Abstract
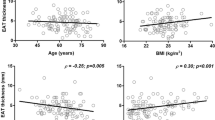
The present study tested the hypothesis that epicardial fat may be associated with augmented central aortic pressure and impaired left ventricular (LV) function. We studied 134 consecutive patients undergoing left-sided cardiac catheterization for coronary artery disease (CAD) and examined the relation of epicardial fat volume measured by multi-detector computed tomography to ascending aortic pressure and LV ejection fraction determined by cardiac catheterization as well as indices of LV diastolic function assessed by Doppler echocardiography [early diastolic mitral annular velocity (e′) and a ratio of early diastolic mitral inflow to annular velocities (E/e′)]. Epicardial fat volume indexed to body surface area correlated positively with age (r = 0.24, P < 0.01), body mass index (r = 0.38, P < 0.001), systolic aortic pressure (r = 0.21, P < 0.05), aortic pulse pressure (r = 0.23, P < 0.01), LV ejection fraction (r = 0.22, P < 0.05) and E/e′ (r = 0.24, P < 0.05) and did negatively with e′ (r = −0.31, P < 0.05). In multivariate linear regression including potential confounders, increased epicardial fat volume index correlated with aortic systolic and pulse pressure and LV diastolic function indices, but not LV ejection fraction. In conclusion, we found that epicardial fat was associated with augmented central aortic pressure and LV diastolic dysfunction in patients with known or suspected CAD.
Similar content being viewed by others
References
Iacobellis G, Corradi D, Sharma AM (2005) Epicardial adipose tissue: anatomic, biomolecular and clinical relationships with the heart. Nat Clin Pract Cardiovasc Med 2:536–543
Shimabukuro M (2009) Cardiac adiposity and global cardiometabolic risk: new concept and clinical implication. Circ J 73:27–34
Lim S, Meigs JB (2013) Ectopic fat and cardiometabolic and vascular risk. Int J Cardiol 169:166–176
Korkmaz L, Cirakoglu OF, Agac MT et al (2013) Relation of epicardial adipose tissue with arterial compliance and stiffness in patients with hypertension. Angiology (in press)
Kim BJ, Kim BS, Kang JH (2013) Echocardiographic epicardial fat thickness is associated with arterial stiffness. Int J Cardiol 167:2234–2238
Natale F, Tedesco MA, Mocerino R et al (2009) Visceral adiposity and arterial stiffness: echocardiographic epicardial fat thickness reflects, better than waist circumference, carotid arterial stiffness in a large population of hypertensives. Eur J Echocardiogr 10:549–555
Brinkley TE, Hsu FC, Carr JJ et al (2011) Pericardial fat is associated with carotid stiffness in the Multi-Ethnic Study of Atherosclerosis. Nutr Metab Cardiovasc Dis 21:332–338
O’Rourke MF, Mancia G (1999) Arterial stiffness. J Hypertens 17:1–4
Seino Y, Nanjo K, Tajima N et al (2010) Report of the committee on the classification and diagnostic criteria of diabetes mellitus. J Diabetes Investig 1:212–228
Teramoto T, Sasaki J, Ueshima H et al (2007) Executive summary of Japan Atherosclerosis Society (JAS) guideline for diagnosis and prevention of atherosclerotic cardiovascular diseases for Japanese. J Atheroscler Thromb 14:45–50
Dey D, Nakazato R, Li D, Berman DS (2012) Epicardial and thoracic fat—noninvasive measurement and clinical implications. Cardiovasc Diagn Ther 2:85–93
Chapman CB, Baker O, Reynolds J, Bonte FJ (1958) Use of biplane cinefluorography for measurement of ventricular volume. Circulation 18:1105–1117
Nagueh SF, Appleton CP, Gillebert TC et al (2009) Recommendations for the evaluation of left ventricular diastolic function by echocardiography. J Am Soc Echocardiogr 22:107–133
Schiller NB, Shah PM, Crawford M et al (1989) Recommendations for quantitation of the left ventricle by two-dimensional echocardiography. American Society of Echocardiography Committee on Standards, Subcommittee on Quantitation of Two-Dimensional Echocardiograms. J Am Soc Echocardiogr 2:358–367
Matsuo S, Imai E, Horio M et al (2009) Revised equations for estimated GFR from serum creatinine in Japan. Am J Kidney Dis 53:982–992
Hope SA, Tay DB, Meredith IT, Cameron JD (2003) Use of arterial transfer functions for the derivation of aortic waveform characteristics. J Hypertens 21:1299–1305
Iacobellis G, Leonetti F, Singh N, Sharma M (2007) Relationship of epicardial adipose tissue with atrial dimensions and diastolic function in morbidly obese subjects. Int J Cardiol 115:272–273
Cavalcante JL, Tamarappoo BK, Hachamovitch R et al (2012) Association of epicardial fat, hypertension, subclinical coronary artery disease, and metabolic syndrome with left ventricular diastolic dysfunction. Am J Cardiol 110:1793–1798
Park HE, Choi SY, Kim M (2014) Association of epicardial fat with left ventricular diastolic function in subjects with metabolic syndrome: assessment using 2-dimensional echocardiography. BMC Cardiovasc Disord 14:3
Hori M, Inoue M, Kitakaze M, Kitabatake A, Abe H (1985) Altered loading sequence as an underlying mechanism of afterload dependency of ventricular relaxation in hearts in situ. Jpn Circ J 49:245–254
Kohno F, Kumada T, Kambayashi M et al (1996) Change in aortic end-systolic pressure by alterations in loading sequence and its relation to left ventricular isovolumic relaxation. Circulation 93:2080–2087
Leite-Moreira AF, Correia-Pinto J, Gillebert TC (1999) Afterload induced changes in myocardial relaxation: a mechanism for diastolic dysfunction. Cardiovasc Res 43:344–353
Buckberg GD, Fixler DE, Archie JP, Hoffman JI (1972) Experimental subendocardial ischemia in dogs with normal coronary arteries. Circ Res 30:67–81
Paulus WJ, Grossman W, Serizawa T et al (1985) Different effects of two types of ischemia on myocardial systolic and diastolic function. Am J Physiol 248:H719–H728
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hachiya, K., Fukuta, H., Wakami, K. et al. Relation of epicardial fat to central aortic pressure and left ventricular diastolic function in patients with known or suspected coronary artery disease. Int J Cardiovasc Imaging 30, 1393–1398 (2014). https://doi.org/10.1007/s10554-014-0472-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10554-014-0472-2