Abstract
Background
A variety of studies have shown rising trends in the occurrence of colorectal cancer in younger patients as opposed to falling trends among older patients aged 55 years or more. We hypothesized that the time trends of benign colonic precursor lesions would reveal similar patterns.
Aims
The present study was designed to test this hypothesis in a large nationwide sample of the US population undergoing colonoscopy in community-based endoscopy centers.
Methods
The Inform Diagnostics database is an electronic repository of histopathologic records of patients distributed throughout the USA. A cross-sectional study analyzed the detection rates of sessile serrated adenomas (SSA), hyperplastic polyps (HP), tubular adenomas (TA), traditional serrated adenomas (TSA), or adenocarcinomas (colorectal cancer, CRC) in 2,910,174 colonoscopies done 2008–2020.
Results
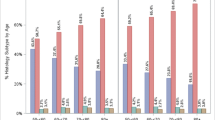
During the 13-year time period, the rate of SSA showed a significant rise, both in patients younger and older than 55 years. HP and TA both showed a significant decline during the same time period. The trends of CRC in the older age group decreased significantly between 2008 (or its peak in 2012) and 2020. The trends of CRC in the younger age group increased significantly between 2008 and its peak in 2017.
Conclusions
The age-specific time trends of benign and malignant colonic neoplasia are characterized by dissimilar temporal patterns. Such dissimilarity could suggest that besides a set of shared risk factors that affect all types of colonic neoplasia alike, there is yet another set of environmental risk factors that specifically influence malignant transformation.




Similar content being viewed by others
References
Stoffel EM, Murphy CC. Epidemiology and mechanisms of the increasing incidence of colon and rectal Cancers in young adults. Gastroenterology 2020;158:341–353.
Siegel RL, Fedewa SA, Anderson WF, et al. Colorectal cancer incidence patterns in the United States, 1974–2013. J Natl Cancer Inst 2017:109.
Siegel RL, Miller KD, Jemal A. Colorectal cancer mortality rates in adults aged 20 to 54 years in the United States, 1970–2014. JAMA 2017;318:572–574.
Vuik FER, Nieuwenburg SAV, Bardou M et al. Increasing incidence of colorectal cancer in young adults in Europe over the last 25 years. Gut 2019;68:1820–1826.
Siegel RL, Lindsey A, Torre LA, Soerjomataram I et al. Global patterns and trends in colorectal cancer incidence in young adults. Gut 2019;68:2179–2185.
Wolf AMD, Fontham ETH, Church TR et al. Colorectal cancer screening for average-risk adults: 2018 guideline update from the American Cancer Society. CA Cancer J Clin 2018;68:250–281.
Sonnenberg A, Turner KO, Genta RM. Ethnic variations in the occurrence of colonic neoplasms. United Eur Gastroenterol J 2017;5:424–431.
Turner KO, Genta RM, Sonnenberg A. Lesions of all types exist in colon polyps of all sizes. Am J Gastroenterol 2018;113:303–306.
Sonnenberg A, Genta RM. Helicobacter pylori is a risk factor for colonic neoplasms. Am J Gastroenterol 2013;108:208–215.
Sonnenberg A, Turner KO, Genta RM. Low prevalence of Helicobacter pylori-positive peptic ulcers in private outpatient endoscopy centers in the United States. Am J Gastroenterol 2020;115:1145.
Sonnenberg A, Turner KO, Genta RM. Associations between gastric histopathology and the occurrence of colon polyps. Colorectal Dis 2020;22:812–815.
Sonnenberg A. Effects of birth cohort on long-term trends in mortality from colorectal cancer. Clin Gastroenterol Hepatol 2012;10:1389–1394.
Johnson CM, Wei C, Ensor JE et al. Meta-analyses of colorectal cancer risk factors. Cancer Causes Control 2013;24:1207–1222.
Dwyer AJ, Murphy CC, Boland CR et al. A summary of the fight colorectal cancer working meeting: exploring risk factors and etiology of sporadic early-age onset colorectal cancer. Gastroenterology 2019;157:280–308.
Jeffrey K, Lee JK, Merchant SA, Schneider JL et al. Proton pump inhibitor use and risk of gastric, colorectal, liver, and pancreatic cancers in a community-based population. Am J Gastroenterol 2020;115:706–715.
Rex DK, Ahnen DJ, Baron JA et al. Serrated lesions of the colorectum: review and recommendations from an expert panel. Am J Gastroenterol 2012;107:1315–1329.
Shaukat A, Holub J, Greenwald D, Eisen G, Schmitt C. Variation over time and factors associated with detection rates of sessile serrated lesion across the United States: results form a national sample using the GIQuIC Registry. Am J Gastroenterol 2021;116:95–99.
Funding
No funding was obtained for this study.
Author information
Authors and Affiliations
Contributions
Study conception and design: A Sonnenberg, KO Turner, RM Genta; data analysis: A Sonnenberg, RM Genta, KO Turner; writing of manuscript: A Sonnenberg, RM Genta.
Corresponding author
Ethics declarations
Conflict of interest
A Sonnenberg has no conflict of interest to declare. KO Turner and RM Genta are employed by Inform Diagnostics, Irving, TX.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sonnenberg, A., Turner, K.O. & Genta, R.M. Trends of Colonic Neoplasia in US Outpatient Endoscopy Centers. Dig Dis Sci 67, 4702–4707 (2022). https://doi.org/10.1007/s10620-021-07358-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-021-07358-8