Abstract
Background/Aims
Bacterial translocation (BT) promotes microinflammation in predialysis patients with end-stage renal disease (ESRD). However, the change in BT has not been reported in ESRD patients undergoing regular hemodialysis treatment. The present study investigated whether hemodialysis promotes gut BT and microinflammation.
Methods
The blood, gut, and dialysate of hemodialysis patients were analyzed using bacterial 16S rDNA amplification and DNA pyrosequencing to determine the presence of bacteria and alteration in gut microbiomes. High-sensitive C-reactive protein (hs-CRP), interleukin-6 (IL-6), and endotoxin were also determined. Plasma d-lactate was tested for gut permeability.
Results
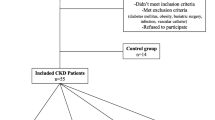
Bacteria were present in the plasma of 12 out of 52 ESRD patients. The majority of the bacteria detected in the blood were also distributed in the gut of ESRD patients on the basis of the phylogenetics of the blood and gut microbial specimens in the patients. In patient, groups treated with and without hemodialysis, the plasma hs-CRP, IL-6, and endotoxin levels differed between the positive and negative plasma bacterial DNA. In patients who were positive in blood bacteria, the bacterial DNA concentration was positively correlated with plasma levels of CRP and IL-6. The ESRD patients who underwent hemodialysis had a different flora and showed slightly higher levels of hs-CRP, IL-6, and plasma endotoxin, compared with those in ESRD patients who did not undergo hemodialysis.
Conclusion
ESRD, rather than hemodialysis, primarily contributes to BT and microinflammation in ESRD patients. Hemodialysis may exaggerate microinflammation in ESRD patients to some extent.



Similar content being viewed by others
References
Schindler R. Causes and therapy of microinflammation in renal failure[J]. Nephrol Dial Transpl. 2004;19:V34–V40.
Zimmermann J, Herrlinger S, Pruy A, et al. Inflammation enhances cardiovascular risk and mortality in hemodialysis patients[J]. Kidney Int. 1999;55:648–658.
Kotanko P, Carter M, Levin NW. Intestinal bacterial microflora–a potential source of chronic inflammation in patients with chronic kidney disease[J]. Nephrol Dial Transpl. 2006;21:2057–2060.
Wang F, Jiang H, Shi K, et al. Gut bacterial translocation is associated with microinflammation in end-stage renal disease patients[J]. Nephrology (Carlton). 2012;17:733–738.
Wang F, Zhang P, Jiang H, et al. Gut bacterial translocation contributes to microinflammation in experimental uremia[J]. Dig Dis Sci. 2012;57:2856–2862.
Zimmermann J, Herrlinger S, Pruy A, et al. Inflammation enhances cardiovascular risk and mortality in hemodialysis patients[J]. Kidney Int. 1999;55:648–658.
Mcintyre CW, Harrison LE, Eldehni MT, et al. Circulating endotoxemia: a novel factor in systemic inflammation and cardiovascular disease in chronic kidney disease[J]. Clin J Am Soc Nephrol. 2011;6:133–141.
Zaza G, Granata S, Rascio F, et al. A specific immune transcriptomic profile discriminates chronic kidney disease patients in predialysis from hemodialyzed patients[J]. BMC Med Genomics. 2013;6:17.
Vaziri ND, Wong J, Pahl M, et al. Chronic kidney disease alters intestinal microbial flora[J]. Kidney Int. 2013;83:308–315.
Vaziri ND, Dure-Smith B, Miller R, et al. Pathology of gastrointestinal tract in chronic hemodialysis patients: an autopsy study of 78 cases[J]. Am J Gastroenterol. 1985;80:608–611.
Bossola M, Sanguinetti M, Scribano D, et al. Circulating bacterial-derived DNA fragments and markers of inflammation in chronic hemodialysis patients[J]. Clin J Am Soc Nephrol. 2009;4:379–385.
Murphy MA, Kendall KC, Higbee JA. An evaluation of long-term preservation methods for brown bear (Ursus arctos) faecal DNA samples[J]. Conserv Genet. 2002;3:435–440.
Gomila M, Gasco J, Gil J, et al. A molecular microbial ecology approach to studying hemodialysis water and fluid[J]. Kidney Int. 2006;70:1567–1576.
Bossola M, Sanguinetti M, Scribano D, et al. Circulating bacterial-derived DNA fragments and markers of inflammation in chronic hemodialysis patients[J]. Clin J Am Soc Nephrol. 2009;4:379–385.
Naaber P, Smidt I, Tamme K, et al. Translocation of indigenous microflora in an experimental model of sepsis[J]. J Med Microbiol. 2000;49:431–439.
de Almeida DJ, de Aguilar-Nascimento JE, Nascimento M, et al. Bacterial translocation in experimental uremia[J]. Urol Res. 2004;32:266–270.
Bossola M, Sanguinetti M, Scribano D, et al. Circulating bacterial-derived DNA fragments and markers of inflammation in chronic hemodialysis patients[J]. Clin J Am Soc Nephrol. 2009;4:379–385.
Merino A, Nogueras S, Garcia-Maceira T, et al. Bacterial DNA and endothelial damage in haemodialysis patients[J]. Nephrol Dial Transpl. 2008;23:3635–3642.
Ritz E. Intestinal-renal syndrome: mirage or reality?[J]. Blood Purif. 2011;31:70–76.
Flobert C, Cellier C, Berger A, et al. Right colonic involvement is associated with severe forms of ischemic colitis and occurs frequently in patients with chronic renal failure requiring hemodialysis[J]. Am J Gastroenterol. 2000;95:195–198.
Berg RD, Wommack E, Deitch EA. Immunosuppression and intestinal bacterial overgrowth synergistically promote bacterial translocation[J]. Arch Surg. 1988;123:1359–1364.
Navarro JF, Mora C, Leon C, et al. Amino acid losses during hemodialysis with polyacrylonitrile membranes: effect of intradialytic amino acid supplementation on plasma amino acid concentrations and nutritional variables in nondiabetic patients[J]. Am J Clin Nutr. 2000;71:765–773.
Vaziri ND, Yuan J, Rahimi A, et al. Disintegration of colonic epithelial tight junction in uremia: a likely cause of CKD-associated inflammation[J]. Nephrol Dial Transpl. 2012;27:2686–2693.
Vaziri ND, Yuan J, Nazertehrani S, et al. Chronic kidney disease causes disruption of gastric and small intestinal epithelial tight junction[J]. Am J Nephrol. 2013;38:99–103.
Vaziri ND, Goshtasbi N, Yuan J, et al. Uremic plasma impairs barrier function and depletes the tight junction protein constituents of intestinal epithelium[J]. Am J Nephrol. 2012;36:438–443.
Vaziri ND, Yuan J, Norris K. Role of urea in intestinal barrier dysfunction and disruption of epithelial tight junction in chronic kidney disease[J]. Am J Nephrol. 2012;37:1–6.
Vaziri ND, Yuan J, Khazaeli M, et al. Oral activated charcoal adsorbent (AST-120) ameliorates chronic kidney disease-induced intestinal epithelial barrier disruption[J]. Am J Nephrol. 2013;37:518–525.
Martinez VB, Gonzalez-Juanatey JR. Markers of inflammation and cardiovascular disease: clinical applications of C-reactive protein determination[J]. Am J Cardiovasc Drugs. 2009;9:3–7.
Acknowledgments
The authors wish to thank the patients and dialysis staff for their participation. The authors are also grateful to Mr. Shaoli Cheng (Medicine School of Xi’an Jiaotong University, China) in critically revising the manuscript. This work was supported by National Natural Science Foundation of China, No. 30872457.
Conflict of interest
The authors have no conflict of interest to disclose. The results presented in this paper have not been published elsewhere.
Author information
Authors and Affiliations
Corresponding author
Additional information
Kehui Shi and Feiqian Wang have contributed equally to this work.
Rights and permissions
About this article
Cite this article
Shi, K., Wang, F., Jiang, H. et al. Gut Bacterial Translocation May Aggravate Microinflammation in Hemodialysis Patients. Dig Dis Sci 59, 2109–2117 (2014). https://doi.org/10.1007/s10620-014-3202-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-014-3202-7