Abstract
Background
Liver metastasis is an indicator of unfavorable responses to immunotherapy in colorectal cancer patients. However, the difference of immune microenvironment between primary tumors and liver metastases has not been well understood.
Patients and Methods
Fifty-four colon cancer with liver metastasis patients who received resection of both primary and metastasis lesions have been analyzed. The immune score is based on the density of infiltrating immune cells (CD3+ cell, CD8+ cell, CD11b+ cell, CD11c+ cell, and CD33+ cell) in the center and margin of the tumor. The expression of immune markers between the primary tumor and hepatic metastases was analyzed using Wilcoxon’s signed rank test.
Results
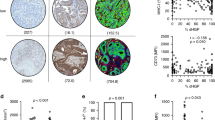
All the five markers had higher expression in tumor margins than center tumor in both primary tumor and hepatic metastases lesions. The expression of CD11c and CD11b had no difference between metastatic lesions and primary tumor. In tumor margins, except CD11b, all the other 4 markers expressed significantly higher in hepatic metastases than in primary tumor. Intra-tumor, CD3 had higher expression in primary tumor than in hepatic metastases, while CD33 had higher expression in hepatic metastases than in primary tumor. CD8+ CD3+ cells of the total CD8+ cell population in primary tumor was significantly higher than in hepatic metastases (36.42% vs. 24.88%, p = 0.0069).
Conclusions
The immune microenvironment between primary tumor and hepatic metastasis is different. More immunosuppressing cells in liver may partially explain why immunotherapy in colon cancer is less effective with liver metastatic disease.


Similar content being viewed by others
References
Darvin P, Toor SM, Sasidharan Nair V, Elkord E. Immune checkpoint inhibitors: recent progress and potential biomarkers. Exp Mol Med. 2018;50:165.
Ahn BC, Pyo KH, Xin CF, et al. Comprehensive analysis of the characteristics and treatment outcomes of patients with non-small cell lung cancer treated with anti-PD-1 therapy in real-world practice. J Cancer Res Clin Oncol. 2019;145:1613–1623.
Garde-Noguera J, Martin-Martorell P, De Julian M, et al. Predictive and prognostic clinical and pathological factors of nivolumab efficacy in non-small-cell lung cancer patients. Clin Transl Oncol. 2018;20:1072–1079.
Nosrati A, Tsai KK, Goldinger SM, et al. Evaluation of clinicopathological factors in PD-1 response: derivation and validation of a prediction scale for response to PD-1 monotherapy. Br J Cancer. 2017;116:1141–1147.
Tamiya M, Tamiya A, Inoue T, et al. Metastatic site as a predictor of nivolumab efficacy in patients with advanced non-small cell lung cancer: a retrospective multicenter trial. PLoS ONE. 2018;13:e0192227.
Tumeh PC, Hellmann MD, Hamid O, et al. Liver metastasis and treatment outcome with anti-PD-1 monoclonal antibody in patients with melanoma and NSCLC. Cancer Immunol Res. 2017;5:417–424.
Gordon SR, Maute RL, Dulken BW, et al. PD-1 expression by tumour-associated macrophages inhibits phagocytosis and tumour immunity. Nature. 2017;545:495–499.
Mayo SC, Pawlik TM. Current management of colorectal hepatic metastasis. Expert Rev Gastroenterol Hepatol. 2009;3:131.
Vibert E, Canedo L, Adam R. Strategies to treat primary unresectable colorectal liver metastases. Semin Oncol. 2005;32:33–39.
Kemeny N. Management of liver metastases from colorectal cancer. Oncology. 2006;20:1161–1176.
Lau WY, Lai ECH. Hepatic resection for colorectal liver metastases. Singap Med J. 2007;48:635–639.
Xu J, Fan J, Qin X, et al. Chinese guidelines for the diagnosis and comprehensive treatment of colorectal liver metastases (version 2018). J Cancer Res Clin Oncol. 2019;145:725–736.
Simoneau E, Vauthey JN. Progression of colorectal cancer liver metastasis after chemotherapy: a new test of time? Ann Surg Oncol. 2018;25:1469–1470.
Le DT, Uram JN, Wang H, et al. PD-1 blockade in tumors with mismatch-repair deficiency. N Engl J Med. 2015;372:2509–2520.
Angelova M, Mlecnik B, Vasaturo A, et al. Evolution of metastases in space and time under immune selection. Cell. 2018;175:751–765.e16.
Becht E, Giraldo NA, Germain C, et al. Immune contexture, immunoscore, and malignant cell molecular subgroups for prognostic and theranostic classifications of cancers. Adv Immunol. 2016;130:95–190.
McLemore LE, Janakiram M, Albanese J, et al. An immunoscore using PD-L1, CD68, and tumor-infiltrating lymphocytes (TILs) to predict response to neoadjuvant chemotherapy in invasive breast cancer. Appl Immunohistochem Mol Morphol. 2018;26:611–619.
Zou MX, Lv GH, Wang XB, et al. Clinical impact of the immune microenvironment in spinal chordoma: immunoscore as an independent favorable prognostic factor. Neurosurgery. 2019;84:E318–E333.
Sherwood AM, Emerson RO, Scherer D, et al. Tumor-infiltrating lymphocytes in colorectal tumors display a diversity of T cell receptor sequences that differ from the T cells in adjacent mucosal tissue. Cancer Immunol Immunother. 2013;62:1453–1461.
Kmiecik J, Poli A, Brons NH, et al. Elevated CD3+ and CD8+ tumor-infiltrating immune cells correlate with prolonged survival in glioblastoma patients despite integrated immunosuppressive mechanisms in the tumor microenvironment and at the systemic level. J Neuroimmunol. 2013;264:71–83.
Wang Y, Lin HC, Huang MY, et al. The immunoscore system predicts prognosis after liver metastasectomy in colorectal cancer liver metastases. Cancer Immunol Immunother. 2018;67:435–444.
Zhang QQ, Hu XW, Liu YL, et al. CD11b deficiency suppresses intestinal tumor growth by reducing myeloid cell recruitment. Sci Rep. 2015;5:15948.
Schmid MC, Khan SQ, Kaneda MM, et al. Integrin CD11b activation drives anti-tumor innate immunity. Nat Commun. 2018;9:5379.
Sun HL, Zhou X, Xue YF, et al. Increased frequency and clinical significance of myeloid-derived suppressor cells in human colorectal carcinoma. World J Gastroenterol. 2012;18:3303–3309.
Yang R, Cai TT, Wu XJ, et al. Tumour YAP1 and PTEN expression correlates with tumour-associated myeloid suppressor cell expansion and reduced survival in colorectal cancer. Immunology. 2018;155:263–272.
Rostamzadeh D, Haghshenas MR, Daryanoosh F, et al. Altered frequency of CD8(+) CD11c(+) T cells and expression of immunosuppressive molecules in lymphoid organs of mouse model of colorectal cancer. J Cell Physiol. 2019;234:11986–11998.
Wang Y, Lin HC, Huang MY, et al. The immunoscore system predicts prognosis after liver metastasectomy in colorectal cancer liver metastases. Cancer Immunol Immunother. 2017;67:1–10.
Patel S, Chung SH, White G, Bao S, Celermajer DS. The “atheroprotective” mediators apolipoprotein A-I and Foxp3 are over-abundant in unstable carotid plaques. Int J Cardiol. 2010;145:183–187.
Jamal R, Lapointe R, Cocolakis E, et al. Peripheral and local predictive immune signatures identified in a phase II trial of ipilimumab with carboplatin/paclitaxel in unresectable stage III or stage IV melanoma. J Immunother Cancer. 2017;5:83.
Markl B, Wieberneit J, Kretsinger H, et al. Number of intratumoral T lymphocytes is associated with lymph node size, lymph node harvest, and outcome in node-negative colon cancer. Am J Clin Pathol. 2016;145:826–836.
Pages F, Mlecnik B, Marliot F, et al. International validation of the consensus Immunoscore for the classification of colon cancer: a prognostic and accuracy study. Lancet. 2018;391:2128–2139.
Richards CH, Roxburgh CS, Powell AG, Foulis AK, Horgan PG, McMillan DC. The clinical utility of the local inflammatory response in colorectal cancer. Eur J Cancer. 2014;50:309–319.
Toor SM, Syed Khaja AS, El Salhat H, et al. Increased levels of circulating and tumor-infiltrating granulocytic myeloid cells in colorectal cancer patients. Front Immunol. 2016;7:560.
Sottoriva A, Spiteri I, Piccirillo SG, et al. Intratumor heterogeneity in human glioblastoma reflects cancer evolutionary dynamics. Proc Natl Acad Sci USA. 2013;110:4009–4014.
Thorn M, Point GR, Burga RA, Nguyen CT, Joseph Espat N, Katz SC. Liver metastases induce reversible hepatic B cell dysfunction mediated by Gr-1+ CD11b+ myeloid cells. J Leukoc Biol. 2014;96:883–894.
Halama N, Zoernig I, Berthel A, et al. Tumoral immune cell exploitation in colorectal cancer metastases can be targeted effectively by anti-CCR5 therapy in cancer patients. Cancer Cell. 2016;29:587–601.
Forestier C, Park SH, Wei D, Benlagha K, Teyton L, Bendelac A. T cell development in mice expressing CD1d directed by a classical MHC class II promoter. J Immunol. 2003;171:4096–4104.
Schimanski CC, Moehler M, Gockel I, et al. Expression of chemokine receptor CCR5 correlates with the presence of hepatic molecular metastases in K-ras positive human colorectal cancer. J Cancer Res Clin Oncol. 2011;137:1139–1145.
Qian DC, Xiao X, Byun J, et al. PI3K/Akt/mTOR signaling and plasma membrane proteins are implicated in responsiveness to adjuvant dendritic cell vaccination for metastatic colorectal cancer. Clin Cancer Res. 2017;23:399–406.
Acknowledgments
No.
Funding
This study was supported by National Natural Science Foundation of China (NSFC: 81602066 and 81772587); Natural Science Foundation of Guangdong Province (2016A030313280 and 2018A030310260); The Sci-Tech Foundation of Guangdong Province (2018YJ021); The Medical Science Foundation of Guangdong Province (A2016023 and 2018102516469945). Natural Science Foundation of Guangdong Province (Grant Number 2014A030312015), Science and Technology Program of Guangdong (Grant Number 2015B020232008), Science and Technology Program of Guangzhou (Grant Numbers 15570006, 201508020250, 201510161726583, 201604020003), Guangdong Esophageal Cancer Institute Science and Technology Program (Grant Number M201809), CSCO-HengRui Oncology Research Fund (Grant Number Y-HR2018-184), the third outstanding young talents training plan and Medical Scientist program of Sun Yat-sen University cancer center, Medical Science and Technology Research Fund Project of Guangdong Province (Grant Number A2015003).
Author information
Authors and Affiliations
Contributions
Conception and design of this study were carried out by MZQ, DJY, and LZ, QYL, MXP and SNZ. WTP conducted most part of the experiments, analyzed the data and wrote the manuscript. XLY, LPY and YXZ preformed the immunofluorescence. JZL, and YJZ collected the clinical data.
Corresponding author
Ethics declarations
Conflict of interest
No potential conflict of interest was disclosed.
Ethics approval and Consent to participate
All experiments were performed under the guidance of Sun Yat-Sen University Ethics Committee.
Consent for publication
All the authors have read and approved the manuscript.
Data availability
Data are available when request.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Zhou, SN., Pan, WT., Pan, MX. et al. Comparison of Immune Microenvironment Between Colon and Liver Metastatic Tissue in Colon Cancer Patients with Liver Metastasis. Dig Dis Sci 66, 474–482 (2021). https://doi.org/10.1007/s10620-020-06203-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-020-06203-8