Abstract
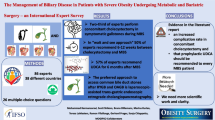
Objective To prospectively evaluate the frequency of upper gastrointestinal symptoms and associated disorders in morbidly obese patients with endoscopy and histology prior to their gastric bypass surgery in comparison with age- and sex-matched nonobese control subjects. Methods All patients who were scheduled to undergo laparoscopic gastric bypass for treatment of morbid obesity (body mass index, BMI > 40 kg/m2) during a 1-year period (n = 101) were included in the study. Age- and sex-matched nonobese patients who were seen in the medical clinics during the study period were enrolled as control subjects. The demographic data, total body weight, body mass index, and gastrointestinal symptoms were recorded, and the results of upper endoscopy and histology were tabulated. Endoscopic documentation of hiatal hernia, esophagitis, gastritis, gastric polyps, and peptic ulcer disease was also noted along with the histologic findings of the mucosal biopsies from the upper gastrointestinal tract. Results The prevalence of heartburn as a symptom was significantly higher (P < 0.05) in the morbidly obese patients (32.6%) compared with in the control group (18.8%). Endoscopically, the prevalence of hiatal hernia was also significantly higher (P < 0.05) in the morbidly obese group (38.6%) compared with in the control group (13.8%). Similarly the frequency of endoscopically and histologically identified gastritis was significantly higher (P < 0.01) in the morbidly obese patient group. However, the frequency of histologically identified Helicobacter pylori was not statistically different in the two groups. Conclusion These observations suggest a significant increase in the frequency of heartburn, hiatal hernia, and histologically identified gastritis in morbidly obese patients.

Similar content being viewed by others
References
Flegal KM, Carroll MD, Ogden CL, et al. Prevalence and trends in obesity among U.S. adults, 1999–2000. JAMA. 2002;288:1723–1727.
Burton BT, Foster WR, Hirsch J, et al. Health implications of obesity. National Institute of Health Consensus Development conference statement. Ann Intern Med. 1985;103:1073–1077.
Delgado-Aros S, Locke Gr, Camilleri M, et al. Obesity is associated with increased risk of gastrointestinal symptoms: a population based study. Am J Gastroenterol. 2004;99:1801–1806. doi:10.1111/j.1572-0241.2004.30887.x.
Sutter M, Dorta G, Giusti V, et al. Gastroesophageal reflux and esophageal motility disorders in morbidly obese patients. Obes Surg. 2004;14:959–966. doi:10.1381/0960892041719581.
Stene-Larson G, Weberg R, Froshov Larson I, et al. Relationship of overweight to hiatus hernia and reflux esophagitis. Scand J Gastroenterol. 1988;23:427–432. doi:10.3109/00365528809093890.
Lundell L, Ruth M, Sandberg N, et al. Does massive obesity promote abnormal gastroesophageal reflux. Dig Dis Sci. 1995;40:1632–1635. doi:10.1007/BF02212682.
Buchwald H. Consensus conference statement: bariatric surgery for morbid obesity; health implications for patients, health professionals and third party players. J Am Coll Surg. 2005;200:593–604. doi:10.1016/j.jamcollsurg.2004.10.039.
Freedman DS, Khan LK, Serdula MK, et al. Trends and correlates of class 3 obesity in the United States from 1990 through 2000. JAMA. 2002;288(14):1758–1761. doi:10.1001/jama.288.14.1758.
NIH consensus statement. Gastrointestinal surgery for severe obesity. NIH Consensus Development Conference. 1991;9
Singh R, Fisher BL. Sensitivity and specificity of post operative upper GI series following gastric bypass. Obes Surg. 2003;13:73–75. doi:10.1381/096089203321136629.
Crowell MD, Cheskin LJ, Musial F. Prevalence of gastrointestinal symptoms in obese and normal weight binge eaters. Am J Gastroenterol. 1994;89:387–391.
Locke GRIII, Talley NJ, Fett SL, et al. Risk factors associated with symptoms of gastroesophageal reflux. Am J Med. 1999;106:642–649. doi:10.1016/S0002-9343(99)00121-7.
Tally NJ, Howell S, Poulton R. Obesity and chronic gastrointestinal tract symptoms in young adults: a birth cohort study. Am J Gastroenterol. 2004;99:1807–1814. doi:10.1111/j.1572-0241.2004.30388.x.
Frezza EE, Shebani KO, Robertson J, et al. Morbid obesity causes, chronic increase of intraabdominal pressure. Dig Dis Sci. 2007;52:1038–1041.
Mahmood Z, Mc Namara D. Gastroesophageal reflux disease and ulcer disease. Aliment Pharmacol Ther. 2003;18(suppl 3):31–37.
Renshaw AA, Rabaza JR, Gonzalez AM, et al. Helicobacter pylori infection in patients undergoing gastric bypass surgery for morbid obesity. Obes Surg. 2001;11(3):281–283.
Everhart JE, Kruszon- Moran D, et al. Seroprevalence and ethnic differences in Helicobacter pylori infection among adults in the United States. J Infect Dis. 2000;181:1359–1363.
Zigman JM, Elmquist JK. Minireview: from anorexia to obesity—the Yin and Yang of body weight control. Endcrinology. 2003;144(9):3749–3756.
Lee H-M, Wang G, Englander EW, et al. Ghrelin, a new gastrointestinal endocrine peptide that stimulates insulin secretion: enteric distribution, ontogeny, influence of endocrine, and dietary manipulations. Endocrinology. 2002;143(1):185–190.
Mora M, Scarfone A, Valenza V, et al. Ghrelin does not influence gastric emptying in obese subjects. Obes Res. 2005;13:739–744.
Tschop M, Weyer C, Tataranni PA, et al. Circulating ghrelin levels are decreased in human obesity. Diabetes. 2001;50:707–709.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Dutta, S.K., Arora, M., Kireet, A. et al. Upper Gastrointestinal Symptoms and Associated Disorders in Morbidly Obese Patients: A Prospective Study. Dig Dis Sci 54, 1243–1246 (2009). https://doi.org/10.1007/s10620-008-0485-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-008-0485-6