Abstract
Pancreatic cancer is a deadly disease that is increasing in incidence throughout the world. There are no clear causal factors associated with the incidence of pancreatic cancer; however, some correlation to smoking, diabetes and alcohol has been described. Recently, a few studies have linked the human microbiome (oral and gastrointestinal tract) to pancreatic cancer development. A perturbed microbiome has been shown to alter normal cells while promoting cancer-related processes such as increased cell signaling, immune system evasion and invasion. In this article, we will review in detail the alterations within the gut and oral microbiome that have been linked to pancreatic cancer and explore the ability of other microbiomes, such as the lung and skin microbiome, to contribute to disease development. Understanding ways to identify a perturbed microbiome can result in advancements in pancreatic cancer research and allow for prevention, earlier detection and alternative treatment strategies for patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
1.1 Pancreatic Cancer
Pancreatic cancer is a deadly and aggressive disease with increase in incidence rates throughout the world. Currently within the USA, the 5-year overall survival rate is 10.8% for pancreatic cancer [1]. Within the scope of pancreatic cancer, there are two main types of tumors: pancreatic ductal adenocarcinoma (PDAC) and pancreatic neuroendocrine tumors (PanNETs). PDAC tumors, the most common type, are epithelial exocrine tumors that normally originate within the pancreatic ducts, whereas PNETs originate from pancreatic islet cells and are sometimes functioning endocrine tumors, capable of secreting various hormones such as insulin and glucagon [2,3,4]. Regardless of the type of pancreatic cancer, this deadly disease lacks early detection markers, has no effective therapies and has an overall poor prognosis.
Currently, there are some identified causes of pancreatic cancer including correlations to diet, obesity and smoking but the underlying genetic risk factors are largely unknown. PDAC has been linked to mutations in the Breast Cancer Gene 2 (BRCA2) protein and other DNA damage repair proteins but these mutations are present only in a small subset of patients, 5–7% [3]. Individuals who carry familial syndromes such as multiple endocrine neoplasia syndrome 1 (MEN1), von Hippel-Lindau disease (VHL), neurofibromatosis type 1 (NF-1) and tuberous sclerosis (TSC) are at a higher risk of developing PNET type tumors but this only accounts for < 10% of the PNET patient population [4]. Regardless of the cause of disease, the majority of pancreatic cancers are not detected until they are in their final stages due to ambiguous symptoms such as back pain and loss of appetite that are normally mistaken for other etiologies. There is a lack of understanding of the underlying pathogenesis of this disease as well as a lack of effective strategies for early detection and prevention. One route of exploration is the link between the human microbiome and pancreatic cancer development. In this review, we will highlight some of the cutting-edge research that is being performed in relation to pancreatic cancer and the microbiome and offer a fresh perspective into future directions and ways to enhance this area of study.
1.2 History of the Microbiome
Recent research has been dedicated to understanding human microbiome and how alterations within the microbiome contributes to disease development. The microbiome consists of a large and heterogeneous population of bacteria that resides within a specific organ or region of the body and has a role in assisting the host in survival. There are various areas in the body where microbiomes reside including the gut, mouth and skin. The human microbiome has been identified as a contributing factor to disease as early as the 1600s [5]. In the 1860s, the pediatrician Theodor Escherich discovered the colon microbe Escherichia coli and revolutionized the concept that the human body symbiotically survives with microbial organisms [5]. Dr. Henry Tissier was the first to isolate Bifidobacterium and administer it as a probiotic [6]. The discovery of classical microbiology techniques such as the gram stain and bacterial isolation techniques have paved the way for current research into the human microbiome. Microbiome includes bacteria, viruses, archaea and fungi, whereas in healthy individuals all of these species coexist symbiotically to perform critical functions such as metabolism, which the host needs to survive.
1.3 The Gut and Oral Microbiome
The gut microbiome is located within the gastrointestinal tract and is responsible for a variety of physiologic functions including enhancing digestion and metabolism and contributing to the host immune defense [7]. The gut microbiome is composed of two separate bacterial phyla: the Firmicutes and the Bacteroidetes, but the presence of other phyla such as Proteobacteria, Actinobacteria and organisms like yeast can also be present [7]. The microbiome of the oral cavity consists of over 700 bacterial species along with fungi, viruses and protozoa with only around 60% of bacterial species having been categorized [8, 9]. As the digestion process starts with saliva breakdown of food in the oral cavity, the microbiome’s role begins here.
Gut dysbiosis was found to be a contributing factor to many diseases including inflammatory bowel disease (IBD), pancreatic cancer, obesity, allergies and autism [10]. Gut dysbiosis is also linked to chronic diseases. One example is Pseudomonas aeruginosa, which is found in the oral cavities of cystic fibrosis patients [11]. The integrity and composition of the oral microbiome is directly correlated to maintaining oral and systemic body health [12]. A clear link exists between poor oral health (untreated dental and periodontal diseases), improper dental care and an increased risk for disease development later in life such as cancer, heart attack, stroke, pneumonia and rheumatoid arthritis (RA) [13,14,15,16,17]. During inflammation of the oral cavity or periodontitis, the increase in pro-inflammatory cytokines and infiltration of T cells is an initiating stress event within the body leading to these conditions [13]. Moreover, it has been hypothesized that bacteria may invade endothelial cells and secrete toxins and other proteases, which contributes further to disease development. Patients that have had aortic aneurysms have been found to have an infiltration of various species of gram-positive bacteria like Streptococcus mutans [15]. High-risk RA has been strongly linked to oral microbe dysbiosis and bacteria within the saliva of RA patients are being explored as potential biomarkers for this disease [16]. A socioeconomic disparity exists within populations of non-Caucasian descent exhibiting poorer oral microbial health due to difficulties either accessing care due to logistic or cost of care issues [18]. In addition, periodontitis microbiota of HIV infected individuals was assessed in order to understand how pathogenic microflora are altered in special patient populations [19].
Initially, studies involving the microbiome were focused on specific bacteria within a specific organ or region of the body. It was not until 1995 that the whole genome of a bacteria, Haemophilus influenzae, was sequenced and what followed was an explosion into the field of microbiology [20]. After the development of second- and third-generation sequencing, coined next-generation sequencing, samples of complex biological mixtures containing abundant and rare samples could be assessed using their 16S rRNA sequences, highly conserved nucleotide sequences and separated out using computational methods [21]. Nevertheless, the field lacks a streamlined way to obtain useful and clinically relevant information from these massive datasets due to costs, time and other practical considerations.
1.4 The Skin Microbiome
The skin is the largest organ of the body and is a host to a variety of microbes including bacteria and fungi. Understanding the skin microbiome is a paradoxical concept as the skin protects the body from invading pathogens; however, it is a host to millions of these microbes. Depending on the condition of the skin: oily or dry, the composition of the microbiome differs. Grice et al. found that sebaceous sites (oily) had a large composition of Propionibacteria and Staphylococci species, whereas Corynebacterium mainly colonized in moist sites and both ß-proteobacteria and flavobacteriales were in the sites of dry skin [22]. The microbiome of the skin evolves throughout life. The microflora of the skin forms during birth through initial bacterial colonization on the skin and during developmental changes during puberty into adulthood, where the microbiome shifts further [23]. It is also important to note that females have more microbiota diversity than males due to sex hormones, thinner skin and less sweating and the skin microbiome may be more diverse than the gut microbiome [24, 25].
Since the skin is the barrier to the inside of the body, dysbiosis of the skin microbiome is mainly attributed to systemic infections and inflammatory skin diseases such as acne, psoriasis and rosacea [26]. Although these conditions are not as severe as others that are caused by the oral and gut microbiome, a case can be made for linking diseases of the skin to other systemic diseases. Psoriasis is normally found to be on the skin as abnormal growth of plaques but in a handful of patients (7%–26%) can also turn to psoriatic arthritis, a painful autoimmune condition, which has a similar presentation to RA. Severe cases have been linked to an increased risk of chronic pancreatitis, pancreatic and other gastrointestinal cancer development [27, 28]. Infection with the human papillomavirus (HPV), which can cause warts on the skin, has been linked to a variety of cancers including cervical, anal and oral cancer [29]. Recently, a strain of HPV, HPV-16, was found to be present within a mucinous neoplastic cyst of the pancreas suggesting a possible role in pancreatic cancer carcinogenesis [30].
1.5 Lung Microbiome
The lung microbiome also consists of a variety of organisms (bacteria, viruses, fungi etc) that are commonly obtained from the air inhalation of a particular environment [31]. Depending on the environment, the inhalation can consist of either commensal bacterial species (Streptococcus spp., Haemophilus spp., Veillonella spp., Aspergillus spp. and Candida spp.) or specifically harmful bacteria (Haemophilus influenzae, Streptococcus pneumoniae and Moraxella catarrhalis) [31]. There is a proposed link between the lung and gut microbiome that requires further investigation. Unlike the gut, the lung microbiome is constantly exposed to changing conditions such as changes in temperature, pH and pressure and has to adapt accordingly [31]. Further, Wang et al. have found that patients who experience digestive problems, such as inflammatory bowel disease (IBD), have more issues with pulmonary abnormalities and increased inflammation [32]. Recently, it was found that patients with chronic obstructive pulmonary disease (COPD) have a perturbed gut microbiome including increases in the Streptococcus and Lachnospiraceae species, particularly the Streptococcus parasanguinis B bacteria [33]. Although there is no direct anatomical connection between the two organs, the body is a dynamic and rapidly changing system that frequently experiences cross talk between differing organ systems.
2 The Microbiome Influences Pancreatic Cancer Development
2.1 Inflammation and Pancreatic Cancer
Inflammation is among a root cause of pancreatic cancer development, specifically PDAC. Chronic inflammation of the pancreas, caused by chronic pancreatitis, results in exocrine and endocrine damage leading to a cycle of necrosis and fibrosis events mediated by pancreatic stellate cells (PSCs) [34]. PSCs are exocrine functioning cells, mainly the acini, which are involved in tissue repair and secreting digestion enzymes [35]. Not only are cells within the pancreas susceptible to inflammation signaling but also inflammatory changes alter the tumor microenvironment, specifically cancer associated fibroblasts (CAFs). CAFs compose a large portion of the pancreatic tumor microenvironment and are involved with the secretion of extracellular matrix and other inflammatory factors. CAFs are essentially differentiated PSCs that result in perpetuating disease and influencing treatment resistance [36]. CAFs have the ability to secrete various inflammatory signals such as interleukins, chemokines and inflammatory factors [37].
There has been a clear link established between inflammation, via Ikß Kinase 2 or COX2, to P53 deficient pancreatic cells developing into PDAC [38]. Interleukin 1a (IL-1a) is another pro-inflammatory cytokine that is secreted by the tumor microenvironment, specifically CAFs, that perpetuates this disease to drive KRAS signaling [39]. STAT3, a well-known pancreatic cancer-driving gene, was found to be activated by KRAS mutant cells that recruit myeloid cells to secrete IL-6 and perpetuate disease development and progression [39]. CAFs are normally heterogeneous within the microenvironment and have either inflammatory functions or myofibroblastic functions [40]. Studies have shown that the myofibroblastic subset, although not specifically signaling for inflammatory markers, can indirectly increase the inflammatory CAF population leading to a decrease in cytotoxic T-cells and expand regulatory T-cells leading to immune evasion [40].
Not only is PDAC regulated by inflammation but also inflammatory processes influence PanNETs development. Gaitanidis et al. performed a retrospective study of PNET patients and found that the neutrophil-to-lymphocyte ratio and metastatic potential were independently prognostic, whereas platelet-to-lymphocyte ratio was indicative of disease progression and lymphocyte-to-monocyte ratio was indicative of tumor recurrence after surgical resection [41]. Individual cytokines such as interleukin-1 (IL-1), tumor necrosis factor alpha (TNF-α) and interleukin-6 have been implicated with chronic inflammation leading to a specific type of PNETs called gastroenteropancreatic neuroendocrine tumors (GEP-NETs) [42]. Clinically these GEP-NETs can be functional, and secrete various hormones, or non-functional and are differentiated by serum IL-2 levels, TNF-α or IL-6 [42]. Although there have been inflammatory changes found within PNET tumor populations, little is known about the immune landscape of the PNET tumor microenvironment. It has been largely observed that the immune landscape is highly heterogeneous with infiltration of various immune cells, such as neutrophils and mast cells [43].
2.2 The Gut Microbiome and Pancreatic Cancer
Inflammation can be modulated by disturbances in the gut microbiome. Recently, it was found that the pancreatic cancer microbiome causes signaling of both adaptive and innate immune system responses resulting in immune suppression and pancreatic cancer evasion [44]. An example of such microbes are Helicobacter pylori and Hepatitis B virus (HBV) [45]. H. pylori is a well-known bacterial carcinogen that perpetuates gastric cancer development and the evidence of its presence within pancreatic cancer patients is controversial and is largely linked to an indirect mechanism based on triggering inflammatory processes [45]. The bacterial microbes can induce inflammation through secretion of bacterial proteins such as lipopolysaccharide (LPS) chains that induce immune responses mainly through NF-kB activation [46]. The presence of LPS was found to induce severe pancreatitis, a precursor event to pancreatic cancer and modulate the CD4 + T-cells to secrete tumor necrosis factor alpha (TNF-a), interleukin 1 beta (IL-1β) and interleukin 8 (IL-8) [47].
Bacteria are not the only organisms within the gut microbiome but viruses comprise a large portion of the population and a recent study has found over 100,000 viruses, many of which have not been previously identified or studied [8]. Many correlative studies suggest that past exposure to HBV is linked to pancreatic cancer development due to the proximity between the pancreas and the liver [48]. The association of the same blood vessels and ducts allows HBV to travel between these two organs. A HBV infection marker, the Hepatitis B surface antigen, can be found within the pancreatic juice [49]. Although hepatitis mainly infects the liver, there is also a clear connection between the gut microbiome and HBV infection, which patients universally present with gastric mucosal lesions [50]. Currently, hepatitis infections are the only ones linked to pancreatic cancer development but because over 100,000 viruses exist within the microbiome, more work is needed to identify a link between the two. The mycobiome, which includes fungi and yeast, also contributes to pancreatic disease. The Candida genus is a diverse fungal component that makes up a large percentage of the mycobiome within the gut. A recent case report of a 56-year old immunocompromised male showed multiple pancreatic cysts that were thought to be malignant [45]. After further investigation, it was found that the cysts were the result of the fungal infection Candidiasis that mimicked pancreatic cancer [51]. Further evidence suggests that patients with Candida infection that are immunocompromised have increased rates of a variety of cancers, including pancreatic cancer [52].
2.3 The Oral Microbiome and Pancreatic Cancer Development
The oral microbiome resides in the oral cavity and consists of a variety of bacteria that is significantly altered in pancreatic cancer patients. Wei et al. reported an increase in Streptococcus spp. and Leptrotrichinia spp., bacteria in pancreatic cancer patients in a retrospective analysis, which may distinguish between the saliva of healthy individuals and those with pancreatic cancer [53]. These species were found to be present in the saliva of pancreatic cancer patients located in Asia. A retrospective study taken from patients within the USA suggested that the presence of Porphyromonas gingivitis and Aggregatibacter actinomycetemcomitans resulted in higher rates of pancreatic cancer development, whereas when specifically assessed in the African American population showed no significant differences in the oral microbiomes of healthy patients and those with pancreatic cancer. Regardless of this lack of difference, it was found that African American women were at higher risk of developing pancreatic cancer due to the socioeconomic disadvantages found within many African American communities [54,55,56].
Oral diseases, such as periodontal disease, were found to be significantly associated with pancreatic cancer (PDAC) development in an older population > 65 years old and were independent of other conditions such as diabetes or pancreatitis [57]. Periodontal disease occurs when there is rapid decay of the periodontal tissues leading to abscesses, infection and tooth loss. Many bacteria that are associated with periodontal disease are gram-negative anaerobic bacteria such as P. gingivitis and T. denticola [58]. The mechanism by which the oral and gut bacteria travels to the pancreas is still under investigation, but it is known that oral ingestion leads to a direct entry to the pancreas through portal circulation of the lower gastrointestinal tract [59].
2.4 The Skin Microbiome and Pancreatic Cancer
Although it seems unlikely that the skin microbiome could contribute to pancreatic cancer development, there is sufficient indirect evidence connecting the two. The skin commonly has a large population of gram-positive bacteria, but recent 16S sequencing has revealed that there is a smaller population of gram-negative bacteria present specifically proteobacteria [60]. Proteobacteria were found to be present more so in patients with PDAC tumors than healthy individuals [61]. Aykut et al. have found that PDAC tumors were enriched for Malassezia species and there was a significant loss of others such as the Candida and Saccharomyces species. The Malassezia species, a unicellular fungus, were found to contribute to oncogenic progression through binding of the mannose-binding lectin (MBL) and activate a complement cascade to evade immune processes and is over 3000 times higher in pancreatic cancer tissues than normal pancreatic tissues [62]. This species of fungi is commonly found within the skin microbiome, mainly the scalp, and contributes to dandruff and seborrheic dermatitis [63]. Proteus spp. was also found to be highly upregulated in pancreatic cancer tumors [59]. Proteus species were found to be present in ~ 90% of skin and urinary tract infections, has high virulence potential and linked to obesity [64, 65].
2.5 The Lung Microbiome and Pancreatic Cancer
As with the skin microbiome, there have been no studies identifying a direct link between the lung microbiome and pancreatic cancer development, but many of the processes that occur within the lung microbiome were found to contribute to pancreatic cancer development. For example, interleukin-17 (IL-17) signaling activation was found to occur in patients with asthma and sarcoidosis and related to pathogenic bacteria colonization within the lungs [31, 66]. Over-expression of IL-17 was found to promote the progression of acinar–ductal metaplasia (ADM) and intraepithelial pancreatic neoplasia (PanIN) as well as PDAC due to enhanced states of inflammation and activation of ERK 1/2, fibrogenesis genes and the generation of reactive nitric oxide (NO) and oxidative species [66]. Not only do perturbations within the lung microbiome impact disease development but also the state of which the lungs operate due to trauma or microbial perturbations can contribute to pancreatic cancer development. Various lung diseases caused by bacterial or viral colonization, such as bronchitis, COVID-19 and/or pneumonia, can cause hypoxic or hypoxemia conditions. Pancreatic cancer development is commonly driven by hypoxic conditions, where the low vasculature creates hypoxic tumor microenvironment that prevents appropriate drug penetration, leading to reduced response rates and poor overall survival. Specifically, the HIF-1α hypoxia genes have been shown to regulate pancreatic tumorigenesis [67].
3 Gut Microbiome Dysbiosis and its Impact on the Efficacy of Cancer Therapeutics
Although microbiome disturbances have been connected to a variety of systemic diseases, such as ulcerative colitis and IBD, the focus of this article is to understand the disturbances in the human microbiome and its relation to pancreatic cancer pathogenesis. Normally the pancreas is an immune cold site that does not have immune infiltration unless there is an acute case of pancreatitis or autoimmune pancreatitis. In the case of pancreatic cancer, this is a unique condition where disturbances within the human microbiome can trigger immune processes, such as inflammation, and lead to disease development. Below we will detail evidence that correlates these two adverse events and how the presence of an imbalanced gut microbiome can alter treatment efficacy of commonly used clinical therapeutics.
3.1 The Gut Microbiome: Metabolic Dysfunction
The imbalance in gut microbiome can alter normal metabolic processes that have been linked to cancer development. This can occur with a rapid proliferation of the genera Bacteroidetes over Firmicutes [68]. Bacteroidetes genera consist of large and diverse gram-negative bacterial species that normally assists in breaking down complex carbohydrates whereas Firmicutes are gram-positive bacteria and assist in energy resorption [69, 70]. The ratio of Firmicutes to Bacteroidetes (12 to 260) is considered a factor that helps reduce obesity and Type 2 diabetes and a change to this ratio can lead to physiologic consequences [68, 71].
The impact of harmful gut microbes or microbiome perturbations include a thickening of the mucus layer secreted by these microorganisms, secretion of bacterial metabolites that dampen host defenses to perpetuate and the transformation of bacterial metabolites [72]. Harmful metabolites include the secretion of bile acids, complex amino acids, trimethylamine N-oxide and indole derivatives leading to metabolic disorders, such as Type 2 diabetes [72]. Type 2 diabetes is a common metabolic disease that is sometimes followed by a pancreatic cancer diagnosis. Statistics show that around 80% of new onset pancreatic cancer patients have had metabolic dysfunction, either hyperglycemic or diabetes, at diagnosis and newly onset diabetes is associated higher with pancreatic cancer risks and this risk decreases during disease progression [73]. A recent Italian case–control study has showed that there was a relationship between metabolic syndrome and pancreatic cancer development [74]. Metabolic syndrome is defined as the presence of three metabolic conditions including diabetes, hypertension, hyperlipidemia and/or obesity. This study showed a positive correlation between metabolic syndrome and pancreatic cancer risk (RR 1.55) [74].
The secretion of metabolites from the gut microbiome has been shown to increase the risk for pancreatic cancer development. Huang et al. found TMAO, a choline metabolite, secreted from the gut microbiome had a positive association to pancreatic cancer development, whereas other groups have found in response to deoxycholate (DCA) chenodeoxycholate (CDCA) the body produces inflammatory signals such as cyclooxygenase, COX2 and prostaglandin E2 (PGE2) [75,76,77,78].
Gut bacteria can also mediate resistance to commonly used chemotherapies. For example, perturbations in the gut with upregulation of pathogenic bacteria, such as Escherichia/ Shigella and Enterobacter, have been shown to affect the efficacy of antimetabolite compounds like 5-fluorouracil (5-FU) [79]. Sensitivity to gemcitabine, an antimetabolite chemotherapeutic agent used in pancreatic cancer, can be altered by the presence of intra tumoral bacteria such as the Gammaproteobacteria class Klebsiella pneumoniae [80]. Using a mice model, Panebianco et al. have suggested that gemcitabine treatment decreased the Firmicutes and Bacteroidetes compositions while increasing the Proteobacteria and Verrucomicrobia phyla leading to an increase in inflammation producing bacteria and a decrease in purine metabolites such as xanthine [81]. The Bifidobacterium and Lactobacillus microbes have shown anti-cancer properties by their ability to induce apoptosis and inhibit cell cycle leading to cancer cell death and anti-metabolite chemotherapies, such as methotrexate, were found to reduce the composition of Bifidobacterium and Lactobacillus after treatment [82, 83].
It is clear that metabolic dysfunction caused by perturbations in the gut microbiome lead to inflammatory processes that contribute to pancreatic cancer development. Further investigation is needed to identify interventions to use the gut microbiome as a tool to treat this disease.
3.2 The Gut Microbiome: Immunotherapy Blockade
Results from clinical trials have made it clear that immunotherapies such as Programmed Death Ligand 1 (PD-L1) and Programmed Cell Death Protein 1 (PD-1) inhibitors do little to mitigate pancreatic cancer disease [84]. This is in part due to a low tumor mutational rate in pancreatic cancer as well as low PD-L1 expression and immunosuppressive properties [84]. Clinical trials for pancreatic cancer and immunotherapies have shown little success including the Phase II randomized clinical trial with PD-L1 and CTLA-4 inhibitors that showed a response rate of 3.1% with combination PD-L1 and cytotoxic T-lymphocyte associated protein (CTLA-4) inhibitors but a 0% response rate with either monotherapy [85, 86]. An alternative explanation for pancreatic cancer immune evasion may be due to perturbations within the microbiome.
H. pylori infection and its influence on pancreatic cancer development remains controversial. At the same time, studies have linked H. pylori infection to suppressed efficacy of immune checkpoint blockade in several cancers [87]. Oster et al. found that non-small cell lung cancer (NSCLC) patients infected with H. pylori were found to have reduced sensitivity rates to PD-1 immunotherapy (9.3 month overall survival compared to 21.7 month overall survival) [88]. Recently, H. pylori has been shown to be positively and significantly associated with PDAC development in those with a family history of pancreatic cancer and may be a reason why immunotherapy is somewhat ineffective [89]. Studies showed enrichment of pancreatic cyst fluid in Bactericides and Escherichia/Shigella spp [90]. The Bacteroidetes genus has both stimulating and repressive effects on CTLA-4 immunotherapy depending on the type of bacteria. For example, Bacteroidales fragils and Bacteroidales thetaiotaomicron were found to enhance CTLA-4 immunotherapy in both patients and mice, whereas most of the other microbes belonging to the Bacteroides spp. are associated with worse tumor prognoses in melanoma patients treated with the CTLA-4 immunotherapy ipilimumab [91]. Further, a subgroup of Escherichia coli bacteria that produces colibactin has been shown to have precancerous properties and interferes with PD-1 immunotherapy in colorectal cancer through impairing the T-cell response [92]. Various bacteria are associated with enhanced responses to immune checkpoint therapy in other disease models. For example, a B16 melanoma model treated with PDL-1 immunotherapy showed enhanced responses in the presence of Bifidobacterium, whereas in a RET melanoma and LLC lung carcinoma models Akkermansia muchinphilia and Alistipes were shown to enhance responses to PD-1 immunotherapy [93,94,95]
Viruses can also modulate immunotherapy responses and disease outcomes. Patients who have undergone PD-1 targeted immunotherapy were shown to have a significant increase in developing a hepatitis flare-up if they have been previously infected with the HBV virus [96]. Although some viruses have been shown to dampen the immunotherapy response many are trying to utilize viruses to treat cancer, some of which can be found within the gut microbiome. Oncolytic viruses are genetically engineered viruses (herpes simplex, adenoviruses, poliovirus and measles) which cannot replicate in normal cells but preferentially infect and kill tumor cells and are under investigation in melanoma, pancreatic cancer and colorectal cancer [97]. The most prominent example of a successful oncolytic virus is the Talimogene laherparepvec (T-VEC) which is a herpes simplex virus-1 derived immunotherapy used to treat patients with advanced melanoma (23.3 month overall survival) that was FDA approved in 2015 [98]. In pancreatic cancer, the modified adenovirus ONYX-015 is an oncolytic virus found to be beneficial in a Phase I trial where four patients had partial or minor disease regressions and six had stable disease after 8 weeks of treatment in combination with gemcitabine [99].
The mycobiome of the gut and organs is also being investigated whether it can influence responses to immunotherapy. Studies have shown that PD-1 and CTLA-4 immunotherapy can improve survival in patients with fungal sepsis while other studies have reported that PD-1 immunotherapy has been linked to clear specific types of protective fungi lung infections in mice models [100, 101]. Pancreatic cancer patients undergoing chemotherapy or radiation treatment are highly susceptible to fungal infections due to their immunocompromised states and a clearer understanding of how immunotherapy alters the mycobiome is needed.
3.3 The Gut Microbiome and Radiation
Dysbiosis of the gut microbiome also contributes to dampened efficacy with radiation in cancer patients. Radiation is frequently given to pancreatic cancer patients in a palliative setting but Phase I/II clinical trials are currently testing radiation in combination with immunotherapies [102]. Radiation currently gives somewhat of a benefit to pancreatic cancer patients as has been demonstrated by Krishnan et al., who suggests that radiation doses above 70 grays increases overall survival (17.8 months vs 15.0 months) [103]. Further re-irradiation of stereotactic body radiotherapy showed an increased overall survival rates, disease control rates and pain reduction [104]. Although there is some progress in understanding the impacts of radiation in pancreatic cancer, the correlation between response rates to radiation and the gut microbiome has not been explored in pancreatic cancer as it was studied in other cancers. Further investigation may improve response rates.
Gamma irradiation can produce significant changes to the gut microbiome including an increase in the Alistipes spp. (Bacteroidetes) and Corynebacterium (Actinobacteria) genera and decreases in the Prevotella genus (Bacteroidetes) [105]. The Alistipes species, particularly A. onderdonkii, is downregulated in pancreatic cancer and its upregulation was linked to the proliferation suppression of pancreatic cancer cells [105]. A comparison between pancreatic cancer patients and healthy patients revealed a suppression of the Corynebacterium genera while there was increased levels of the Prevotella genera which contributed to innate and adaptive immune suppression [106, 107]. These results suggest that radiation is not only influencing pancreatic cancer cell death through inducing DNA damage to the tumor but also influencing the composition of the gut microbiome. This topic requires further investigation to uncover ways to enhance radiation therapy by altering the microbiome with probiotics or other intervention strategies.
4 The Oral and Skin Microbiomes and the Efficacy of Cancer Therapeutics
There have been few studies assessing the impact of composition of the gut microbiome on cancer treatment efficacy but some have shown the oral and skin microbiome dominant organisms can alter the efficacy of anti-metabolites that are used to treat pancreatic cancer [108]. Some of the organisms found to be in abundance among the oral microbiome of pancreatic cancer patients includes Porphyromonas gingivitis and Aggregatibacter actinomycetemcomitans [108].
Porphyromonas gingivitis belongs to the Bacteroidetes genus, a gram negative and anaerobic pathogenic bacterium. This bacterium makes and secretes peptidyl-arginine deaminase (PAD), an enzyme that catalyzes the Arginine residues to proteins to citrulline, which can boost free radical production, such as nitric oxide, within the body that has damaging effects on the body in large amounts [109]. In gastric cancer, it was shown that upregulation of peptidyl-arginine deaminase 4 (PAD4) with the anti-metabolite 5-FU suppressed gastric cancer growth and was reversed by downregulation of PAD4 expression [110]. Further, it was found that depletion of arginine, a product of citrulline and aspartate, induced apoptotic cell death in leukemia models, whereas upregulation of L-citrulline rescued the effects of arginine deprivation in PDAC cells suggestive of the impact of this enzyme [111].
Aggregatibacter actinomycetemcomitans is a gram-negative anaerobe that metabolizes lactate into carbon dioxide, lactic and acetic acids ultimately to make the H2O2 free radical as a byproduct [112]. Pancreatic cancer is largely driven by glycolysis and produces lactic acid within the tumor microenvironment leading to an increased expression of angiogenesis genes such as HIF-1α [113]. Lactic acid also forms an acidic buffer within the tumor microenvironment that promotes invasion while the glycolysis intermediates help the tumor grow via Connexin-43 channels [114]. H2O2 is a two-edged sword that can drive pancreatic cancer growth while also being explored for its ability to treat this disease. Lei et al. have found that hydrogen peroxide mediates the invasive ability of pancreatic cancer by driving the MAPK/ERK growth pathway while also driving inflammatory processes within cancer cells through NF-kB upregulation and HIF-1α simultaneously also driving the tumor storm through inflammation and inducing DNA damage [115,116,117,118,119]. Antioxidants and free radicals, such as H2O2, were found to decrease the apoptotic effect of the compound 5-FU in colon cancer, whereas gemcitabine is known to elevate peroxiporins, or aquaporin channels that transport H2O2 across the membrane [120, 121].
Studies have shown that a colonization of fungi within the gut, specifically the Malassezia spp., contributes to the pathogenesis of pancreatic cancer in mice and humans through infection with the mannose-binding lectin protein (MBL) and infiltration of pancreatic tumors and targeting this fungus was shown to cause enhanced sensitivity to gemcitabine treatment [55]. More work is needed to identify the impact of perturbed microbiomes on the efficacy of therapeutics being used to treat pancreatic cancer.
5 Utilizing the Microbiome as a Preventative or Therapeutic for Pancreatic Cancer
5.1 Fecal Transplants
Fecal transplantation is a way to treat a perturbed microbiome by transplanting the stool from a healthy donor into a recipient donor [122]. For pancreatic cancer, there have been studies dedicated to exploring the therapeutic benefit of this treatment and a Phase I clinical trial is underway (NCT04975217). The overall rationale for using this type of treatment is due to the fact that (1) there is bacteria within the pancreatic tumor, such as Aggregatibacter actinomycetemcomitans, Porphyromonas gingivalis and Fusobacterium, (2) healthy individuals have been shown to have a different composition of bacterial species within their gastrointestinal microbiomes that seem to suppress these harmful bacteria and (3) suppression of these pancreatic cancer driving bacteria can lead to a reversal of cancer promoting phenotypes such as immune evasion, sensitization to immunotherapy while also down-regulating metastatic and invasive properties. Although fecal transplantation seems to be a promising strategy to treat pancreatic cancer, there is more work needed to truly identify the microbiome profile of a candidate healthy donor along with more characterization and discovery into rare bacteria that may be located within the donor’s microbiome. A recent report showed that a death was caused by a fecal transplant due to a drug resistant bacteria found within the sample [123]. Although the drug resistant bacteria did not cause harm to the donor, its transplantation into an immunocompromised individual was detrimental [123].
5.2 Probiotics
Probiotics are live bacteria and yeast, which can be found in fermented foods such as yogurt and cheese or in pill form. The live bacteria within probiotics are normally belonging to the Lactobacillus genus. Lactobacillus spp. are gram-positive anaerobes categorized as “good bacteria” which metabolizes carbohydrates and competes against more harmful bacteria within the gut. Chen et al. found that the probiotic Lactobacillus synergizes with gemcitabine in an in vivo pancreatic cancer model where Konishi et al. found that Aspergillus oryzae was found to have anti-tumor properties through altering MAPK/ERK signaling [124, 125]. Pancreatic cancer was also found to be inhibited by the ferrichrome compound, an iron molecule that can be found in probiotics, and was shown to be effective in 5-FU resistant cells [126]. Probiotics have a preventative effect against pancreatic cancer in addition to their ability to enhance pancreatic cancer cell death. Studies have shown that a diet rich in probiotics can reduce inflammation, which leads to pancreatitis and in some cases, can cause pancreatic cancer [127, 128].
5.3 Preventative Strategies
Forty-eight percent of the population is estimated to have periodontal disease and/or is living with risk factors leading to this condition like smoking, diabetes, age, stress and poor oral hygiene [129]. In addition to the correlation between the poor periodontal health and cardiovascular disease, also it seems to contribute to pancreatic cancer, as we have discussed above. In addition, socioeconomic disparities, such as limited access to dental health, the ability to obtain unhealthy food at cheaper costs than healthy food, increases in tobacco use and living in rural communities, make it difficult for a large percentage of the population to maintain good oral health. A better understanding and awareness of the risks of poor oral health and pancreatic cancer development in the healthcare field and the community will help address solutions to close the disparities gap within vulnerable communities.
Poor diet can lead to perturbed microbiomes within the body, which can in turn lead to pancreatic cancer development. Education and understanding healthy food choices over processed foods, fats and sugars may be a key to keeping the microbiome in check. Increasing the consumption of fermented foods, such as yogurt, high fiber and whole foods has been shown to reverse the pathogenic activity of bacteria within the gut microbiome [130, 131]. In the US, food insecurity, hunger and inability to access healthy food is a major issue. It is estimated that 10.5% of households have experienced food insecurity in 2020, according to the USDA, whereas the official poverty rate was 11.4% in 2020, which has increased since 2019 [132, 133]. These numbers indicate that access to healthy foods, oral care and health care is non-existent for a percentage of the population and may lead to dire health consequences in the future, such as pancreatic cancer. Although this topic is not within the scope of this manuscript, these issues need to be addressed at the local, state and federal levels and a comprehensive solution is needed to assist those in need.
Smoking is another factor that can alter the human microbiome and lead to growth of pathogenic bacteria in the gut, which can alter the intestinal pH [134]. Moreover, smoking was shown to enhance the intestinal pH through the effects of nicotine either directly or by exposing the microbiome to harmful additives in cigarettes such as polycyclic aromatic hydrocarbons, volatile organic compounds and aldehydes [134]. Smoking is directly linked to pancreatic cancer development and is associated with a twofold increased risk. It also negatively influences the human microbiome. Preventing the use of nicotine and tobacco products would be helpful in stopping some of the risk that tobacco use has on health while also protecting the microbiome from eliciting pathogenic effects on the body [135].
Finally, there are many studies that show conclusive evidence that taking supplements and vitamins is beneficial to maintaining a healthy microbiome. For example, it was found that taking B-vitamins supports positive gut microbiome health by suppressing pathogenic and competitive bacterial species while also supporting the symbiotic relationship between the host and the gut microbiome [136]. Taking vitamin D supplements has shown benefit to maintaining a healthy microbiome, specifically in older men [137]. Using a diversity analysis from 16S rRNA bacterial sequencing, it was found that increases in vitamin D, specifically with higher levels of 1, 25(OH) 2D levels, had increases in the Firmicutes phylum and specifically have more butyrate-producing bacteria [137]. Butyrate was shown to inhibit pancreatic cancer invasion and can sensitize pancreatic cancer cells to therapeutics such as histone deacetylases and gemcitabine [138,139,140].
6 Conclusions
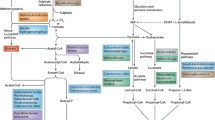
Pancreatic cancer is a highly aggressive and deadly disease. Some mechanisms of pathogenicity have been identified including the association with other health conditions, such as Type 2 diabetes and pancreatitis, but there is currently no clear understanding of how we can screen for this disease in its early stages to thwart disease progression and/or development. Evidence is emerging on the correlation between a disturbed human microbiome and pancreatic cancer development, specifically in relation to the Bacteroidetes/Firmicutes ratio. Although the gut is the most well-studied area of microbiome, there is evidence to support that other microbiomes (lung, skin, oral cavity) within the body contribute to pancreatic cancer development and can enhance or inhibit the effects of therapeutics used to treat cancer (Fig. 1). In recent years, there has also been a correlation between poor oral health and pancreatic cancer development due to the pathogenicity and invasiveness of specific oral microbes, such as P. gingivalis. Understanding the impacts of the gut microbiome is critical toward making advancements to pancreatic cancer research. Further, understanding ways to utilize this knowledge as a preventative is just as critical and a step toward reducing the risks associated with pancreatic cancer that can be found in everyday life.
Change history
10 May 2022
A Correction to this paper has been published: https://doi.org/10.1007/s10555-022-10037-3
References
Seer.cancer.gov. Cancer Stat Facts: Pancreatic Cancer. Surveillance, Epidemiology and End Results Program. Accessed 11/12/2021.
Stark, A., & Eibl, G. (2015). Pancreatic Ductal Adenocarcinoma. Pancreapedia: Exocrine Pancreas Knowledge Base. https://doi.org/10.3998/panc.2015.14
Alkassis, S., Yazdanpanah, O., & Philip, P. A. (2021). BRCA mutations in pancreatic cancer and progress in their targeting. Expert Opinion on Therapeutic Targets, 25(7), 547–557. https://doi.org/10.1080/14728222.2021.1957462
Ro, C., Chai, W., Yu, V. E., & Yu, R. (2013). Pancreatic neuroendocrine tumors: Biology, diagnosis, and treatment. Chinese Journal of Cancer, 32(6), 312–324. https://doi.org/10.5732/cjc.012.10295
Shulman, S. T., Friedmann, H. C., & Sims, R. H. (2007). Theodor Escherich: The first pediatric infectious diseases physician? Clinical Infectious Diseases, 45(8), 1025–1029. https://doi.org/10.1086/521946
McFarland, L. V. (2015). From Yaks to Yogurt: The History, Development and Current Use of Probiotics. Clinical Infectious Disease., 60(2), S85–S90. https://doi.org/10.1093/cid.civ054
Cani, P. D. (2018). Human gut microbiome: Hopes, threats and promises. Gut, 67, 1716–1725. https://doi.org/10.1136/gutjnl-2018-316723
Nayfach, S., Páez-Espino, D., Call, L., et al. (2021). Metagenomic compendium of 189,680 DNA viruses from the human gut microbiome. Nature Microbiology, 6, 960–970. https://doi.org/10.1038/s41564-021-00928-6
Deo, P. N., & Deshmukh, R. (2019). Oral microbiome: Unveiling the fundamentals. Journal of oral and maxillofacial pathology: JOMFP, 23(1), 122–128. https://doi.org/10.4103/jomfp.JOMFP_304_18
Cresci, G. A., & Bawden, E. (2015). Gut Microbiome: What We Do and Don’t Know. Nutrition in Clinical Practice, 30(6), 734–746. https://doi.org/10.1177/0884533615609899
Komiyama, K., Tynan, J. J., Habbick, B. F., Duncan, D. E., & Liepert, D. J. (1985). Pseudomonas aeruginosa in the oral cavity and sputum of patients with cystic fibrosis. Oral Surgery, Oral Medicine, and Oral Pathology, 59(6), 590–594. https://doi.org/10.1016/0030-4220(85)90187-2
DeGruttola, A. K., Low, D., Mizoguchi, A., & Mizoguchi, E. (2016). Current Understanding of Dysbiosis in Disease in Human and Animal Models. Inflammatory Bowel Diseases, 22(5), 1137–1150. https://doi.org/10.1097/MIB.0000000000000750
Slots, J., & Rams, T. E. (1991). New views on periodontal microbiota in special patient categories. Journal of Clinical Periodontology, 18(6), 411–420. https://doi.org/10.1111/j.1600-051x.1991.tb02309.x
Benjamin R. M. (2010). Oral health: the silent epidemic. Public health reports (Washington, D.C.: 1974), 125(2), 158–159. https://doi.org/10.1177/003335491012500202
Leishman, S. J., Do, H. L., & Ford, P. J. (2010). Cardiovascular disease and the role of oral bacteria. Journal of oral microbiology, 2. https://doi.org/10.3402/jom.v2i0.5781.10.3402/jom.v2i0.5781
Tong, Y., Zheng, L., Qing, P., Zhao, H., Li, Y., Su, L., Zhang, Q., Zhao, Y., Luo, Y., & Liu, Y. (2020). Oral Microbiota Perturbations are Linked to High Risk for Rheumatoid Arthritis. Frontiers in Cellular and Infection Microbiology. https://doi.org/10.3389/fcimb.2019.00475
Meurman J. H. (2010). Oral microbiota and cancer. Journal of oral microbiology, 2. https://doi.org/10.3402/jom.v2i0.5195.10.3402/jom.v2i0.5195
Northridge, M. E., Kumar, A., & Kaur, R. (2020). Disparities in Access to Oral Health Care. Annual review of public health, 41, 513–535. https://doi.org/10.1146/annurev-publhealth-040119-094318
Winkler, J. R., & Robertson, P. B. (1992). Periodontal disease associated with HIV infection. Oral Surgery, Oral Medicine, and Oral Pathology, 73(2), 145–150. https://doi.org/10.1016/0030-4220(92)90186-t
Koonin, E. V., Mushegian, A. R., & Rudd, K. E. (1996). Sequencing and analysis of bacterial genomes. Current Biology., 6(4), 404–416. https://doi.org/10.1016/S0960-9822(02)00508-0
Clarridge J. E., 3rd (2004). Impact of 16S rRNA gene sequence analysis for identification of bacteria on clinical microbiology and infectious diseases. Clinical microbiology reviews, 17(4), 840–862. https://doi.org/10.1128/CMR.17.4.840-862.2004
Grice, E. A., Kong, H. H., Conlan, S., Deming, C. B., Davis, J., Young, A. C., NISC Comparative Sequencing Program, Bouffard, G. G., Blakesley, R. W., Murray, P. R., Green, E. D., Turner, M. L., & Segre, J. A. (2009). Topographical and temporal diversity of the human skin microbiome. Science (New York, N.Y.), 324(5931), 1190–1192. https://doi.org/10.1126/science.1171700
Luna, P. C. (2020). Skin Microbiome as Years Go By. American journal of clinical dermatology, 21(Suppl 1), 12–17. https://doi.org/10.1007/s40257-020-00549-5
Boxberger, M., Cenizo, V., Cassir, N., et al. (2021). Challenges in exploring and manipulating the human skin microbiome. Microbiome, 9, 125. https://doi.org/10.1186/s40168-021-01062-5
Grice, E. A., Kong, H. H., Conlan, S., Deming, C. B., Davis, J., Young, A. C., et al. (2009). Topographical and temporal diversity of the human skin microbiome. Science, 324, 1190–1192.
Nørreslet, L. B., Agner, T., & Clausen, M. L. (2020). The Skin Microbiome in Inflammatory Skin Diseases. Current Dermatology Reports, 9, 141–151. https://doi.org/10.1007/s13671-020-00297-z
Busse, K., & Liao, W. (2010). Which Psoriasis Patients Develop Psoriatic Arthritis? Psoriasis forum, 16(4), 17–25.
Chiu, H. Y., Hsieh, C. F., Chiang, Y. T., Huang, W. F., & Tsai, T. F. (2016). The Risk of Chronic Pancreatitis in Patients with Psoriasis: A Population-Based Cohort Study. PLoS ONE, 11(7), e0160041. https://doi.org/10.1371/journal.pone.0160041
Pfister, H., & zur Hausen, H. (1978). Seroepidemiological studies of human papilloma virus (HPV-1) infections. International Journal of Cancer, 21(2), 161–5. https://doi.org/10.1002/ijc.2910210206
Tong, T. R., Chan, A., Lai, T. W., Chan, O. W., Lee, K. C., Lo, S. T., Lung, R., Li, J. Y., & Chow, T. C. (2007). Identification of HPV-16 in Borderline Mucinous Cystic Neoplasm of Pancreas. International journal of biomedical science : IJBS, 3(1), 72–75.
Liu, N. N., Ma, Q., Ge, Y., Yi, C. X., Wei, L. Q., Tan, J. C., Chu, Q., Li, J. Q., Zhang, P., & Wang, H. (2020). Microbiome dysbiosis in lung cancer: From composition to therapy. NPJ precision oncology, 4(1), 33. https://doi.org/10.1038/s41698-020-00138-z
Wang, H., Liu, J. S., Peng, S. H., Deng, X. Y., Zhu, D. M., Javidiparsijani, S., Wang, G. R., Li, D. Q., Li, L. X., Wang, Y. C., & Luo, J. M. (2013). Gut-lung crosstalk in pulmonary involvement with inflammatory bowel diseases. World Journal of Gastroenterology, 19(40), 6794–6804. https://doi.org/10.3748/wjg.v19.i40.6794
Bowerman, K. L., Rehman, S. F., Vaughan, A., et al. (2020). Disease-associated gut microbiome and metabolome changes in patients with chronic obstructive pulmonary disease. Nature Communications, 11, 5886. https://doi.org/10.1038/s41467-020-19701-0
Witt, H., Apte, M. V., Keim, V., & Wilson, J. S. (2007). Chronic pancreatitis: Challenges and advances in pathogenesis, genetics, diagnosis, and therapy. Gastroenterology, 132(4), 1557–1573. https://doi.org/10.1053/j.gastro.2007.03.001
Omary, M. B., Lugea, A., Lowe, A. W., & Pandol, S. J. (2007). The pancreatic stellate cell: A star on the rise in pancreatic diseases. The Journal of Clinical Investigation, 117(1), 50–59. https://doi.org/10.1172/JCI30082
Ohlund, D., Handly-Santana, A., Biffi, G., Elyada, E., Almeida, A. S., Ponz-Sarvise, M., Corbo, V., Oni, T. E., Hearn, S. A., Lee, E. J., et al. (2017). Distinct populations of inflammatory fibroblasts and myofibroblasts in pancreatic cancer. Journal of Experimental Medicine., 214(3), 579–596.
Domen, A., Quatannens, D., Zanivan, S., Deben, C., Van Audenaerde, J., Smits, E., Wouters, A., Lardon, F., Roeyen, G., Verhoeven, Y., Janssens, A., Vandamme, T., van Dam, P., Peeters, M., & Prenen, H. (2021). Cancer-Associated Fibroblasts as a Common Orchestrator of Therapy Resistance in Lung and Pancreatic Cancer. Cancers, 13(5), 987. https://doi.org/10.3390/cancers13050987
Swidnicka-Siergiejko, A., Gomez-Chou, S., Cruz-Monserrate, Z., et al. (2017). Chronic inflammation initiates multiple forms of K-Ras-independent mouse pancreatic cancer in the absence of TP53. Oncogene, 36, 3149–3158. https://doi.org/10.1038/onc.2016.461
Tjomsland, V., Bojmar, L., Sandstrom, P., Brathail, C., Messmer, D., Spangeus, A., & Larsson, M. (2013). IL-1a Expression in Pancreatic Ductal Adenocarcinoma Affects the Tumor Cell Migration and Is Regulated by the p38MAPK Signaling Pathway. PLoS ONE. https://doi.org/10.1371/journal.pone.0070874
Steele, N. G., Biffi, G., Kemp, S. B., Zhang, Y., Drouillard, D., Syu, L., Hao, Y., Oni, T. E., Brosnan, E., Elyada, E., Doshi, A., Hansma, C., Espinoza, C., Abbas, A., The, S., Irizarry-Negron, V., Halbrook, C. J., Franks, N. E., Hoffman, M. T., … Pasca di Magliano, M. (2021). Inhibition of Hedgehog Signaling Alters Fibroblast Composition in Pancreatic Cancer. Clinical Cancer Research, 27(7), 2023–2037. https://doi.org/10.1158/1078-0432.CCR-20-3715
Gaitanidis, A., Patel, D., Nilubol, N., Tirosh, A., Sadowski, S., & Kebebew, E. (2018). Markers of Systemic Inflammatory Response are Prognostic Factors in Patients with Pancreatic Neuroendocrine Tumors (PNETs): A Prospective Analysis. Annals of Surgical Oncology, 25(1), 122–130. https://doi.org/10.1245/s10434-017-6241-4
Cigrovski Bervkovic, M., Cacev, T., Catela Ivkovic, T., Zjacic-Rotkvic, V., & Kapitanovic, S. (2014). New Insights into the Role of Chronic Inflammation and Cytokines in the Etiopathogenesis of Gastroenteropancreatic Neuroendocrine Tumors. Neuroendocrinology, 99, 75–84. https://doi.org/10.1159/0003624339
Cives, M., Pelle’, E., Quaresmini, D., Rizzo, F. M., Tucci, M., & Silvestris, F. (2019). The Tumor Microenvironment in Neuroendocrine Tumors: Biology and Therapeutic Implications. Neuroendocrinology, 109(2), 83–99. https://doi.org/10.1159/000497355
Zambirinis, C. P., Pushalkar, S., Saxena, D., & Miller, G. (2014). Pancreatic cancer, inflammation, and microbiome. Cancer Journal (Sudbury, Mass.), 20(3), 195–202. https://doi.org/10.1097/PPO.0000000000000045
Bulajic, M., Panic, N., & Löhr, J. M. (2014). Helicobacter pylori and pancreatic diseases. World Journal of Gastrointestinal Pathophysiology, 5(4), 380–383. https://doi.org/10.4291/wjgp.v5.i4.380
Ikebe, M., Kitaura, Y., Nakamura, M., Tanaka, H., Yamasaki, A., Nagai, S., Wada, J., Yanai, K., Koga, K., Sato, N., Kubo, M., Tanaka, M., Onishi, H., & Katano, M. (2009). Lipopolysaccharide (LPS) increases the invasive ability of pancreatic cancer cells through the TLR4/MyD88 signaling pathway. Journal of Surgical Oncology, 100(8), 725–731. https://doi.org/10.1002/jso.21392
Vaccaro, M. I., Calvo, E. L., Suburo, A. M., Sordelli, D. O., Lanosa, G., & Iovanna, J. L. (2000). Lipopolysaccharide directly affects pancreatic acinar cells: Implications on acute pancreatitis pathophysiology. Digestive Diseases and Sciences, 45(5), 915–926. https://doi.org/10.1023/a:1005521007609
Hoefs, J. C., Renner, I. G., Askhcavai, M., & Redeker, A. G. (1980). Hepatitis B surface antigen in pancreatic and biliary secretions. Gastroenterology, 79(2), 191–194.
Hassan, M. M., Li, D., El-Deeb, A. S., Wolff, R. A., Bondy, M. L., Davila, M., & Abbruzzese, J. L. (2008). Association between hepatitis B virus and pancreatic cancer. Journal of clinical oncology : Official journal of the American Society of Clinical Oncology, 26(28), 4557–4562. https://doi.org/10.1200/JCO.2008.17.3526
Xia JY, Zhou YY, Zhao YY. (2005) [Relationship between hepatitis B virus in gastric mucosa and syndrome of disharmony between liver and stomach in patients with chronic hepatitis B]. Zhong Xi Yi Jie He Xue Bao. 3(1):19–22. Chinese. https://doi.org/10.3736/jcim20050107.
Seong, M., Kang, T. W., & Ha, S. Y. (2015). Pancreatic Candidiasis That Mimics a Malignant Pancreatic Cystic Tumor on Magnetic Resonance Imaging: A Case Report in an Immunocompetent Patient. Korean Journal of Radiology, 16(6), 1253–1256. https://doi.org/10.3348/kjr.2015.16.6.1253
Chung, L., Liang, J., Lin, C., Sun, L., & Kao, C. (2017). Cancer risk in patients with candidiasis: A nationwide population-based cohort study. Oncotarget, 8, 63562–63573. https://doi.org/10.18632/oncotarget.18855
Wei, A. L., Li, M., Li, G. Q., Wang, X., Hu, W. M., Li, Z. L., Yuan, J., Liu, H. Y., Zhou, L. L., Li, K., Li, A., & Fu, M. R. (2020). Oral microbiome and pancreatic cancer. World Journal of Gastroenterology, 26(48), 7679–7692. https://doi.org/10.3748/wjg.v26.i48.7679
Petrick, J. L., Wilkinson, J. E., Michaud, D. S., et al. (2021). The oral microbiome in relation to pancreatic cancer risk in African Americans. British Journal of Cancer. https://doi.org/10.1038/s41416-021-01578-5
Fan, X., Alekseyenko, A. V., Wu, J., Peters, B. A., Jacobs, E. J., Gapstur, S. M., Purdue, M. P., Abnet, C. C., Stolzenberg-Solomon, R., Miller, G., Ravel, J., Hayes, R. B., & Ahn, J. (2018). Human oral microbiome and prospective risk for pancreatic cancer: A population-based nested case-control study. Gut, 67(1), 120–127. https://doi.org/10.1136/gutjnl-2016-312580
Gerlovin, H., Michaud, D. S., Cozier, Y. C., & Palmer, J. R. (2019). Oral Health in Relation to Pancreatic Cancer Risk in African American Women. Cancer Epidemiology, Biomarkers & Prevention, 28(4), 675–679. https://doi.org/10.1158/1055-9965.EPI-18-1053
Michaud, D. S., & Izard, J. (2014). Microbiota, oral microbiome, and pancreatic cancer. Cancer journal (Sudbury, Mass.), 20(3), 203–206. https://doi.org/10.1097/PPO.0000000000000046
Lovegrove, J. M. (2004). Dental plaque revisited: Bacteria associated with periodontal disease. Journal of the New Zealand Society of Periodontology, 87, 7–21.
Zhang, W., Zhang, K., Zhang, P., Zheng, J., Min, C., & Li, X. (2021). Research Progress of Pancreas-Related Microorganisms and Pancreatic Cancer. Frontiers in oncology, 10, 604531. https://doi.org/10.3389/fonc.2020.604531
Grice, E. A., & Segre, J. A. (2011). The skin microbiome. Nature reviews. Microbiology, 9(4), 244–253. https://doi.org/10.1038/nrmicro2537
Bellotti, R., Speth, C., Adolph, T. E., Lass-Flörl, C., Effenberger, M., Öfner, D., & Maglione, M. (2021). Micro- and Mycobiota Dysbiosis in Pancreatic Ductal Adenocarcinoma Development. Cancers, 13(14), 3431. https://doi.org/10.3390/cancers13143431
Aykut, B., Pushalkar, S., Chen, R., Li, Q., Abengozar, R., Kim, J. I., Shadaloey, S. A., Wu, D., Preiss, P., Verma, N., Guo, Y., Saxena, A., Vardhan, M., Diskin, B., Wang, W., Leinwand, J., Kurz, E., Kochen Rossi, J. A., Hundeyin, M., … Miller, G. (2019). The fungal mycobiome promotes pancreatic oncogenesis via activation of MBL. Nature, 574(7777), 264–267. https://doi.org/10.1038/s41586-019-1608-2
Rudramurthy, S. M., Honnavar, P., Dogra, S., Yegneswaran, P. P., Handa, S., & Chakrabarti, A. (2014). Association of Malassezia species with dandruff. The Indian journal of medical research, 139(3), 431–437.
Schaffer, J. N., & Pearson, M. M. (2015). Proteus mirabilis and Urinary Tract Infections. Microbiology spectrum, 3(5), https://doi.org/10.1128/microbiolspec.UTI-0017-2013. https://doi.org/10.1128/microbiolspec.UTI-0017-2013
Löwik CAM, Zijlstra WP, Knobben BAS, Ploegmakers JJW, Dijkstra B, de Vries AJ, Kampinga GA, Mithoe G, Al Moujahid A, Jutte PC, Wouthuyzen-Bakker M; Northern Infection Network Joint Arthroplasty (NINJA). (2019) Obese patients have higher rates of polymicrobial and Gram-negative early periprosthetic joint infections of the hip than non-obese patients. PLoS One. 14(4):e0215035. https://doi.org/10.1371/journal.pone.0215035.
Hu, F., Guo, F., Zhu, Y., Zhou, Q., Li, T., Xiang, H., & Shang, D. (2020). IL-17 in pancreatic disease: Pathogenesis and pharmacotherapy. American Journal of Cancer Research, 10(11), 3551–3564.
Jin, X., Dai, L., Ma, Y., et al. (2020). Implications of HIF-1α in the tumorigenesis and progression of pancreatic cancer. Cancer Cell International, 20, 273. https://doi.org/10.1186/s12935-020-01370-0
Magne, F., Gotteland, M., Gauthier, L., Zazueta, A., Pesoa, S., Navarrete, P., & Balamurugan, R. (2020). The Firmicutes/Bacteroidetes Ratio: A Relevant Marker of Gut Dysbiosis in Obese Patients? Nutrients, 12(5), 1474. https://doi.org/10.3390/nu12051474
Wexler, H. M. (2007). Bacteroides: The good, the bad, and the nitty-gritty. Clinical Microbiology Reviews, 20(4), 593–621. https://doi.org/10.1128/CMR.00008-07
Ottman, N., Smidt, H., de Vos, W. M., & Belzer, C. (2012). The function of our microbiota: Who is out there and what do they do? Frontiers in Cellular and Infection Microbiology, 2, 104. https://doi.org/10.3389/fcimb.2012.00104
Larsen, N., Vogensen, F. K., van den Berg, F. W., Nielsen, D. S., Andreasen, A. S., Pedersen, B. K., Al-Soud, W. A., Sørensen, S. J., Hansen, L. H., & Jakobsen, M. (2010). Gut microbiota in human adults with type 2 diabetes differs from non-diabetic adults. PLoS ONE, 5(2), e9085. https://doi.org/10.1371/journal.pone.0009085
Agus, A; Clement, K; Sokol, H. (2020) Gut microbiota-derives metabolites as central regulators in metabolic disorders. Recent Advances in Basic Science. 70(6). https://doi.org/10.1136/gutjnl-2020-323071
Pannala, R., Basu, A., Petersen, G. M., & Chari, S. T. (2009). New-onset diabetes: A potential clue to the early diagnosis of pancreatic cancer. The Lancet. Oncology, 10(1), 88–95. https://doi.org/10.1016/S1470-2045(08)70337-1
Rosato, V., Tavani, A., Bosetti, C., Pelucchi, C., Talamini, R., Polesel, J., Serraino, D., Negri, E., & La Vecchia, C. (2011). Metabolic syndrome and pancreatic cancer risk: A case-control study in Italy and meta-analysis. Metabolism, 60(10), 1372–1378. https://doi.org/10.1016/j.metabol.2011.03.005
Huang, J. Y., Luu, H. N., Butler, L. M., Midttun, Ø., Ulvik, A., Wang, R., Jin, A., Gao, Y. T., Tan, Y., Ueland, P. M., Koh, W. P., & Yuan, J. M. (2020). A prospective evaluation of serum methionine-related metabolites in relation to pancreatic cancer risk in two prospective cohort studies. International Journal of Cancer, 147(7), 1917–1927. https://doi.org/10.1002/ijc.32994
Feng, H. Y., & Chen, Y. C. (2016). Role of bile acids in carcinogenesis of pancreatic cancer: An old topic with new perspective. World journal of gastroenterology, 22(33), 7463–7477. https://doi.org/10.3748/wjg.v22.i33.7463
Tucker, O. N., Dannenberg, A. J., Yang, E. K., & Fahey, T. J. (2004). 3rd Bile acids induce cyclooxygenase-2 expression in human pancreatic cancer cell lines. Carcinogenesis, 25, 419–423.
Phelan, J. P., Reen, F. J., Caparros-Martin, J. A., O’Connor, R., & O’Gara, F. (2017). Rethinking the bile acid/gut microbiome axis in cancer. Oncotarget, 8(70), 115736–115747. https://doi.org/10.18632/oncotarget.22803
Yuan, L., Zhang, S., Li, H., Yang, F., Mushtaq, N., Ullah, S., Shi, Y., An, C., & Xu, J. (2018). The influence of gut microbiota dysbiosis to the efficacy of 5-Fluorouracil treatment on colorectal cancer. Biomedicine & Pharmacotherapy, 108, 184–193. https://doi.org/10.1016/j.biopha.2018.08.165
Thomas, H. (2017). Intra-tumour bacteria promote gemcitabine resistance in pancreatic adenocarcinoma. Nature Reviews. Gastroenterology & Hepatology, 14, 632. https://doi.org/10.1038/nrgastro.2017.142
Panebianco, C., Adamberg, K., Jaagura, M., Copetti, M., Fontana, A., Adamberg, S., Kolk, K., Vilu, R., Andriulli, A., & Pazienza, V. (2018). Influence of gemcitabine chemotherapy on the microbiota of pancreatic cancer xenografted mice. Cancer Chemotherapy and Pharmacology, 81(4), 773–782. https://doi.org/10.1007/s00280-018-3549-0
Badgeley, A., Anwar, H., Modi, K., Murphy, P., & Lakshmikuttyamma, A. (2021). Effect of probiotics and gut microbiota on anti-cancer drugs: Mechanistic perspectives. Biochimica et Biophysica Acta - Reviews on Cancer, 1875(1), 188494. https://doi.org/10.1016/j.bbcan.2020.188494
Huang, Y., Yang, W., Liu, H., Duan, J., Zhang, Y., Liu, M., Li, H., Hou, Z., & Wu, K. K. (2012). Effect of high-dose methotrexate chemotherapy on intestinal Bifidobacteria, Lactobacillus and Escherichia coli in children with acute lymphoblastic leukemia. Experimental Biology and Medicine (Maywood, N.J.), 237(3), 305–311. https://doi.org/10.1258/ebm.2011.011297
Mucciolo, G., Roux, C., Scagliotti, A., Brugiapaglia, S., Novelli, F., & Cappello, P. (2020). The dark side of immunotherapy: Pancreatic cancer. Cancer Drug Resistance., 3, 491–520. https://doi.org/10.20517/cdr.2020.13
O’Reilly, E. M., Oh, D. Y., Dhani, N., Renouf, D. J., Lee, M. A., Sun, W., Fisher, G., Hezel, A., Chang, S. C., Vlahovic, G., Takahashi, O., Yang, Y., Fitts, D., & Philip, P. A. (2019). Durvalumab With or Without Tremelimumab for Patients With Metastatic Pancreatic Ductal Adenocarcinoma: A Phase 2 Randomized Clinical Trial. JAMA oncology, 5(10), 1431–1438. https://doi.org/10.1001/jamaoncol.2019.1588
Torphy, R. J., Zhu, Y., & Schulick, R. D. (2018). Immunotherapy for pancreatic cancer: Barriers and breakthroughs. Annals of Gastroenterological Surgery, 2(4), 274–281. https://doi.org/10.1002/ags3.12176
Matson, V., Chervin, C. S., & Gajewski, T. F. (2021). Cancer and the Microbiome-Influence of the Commensal Microbiota on Cancer, Immune Responses, and Immunotherapy. Gastroenterology, 160(2), 600–613. https://doi.org/10.1053/j.gastro.2020.11.041
Oster, P., Vaillant, L., Riva, E., McMillan, B., Begka, C., Truntzer, C., Richard, C., Leblond, M. M., Messaoudene, M., Machremi, E., et al. (2020). Helicobacter pylori infection has a detrimental impact on the efficacy of cancer immunotherapies. Gut. https://doi.org/10.1136/gutjnl-2020-323392
Otieno, S; Jain, A.L.; Mohammed, O; Patel, J.R.; Collyer, J; Deleeuw, P; Husain, A; Weir, A.B. (2021) Positive association between Helicobacter pylori infection and pancreatic cancer: A Case control study. Journal of Clinical Oncology. e16243.
Li, S., Fuhler, G. M., Bn, N., Jose, T., Bruno, M. J., Peppelenbosch, M. P., & Konstantinov, S. R. (2017). Pancreatic cyst fluid harbors a unique microbiome. Microbiome., 5(1), 147. https://doi.org/10.1186/s40168-017-0363-6
Vétizou, M., Pitt, J. M., Daillère, R., Lepage, P., Waldschmitt, N., Flament, C., Rusakiewicz, S., Routy, B., Roberti, M. P., Duong, C. P., Poirier-Colame, V., Roux, A., Becharef, S., Formenti, S., Golden, E., Cording, S., Eberl, G., Schlitzer, A., Ginhoux, F., Mani, S., et al. (2015). Anticancer immunotherapy by CTLA-4 blockade relies on the gut microbiota. Science (New York, N.Y.), 350(6264), 1079–1084. https://doi.org/10.1126/science.aad1329
Chaput, N., Lepage, P., Coutzac, C., Soularue, E., Le Roux, K., Monot, C., Boselli, L., Routier, E., Cassard, L., Collins, M., Vaysse, T., Marthey, L., Eggermont, A., Asvatourian, V., Lanoy, E., Mateus, C., Robert, C., & Carbonnel, F. (2017). Baseline gut microbiota predicts clinical response and colitis in metastatic melanoma patients treated with ipilimumab. Annals of Oncology, 28(6), 1368–1379. https://doi.org/10.1093/annonc/mdx108.Erratum.In:AnnOncol.2019Dec1;30(12):2012
Lopès, A., Billard, E., Casse, A. H., Villéger, R., Veziant, J., Roche, G., Carrier, G., Sauvanet, P., Briat, A., Pagès, F., Naimi, S., Pezet, D., Barnich, N., Dumas, B., & Bonnet, M. (2020). Colibactin-positive Escherichia coli induce a procarcinogenic immune environment leading to immunotherapy resistance in colorectal cancer. International Journal of Cancer, 146(11), 3147–3159. https://doi.org/10.1002/ijc.32920
Sivan, A., Corrales, L., Hubert, N., Williams, J. B., Aquino-Michaels, K., Earley, Z. M., Benyamin, F. W., Lei, Y. M., Jabri, B., Alegre, M. L., Chang, E. B., & Gajewski, T. F. (2015). Commensal Bifidobacterium promotes antitumor immunity and facilitates anti-PD-L1 efficacy. Science, 350(6264), 1084–1089. https://doi.org/10.1126/science.aac4255
Dutta, D., & Lim, S. H. (2020). Bidirectional interaction between intestinal microbiome and cancer: Opportunities for therapeutic interventions. Biomark Res, 8, 31. https://doi.org/10.1186/s40364-020-00211-6
Zhang, X., Zhou, Y., Chen, C., et al. (2019). Hepatitis B virus reactivation in cancer patients with positive Hepatitis B surface antigen undergoing PD-1 inhibition. Journal Immunotherapy Cancer, 7, 322. https://doi.org/10.1186/s40425-019-0808-5
Goradel NH, Alizadeh A, Hosseinzadeh S, Taghipour M, Ghesmati Z, Arashkia A, Negahdari B. (2021) Oncolytic virotherapy as promising immunotherapy against cancer: mechanisms of resistance to oncolytic viruses. Future Oncol. 25. https://doi.org/10.2217/fon-2021-0802
Conry, R. M., Westbrook, B., McKee, S., & Norwood, T. G. (2018). Talimogene laherparepvec: First in class oncolytic virotherapy. Human Vaccines & Immunotherapeutics, 14(4), 839–846. https://doi.org/10.1080/21645515.2017.1412896
Ries, S., & Korn, W. M. (2002). ONYX-015: Mechanisms of action and clinical potential of a replication-selective adenovirus. British Journal of Cancer, 86(1), 5–11. https://doi.org/10.1038/sj.bjc.6600006
Roussey, J. A., Viglianti, S. P., Teitz-Tennenbaum, S., Olszewski, M. A., & Osterholzer, J. J. (2017). Anti-PD-1 Antibody Treatment Promotes Clearance of Persistent Cryptococcal Lung Infection in Mice. The Journal of Immunology, 199(10), 3535–3546. https://doi.org/10.4049/jimmunol.1700840
Chang, K. C., Burnham, C. A., Compton, S. M., Rasche, D. P., Mazuski, R. J., McDonough, J. S., Unsinger, J., Korman, A. J., Green, J. M., & Hotchkiss, R. S. (2013). Blockade of the negative co-stimulatory molecules PD-1 and CTLA-4 improves survival in primary and secondary fungal sepsis. Critical Care, 17(3), R85. https://doi.org/10.1186/cc12711
Vernuccio, F., Messina, C., Merz, V., Cannella, R., & Midiri, M. (2021). Resectable and Borderline Resectable Pancreatic Ductal Adenocarcinoma: Role of the Radiologist and Oncologist in the Era of Precision Medicine. Diagnostics (Basel)., 11(11), 2166. https://doi.org/10.3390/diagnostics11112166
Krishnan, S., Chadha, A. S., Suh, Y., Chen, H. C., Rao, A., Das, P., Minsky, B. D., Mahmood, U., Delclos, M. E., Sawakuchi, G. O., Beddar, S., Katz, M. H., Fleming, J. B., Javle, M. M., Varadhachary, G. R., Wolff, R. A., & Crane, C. H. (2016). Focal Radiation Therapy Dose Escalation Improves Overall Survival in Locally Advanced Pancreatic Cancer Patients Receiving Induction Chemotherapy and Consolidative Chemoradiation. International Journal of Radiation Oncology, Biology, Physics, 94(4), 755–765. https://doi.org/10.1016/j.ijrobp.2015.12.003
Shen, Y., Zhu, X., Cao, F., Xie, H., Ju, X., Cao, Y., Qing, S., Jia, Z., Gu, L., Fang, F., & Zhang, H. (2021). Re-Irradiation With Stereotactic Body Radiotherapy for In-Field Recurrence of Pancreatic Cancer After Prior Stereotactic Body Radiotherapy: Analysis of 24 Consecutive Cases. Frontiers in Oncology, 11, 729490. https://doi.org/10.3389/fonc.2021.729490
Kim, Y. S., Kim, J., & Park, S. J. (2015). High-throughput 16S rRNA gene sequencing reveals alterations of mouse intestinal microbiota after radiotherapy. Anaerobe, 33, 1–7. https://doi.org/10.1016/j.anaerobe.2015.01.004
Parker, M.J.; Wearsch, P.A.; Veloo, A.C.M.; PRodriguez-Palacios, A. (2020) The Genus Alistipes: Gut Bacteria with Emerging Implications to Inflammation, Cancer and Mental Health. Front Immunol. https://doi.org/10.3389/fimmu.2020.00906.
Pushalkar, S., Hundeyin, M., Daley, D., Zambrinis, C. P., Kurz, E., Mishra, A., Mohan, N., Aykut, B., Usyk, M., Torres, L. E., et al. (2018). The Pancreatic Cancer Microbiome Promotes Oncogenesis by Induction of Innate and Adaptive Immune Suppression. https://doi.org/10.1158/2159-8290.CD-17-1134
F.
Bicker, K. L., & Thompson, P. R. (2013). The protein arginine deiminases: Structure, function, inhibition, and disease. Biopolymers, 99(2), 155–163. https://doi.org/10.1002/bip.22127
Xin, J., & Song, X. (2016). Role of peptidylarginine deaminase type 4 in gastric cancer. Experimetnatl and Therapeutic Medicine, 3155–60. https://doi.org/10.3892/etm.2016.3798
Bowles, T., Kim, R., Galante, J., Parsons, C., Virudachalam, S., Kung, H., & Bold, R. (2008). International Journal of Cancer, 123(8), 1950–1955. https://doi.org/10.1002/ijc.23723
Fine, D. H., Patil, A. G., & Velusamy, S. K. (2019). Aggregatibacter actinomycetemcomitans (Aa) Under the Radar: Myths and Misunderstandings of Aa and its role in Aggressive Periodontitis. Frontiers in Immunology. https://doi.org/10.3389/fimmu.2019.00728
Blum, R., & Kloog, Y. (2014). Metabolism addiction in pancreatic cancer. Cell Death & Disease, 5(2), e1065. https://doi.org/10.1038/cddis.2014.38
Cameron, M. E., Yakovenko, A., & Trevino, J. G. (2018). Glucose and Lactate Transport in Pancreatic Cancer: Glycolytic Metabolism Revisited. Journal of Oncology, 2018, 6214838. https://doi.org/10.1155/2018/6214838
Li, W; Han, L; Ma, Q. (2013) Hydrogen Peroxide Mediates Hyperglycemia-Enhanced Invasive Ability of Pancreatic Cancer Cells Via ERK and P38 MAPK Pathways. Annals of Oncology. 24(4): iv38-iv121. https://doi.org/10.1093/annonc/mdt203.39.
Waghray, M., Cui, Z., Horowitz, J. C., Subramanian, I. M., Martinez, F. J., Toews, G. B., et al. (2005). Hydrogen peroxide is a diffusible paracrine signal for the induction of epithelial cell death by activated myofibroblasts. The FASEB Journal, 19, 854–856.
Toullec, A., Gerald, D., Despouy, G., Bourachot, B., Cardon, M., Lefort, S., et al. (2010). Oxidative stress promotes myofibroblast differentiation and tumour spreading. EMBO Molecular Medicine, 2, 211–230. https://doi.org/10.1002/emmm.201000073
Kobayashi, Y., Nishikawa, M., Hyoudou, K., Yamashita, F., & Hashida, M. (2008). Hydrogen peroxide-mediated nuclear factor kappaB activation in both liver and tumor cells during initial stages of hepatic metastasis. Cancer Science, 99, 1546–1552. https://doi.org/10.1111/j.1349-7006.2008.00856.x
Lisanti, M. P., Martinez-Outschoorn, U. E., Lin, Z., Pavlides, S., Whitaker-Menezes, D., Pestell, R. G., Howell, A., & Sotgia, F. (2011). Hydrogen peroxide fuels aging, inflammation, cancer metabolism and metastasis: the seed and soil also needs “fertilizer.” Cell cycle (Georgetown, Tex.), 10(15), 2440–2449. https://doi.org/10.4161/cc.10.15.16870
Fu, Y., Yang, G., Zhu, F., et al. (2014). Antioxidants decrease the apoptotic effect of 5-Fu in colon cancer by regulating Src-dependent caspase-7 phosphorylation. Cell Death & Disease, 5, e983. https://doi.org/10.1038/cddis.2013.509
Erudaitius, D., Huang, A., Kazmi, S., Buettner, G. R., & Rodgers, V. G. J. (2017). Peroxporin Expression is an Important Factor for Cancer Cell susceptibility to Therapeutic H202: Implications for Pharmacological Ascorbate Therapy. PLOS ONE., 12(1), e0170442. https://doi.org/10.1371/journal.pone.0170442
Li, J. J., Zhu, M., Kashyap, P. C., et al. (2021). The role of microbiome in pancreatic cancer. Cancer and Metastasis Reviews, 40, 777–789. https://doi.org/10.1007/s10555-021-09982-2
Graham, F. (2019) Daily briefing: Fecal Transplant linked to patient’s death. Nature Briefing.
Chen, S. M., Chieng, W. W., Huang, S. W., et al. (2020). The synergistic tumor growth-inhibitory effect of probiotic Lactobacillus on transgenic mouse model of pancreatic cancer treated with gemcitabine. Science and Reports, 10, 20319. https://doi.org/10.1038/s41598-020-77322-5
Konishi, H., Isozaki, S., Kashima, S., et al. (2021). Probiotic Aspergillus oryzae produces anti-tumor mediator and exerts anti-tumor effects in pancreatic cancer through the p38 MAPK signaling pathway. Science and Reports, 11, 11070. https://doi.org/10.1038/s41598-021-90707-4
Kita, A., Fujiya, M., Konishi, H., Tanaka, H., Kashima, S., Iwama, T., Ijiri, M., Murakami, Y., Takauji, S., Goto, T., Sakatani, A., Ando, K., Ueno, N., Ogawa, N., & Okumura, T. (2020). Probiotic-derived ferrichrome inhibits the growth of refractory pancreatic cancer cells. International Journal of Oncology, 57(3), 721–732. https://doi.org/10.3892/ijo.2020.5096
Oláh, A., Belágyi, T., Pótó, L., Romics, L., Jr., & Bengmark, S. (2007). Synbiotic control of inflammation and infection in severe acute pancreatitis: A prospective, randomized, double blind study. Hepato-Gastroenterology, 54(74), 590–594.
Yadav, D., & Lowenfels, A. B. (2013). The epidemiology of pancreatitis and pancreatic cancer. Gastroenterology, 144(6), 1252–1261. https://doi.org/10.1053/j.gastro.2013.01.068
Genco, R. J., & Borgnakke, W. S. (2013). Risk factors for periodontal disease. Periodontol 2000, 62(1), 59–94. https://doi.org/10.1111/j.1600-0757.2012.00457.x
Leeming, E. R., Johnson, A. J., Spector, T. D., & Le Roy, C. I. (2019). Effect of Diet on the Gut Microbiota: Rethinking Intervention Duration. Nutrients, 11(12), 2862. https://doi.org/10.3390/nu11122862
Oliver, A., Chase, A. B., Weihe, C., Orchanian, S. B., Riedel, S F., Hendrickson, C. L., Lay, M., Sewall, J. M., Martiny, J. B. H., & Whiteson, K. (2021). High-Fiber, whole-food dietary intervention alters the human gut microbiome but not fecal short chain fatty acids. Journal of Clinical Microbiology. https://doi.org/10.1128/mSystems.00115-21
USDA Economic Research Service. (2020). Key Statistics and Graphics. Accessed 11/30/2021.
Shrider, E. A., Kollar, M., Semega, J. (2021). Income and poverty in the United States: 2020. United States Census Bureau. Accessed 11/30/2021.
Gui, X; Yang, Z; Li, M.D. (2021) Effect of cigarette smoke on gut microbiota: State of knowledge. Frontiers in Physiology. https://doi.org/10.3389/fphys.2021.673341.
Pandol, S. J., Apte, M. V., Wilson, J. S., Gukovskaya, A. S., & Edderkaoui, M. (2012). The burning question: why is smoking a risk factor for pancreatic cancer?. Pancreatology : official journal of the International Association of Pancreatology (IAP) ... [et al.], 12(4), 344–349. https://doi.org/10.1016/j.pan.2012.06.002
Uebanso, T., Shimohata, T., Mawatari, K., & Takahashi, A. (2020). Functional roles of B-vitamins in the gut and gut microbiome. Molecular Nutrition & Food Research, 64(18), 20000426. https://doi.org/10.1002/mnfr.202000426
Thomas, R. L., Jiang, L., Adams, J. S., et al. (2020). Vitamin D metabolites and the gut microbiome in older men. Nature Communications, 11, 5997. https://doi.org/10.1038/s41467-020-19793-8
Farrow, B., Rychahou, P., O’Connor, K. L., & Evers, B. M. (2003). Butyrate inhibits pancreatic cancer invasion. Journal of Gastrointestinal Surgery, 7(7), 864–870. https://doi.org/10.1007/s11605-003-0031-y
Natoni, F., Diolordi, L., Santoni, C., & Gilardini Montani, M. S. (2005). Sodium butyrate sensitises human pancreatic cancer cells to both the intrinsic and the extrinsic apoptotic pathways. Biochimica et Biophysica Acta, 1745(3), 318–329. https://doi.org/10.1016/j.bbamcr.2005.07.003
Chen, J., Zhao, K. N., & Vitetta, L. (2019). Effects of Intestinal Microbial-Elaborated Butyrate on Oncogenic Signaling Pathways. Nutrients, 11(5), 1026. https://doi.org/10.3390/nu11051026
Funding
Work in the laboratory of Azmi AS is supported by NIH R37 grant R37CA215427. The authors thank the SKY Foundation, and Perri Family Foundation for supporting part of this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest statement
ASA received funding from Karyopharm, EISAI, Jannsen and Rhizen. ASA received speaker fees from Karyopharm Therapeutics Inc. ASA is a council member at GLG and Guidepoint.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised: Author Misako Nagasaka and her affiliation was not captured in the published article.
Rights and permissions
About this article
Cite this article
Sexton, R.E., Uddin, M.H., Bannoura, S. et al. Connecting the Human Microbiome and Pancreatic Cancer. Cancer Metastasis Rev 41, 317–331 (2022). https://doi.org/10.1007/s10555-022-10022-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10555-022-10022-w