Abstract
Background
The use of volatile organic compounds (VOCs) in bile was recently studied and appeared promising for diagnosis of malignancy. Noninvasive diagnosis of malignant biliary strictures by using VOCs in urine has not been studied.
Aim
To identify potential VOCs in urine to diagnose malignant biliary strictures.
Methods
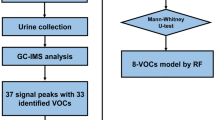
In this prospective cross-sectional study, urine was obtained immediately prior to ERCP from consecutive patients with biliary strictures. Selected-ion flow-tube mass spectrometry was used to analyze the concentration of VOCs in urine samples.
Results
Fifty-four patients with biliary strictures were enrolled. Fifteen patients had malignant stricture [six cholangiocarcinoma (CCA) and nine pancreatic cancer], and 39 patients had benign strictures [10 primary sclerosing cholangitis (PSC) and 29 with benign biliary conditions including chronic pancreatitis and papillary stenosis]. The concentration of several compounds (ethanol and 2-propanol) was significantly different in patients with malignant compared with benign biliary strictures (p < 0.05). Using receiver operating characteristic curve analysis, we developed a model for the diagnosis of malignant biliary strictures adjusted for age and gender based on VOC levels of 2-propranol, carbon disulfide, and trimethyl amine (TMA). The model [−2.4191 * log(2-propanol) + 1.1617 * log(TMA) − 1.2172 * log(carbon disulfide)] ≥ 7.73 identified the patients with malignant biliary stricture [area under the curve (AUC = 0.83)], with 93.3 % sensitivity and 61.5 % specificity (p = 0.009). Comparing patients with CCA and PSC, the model [38.864 * log(ethane) − 3.989 * log(1-octene)] ≤ 169.9 could identify CCA with 80 % sensitivity and 100 % specificity (AUC = 0.9).
Conclusions
Measurement of VOCs in urine may diagnose malignant biliary strictures noninvasively.





Similar content being viewed by others
Abbreviations
- AUC:
-
Area under curve
- CCA:
-
Cholangiocarcinoma
- EUS:
-
Endoscopic ultrasound
- ERCP:
-
Endoscopic retrograde cholangiopancreatography
- FNA:
-
Fine-needle aspiration
- FISH:
-
Fluorescence in situ hybridization
- PSC:
-
Primary sclerosing cholangitis
- TMA:
-
Trimethyl amine
- VOCs:
-
Volatile organic compounds
References
Qureshi K, Jesudoss R, Al-Osaimi AM. The treatment of cholangiocarcinoma: a hepatologist’s perspective. Curr Gastroenterol Rep. 2014;16:412. doi:10.1007/s11894-014-0412-2.
Friman S. Cholangiocarcinoma–current treatment options. Scand J Surg.. 2011;100:30–34.
DeOliveira ML. Liver transplantation for cholangiocarcinoma: current best practice. Curr Opin Organ Transpl. 2014;19:245–252.
Tan X, Xiao K, Liu W, Chang S, Zhang T, Tang H. Prognostic factors of distal cholangiocarcinoma after curative surgery: a series of 84 cases. Hepatogastroenterology. 2013;60:1892–1895.
Navaneethan U, Njei B, Venkatesh PG, Vargo JJ, Parsi MA. Fluorescence in situ hybridization for diagnosis of cholangiocarcinoma in primary sclerosing cholangitis: a systematic review and meta-analysis. Gastrointest Endosc. 2013;. doi:10.1016/j.gie.2013.11.001.
Navaneethan U, Njei B, Lourdusamy V, et al. Comparative effectiveness of biliary brush cytology and intraductal biopsy for detection of malignant biliary strictures: a systematic review and meta-analysis. Gastrointest Endosc. 2014;. doi:10.1016/j.gie.2014.09.017.
Trikudanathan G, Navaneethan U, Njei B, Vargo JJ, Parsi MA. Diagnostic yield of bile duct brushings for cholangiocarcinoma in primary sclerosing cholangitis: a systematic review and meta-analysis. Gastrointest Endosc.. 2014;79:783–789.
Navaneethan U, Njei B, Venkatesh PG, Lourdusamy V, Sanaka MR. Endoscopic ultrasound in the diagnosis of cholangiocarcinoma as the etiology of biliary strictures: a systematic review and meta-analysis. Gastroenterol Rep (Oxf). 2014 Aug 27.
Levy MJ, Heimbach JK, Gores GJ. Endoscopic ultrasound staging of cholangiocarcinoma. Curr Opin Gastroenterol. 2012;28:244–252.
Lin MS, Huang JX, Yu H. Elevated serum level of carbohydrate antigen 19-9 in benign biliary stricture diseases can reduce its value as a tumor marker. Int J Clin Exp Med. 2014;7:744–750.
Ong SL, Sachdeva A, Garcea G, et al. Elevation of carbohydrate antigen 19.9 in benign hepatobiliary conditions and its correlation with serum bilirubin concentration. Dig Dis Sci. 2008;53:3213–3217.
Navaneethan U, Parsi MA, Gutierrez NG, et al. Volatile organic compounds in bile can diagnose malignant biliary strictures in the setting of pancreatic cancer: a preliminary observation. Gastrointest Endosc. 2014;. doi:10.1016/j.gie.2014.04.016.
Navaneethan U, Parsi MA, Gutierrez NG, et al. Volatile organic compounds in bile for early diagnosis of cholangiocarcinoma in patients with primary sclerosing cholangitis: a pilot study. Gastrointest Endosc. 2014;. doi:10.1016/j.gie.2014.09.041.
Metzger J, Negm AA, Plentz RR, et al. Urine proteomic analysis differentiates cholangiocarcinoma from primary sclerosing cholangitis and other benign biliary disorders. Gut. 2013;62:122–130.
Navaneethan U, Gutierrez NG, Venkatesh PG, et al. Lipidomic profiling of bile in distinguishing benign from malignant biliary strictures: a single-blinded pilot study. Am J Gastroenterol. 2014;109:895–902.
de Lacy Costello B, Amann A, Al-Kateb H, et al. A review of the volatiles from the healthy human body. J Breath Res. 2014;8:014001. doi:10.1088/1752-7155/8/1/014001.
de Boer NK, de Meij TG, Oort FA, et al. The scent of colorectal cancer: detection by volatile organic compound analysis. Clin Gastroenterol Hepatol. 2014;12:1085–1089. doi:10.1016/j.cgh.2014.05.005.
Filipiak W, Filipiak A, Sponring A, et al. Comparative analyses of volatile organic compounds (VOCs) from patients, tumors and transformed cell lines for the validation of lung cancer-derived breath markers. J Breath Res. 2014;8:027111. doi:10.1088/1752-7155/8/2/027111.
Altomare DF, Di Lena M, Porcelli F, et al. Exhaled volatile organic compounds identify patients with colorectal cancer. Br J Surg. 2013;100:144–150.
de Meij TG, Larbi IB, van der Schee MP, et al. Electronic nose can discriminate colorectal carcinoma and advanced adenomas by fecal volatile biomarker analysis: proof of principle study. Int J Cancer. 2014;134:1132–1138. doi:10.1002/ijc.28446.
Huang J, Kumar S, Abbassi-Ghadi N, Spaněl P, Smith D, Hanna GB. Selected ion flow tube mass spectrometry analysis of volatile metabolites in urine headspace for the profiling of gastro-esophageal cancer. Anal Chem. 2013;85:3409–3416. doi:10.1021/ac4000656.
Kumar S, Huang J, Cushnir JR, Španěl P, Smith D, Hanna GB. Selected ion flow tube-MS analysis of headspace vapor from gastric content for the diagnosis of gastro-esophageal cancer. Anal Chem. 2012;84:9550–9557. doi:10.1021/ac302409a.
Miekisch W, Schubert JK, Noeldge-Schomburg GF. Diagnostic potential of breath analysis–focus on volatile organic compounds. Clin Chim Acta. 2004;347:25–39.
Probert CS, Ahmed I, Khalid T, Johnson E, Smith S, Ratcliffe N. Volatile organic compounds as diagnostic biomarkers in gastrointestinal and liver diseases. J Gastrointestin Liver Dis. 2009;18:337–343.
Volinsky R, Kinnunen PK. Oxidized phosphatidylcholines in membrane-level cellular signaling: from biophysics to physiology and molecular pathology. FEBS J. 2013;280:2806–2816.
Wang Z, Klipfell E, Bennett BJ, Koeth R, et al. Gut flora metabolism of phosphatidylcholine promotes cardiovascular disease. Nature. 2011;472:57–63.
Tesiram YA, Lerner M, Stewart C, Njoku C, Brackett DJ. Utility of nuclear magnetic resonance spectroscopy for pancreatic cancer studies. Pancreas. 2012;41:474–480.
He XH, Li WT, Gu YJ, et al. Metabonomic studies of pancreatic cancer response to radiotherapy in a mouse xenograft model using magnetic resonance spectroscopy and principal components analysis. World J Gastroenterol. 2013;19:4200–4208.
Acknowledgments
We also would like to thank the Clinical Research Unit members at the Cleveland Clinic who helped in processing the urine samples. The study was supported by a research grant from the American College of Gastroenterology (ACG) Grant (to U.N), BRCP 08-049 Tech 09-003 Third Frontier Program grant from the Ohio Department of Development (ODOD) [to R.D] and in part by the National Institutes of Health, National Center for Research Resources, CTSA, UL1TR 000439-06 Cleveland, Ohio. Dr Dweik was also supported by the following grants: HL107147, HL081064, HL103453, HL109250, and RR026231 from the National Institutes of Health (NIH).
Conflict of interest
The authors declared no financial conflict of interest pertaining to this paper.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Navaneethan, U., Parsi, M.A., Lourdusamy, D. et al. Volatile Organic Compounds in Urine for Noninvasive Diagnosis of Malignant Biliary Strictures: A Pilot Study. Dig Dis Sci 60, 2150–2157 (2015). https://doi.org/10.1007/s10620-015-3596-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-015-3596-x