Abstract
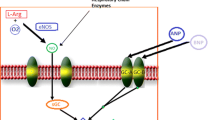
Acute heart failure syndromes (AHFS) are associated with the rapid onset of heart failure (HF) signs and symptoms. Hospitalizations for AHFS continue to rise and are associated with significant mortality and morbidity. Several pharmacological agents are currently approved for the treatment of AHFS, but their use is associated with an increase in short-term mortality. There is a need for new agents that can be given in the acute setting with increased efficacy and safety. Istaroxime is a unique agent with both inotropic and lusitropic properties which is currently being studied for the treatment of AHFS. Istaroxime inhibits the sodium–potassium adenosine triphosphatase (ATPase) and stimulates the sarcoplasmic reticulum calcium ATPase isoform 2 (SERCA-2) thereby improving contractility and diastolic relaxation. Early data from human studies reveal that istaroxime decreases pulmonary capillary wedge pressure (PCWP) and possibly improves diastolic function without causing a significant change in heart rate (HR), blood pressure, ischemic or arrhythmic events. Most commonly reported side effects were related to gastrointestinal intolerance and were dose related. In conclusion, istaroxime is a novel agent being investigated for the treatment of AHFS whose mechanism of action and cellular targets make it a promising therapy. Further studies with longer infusion times in patients with hypotension are required to confirm its efficacy and safety.







Similar content being viewed by others
References
Lloyd-Jones D et al (2009) Heart disease and stroke statistics—2009 update. A report from the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Circulation 119(3):e21–e181. doi:10.1161/CIRCULATIONAHA.108.191261
Lloyd-Jones DM et al (2002) Lifetime risk for developing congestive heart failure: the Framingham Heart Study. Circulation 106(24):3068–3072. doi:10.1161/01.CIR.0000039105.49749.6F
Gheorghiade M et al (2005) Acute heart failure syndromes: current state and framework for future research. Circulation 112(25):3958–3968. doi:10.1161/CIRCULATIONAHA.105.590091
Gheorghiade M et al (2006) Systolic blood pressure at admission, clinical characteristics, and outcomes in patients hospitalized with acute heart failure. J Am Med Assoc 296(18):2217–2226. doi:10.1001/jama.296.18.2217
Elkayam U et al (2007) Use and impact of inotropes and vasodilator therapy in hospitalized patients with severe heart failure. Am Heart J 153(1):98–104. doi:10.1016/j.ahj.2006.09.005
Burger AJ et al (2002) Effect of nesiritide (B-type natriuretic peptide) and dobutamine on ventricular arrhythmias in the treatment of patients with acutely decompensated congestive heart failure: the PRECEDENT study. Am Heart J 144(6):1102–1108. doi:10.1067/mhj.2002.125620
Thackray S et al (2002) The effectiveness and relative effectiveness of intravenous inotropic drugs acting through the adrenergic pathway in patients with heart failure-a meta-regression analysis. Eur J Heart Fail 4(4):515–529. doi:10.1016/S1388-9842(02)00041-7
Packer M et al (1991) Effect of oral milrinone on mortality in severe chronic heart failure. The PROMISE Study Research Group. N Engl J Med 325(21):1468–1475
Cuffe MS et al (2002) Short-term intravenous milrinone for acute exacerbation of chronic heart failure: a randomized controlled trial. J Am Med Assoc 287(12):1541–1547. doi:10.1001/jama.287.12.1541
Felker GM et al (2003) Heart failure etiology and response to milrinone in decompensated heart failure: results from the OPTIME-CHF study. J Am Coll Cardiol 41(6):997–1003. doi:10.1016/S0735-1097(02)02968-6
Mebazaa A et al (2007) Levosimendan vs dobutamine for patients with acute decompensated heart failure: the SURVIVE Randomized Trial. J Am Med Assoc 297(17):1883–1891. doi:10.1001/jama.297.17.1883
Cleland JG et al (2006) Clinical trials update from the American Heart Association: REPAIR-AMI, ASTAMI, JELIS, MEGA, REVIVE-II, SURVIVE, and PROACTIVE. Eur J Heart Fail 8(1):105–110. doi:10.1016/j.ejheart.2005.12.003
Mattera GG et al (2007) Istaroxime: a new luso-inotropic agent for heart failure. Am J Cardiol 99(2A):33A–40A. doi:10.1016/j.amjcard.2006.09.004
Micheletti R et al (2002) Pharmacological profile of the novel inotropic agent (E, Z)-3-((2-aminoethoxy)imino)androstane-6, 17-dione hydrochloride (PST2744). J Pharmacol Exp Ther 303(2):592–600. doi:10.1124/jpet.102.038331
Sabbah HN et al (2007) Hemodynamic properties of a new-generation positive luso-inotropic agent for the acute treatment of advanced heart failure. Am J Cardiol 99(2A):41A–46A. doi:10.1016/j.amjcard.2006.09.005
Ghali JK et al (2007) A phase 1-2 dose-escalating study evaluating the safety and tolerability of istaroxime and specific effects on electrocardiographic and hemodynamic parameters in patients with chronic heart failure with reduced systolic function. Am J Cardiol 99(2A):47A–56A. doi:10.1016/j.amjcard.2006.09.006
Blair JE et al (2008) Rationale and design of the hemodynamic, echocardiographic and neurohormonal effects of istaroxime, a novel intravenous inotropic and lusitropic agent: a randomized controlled trial in patients hospitalized with heart failure (HORIZON-HF) trial. Am J Ther 15(3):231–240. doi:10.1097/MJT.0b013e31816d9186
Gheorghiade M et al (2008) Hemodynamic, echocardiographic, and neurohormonal effects of istaroxime, a novel intravenous inotropic and lusitropic agent: a randomized controlled trial in patients hospitalized with heart failure. J Am Coll Cardiol 51(23):2276–2285. doi:10.1016/j.jacc.2008.03.015
Abraham WT et al (2005) In-hospital mortality in patients with acute decompensated heart failure requiring intravenous vasoactive medications: an analysis from the Acute Decompensated Heart Failure National Registry (ADHERE). J Am Coll Cardiol 46(1):57–64. doi:10.1016/j.jacc.2005.03.051
Hasenfuss G et al (1992) Alteration of contractile function and excitation-contraction coupling in dilated cardiomyopathy. Circ Res 70(6):1225–1232
Bers DM (2008) Calcium cycling and signaling in cardiac myocytes. Annu Rev Physiol 70:23–49. doi:10.1146/annurev.physiol.70.113006.100455
Frank KF et al (2003) Sarcoplasmic reticulum Ca2+ -ATPase modulates cardiac contraction and relaxation. Cardiovasc Res 57(1):20–27. doi:10.1016/S0008-6363(02)00694-6
Bers DM, Bassani JW, Bassani RA (1996) Na-Ca exchange and Ca fluxes during contraction and relaxation in mammalian ventricular muscle. Ann N Y Acad Sci 779:430–442. doi:10.1111/j.1749-6632.1996.tb44818.x
Meyer M et al (1995) Alterations of sarcoplasmic reticulum proteins in failing human dilated cardiomyopathy. Circulation 92(4):778–784
Studer R et al (1994) Gene expression of the cardiac Na(+)-Ca2+ exchanger in end-stage human heart failure. Circ Res 75(3):443–453
Acknowledgments
Dr. Gheorghiade reports receiving research grants from the National Institutes of Health, Otsuka, Sigma-Tau, Merck, and Scios Inc.; being a consultant for Debiopharm, Errekappa Terapeutici, GlaxoSmithKline, Protein Design Laboratories, Medtronic, and Sigma-Tau; and receiving honoraria from Abbott, AstraZeneca, GlaxoSmithKline, Medtronic, Otsuka, Protein Design Laboratories, Scios Inc., and Sigma-Tau. Dr. Metra has occasionally received honoraria and reimbursement for travel expenses from Actelion, Corthera, Merck, NovaCardia, and Servier. Dr. Filippatos reports receiving research grants from the American Heart Association, University of Athens, Otsuka, Medtronic, Sigma-Tau, Roche Diagnostics, Biosite, Brahms. Dr. Sabbah reports receiving research grants and being a consultant to Sigma-Tau. Dr. Porchet is the Vice President Medical Affairs of Debiopharm S.A. Dr. Valentini is an employee of Sigma-Tau. Dr. Blair reports being a consultant for Debiopharm S.A. Dr’s. Khan and Harinstein have nothing to disclose. Mark Vogel has nothing to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Khan, H., Metra, M., Blair, J.E.A. et al. Istaroxime, a first in class new chemical entity exhibiting SERCA-2 activation and Na–K-ATPase inhibition: a new promising treatment for acute heart failure syndromes?. Heart Fail Rev 14, 277–287 (2009). https://doi.org/10.1007/s10741-009-9136-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10741-009-9136-z