Abstract
Background
Serum IgG4 level is a useful diagnostic marker for autoimmune pancreatitis (AIP), but it is difficult to use to predict relapse.
Aims
We investigated whether serum autotaxin (ATX) level is predictive of AIP relapse after steroid therapy.
Methods
Fifty-six patients with type 1 AIP were investigated. We measured serum ATX at the time of diagnosis. We selected 24 males for whom serum samples during steroid therapy had been obtained and measured serum ATX at steroid therapy for induction of remission and at maintenance therapy. In the relapse group, we also measured ATX at the time of relapse.
Results
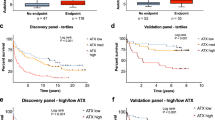
ATX was significantly higher in female patients than in male patients. In order to clarify changes in ATX during steroid therapy, we focused on 24 male patients. We found that ATX decreased significantly during steroid therapy for induction of remission and at the time of maintenance therapy. In half of all patients who relapsed during maintenance therapy, ATX was significantly elevated at the time of relapse compared with that of induction therapy (P = 0.039). When we compared ATX at the time of maintenance therapy between patients with relapse and without, we observed significantly higher ATX in the former (P = 0.024). We found that the combination of ATX and elastase-1 could predict relapse with high accuracy (95%).
Conclusions
Preliminary evidence suggests that serum ATX might serve as a candidate biomarker to predict relapse of AIP as well as to monitor the effect of steroid therapy.





Similar content being viewed by others
References
Yoshida K, Toki F, Takeuchi T, Watanabe S, Shiratori K, Hayashi N. Chronic pancreatitis caused by an autoimmune abnormality. Proposal of the concept of autoimmune pancreatitis. Dig Dis Sci. 1995;40:1561–1568. https://doi.org/10.1007/BF02285209.
Hamano H, Kawa S, Horiuchi A, et al. High serum IgG4 concentrations in patients with sclerosing pancreatitis. N Engl J Med. 2001;344:732–738.
Shimosegawa T, Chari ST, Frulloni L, et al. International consensus diagnostic criteria for autoimmune pancreatitis: guidelines of the International Association of Pancreatology. Pancreas. 2011;40:352–358.
Umehara H, Okazaki K, Masaki Y, et al. A novel clinical entity, IgG4-related disease (IgG4RD): general concept and details. Mod Rheumatol. 2012;22:1–14.
Kamisawa T, Okamoto A. Autoimmune pancreatitis: proposal of IgG4-related sclerosing disease. J Gastroenterol. 2006;41:613–625.
Okazaki K, Uchida K, Miyoshi H, Ikeura T, Takaoka M, Nishio A. Recent concepts of autoimmune pancreatitis and IgG4-related disease. Clin Rev Allergy Immunol. 2011;41:126–138.
Kamisawa T, Ryu JK, Kim MH, Okazaki K, Shimosegawa T, Chung JB. Recent advances in the diagnosis and management of autoimmune pancreatitis: similarities and differences in Japan and Korea. Gut Liver. 2013;7:394–400.
Ikeura T, Miyoshi H, Shimatani M, Uchida K, Takaoka M, Okazaki K. Long-term outcomes of autoimmune pancreatitis. World J Gastroenterol. 2016;22:7760–7766.
Masamune A, Nishimori I, Kikuta K, et al. Randomised controlled trial of long-term maintenance corticosteroid therapy in patients with autoimmune pancreatitis. Gut. 2017;66:487–494.
Kubota K, Kamisawa T, Okazaki K, et al. Low-dose maintenance steroid treatment could reduce the relapse rate in patients with type 1 autoimmune pancreatitis: a long-term Japanese multicenter analysis of 510 patients. J Gastroenterol. 2017;52:955–964.
Nakai Y, Ikeda H, Nakamura K, et al. Specific increase in serum autotaxin activity in patients with pancreatic cancer. Clin Biochem. 2011;44:576–581.
Quan M, Cui JJ, Feng X, Huang Q. The critical role and potential target of the autotaxin/lysophosphatidate axis in pancreatic cancer. Tumour Biol. 2017;39:1010428317694544.
Yamazaki T, Joshita S, Umemura T, et al. Association of serum autotaxin levels with liver fibrosis in patients with chronic hepatitis C. Sci Rep. 2017;7:46705.
Fujimori N, Umemura T, Kimura T, et al. Serum autotaxin levels are correlated with hepatic fibrosis and ballooning in patients with non-alcoholic fatty liver disease. World J Gastroenterol. 2018;24:1239–1249.
Joshita S, Ichikawa Y, Umemura T, et al. Serum autotaxin is a useful liver fibrosis marker in patients with chronic hepatitis B virus infection. Hepatol Res. 2018;48:275–285.
Joshita S, Umemura T, Usami Y, et al. Serum autotaxin is a useful disease progression marker in patients with primary biliary cholangitis. Sci Rep. 2018;8:8159.
Stracke ML, Krutzsch HC, Unsworth EJ, et al. Identification, purification, and partial sequence analysis of autotaxin, a novel motility-stimulating protein. J Biol Chem. 1992;267:2524–2529.
Moolenaar WH, Perrakis A. Insights into autotaxin: how to produce and present a lipid mediator. Nat Rev Mol Cell Biol. 2011;12:674–679.
Pradere JP, Gonzalez J, Klein J, et al. Lysophosphatidic acid and renal fibrosis. Biochim Biophys Acta. 2008;1781:582–587.
Tager AM, LaCamera P, Shea BS, et al. The lysophosphatidic acid receptor LPA1 links pulmonary fibrosis to lung injury by mediating fibroblast recruitment and vascular leak. Nat Med. 2008;14:45–54.
Pearson RK, Longnecker DS, Chari ST, et al. Controversies in clinical pancreatology: autoimmune pancreatitis: does it exist? Pancreas. 2003;27:1–13.
Masuda A, Nakamura K, Izutsu K, et al. Serum autotaxin measurement in haematological malignancies: a promising marker for follicular lymphoma. Br J Haematol. 2008;143:60–70.
Okazaki K, Uchida K. Autoimmune pancreatitis: the past, present, and future. Pancreas. 2015;44:1006–1016.
Kuruma S, Kamisawa T, Tabata T, et al. Clinical characteristics of patients with autoimmune pancreatitis with or without Mikulicz’s disease and Mikulicz’s disease alone. Gut Liver. 2013;7:96–99.
Ishii Y, Serikawa M, Sasaki T, et al. Impact of sclerosing dacryoadenitis/sialadenitis on relapse during steroid therapy in patients with type 1 autoimmune pancreatitis. Scand J Gastroenterol. 2019;54:259–264.
Mahajan VS, Mattoo H, Deshpande V, Pillai SS, Stone JH. IgG4-related disease. Annu Rev Pathol. 2014;9:315–347.
Benesch MG, Zhao YY, Curtis JM, McMullen TP, Brindley DN. Regulation of autotaxin expression and secretion by lysophosphatidate and sphingosine 1-phosphate. J Lipid Res. 2015;56:1134–1144.
Ota M, Katsuyama Y, Hamano H, et al. Two critical genes (HLA-DRB1 and ABCF1) in the HLA region are associated with the susceptibility to autoimmune pancreatitis. Immunogenetics. 2007;59:45–52.
Ghazale A, Chari ST, Zhang L, et al. Immunoglobulin G4-associated cholangitis: clinical profile and response to therapy. Gastroenterology. 2008;134:706–715.
de Pretis N, Amodio A, Bernardoni L, et al. Azathioprine maintenance therapy to prevent relapses in autoimmune pancreatitis. Clin Transl Gastroenterol. 2017;8:e90.
Hart PA, Topazian MD, Witzig TE, et al. Treatment of relapsing autoimmune pancreatitis with immunomodulators and rituximab: the Mayo Clinic experience. Gut. 2013;62:1607–1615.
Majumder S, Mohapatra S, Lennon RJ, et al. Rituximab maintenance therapy reduces rate of relapse of pancreaticobiliary immunoglobulin G4-related disease. Clin Gastroenterol Hepatol. 2018;16:1947–1953.
Kanno A, Masamune A, Okazaki K, et al. Nationwide epidemiological survey of autoimmune pancreatitis in Japan in 2011. Pancreas. 2015;44:535–539.
Acknowledgments
The authors thank the patients who agreed to participate in this study. We also thank the team members at Hiroshima University Hospital for clinical sample collection. We thank Rie Akiyama, Junko Sakamiya, Yumi Shimomura and Miyuki Matsushita for technical assistance; Chizuru Hiraguchi, Akemi Sada, Chikako Kanehara and Emi Nishio for clerical assistance; and other members of the Hiroshima University and RIKEN Center for Integrative Medical Sciences for assistance with various aspects of this study.
Funding
The authors have no grant support for this manuscript.
Author information
Authors and Affiliations
Contributions
KC conceived the study; AF, HF, DM, YI, MS and KC designed the study; AF, HF, YI, MS and KC managed and prepared serum samples; AF, HF, DM, YI, MS, MT, MI, HA and CNH performed data analysis; AF, HF, DM, CNH and KC wrote the manuscript; AF, HF, DM and KC summarized the whole results. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Fukiage, A., Fujino, H., Miki, D. et al. Clinical Usefulness of Serum Autotaxin for Early Prediction of Relapse in Male Patients with Type 1 Autoimmune Pancreatitis. Dig Dis Sci 66, 1268–1275 (2021). https://doi.org/10.1007/s10620-020-06338-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-020-06338-8