Abstract
Background
A history of abdominal surgery is associated with difficulty in colonoscopy insertion. Few studies have reported effective colonoscopy insertion for patients who underwent abdominal surgery due to stomach cancer.
Aim
We aimed to compare the impact of supine position (SP) and left lateral position (LLP) as the starting position of colonoscopy insertion in patients who underwent abdominal surgery due to stomach cancer.
Methods
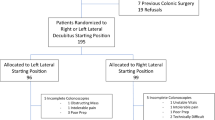
This was a prospective, randomized controlled trial. Patients undergoing colonoscopy for screening or post-polypectomy surveillance after gastrectomy due to stomach cancer were enrolled and randomized to the SP or LLP group as the starting position of colonoscopy insertion. All colonoscopic examinations were performed with a transparent cap. The primary outcome was to compare the cecal intubation time between the two groups.
Results
A total of 224 patients were enrolled. The mean cecal intubation time was not significantly different between the SP and LLP groups (364.5 s versus 306.9 s; p = 0.105). In patients with a lower body mass index (< 21 kg/m2) or who underwent gastrectomy within three years, the mean cecal intubation time of the LLP group was shorter than the SP group. In the multivariate analysis for the factors affecting to increase in the cecal intubation time (> 5 min), the starting position was not an independent factor.
Conclusion
Either the SP or LLP could serve as a possible starting position of colonoscopy insertion for patients who underwent abdominal surgery due to stomach cancer.



Similar content being viewed by others
References
Miller KD, Nogueira L, Mariotto AB et al. Cancer treatment and survivorship statistics, 2019. CA Cancer J Clin 2019;69:363–385. https://doi.org/10.3322/caac.21565.
Jung KW, Won YJ, Hong S et al. Prediction of cancer incidence and mortality in Korea, 2021. Cancer Res Treat 2021;53:316–322. https://doi.org/10.4143/crt.2021.290.
Gupta S, Cole AP, Marchese M et al. Use of preventive health services among cancer survivors in the U.S. Am J Prev Med 2018;55:830–838. https://doi.org/10.1016/j.amepre.2018.07.021.
Gweon TG, Yoon KT, Kim CH et al. Postgastrectomy gastric cancer patients are at high risk for colorectal neoplasia: a case control study. Intest Res 2021;19:239–246. https://doi.org/10.5217/ir.2020.00009.
Kahi CJ, Boland CR, Dominitz JA et al. Colonoscopy surveillance after colorectal cancer resection: recommendations of the US Multi-Society Task Force on colorectal cancer. Gastroenterology 2016;150:758-768.e711. https://doi.org/10.1053/j.gastro.2016.01.001.
Ghevariya V, Duddempudi S, Ghevariya N et al. Barriers to screening colonoscopy in an urban population: a study to help focus further efforts to attain full compliance. Int J Colorectal Dis 2013;28:1497–1503. https://doi.org/10.1007/s00384-013-1708-7.
Denberg TD, Melhado TV, Coombes JM et al. Predictors of nonadherence to screening colonoscopy. J Gen Intern Med 2005;20:989–995. https://doi.org/10.1111/j.1525-1497.2005.00164.x.
Clancy C, Burke JP, Chang KH et al. The effect of hysterectomy on colonoscopy completion: a systematic review and meta-analysis. Dis Colon Rectum 2014;57:1317–1323. https://doi.org/10.1097/dcr.0000000000000223.
Kim S, Choi J, Kim TH et al. Effect of previous gastrectomy on the performance of postoperative colonoscopy. J Gastric Cancer 2016;16:167–176. https://doi.org/10.5230/jgc.2016.16.3.167.
Lee SK, Kim TI, Shin SJ et al. Impact of prior abdominal or pelvic surgery on colonoscopy outcomes. J Clin Gastroenterol 2006;40:711–716. https://doi.org/10.1097/00004836-200609000-00010.
Menzies D, Ellis H. Intestinal obstruction from adhesions—How big is the problem? Ann R Coll Surg Engl 1990;72:60–63.
Ergul E, Korukluoglu B. Peritoneal adhesions: facing the enemy. Int J Surg 2008;6:253–260. https://doi.org/10.1016/j.ijsu.2007.05.010.
Zhao S, Yang X, Meng Q et al. Impact of the supine position versus left horizontal position on colonoscopy insertion: a 2-center, randomized controlled trial. Gastrointest Endosc 2019;89:1193-1201.e1191. https://doi.org/10.1016/j.gie.2019.01.009.
East JE, Bassett P, Arebi N et al. Dynamic patient position changes during colonoscope withdrawal increase adenoma detection: a randomized, crossover trial. Gastrointest Endosc 2011;73:456–463. https://doi.org/10.1016/j.gie.2010.07.046.
Ball AJ, Johal SS, Riley SA. Position change during colonoscope withdrawal increases polyp and adenoma detection in the right but not in the left side of the colon: results of a randomized controlled trial. Gastrointest Endosc 2015;82:488–494. https://doi.org/10.1016/j.gie.2015.01.035.
Klare P, Huth R, Haller B et al. Patient position and hypoxemia during propofol sedation for colonoscopy: a randomized trial. Endoscopy 2015;47:1159–1166. https://doi.org/10.1055/s-0034-1392329.
Vergis N, McGrath AK, Stoddart CH et al. Right Or Left in COLonoscopy (ROLCOL)? A randomized controlled trial of right- versus left-sided starting position in colonoscopy. Am J Gastroenterol 2015;110:1576–1581. https://doi.org/10.1038/ajg.2015.298.
Uddin FS, Iqbal R, Harford WV et al. Prone positioning of obese patients for colonoscopy results in shortened cecal intubation times: a randomized trial. Dig Dis Sci 2013;58:782–787. https://doi.org/10.1007/s10620-012-2468-x.
Rex DK. How I approach colonoscopy in anatomically difficult colons. Am J Gastroenterol 2020;115:151–154. https://doi.org/10.14309/ajg.0000000000000481.
Zhao SB, Yang X, Fang J et al. Effect of left lateral tilt-down position on cecal intubation time: a 2-center, pragmatic, randomized controlled trial. Gastrointest Endosc 2018;87:852–861. https://doi.org/10.1016/j.gie.2017.11.012.
Kim HH, Park SJ, Park MI et al. Transparent-cap-fitted colonoscopy shows higher performance with cecal intubation time in difficult cases. World J Gastroenterol 2012;18:1953–1958. https://doi.org/10.3748/wjg.v18.i16.1953.
Koido S, Ohkusa T, Nakae K et al. Factors associated with incomplete colonoscopy at a Japanese academic hospital. World J Gastroenterol 2014;20:6961–6967. https://doi.org/10.3748/wjg.v20.i22.6961.
Shah HA, Paszat LF, Saskin R et al. Factors associated with incomplete colonoscopy: a population-based study. Gastroenterology 2007;132:2297–2303. https://doi.org/10.1053/j.gastro.2007.03.032.
Anderson JC, Gonzalez JD, Messina CR et al. Factors that predict incomplete colonoscopy: thinner is not always better. Am J Gastroenterol 2000;95:2784–2787. https://doi.org/10.1111/j.1572-0241.2000.03186.x.
Qureshi A, BiBi S, Madhotra R. Body mass index & low CIR in colonoscopy! Gastroenterol Hepatol Bed Bench 2018;11:125–130.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kim, J.H., Choi, Y.J., Kwon, H.J. et al. Colonoscopy Insertion in Patients with Gastrectomy: Does Position Impact Cecal Intubation Time?. Dig Dis Sci 67, 4533–4540 (2022). https://doi.org/10.1007/s10620-021-07325-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-021-07325-3