Abstract
Cisplatin is the effective chemotherapeutic drug in colon cancer treatment, but its therapeutic efficacy is limited by intrinsic or acquired drug resistance and detrimental side effects. Therefore, improving the effect of cisplatin chemotherapy remains a great challenge. The previous study identified that USP39 was relevant to cisplatin resistance of lung cancer. However, the function and mechanisms of USP39 regulating the chemosensitivity of cisplatin in colorectal cancer remain unclear. In this study, we reveal that USP39 is associated with colon cancer cells sensitivity to cisplatin. Depletion of USP39 enhances the cisplatin-induced apoptosis in HCT116 cells. Conversely, overexpression of USP39 attenuates apoptosis in RKO cells. Furthermore, we demonstrate that USP39 depletion promotes apoptosis induced by cisplatin, which is related with the induction of oxidative stress and DNA damage response. Further studies show that USP39 regulates cisplatin-induced apoptosis dependent on p53. The underlying mechanism is demonstrated by knocking down USP39, that results in p53 upregulation, associated with its prolonged half-life. Collectively, our findings reveal that USP39 might be a negative factor of the p53 mediated cisplatin sensitivity of colon cancer, and suggest USP39 as a potential molecular target for cisplatin chemotherapy of colon cancer.
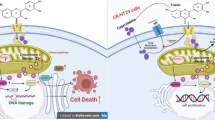
Graphical abstract








Similar content being viewed by others
Data availability
Most of data and materials generated or analyzed during this study are included in this published. Other data are available from the corresponding authors on reasonable request.
References
Allende-Vega N, Dayal S, Agarwala U, Sparks A, Bourdon JC, Saville MK. p53 is activated in response to disruption of the pre-mRNA splicing machinery. Oncogene. 2013;32(1):1–14. https://doi.org/10.1038/onc.2012.38.
Branch P, Masson M, Aquilina G, Bignami M, Karran P. Spontaneous development of drug resistance: mismatch repair and p53 defects in resistance to cisplatin in human tumor cells. Oncogene. 2000;19(28):3138–45. https://doi.org/10.1038/sj.onc.1203668.
Cepeda V, Fuertes MA, Castilla J, Alonso C, Quevedo C, Pérez JM. Biochemical mechanisms of cisplatin cytotoxicity. Anticancer Agents Med Chem. 2007;7(1):3–18. https://doi.org/10.2174/187152007779314044.
Ciombor KK, Bekaii-Saab T. A comprehensive review of sequencing and combination strategies of targeted agents in metastatic colorectal cancer. Oncologist. 2018;23(1):25–34. https://doi.org/10.1634/theoncologist.2017-0203.
Dasari S, Tchounwou PB. Cisplatin in cancer therapy: molecular mechanisms of action. Eur J Pharmacol. 2014;5(740):364–78. https://doi.org/10.1016/j.ejphar.2014.07.025.
Fuertes MA, Castilla J, Alonso C, Pérez JM. Cisplatin biochemical mechanism of action: from cytotoxicity to induction of cell death through interconnections between apoptotic and necrotic pathways. Curr Med Chem. 2003;10(3):257–66. https://doi.org/10.2174/0929867033368484.
Gallagher WM, Cairney M, Schott B, Roninson IB, Brown R. Identification of p53 genetic suppressor elements which confer resistance to cisplatin. Oncogene. 1997;14(2):185–93. https://doi.org/10.1038/sj.onc.1200813.
Galluzzi L, Senovilla L, Vitale I, Michels J, Martins I, Kepp O, et al. Molecular mechanisms of cisplatin resistance. Oncogene. 2012;31(15):1869–83. https://doi.org/10.1038/onc.2011.384.
Hientz K, Mohr A, Bhakta-Guha D, Efferth T. The role of p53 in cancer drug resistance and targeted chemotherapy. Oncotarget. 2017;8(5):8921–46. https://doi.org/10.18632/oncotarget.13475.
Hofseth LJ, Hussain SP, Harris CC. p53: 25 years after its discovery. Trends Pharmacol Sci. 2004;25(4):177–81. https://doi.org/10.1016/j.tips.2004.02.009.
Huang Y, Sadee W. Membrane transporters and channels in chemoresistance and -sensitivity of tumor cells. Cancer Lett. 2006;239(2):168–82. https://doi.org/10.1016/j.canlet.2005.07.032.
Inamura K. Colorectal cancers: an update on their molecular pathology. Cancers (Basel). 2018;10(1):26–44. https://doi.org/10.3390/cancers10010026.
Kalyan A, Kircher S, Shah H, Mulcahy M, Benson A. Updates on immunotherapy for colorectal cancer. J Gastrointest Oncol. 2018;9(1):160–9. https://doi.org/10.21037/jgo.2018.01.17.
Keum N, Giovannucci E. Global burden of colorectal cancer: emerging trends, risk factors and prevention strategies. Nat Rev Gastroenterol Hepatol. 2019;16(12):713–32. https://doi.org/10.1038/s41575-019-0189-8.
Kim CW, Lu JN, Go SI, Jung JH, Yi SM, Jeong JH, et al. p53 restoration can overcome cisplatin resistance through inhibition of Akt as well as induction of Bax. Int J Oncol. 2013;43(5):1495–502. https://doi.org/10.3892/ijo.2013.2070.
Kirsch DG, Kastan MB. Tumor-suppressor p53: implications for tumor development and prognosis. J Clin Oncol. 1998;16(9):3158–68. https://doi.org/10.1200/JCO.1998.16.9.3158.
Lin X, Ramamurthi K, Mishima M, Kondo A, Christen RD, Howell SB. P53 modulates the effect of loss of DNA mismatch repair on the sensitivity of human colon cancer cells to the cytotoxic and mutagenic effects of cisplatin. Cancer Res. 2001;61(4):1508–16.
McQuade RM, Stojanovska V, Bornstein JC, Nurgali K. Colorectal cancer chemotherapy: the evolution of treatment and new approaches. Curr Med Chem. 2017;24(15):1537–57. https://doi.org/10.2174/0929867324666170111152436.
Modest DP, Pant S, Sartore-Bianchi A. Treatment sequencing in metastatic colorectal cancer. Eur J Cancer. 2019;109:70–83. https://doi.org/10.1016/j.ejca.2018.12.019.
Muller PA, Vousden KH. p53 mutations in cancer. Nat Cell Biol. 2013;15(1):2–8. https://doi.org/10.1038/ncb2641.
Park JH, Zhuang J, Li J, Hwang PM. p53 as guardian of the mitochondrial genome. FEBS Lett. 2016;590(7):924–34. https://doi.org/10.1002/1873-3468.12061.
Perego P, Giarola M, Righetti SC, Supino R, Caserini C, Delia D, et al. Association between cisplatin resistance and mutation of p53 gene and reduced bax expression in ovarian carcinoma cell systems. Cancer Res. 1996;56(3):556–62.
Roelands J, Kuppen PJK, Vermeulen L, Maccalli C, Decock J, Marincola FM, et al. Immunogenomic classification of colorectal cancer and therapeutic implications. Int J Mol Sci. 2017;18(10):2229–48. https://doi.org/10.3390/ijms18102229.
Sakaguchi K, Herrera JE, Saito S, Miki T, Bustin M, Vassilev A, Anderson CW, Appella E. DNA damage activates p53 through a phosphorylation-acetylation cascade. Genes Dev. 1998;12(18):2831–41. https://doi.org/10.1101/gad.12.18.2831.
Sanz-Garcia E, Grasselli J, Argiles G. M Elena Elez, Josep Tabernero, Current and advancing treatments for metastatic colorectal cancer. Expert Opin Biol Ther. 2016;16(1):93–110. https://doi.org/10.1517/14712598.2016.1108405.
Siegel RL, Miller KD, Jemal A. Cancer statistics, 2019. CA Cancer J Clin. 2019;69(1):7–34. https://doi.org/10.3322/caac.21551.
Srinivas US, Tan BWQ, Vellayappan BA, Jeyasekharan AD. ROS and the DNA damage response in cancer. Redox Biol. 2019;25:101084. https://doi.org/10.1016/j.redox.2018.101084.
Swift LH, Golsteyn RM. Cytotoxic amounts of cisplatin induce either checkpoint adaptation or apoptosis in a concentration-dependent manner in cancer cells. Biol Cell. 2016;108(5):127–48. https://doi.org/10.1111/boc.201500056.
Taguchi T, Nazneen A, Abid MR, Razzaque MS. Cisplatin-associated nephrotoxicity and pathological events. Contrib Nephrol. 2005;148:107–21. https://doi.org/10.1159/000086055.
Wang L, Chen T, Li X, Yan W, Lou Y, Liu Z, et al. USP39 promotes ovarian cancer malignant phenotypes and carboplatin chemoresistance. Int J Oncol. 2019;55(1):277–88. https://doi.org/10.3892/ijo.2019.4818.
Wu C. Systemic therapy for colon cancer. Surg Oncol Clin N Am. 2018;27(2):235–42. https://doi.org/10.1016/j.soc.2017.11.001.
Wu J, Chen Y, Geng G, Li L, Yin P, Nowsheen S, et al. USP39 regulates DNA damage response and chemo-radiation resistance by deubiquitinating and stabilizing CHK2. Cancer Lett. 2019;449:114–24. https://doi.org/10.1016/j.canlet.2019.02.015.
Xing Z, Sun F, He W, Wang Z, Song X, Zhang F. Downregulation of ubiquitin-specific peptidase 39 suppresses the proliferation and induces the apoptosis of human colorectal cancer cells. Oncol Lett. 2018;15(4):5443–50. https://doi.org/10.3892/ol.2018.8061.
Yan C, Yuan J, Xu J, Zhang G, Li X, Zhang B, et al. Ubiquitin-specific peptidase 39 regulates the process of proliferation and migration of human ovarian cancer via p53/p21 pathway and EMT. Med Oncol. 2019;36(11):95–107. https://doi.org/10.1007/s12032-019-1308-7.
Yuan J, Li X, Zhang G, Cheng W, Wang W, Lei Y, Ma Q, Song G. USP39 mediates p21-dependent proliferation and neoplasia of colon cancer cells by regulating the p53/p21/CDC2/cyclin B1 axis. Mol Carcinog. 2021;60(4):265–78. https://doi.org/10.1002/mc.23290.
Zhang P, Yi LH, Meng GY, Zhang HY, Sun HH, Cui LQ. Apelin-13 attenuates cisplatin-induced cardiotoxicity through inhibition of ROS-mediated DNA damage and regulation of MAPKs and AKT pathways. Free Radic Res. 2017;51(5):449–59. https://doi.org/10.1080/10715762.2017.1313414.
Zhao Y, Zhang B, Lei Y, Sun J, Zhang Y, Yang S, et al. Knockdown of USP39 induces cell cycle arrest and apoptosis in melanoma. Tumour Biol. 2016;37(10):13167–76. https://doi.org/10.1007/s13277-016-5212-x.
Acknowledgements
We thank Prof. Han You for HCT116p53null cell line, and we also would like to acknowledge the editors and reviewers for their helpful suggestions on this manuscript.
Funding
This work is supported by the grants from the National Natural Science Foundation of China (81872045), and the Special Fund for Public Welfare Research Institutes of Fujian Province (2020R11010032-3).
Author information
Authors and Affiliations
Contributions
Jiahui Yuan and Gang Song designed and conceived the experiments; Jiahui Yuan, Xiaomei Li, and Yuqi Zhang performed the experiments and collected and analyzed data; Weiwei Wang, Weipeng Cheng, and Yongbin Lei collected data, and provided support for flow cytometry; Jiahui Yuan wrote the paper; Jiahui Yuan and Gang Song were responsible for the revision of manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
All animal research protocols were approved by the Institutional Animal Care and Use Committee of Xiamen University (IACUC No. XMULAC20180056).
Consent to participate
Not applicable.
Consent for publication
All authors have agreed to publish this manuscript.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Highlights
1. USP39 attenuates the antitumor activity of cisplatin on colon cancer cells.
2. USP39 depletion enhances cisplatin-induced apoptosis via the induction of oxidative stress and DNA damage response.
3. USP39 regulates cisplatin-induced apoptosis dependent on p53.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Yuan, J., Li, X., Zhang, Y. et al. USP39 attenuates the antitumor activity of cisplatin on colon cancer cells dependent on p53. Cell Biol Toxicol 39, 1995–2010 (2023). https://doi.org/10.1007/s10565-021-09683-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10565-021-09683-0