Abstract
Background
Intestinal fibrosis is a common complication of Crohn’s disease (CD). Its exact mechanism is still unclear, and effective treatments to control or reverse the fibrosis process are unavailable. Epithelial–mesenchymal transition (EMT) may promote intestinal fibrosis by increasing deposition of extracellular matrix protein. IL-17A is a pro-inflammatory cytokine, and it has been shown as a profibrotic factor as its association with fibrosis of multiple organs was reported.
Aims
To assess the roles of IL-17A and EMT in the initiation and development of intestinal fibrosis and to verify the potential inductive effect of IL-17A on EMT.
Methods
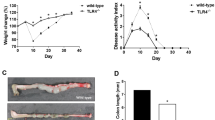
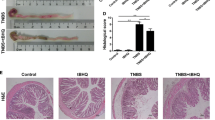
In this study, we evaluated the expression of IL-17A and EMT-related genes in colonic mucosal biopsy tissues of CD patients and control individuals. Then, we examined the changes of EMT-related genes and fibrosis-related genes of IEC-6 cells which cultured for 72 h under increasing concentrations of IL-17A or with TGF-β1, to verify the potential inductive effect of IL-17A on EMT in vitro. We blocked the IL-17A of the mouse model of TNBS-induced experimental intestinal colitis and fibrosis to further verify the potential inductive effect of IL-17A on EMT in vivo.
Results
We found the occurrence of EMT and high-level expression of IL-17A in intestinal mucosa of CD patients. Using IEC-6 cells, we showed that IL-17A may induce EMT in intestinal epithelial cells that come with reduced E-cadherin expression and increased expression of vimentin, snail, and α-SMA. We further found that anti-IL-17A treatment alleviated intestinal fibrosis through reducing EMT in mouse intestine.
Conclusions
Our study confirmed the involvement of IL-17A in the development of intestinal fibrosis through inducing EMT.








Similar content being viewed by others
References
Latella G, Di Gregorio J, Flati V, Rieder F, Lawrance IC. Mechanisms of initiation and progression of intestinal fibrosis in IBD. Scand J Gastroenterol. 2015;50:53–65.
Jeuring S, Van den Heuvel T, Zeegers M, et al. Disease behavior in Crohn’s disease patients diagnosed in the biological era—a Dutch population-based IBD-SL cohort study. Gastroenterology. 2015;148:2.
Cosnes J, Bourrier A, Nion-Larmurier I, Sokol H, Beaugerie L, et al. Factors affecting outcomes in Crohn’s disease over 15 years. Gut. 2012;61:1140–1145.
Pittet V, Rogler G, Michetti P, Fournier N, Vader JP, et al. Penetrating or stricturing diseases are the major determinants of time to first and repeat resection surgery in Crohn’s disease. Digestion. 2013;87:212–221.
Latella G, Papi C. Crucial steps in the natural history of inflammatory bowel disease. World J Gastroenterol. 2012;18:3790–3799.
Bernstein CN, Loftus EV Jr, Ng SC, Lakatos PL, Moum B, et al. Hospitalisations and surgery in Crohn’s disease. Gut. 2012;61:622–629.
Latella G, Sferra R, Vetuschi A, Zanninelli G, D’Angelo A, et al. Prevention of colonic fibrosis by Boswellia and Scutellaria extracts in rats with colitis induced by 2,4,5-trinitrobenzene sulphonic acid. Eur J Clin Invest. 2008;38:410–420.
Speca S, Giusti I, Rieder F, Latella G. Cellular and molecular mechanisms of intestinal fibrosis. World J Gastroenterol. 2012;18:3635–3661.
Rieder F, Fiocchi C. Intestinal fibrosis in inflammatory bowel disease—current knowledge and future perspectives. J Crohns Colitis. 2008;2:279–290.
Rieder F, Fiocchi C, Rogler G. Mechanisms, management, and treatment of fibrosis in patients with inflammatory bowel diseases. Gastroenterology. 2017;152:e346.
Lawrance IC, Rogler G, Bamias G, Breynaert C, Florholmen J, et al. Cellular and molecular mediators of intestinal fibrosis. J Crohns Colitis. 2017;11:1491–1503.
Rieder F. The gut microbiome in intestinal fibrosis: Environmental protector or provocateur? Sci Transl Med. 2013;5:190ps110.
Scharl M, Huber N, Lang S, Furst A, Jehle E, et al. Hallmarks of epithelial to mesenchymal transition are detectable in Crohn’s disease associated intestinal fibrosis. Clin Transl Med. 2015;4:1.
Scharl M, Frei S, Pesch T, Kellermeier S, Arikkat J, et al. Interleukin-13 and transforming growth factor beta synergise in the pathogenesis of human intestinal fistulae. Gut. 2013;62:63–72.
Flier SN, Tanjore H, Kokkotou EG, Sugimoto H, Zeisberg M, et al. Identification of epithelial to mesenchymal transition as a novel source of fibroblasts in intestinal fibrosis. J Biol Chem. 2010;285:20202–20212.
Rieder F, Kessler SP, West GA, Bhilocha S, de la Motte C, et al. Inflammation-induced endothelial-to-mesenchymal transition: a novel mechanism of intestinal fibrosis. Am J Pathol. 2011;179:2660–2673.
Rieder F, Brenmoehl J, Leeb S, Scholmerich J, Rogler G. Wound healing and fibrosis in intestinal disease. Gut. 2007;56:130–139.
Uehara H, Nakagawa T, Katsuno T, Sato T, Isono A, et al. Emergence of fibrocytes showing morphological changes in the inflamed colonic mucosa. Dig Dis Sci. 2010;55:253–260. https://doi.org/10.1007/s10620-009-0730-7.
Brittan M, Chance V, Elia G, Poulsom R, Alison MR, et al. A regenerative role for bone marrow following experimental colitis: contribution to neovasculogenesis and myofibroblasts. Gastroenterology. 2005;128:1984–1995.
Nieto MA, Huang RY, Jackson RA, Thiery JP. Emt. Cell. 2016;166:21–45.
Grigore AD, Jolly MK, Jia D, Farach-Carson MC, Levine H. Tumor budding: the name is EMT. Partial EMT. J Clin Med. 2016;5:51.
Lamouille S, Xu J, Derynck R. Molecular mechanisms of epithelial-mesenchymal transition. Nat Rev Mol Cell Biol. 2014;15:178–196.
Yang J, Zhou CZ, Zhu R, Fan H, Liu XX, et al. miR-200b-containing microvesicles attenuate experimental colitis associated intestinal fibrosis by inhibiting epithelial-mesenchymal transition. J Gastroenterol Hepatol. 2017;32:1966–1974.
Scharl M, Bruckner RS, Rogler G. The two sides of the coin: similarities and differences in the pathomechanisms of fistulas and stricture formations in irritable bowel disease. United Eur Gastroenterol J. 2016;4:506–514.
Okamoto Y, Hasegawa M, Matsushita T, Hamaguchi Y, Huu DL, et al. Potential roles of interleukin-17A in the development of skin fibrosis in mice. Arthritis Rheum. 2012;64:3726–3735.
Wilson MS, Madala SK, Ramalingam TR, Gochuico BR, Rosas IO, et al. Bleomycin and IL-1beta-mediated pulmonary fibrosis is IL-17A dependent. J Exp Med. 2010;207:535–552.
Tan Z, Qian X, Jiang R, Liu Q, Wang Y, et al. IL-17A plays a critical role in the pathogenesis of liver fibrosis through hepatic stellate cell activation. J Immunol. 2013;191:1835–1844.
Guan Q, Ma Y, Hillman CL, Qing G, Ma AG, et al. Targeting IL-12/IL-23 by employing a p40 peptide-based vaccine ameliorates TNBS-induced acute and chronic murine colitis. Mol Med. 2011;17:646–656.
Latella G, Caprilli R, Travis S. In favour of early surgery in Crohn’s disease: a hypothesis to be tested. J Crohns Colitis. 2011;5:1–4.
Quencer KB, Nimkin K, Mino-Kenudson M, Gee MS. Detecting active inflammation and fibrosis in pediatric Crohn’s disease: prospective evaluation of MR-E and CT-E. Abdominal Imaging. 2013;38:705–713.
Scheiffele F, Fuss IJ. Induction of TNBS colitis in mice. Curr Protoc Immunol. 2002;49:19.
Fichtner-Feigl S, Fuss IJ, Young CA, Watanabe T, Geissler EK, et al. Induction of IL-13 triggers TGF-beta1-dependent tissue fibrosis in chronic 2,4,6-trinitrobenzene sulfonic acid colitis. J Immunol. 2007;178:5859–5870.
Alex P, Zachos NC, Nguyen T, Gonzales L, Chen TE, et al. Distinct cytokine patterns identified from multiplex profiles of murine DSS and TNBS-induced colitis. Inflamm Bowel Dis. 2009;15:341–352.
Dieleman LA, Pena AS, Meuwissen SG, van Rees EP. Role of animal models for the pathogenesis and treatment of inflammatory bowel disease. Scand J Gastroenterol Suppl. 1997;223:99–104.
Videla S, Vilaseca J, Medina C, Mourelle M, Guarner F, et al. Selective inhibition of phosphodiesterase-4 ameliorates chronic colitis and prevents intestinal fibrosis. J Pharmacol Exp Ther. 2006;316:940–945.
Wirtz S, Neufert C, Weigmann B, Neurath MF. Chemically induced mouse models of intestinal inflammation. Nat Protoc. 2007;2:541–546.
Lawrance IC, Wu F, Leite AZ, Willis J, West GA, et al. A murine model of chronic inflammation-induced intestinal fibrosis down-regulated by antisense NF-kappa B. Gastroenterology. 2003;125:1750–1761.
Bettenworth D, Rieder F. Reversibility of stricturing Crohn’s disease-fact or fiction? Inflamm Bowel Dis. 2016;22:241–247.
Fiocchi C, Lund PK. Themes in fibrosis and gastrointestinal inflammation. Am J Physiol Gastrointest Liver Physiol. 2011;300:G677–G683.
Rieder F, Fiocchi C. Mechanisms of tissue remodeling in inflammatory bowel disease. Dig Dis. 2013;31:186–193. https://doi.org/10.1159/000353364.
Peinado H, Olmeda D, Cano A. Snail, Zeb and bHLH factors in tumour progression: An alliance against the epithelial phenotype? Nat Rev Cancer. 2007;7:415–428.
Biancheri P, Pender SL, Ammoscato F, Giuffrida P, Sampietro G, et al. The role of interleukin 17 in Crohn’s disease-associated intestinal fibrosis. Fibrogenesis Tissue Repair. 2013;6:13.
Mi S, Li Z, Yang HZ, Liu H, Wang JP, et al. Blocking IL-17A promotes the resolution of pulmonary inflammation and fibrosis via TGF-beta1-dependent and -independent mechanisms. J Immunol. 2011;187:3003–3014.
Vittal R, Fan L, Greenspan DS, Mickler EA, Gopalakrishnan B, et al. IL-17 induces type V collagen overexpression and EMT via TGF-beta-dependent pathways in obliterative bronchiolitis. Am J Physiol Lung Cell Mol Physiol. 2013;304:L401–L414.
Mendez MG, Kojima S, Goldman RD. Vimentin induces changes in cell shape, motility, and adhesion during the epithelial to mesenchymal transition. FASEB J. 2010;24:1838–1851.
Mifflin RC, Pinchuk IV, Saada JI, Powell DW. Intestinal myofibroblasts: targets for stem cell therapy. Am J Physiol Gastrointest Liver Physiol. 2011;300:G684–G696.
Zhu MY, Lu YM, Ou YX, Zhang HZ, Chen WX. Dynamic progress of 2,4,6-trinitrobenzene sulfonic acid induced chronic colitis and fibrosis in rat model. J Dig Dis. 2012;13:421–429.
Fichtner-Feigl S, Strober W, Geissler EK, Schlitt HJ. Cytokines mediating the induction of chronic colitis and colitis-associated fibrosis. Mucosal Immunol. 2008;1:S24–S27.
Verstockt B, Ferrante M, Vermeire S, Van Assche G. New treatment options for inflammatory bowel diseases. J Gastroenterol. 2018;53:585–590.
Zorzi F, Monteleone I, Sarra M, Calabrese E, Marafini I, et al. Distinct profiles of effector cytokines mark the different phases of Crohn’s disease. Gastroenterology. 2013;144:S820–S820.
Acknowledgments
This work was supported by Liaoning Province Science and Technology Project (2013225049). The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Author information
Authors and Affiliations
Contributions
MJ-S was involved in conception and design, interpretation of data, and manuscript revision. HJ-Z, YN-Z, and HZ performed the experiments. LG and YL collected the biopsy samples. HJ-Z YN-Z analyzed the data. MJ-S contributed reagents/materials/analysis tools. HJ-Z and YN-Z wrote the paper. All authors approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
All authors do not have a commercial or other association that might pose a conflict of interest.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Zhang, HJ., Zhang, YN., Zhou, H. et al. IL-17A Promotes Initiation and Development of Intestinal Fibrosis Through EMT. Dig Dis Sci 63, 2898–2909 (2018). https://doi.org/10.1007/s10620-018-5234-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-018-5234-x