 (6): 532–539. https://doi.org/10.1097/SHK.0000000000000250.
Mancuso, G., A. Midiri, C. Biondo, C. Beninati, S. Zummo, R. Galbo, F. Tomasello, et al. 2007. Type I IFN signaling is crucial for host resistance against different species of pathogenic bacteria. Journal of Immunology 178 (5): 3126–3133.
O'Connell, R.M., S.K. Saha, S.A. Vaidya, K.W. Bruhn, G.A. Miranda, B. Zarnegar, A.K. Perry, et al. 2004. Type I interferon production enhances susceptibility to Listeria monocytogenes infection. The Journal of Experimental Medicine 200 (4): 437–445. https://doi.org/10.1084/jem.20040712.
Packiriswamy, N., T. Lee, P.B. Raghavendra, H. Durairaj, H. Wang, and N. Parameswaran. 2013. G-protein-coupled receptor kinase-5 mediates inflammation but does not regulate cellular infiltration or bacterial load in a polymicrobial sepsis model in mice. Journal of Innate Immunity 5 (4): 401–413. https://doi.org/10.1159/000347002.
Packiriswamy, N., M. Steury, I.C. McCabe, S.D. Fitzgerald, and N. Parameswaran. 2016. Bacterial dose-dependent role of G protein-coupled receptor kinase 5 in Escherichia coli-induced pneumonia. Infection and Immunity 84 (5): 1633–1641. https://doi.org/10.1128/IAI.00051-16.
Pyles, R.B., G.E. Jezek, and T.D. Eaves-Pyles. 2010. Toll-like receptor 3 agonist protection against experimental Francisella tularensis respiratory tract infection. Infection and Immunity 78 (4): 1700–1710. https://doi.org/10.1128/IAI.00736-09.
Rice, Lauren, Daniel Orlow, Katherine Ceonzo, Gregory L. Stahl, Aurthur O. Tzianabos, Hiromi Wada, William C. Aird, and Jon A. Buras. 2005. CpG oligodeoxynucleotide protection in polymicrobial sepsis is dependent on interleukin-17. The Journal of Infectious Diseases 191 (8): 1368–1376. https://doi.org/10.1086/428452.
Savva, A., and T. Roger. 2013. Targeting toll-like receptors: promising therapeutic strategies for the management of sepsis-associated pathology and infectious diseases. Frontiers in Immunology 4: 387. https://doi.org/10.3389/fimmu.2013.00387.
Sharma, D., A. Malik, M.D. Steury, P.C. Lucas, and N. Parameswaran. 2015. Protective role of beta-arrestin2 in colitis through modulation of T-cell activation. Inflammatory Bowel Diseases 21 (12): 2766–2777. https://doi.org/10.1097/MIB.0000000000000563.
Sharma, D., N. Packiriswamy, A. Malik, P.C. Lucas, and N. Parameswaran. 2014. Nonhematopoietic beta-Arrestin-1 inhibits inflammation in a murine model of polymicrobial sepsis. The American Journal of Pathology 184 (8): 2297–2309. https://doi.org/10.1016/j.ajpath.2014.05.002.
Shi, Dong-Wei, Jing Zhang, Hong-Ni Jiang, Chao-Yang Tong, Gu Guo-Rong, Yuan Ji, Hanssa Summah, and Jie-Ming Qu. 2011. LPS pretreatment ameliorates multiple organ injuries and improves survival in a murine model of polymicrobial sepsis. Inflammation 60 (9): 841–849. https://doi.org/10.1007/s00011-011-0342-5.
Stearns-Kurosawa, D.J., M.F. Osuchowski, C. Valentine, S. Kurosawa, and D.G. Remick. 2011. The pathogenesis of sepsis. Annual Review of Pathology 6: 19–48. https://doi.org/10.1146/annurev-pathol-011110-130327.
Walker, W.E., A.T. Bozzi, and D.R. Goldstein. 2012. IRF3 contributes to sepsis pathogenesis in the mouse cecal ligation and puncture model. Journal of Leukocyte Biology 92 (6): 1261–1268. https://doi.org/10.1189/jlb.0312138.
Weighardt, H., C. Feterowski, M. Veit, M. Rump, H. Wagner, and B. Holzmann. 2000. Increased resistance against acute polymicrobial sepsis in mice challenged with immunostimulatory CpG oligodeoxynucleotides is related to an enhanced innate effector cell response. Journal of Immunology (Baltimore, Md. : 1950) 165 (8): 4537–4543. https://doi.org/10.4049/jimmunol.165.8.4537.
Wheeler, Derek S., Patrick M. Lahni, Alvin G. Denenberg, Sue E. Poynter, Hector R. Wong, James A. Cook, and Basilia Zingarelli. 2008. Induction of endotoxin tolerance enhances bacterial clearance and survival in murine polymicrobial sepsis. Shock: 1–7. https://doi.org/10.1097/shk.0b013e318162c190.
Wynn, James L., Philip O. Scumpia, Robert D. Winfield, Matthew J. Delano, Kindra Kelly-Scumpia, Tolga Barker, Ricardo Ungaro, Ofer Levy, and Lyle L. Moldawer. 2008. Defective innate immunity predisposes murine neonates to poor sepsis outcome but is reversed by TLR agonists. Blood 112 (5): 1750–1758. https://doi.org/10.1182/blood-2008-01-130500.
Acknowledgements
We gratefully acknowledge the support from NIH (grants HL095637, AI099404, and AR056680 to N.P.). We thank the University lab animal resources for taking excellent care of our animals and the Histopathology laboratory for their excellent service.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sharma, D., Malik, A., Packiriswamy, N. et al. Poly(I:C) Priming Exacerbates Cecal Ligation and Puncture-Induced Polymicrobial Sepsis in Mice. Inflammation 41, 328–336 (2018). https://doi.org/10.1007/s10753-017-0690-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-017-0690-6