Abstract
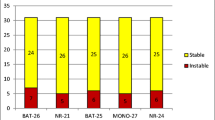
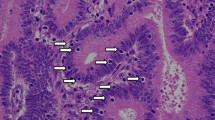
We assessed the molecular characteristics and the frequency of mutations in mismatch-repair genes among Bedouin patients with colorectal cancer (CRC) in Israel. Bedouin patients with a diagnosis of CRC at a major hospital in the southern part of Israel were deemed eligible for this study. The primary screening method was immunohistochemical staining for mismatch-repair proteins (MLH1, MSH2, MSH6, and PMS2). For subjects with abnormal immunohistochemical staining, we performed microsatellite instability (MSI) analyses, and for tumors with a loss of MLH1 expression we also performed BRAF testing. In MSI high cases we searched further for germline mutations. Of the 24 patients enrolled, four subjects (16.7%) had MSI high tumors: one subject was found to harbor a biallelic PMS2 mutation, one subject had Lynch syndrome (LS) with MSH6 mutation and two subjects had a loss of MLH1/PMS2 proteins/BRAF wild type/normal MLH1 sequence. Ten patients (41.7%) were younger than 50 at the time of diagnosis and none had first degree relatives with CRC. In conclusion, in this cohort of 24 consecutive Arab Bedouins with CRC, one patient was found to harbor a constitutional mismatch repair deficiency, one patient had LS with MSH6 mutation, and two patients had unresolved loss of MLH1/PMS2 proteins/BRAF wild type phenotype.

Similar content being viewed by others
References
Shia J (2015) Evolving approach and clinical significance of detecting DNA mismatch repair deficiency in colorectal carcinoma. Semin Diagn Pathol 32:352–361
Giardiello FM, Allen JI, Axilbund JE et al (2014) Guidelines on Genetic evaluation and management of Lynch syndrome: a consensus statement by the US Multi-society task force on colorectal cancer. Am J Gastroenterol 109:1159–1179
Icli F, Akbulut H, Bazarbashi S et al (2010) Modification and implementation of NCCN guidelines on colon cancer in the Middle East and North Africa region. J Natl Compr Canc Netw 8(Suppl 3):S22–S25
GLOBOCAN (2015) Colorectal cancer, estimated incidence, mortality and prevalence worldwide in 2012
Rozen P, Rosner G, Liphshitz I, Barchana M (2007) The changing incidence and sites of colorectal cancer in the Israeli Arab population and their clinical implications. Int J Cancer 120:147–151
Mosli MH, Al-Ahwal MS (2012) Colorectal cancer in the Kingdom of Saudi Arabia: need for screening. Asian Pac J Cancer Prev 13:3809–3813
Al Quorain AA, Satti MB, Al Gindan YM, Al-Hamdan A (2000) The pattern of lower gastrointestinal disease in the eastern region of Saudi Arabia: a retrospective analysis of 1590 consecutive patients. Saudi J Gastroenterol 6:27–32
Rainis T, Halloun L, Keren D et al (2010) Colorectal cancer among Arab-Israeli women-possible reasons for increased incidence and mortality. J Gastrointest Cancer 41:130–134
Olefson S, Moss SF (2015) Obesity and related risk factors in gastric cardia adenocarcinoma. Gastric Cancer 18:23–32
Shpitz B, Millman M, Ziv Y et al (2006) Predominance of younger age, advanced stage, poorly-differentiated and mucinous histology in Israeli Arab patients with colorectal cancer. Anticancer Res 26:533–537
Alsanea N (2014) The dilemma of the threshold age to start screening for colorectal cancer in Saudi Arabia. Saudi J Gastroenterol 20:141–142
Albasri A, Yosef H, Hussainy AS et al (2014) Histopathological features of colorectal cancer in Al-Madinah region of Saudi Arabia: 8 years experience. Asian Pac J Cancer Prev 15:3133–3137
Syngal S, Brand RE, Church JM et al (2015) ACG clinical guideline: genetic testing and management of hereditary gastrointestinal cancer syndromes. Am J Gastroenterol 110:223–262
Siraj AK, Bu R, Prabhakaran S et al (2014) A very low incidence of BRAF mutations in Middle Eastern colorectal carcinoma. Mol Cancer 13:168
Vilkin A, Niv Y, Nagasaka T et al (2009) Microsatellite instability, MLH1 promoter methylation, and BRAF mutation analysis in sporadic colorectal cancers of different ethnic groups in Israel. Cancer 115:760–769
Zahrani A, Kandil M, Badar T et al (2014) Clinico-pathological study of K-ras mutations in colorectal tumors in Saudi Arabia. Tumori 100:75–79
Goldberg Y, Barnes-Kedar I, Lerer I et al (2015) Genetic features of Lynch syndrome in the Israeli population. Clin Genet 87:549–553
Abuhazira YS (2010) The Bedouin Population in Israel-In. http://www.cbs.gov.il
Shia J, Stadler Z, Weiser MR et al (2011) Immunohistochemical staining for DNA mismatch repair proteins in intestinal tract carcinoma: how reliable are biopsy samples? Am J Surg Pathol 35:447–454
Levi Z, Kariv R, Barnes-Kedar I et al (2015) The gastrointestinal manifestation of constitutional mismatch repair deficiency syndrome: from a single adenoma to polyposis-like phenotype and early onset cancer. Clin Genet 88:474–478
Baris HN, Barnes-Kedar I, Toledano H et al (2016) Constitutional mismatch repair deficiency in Israel: high proportion of founder mutations in MMR genes and consanguinity. Pediatr Blood Cancer 63:418–427
Vasen HF, Ghorbanoghli Z, Bourdeaut F et al (2014) Guidelines for surveillance of individuals with constitutional mismatch repair-deficiency proposed by the European Consortium “Care for CMMR-D” (C4CMMR-D). J Med Genet 51:283–293
Wimmer K, Kratz CP, Vasen HF et al (2014) Diagnostic criteria for constitutional mismatch repair deficiency syndrome: suggestions of the European consortium ‘care for CMMRD’ (C4CMMRD). J Med Genet 51:355–365
Durno CA, Holter S, Sherman PM, Gallinger S (2010) The gastrointestinal phenotype of germline biallelic mismatch repair gene mutations. Am J Gastroenterol 105:2449–2456
Vardi-Saliternik R, Friedlander Y, Cohen T (2002) Consanguinity in a population sample of Israeli Muslim Arabs, Christian Arabs and Druze. Ann Hum Biol 29:422–431
Shia J (2008) Immunohistochemistry versus microsatellite instability testing for screening colorectal cancer patients at risk for hereditary nonpolyposis colorectal cancer syndrome: Part I. The utility of immunohistochemistry. J Mol Diagn 10:293–300
Shia J, Tang LH, Vakiani E et al (2009) Immunohistochemistry as first-line screening for detecting colorectal cancer patients at risk for hereditary nonpolyposis colorectal cancer syndrome: a 2-antibody panel may be as predictive as a 4-antibody panel. Am J Surg Pathol 33:1639–1645
Shia J, Holck S, Depetris G et al (2013) Lynch syndrome-associated neoplasms: a discussion on histopathology and immunohistochemistry. Fam Cancer 12:241–260
Moreira L, Munoz J, Cuatrecasas M et al (2015) Prevalence of somatic mutl homolog 1 promoter hypermethylation in Lynch syndrome colorectal cancer. Cancer 121:1395–1404
Carethers JM, Stoffel EM (2015) Lynch syndrome and Lynch syndrome mimics: the growing complex landscape of hereditary colon cancer. World J Gastroenterol 21:9253–9261
Carethers JM (2014) Differentiating Lynch-like from Lynch syndrome. Gastroenterology 146:602–604
Ladabaum U, Ford JM, Martel M, Barkun AN (2015) American gastroenterological association technical review on the diagnosis and management of Lynch syndrome. Gastroenterology 149:783–813
Boland CR (2013) The mystery of mismatch repair deficiency: Lynch or Lynch-like? Gastroenterology 144:868–870
Mensenkamp AR, Vogelaar IP, van Zelst-Stams WA et al (2014) Somatic mutations in MLH1 and MSH2 are a frequent cause of mismatch-repair deficiency in Lynch syndrome-like tumors. Gastroenterology 146:643–646
Castillejo A, Vargas G, Castillejo MI et al (2014) Prevalence of germline MUTYH mutations among Lynch-like syndrome patients. Eur J Cancer 50:2241–2250
Inra JA, Syngal S (2015) Colorectal cancer in young adults. Dig Dis Sci 60:722–733
Tanskanen T, Gylfe AE, Katainen R et al (2015) Systematic search for rare variants in finnish early-onset colorectal cancer patients. Cancer Genet 208:35–40
Kilpivaara O, Aaltonen LA (2013) Diagnostic cancer genome sequencing and the contribution of germline variants. Science 339:1559–1562
Glushko Y, Basher W, Barchana M, Zidan J (2010) Differences in clinical and pathological characteristics of colorectal cancer in Arab as compared to Jewish patients in Northern Israel. Fam Cancer 9:327–330
Freedman LS, Barchana M, Al-Kayed S et al (2003) A comparison of population-based cancer incidence rates in Israel and Jordan. Eur J Cancer Prev 12:359–365
Kamat N, Khidhir MA, Alashari MM, Rannug U (2013) Microsatellite instability and loss of heterozygosity detected in middle-aged patients with sporadic colon cancer: a retrospective study. Oncol Lett 6:1413–1420
Chen-Shtoyerman R, Theodor L, Harmati E et al (2003) Genetic analysis of familial colorectal cancer in Israeli Arabs. Hum Mutat 21:446–447
Qumseya BJ, Tayem YI, Dasa OY et al (2014) Barriers to colorectal cancer screening in Palestine: a national study in a medically underserved population. Clin Gastroenterol Hepatol 12:463–469
Cohen M (2014) An integrated view of cultural perceptions of cancer among Arab people in Israel. Health Psychol Rev 8:490–508
Funding
The Israel Cancer Association funded the study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
There are no conflicts of interest for any of the authors.
Additional information
Yael Goldberg and Zohar Levi have contributed equally.
Rights and permissions
About this article
Cite this article
Abu Freha, N., Leibovici Weissman, Y., Fich, A. et al. Constitutional mismatch repair deficiency and Lynch syndrome among consecutive Arab Bedouins with colorectal cancer in Israel. Familial Cancer 17, 79–86 (2018). https://doi.org/10.1007/s10689-017-0009-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10689-017-0009-7