Abstract
Background
The incidence of cholangiocarcinoma (CCA) continues to rise. Orthotopic liver transplantation (OLT) can be used for selected patients with localized but unresectable hilar CCA. Although initial post-OLT survival rates were poor, outcomes after introduction of the Mayo Clinic protocol have been more promising and there has been increased interest in OLT for CCA nationally.
Aims
The aim of this study is to determine post-transplant survival and prognostic factors for patients undergoing OLT for CCA.
Methods
A retrospective analysis of all patients with CCA listed nationwide for OLT between October 1987 and May 2008 was performed using the Scientific Registry of Transplant Recipients database. Survival curves were generated using the Kaplan–Meier method and compared using log-rank test.
Results
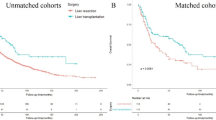
Of 595 patients with CCA listed for OLT, 359 (60.3 %) underwent OLT. Median age at OLT was 49 years, 66 % were male and 91 % were Caucasian. The median follow-up time was 2 years. There has been an increasing number of liver transplants performed for CCA since 2000. The 1- and 5-year probability of survival was 85.8 and 51.4 %, respectively. On multivariate analysis, significant prognostic factors for decreased post-OLT survival included transplant before 2000 (HR 11.25, 95 % CI 1.28–98.7) and acute cellular rejection (HR 5.64, 95 % CI 1.14–27.8).
Conclusions
Survival after transplant for CCA has improved over time, and OLT is being used more frequently in the treatment of CCA. Significant predictors of post-OLT survival include a history of acute rejection and date of transplant in relation to the publication of Mayo protocol results.




Similar content being viewed by others
References
Shaib Y, El-Serag HB. The epidemiology of cholangiocarcinoma. Semin Liver Dis. 2004;24:115–125.
Shaib YH, Davila JA, McGlynn K, El-Serag HB. Rising incidence of intrahepatic cholangiocarcinoma in the United States: a true increase? J Hepatol. 2004;40:472–477.
Taylor-Robinson SD, Toledano MB, Arora S, et al. Increase in mortality rates from intrahepatic cholangiocarcinoma in England and Wales 1968–1998. Gut. 2001;48:816–820.
Broome U, Olsson R, Loof L, et al. Natural history and prognostic factors in 305 Swedish patients with primary sclerosing cholangitis. Gut. 1996;38:610–615.
Singal AG, Rakoski MO, Salgia RJ, et al. The clinical presentation and prognostic factors for intrahepatic and extrahepatic cholangiocarcinoma in a tertiary care centre. Aliment Pharmacol Ther. 2010;31:625–633.
Ahrendt SA, Cameron JL, Pitt HA. Current management of patients with perihilar cholangiocarcinoma. Adv Surg. 1996;30:427–452.
Madariaga JR, Iwatsuki S, Todo S, Lee RG, Irish W, Starzl TE. Liver resection for hilar and peripheral cholangiocarcinomas: a study of 62 cases. Ann Surg. 1998;227:70–79.
Malhi H, Gores GJ. Review article: the modern diagnosis and therapy of cholangiocarcinoma. Aliment Pharmacol Ther. 2006;23:1287–1296.
Guthrie CM, Haddock G, De Beaux AC, Garden OJ, Carter DC. Changing trends in the management of extrahepatic cholangiocarcinoma. Br J Surg. 1993;80:1434–1439.
Bismuth H, Nakache R, Diamond T. Management strategies in resection for hilar cholangiocarcinoma. Ann Surg. 1992;215:31–38.
Tan JC, Coburn NG, Baxter NN, Kiss A, Law CH. Surgical management of intrahepatic cholangiocarcinoma—a population-based study. Ann Surg Oncol. 2008;15:600–608.
Grossman EJ, Millis JM. Liver transplantation for non-hepatocellular carcinoma malignancy: indications, limitations, and analysis of the current literature. Liver Transpl. 2010;16:930–942.
Castaldo ET, Pinson CW. Liver transplantation for non-hepatocellular carcinoma malignancy. HPB (Oxf). 2007;9:98–103.
Penn I. Hepatic transplantation for primary and metastatic cancers of the liver. Surgery. 1991;110:726–735.
Singal A, Welling TH, Marrero JA. Role of liver transplantation in the treatment of cholangiocarcinoma. Expert Rev Anticancer Ther. 2009;9:491–502.
De Vreede I, Steers JL, Burch PA, et al. Prolonged disease-free survival after orthotopic liver transplantation plus adjuvant chemoirradiation for cholangiocarcinoma. Liver Transpl. 2000;6:309–316.
Gores GJ, Heimbach JK, Rosen CB. Liver transplantation for non-hepatocellular carcinoma malignancies. Liver Transpl. 2010;16:S22–S25.
Murad D, Kim WR, Harnois DM, et al. Effects of neoadjuvant chemoradiation, followed by liver transplantation, for perihilar cholangiocarcinoma at 12 US centers. Gastroenterology. 2012;143:88–98.
Meyer CG, Penn I, James L. Liver transplantation for cholangiocarcinoma: results in 207 patients. Transplantation. 2000;69:1633–1637.
Becker NS, Rodriguez JA, Barshes NR, O’Mahony CA, Goss JA, Aloia TA. Outcomes analysis for 280 patients with cholangiocarcinoma treated with liver transplantation over an 18-year period. J Gastrointest Surg. 2008;12:117–122.
Heimbach JK, Gores GJ, Haddock MG, et al. Predictors of disease recurrence following neoadjuvant chemotherapy and liver transplantation for unresectable perihilar cholangiocarcinoma. Transplantation. 2006;82:1703–1707.
Acknowledgments
The data reported here have been supplied by the Arbor Research Collaborative for Health (Arbor Research) as the contractor for the SRTR. The interpretation and reporting of these data are the responsibility of the author(s) and in no way should be seen as an official policy of or interpretation by the SRTR or the US Government. The authors have no grant support to report for this study.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Salgia, R.J., Singal, A.G., Fu, S. et al. Improved Post-Transplant Survival in the United States for Patients with Cholangiocarcinoma After 2000. Dig Dis Sci 59, 1048–1054 (2014). https://doi.org/10.1007/s10620-013-2626-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-013-2626-9