Abstract
Purpose
Breast cancer incidence among younger women (under age 50) has increased over the past 25 years, yet little is known about the etiology among this age group. The objective of this study was to investigate relationships between modifiable and non-modifiable risk factors and early-onset breast cancer among three prospective Canadian cohorts.
Methods
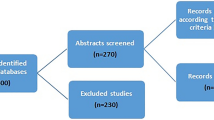
A matched case–control study was conducted using data from Alberta’s Tomorrow Project, BC Generations Project, and the Ontario Health Study. Participants diagnosed with breast cancer before age 50 were identified through provincial registries and matched to three control participants of similar age and follow-up. Conditional logistic regression was used to examine the association between factors and risk of early-onset breast cancer.
Results
In total, 609 cases and 1,827 controls were included. A body mass index ≥ 30 kg/m2 was associated with a lower risk of early-onset breast cancer (OR 0.65; 95% CI 0.47–0.90), while a waist circumference ≥ 88 cm was associated with an increased risk (OR 1.58; 95% CI 1.18–2.11). A reduced risk was found for women with ≥ 2 pregnancies (OR 0.76; 95% CI 0.59–0.99) and a first-degree family history of breast cancer was associated with an increased risk (OR 1.95; 95% CI 1.47–2.57).
Conclusions
In this study, measures of adiposity, pregnancy history, and familial history of breast cancer are important risk factors for early-onset breast cancer. Evidence was insufficient to conclude if smoking, alcohol intake, fruit and vegetable consumption, and physical activity are meaningful risk factors. The results of this study could inform targeted primary and secondary prevention for early-onset breast cancer.
Similar content being viewed by others
Data availability
The data that support the findings of this study are available from Alberta’s Tomorrow Project, BC Generations Project, Ontario Health Study, and Cancer Care Ontario but restrictions apply to the availability of these data, which were used under license for the current study, and so are not publicly available. Data are, however, available from the authors upon reasonable request and with permission of Alberta’s Tomorrow Project, BC Generations Project, Ontario Health Study, and Cancer Care Ontario.
References
Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A (2018) Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. Cancer J Clin 68:394–424
Brenner DR, Weir HK, Demers AA et al (2020) Projected estimates of cancer in Canada in 2020. Can Med Assoc J 192:E199
Heer E, Ruan Y, Mealey N, Quan ML, Brenner DR (2020) The incidence of breast cancer in Canada 1971–2015: trends in screening-eligible and young-onset age groups. Can J Public Health 111:787–793
Canadian Cancer Society’s Advisory Committee on Cancer Statistics (2017) Canadian cancer statistics 2017. Canadian Cancer Society, Toronto
Assi HA, Khoury KE, Dbouk H, Khalil LE, Mouhieddine TH, El Saghir NS (2013) Epidemiology and prognosis of breast cancer in young women. J Thorac Dis 5(Suppl 1):S2–S8
Brenner DR, Brockton NT, Kotsopoulos J et al (2016) Breast cancer survival among young women: a review of the role of modifiable lifestyle factors. Cancer Causes Control 27:459–472
Malone KE, Daling JR, Neal C et al (2000) Frequency of BRCA1/BRCA2 mutations in a population-based sample of young breast carcinoma cases. Cancer 88:1393–1402
Peto J, Collins N, Barfoot R et al (1999) Prevalence of BRCA1 and BRCA2 gene mutations in patients with early-onset breast cancer. J Natl Cancer Inst 91:943–949
Butt Z, Haider SF, Arif S et al (2012) Breast cancer risk factors: a comparison between pre-menopausal and post-menopausal women. J Pak Med Assoc 62:120–124
Chollet-Hinton L, Anders CK, Tse C-K et al (2016) Breast cancer biologic and etiologic heterogeneity by young age and menopausal status in the Carolina Breast Cancer Study: a case-control study. Breast Cancer Res 18:79
The Premenopausal Breast Cancer Collaborative G (2018) Association of body mass index and age with subsequent breast cancer risk in premenopausal women. JAMA Oncol 4:e181771
Kabat GC, Kim MY, Lee JS et al (2017) Metabolic obesity phenotypes and risk of breast cancer in postmenopausal women. Cancer Epidemiol Biomark Prev 26:1730–1735
Picon-Ruiz M, Morata-Tarifa C, Valle-Goffin JJ, Friedman ER, Slingerland JM (2017) Obesity and adverse breast cancer risk and outcome: mechanistic insights and strategies for intervention. Cancer J Clin 67:378–397
Rose DP, Vona-Davis L (2010) Interaction between menopausal status and obesity in affecting breast cancer risk. Maturitas 66:33–38
Althuis MD, Brogan DD, Coates RJ et al (2003) Breast cancers among very young premenopausal women (United States). Cancer Causes Control 14:151–160
Tavani A, Gallus S, La Vecchia C et al (1999) Risk factors for breast cancer in women under 40 years. Eur J Cancer 35:1361–1367
Dummer TJB, Awadalla P, Boileau C et al (2018) The Canadian Partnership for Tomorrow Project: a pan-Canadian platform for research on chronic disease prevention. Can Med Assoc J 190:E710
Amadou A, Hainaut P, Romieu I (2013) Role of obesity in the risk of breast cancer: lessons from anthropometry. J Oncol 2013:906495
White AJ, Nichols HB, Bradshaw PT, Sandler DP (2015) Overall and central adiposity and breast cancer risk in the sister study. Cancer 121:3700–3708
Huang Z, Willett WC, Colditz GA et al (1999) Waist circumference, waist: hip ratio, and risk of breast cancer in the nurses’ health study. Am J Epidemiol 150:1316–1324
Lahmann PH, Hoffmann K, Allen N et al (2004) Body size and breast cancer risk: findings from the European prospective investigation into cancer and nutrition (EPIC). Int J Cancer 111:762–771
Harris HR, Willett WC, Terry KL, Michels KB (2010) Body fat distribution and risk of premenopausal breast cancer in the Nurses’ Health Study II. J Natl Cancer Inst 103:273–278
Fagherazzi G, Chabbert-Buffet N, Fabre A et al (2012) Hip circumference is associated with the risk of premenopausal ER−/PR− breast cancer. Int J Obes 36:431–439
Carney PI (2010) Obesity and reproductive hormone levels in the transition to menopause. Menopause 17:678–679
Andrew GR, Michelle H, Anthony H (2006) Insulin-like growth factor (IGF)-I, IGF binding protein-3, and breast cancer risk: eight years on. Endocrine-Relat Cancer Endocr Relat Cancer 13:273–278
Collaborative Group on Hormonal Factors in Breast Cancer (2001) Familial breast cancer: collaborative reanalysis of individual data from 52 epidemiological studies including 58 209 women with breast cancer and 101 986 women without the disease. The Lancet 358:1389–1399
Anders CK, Johnson R, Litton J, Phillips M, Bleyer A (2009) Breast cancer before age 40 years. Semin Oncol 36:237–249
Peto J, Mack TM (2000) High constant incidence in twins and other relatives of women with breast cancer. Nat Genet 26:411–414
Ginsburg OM, Akbari MR, Aziz Z et al (2009) The prevalence of germ-line TP53 mutations in women diagnosed with breast cancer before age 30. Fam Cancer 8:563
Canadian Cancer Society (2020) Getting screened for breast cancer
Canadian Task Force on Preventive Health Care (2020) Breast cancer tools and resources
NCCN Clinical Practise Guidelines In Oncology (2019) Breast Cancer Screening and Diagnosis. Nation Comprehensive Cancer Network
Klarenbach S, Sims-Jones N, Lewin G et al (2018) Recommendations on screening for breast cancer in women aged 40–74 years who are not at increased risk for breast cancer. Can Med Assoc J 190:E1441
Nelson HD, Zakher B, Cantor A et al (2012) Risk factors for breast cancer for women aged 40 to 49 years: a systematic review and meta-analysis. Ann Intern Med 156:635–648
Albrektsen G, Heuch I, Hansen S, Kvåle G (2005) Breast cancer risk by age at birth, time since birth and time intervals between births: exploring interaction effects. Br J Cancer 92:167–175
Liu Q, Wuu J, Lambe M, Hsieh S-F, Ekbom A, Hsieh C-C (2002) Transient increase in breast cancer risk after giving birth: postpartum period with the highest risk (Sweden). Cancer Causes Control 13:299–305
Nichols HB, Schoemaker MJ, Cai J et al (2018) Breast cancer risk after recent childbirth. Ann Intern Med 170:22–30
Russo J, Balogh GA, Russo IH (2008) Full-term pregnancy induces a specific genomic signature in the human breast. Cancer Epidemiol Biomark Prev 17:51–66
Meier-Abt F, Milani E, Roloff T et al (2013) Parity induces differentiation and reduces Wnt/Notch signaling ratio and proliferation potential of basal stem/progenitor cells isolated from mouse mammary epithelium. Breast Cancer Res 15:R36
Lyons TR, Schedin PJ, Borges VF (2009) Pregnancy and breast cancer: when they collide. J Mammary Gland Biol Neoplasia 14:87–98
Akinyemiju TF, Pisu M, Waterbor JW, Altekruse SF (2015) Socioeconomic status and incidence of breast cancer by hormone receptor subtype. Springerplus 4:508
Heck KE, Pamuk ER (1997) Explaining the relation between education and postmenopausal breast cancer. Am J Epidemiol 145:366–372
Robert SA, Strombom I, Trentham-Dietz A et al (2004) Socioeconomic risk factors for breast cancer: distinguishing individual- and community-level effects. Epidemiology 15:442–450
Tweed EJ, Allardice GM, McLoone P, Morrison DS (2018) Socio-economic inequalities in the incidence of four common cancers: a population-based registry study. Public Health 154:1–10
Akinyemiju TF, Demb J, Izano MA et al (2018) The association of early life socioeconomic position on breast cancer incidence and mortality: a systematic review. Int J Public Health 63:787–797
Lundqvist A, Andersson E, Ahlberg I, Nilbert M, Gerdtham U (2016) Socioeconomic inequalities in breast cancer incidence and mortality in Europe—a systematic review and meta-analysis. Eur J Pub Health 26:804–813
Gadeyne S, Deboosere P, Vandenheede H, Neels K (2012) Does birth history account for educational differences in breast cancer mortality? A comparison of premenopausal and postmenopausal women in Belgium. Int J Cancer 131:2878–2885
Lehrer S, Green S, Rosenzweig KE (2016) Affluence and Breast Cancer. Breast J 22:564–567
Borugian MJ, Spinelli JJ, Abanto Z, Xu CL, Wilkins R (2011) Breast cancer incidence and neighbourhood income. Health Rep 22:7–13
Goldberg M, Calderon-Margalit R, Paltiel O et al (2015) Socioeconomic disparities in breast cancer incidence and survival among parous women: findings from a population-based cohort, 1964–2008. BMC Cancer 15:921
Menvielle G, Kunst AE, van Gils CH et al (2010) The contribution of risk factors to the higher incidence of invasive and in situ breast cancers in women with higher levels of education in the european prospective investigation into cancer and nutrition. Am J Epidemiol 173:26–37
de Kok IMCM, van Lenthe FJ, Avendano M, Louwman M, Coebergh J-WW, Mackenbach JP (2008) Childhood social class and cancer incidence: results of the globe study. Soc Sci Med 66:1131–1139
Gerber B, Müller H, Reimer T, Krause A, Friese K (2003) Nutrition and lifestyle factors on the risk of developing breast cancer. Breast Cancer Res Treat 79:265–276
Møller H, Tønnesen H (1997) Alcohol drinking, social class and cancer. IARC Sci Publ 138:251–263
Potter JD (1997) Diet and cancer: possible explanations for the higher risk of cancer in the poor. IARC Sci Publ 138:265–283
Berger E, Castagné R, Chadeau-Hyam M et al (2019) Multi-cohort study identifies social determinants of systemic inflammation over the life course. Nat Commun 10:773
Pepys MB, Baltz ML (1983) Acute phase proteins with special reference to C-reactive protein and related proteins (pentaxins) and serum amyloid A protein. Adv Immunol 34:141–212
McDade TW, Lindau ST, Wroblewski K (2011) Predictors of C-reactive protein in the national social life, health, and aging project. J Gerontol B Psychol Sci Soc Sci 66:129–136
Kershaw KN, Mezuk B, Abdou CM, Rafferty JA, Jackson JS (2010) Socioeconomic position, health behaviors, and C-reactive protein: a moderated-mediation analysis. Health Psychol 29:307–316
Guo L, Liu S, Zhang S et al (2015) C-reactive protein and risk of breast cancer: a systematic review and meta-analysis. Sci Rep 5:10508
Asegaonkar SB, Asegaonkar BN, Takalkar UV, Advani S, Thorat AP (2015) C-reactive protein and breast cancer: new insights from old molecule. Int J Breast Cancer 2015:145647
Robson PJ, Solbak NM, Haig TR et al (2016) Design, methods and demographics from phase I of Alberta’s Tomorrow Project cohort: a prospective cohort profile. CMAJ Open 4:E515–E527
Acknowledgments
We would like to thank and acknowledge the Albert Cancer Registry, Alberta’s Tomorrow Project, BC Generations Project, Ontario Health Study, and Cancer Care Ontario. Alberta’s Tomorrow Project is only possible because of the commitment of its research participants, its staff and its funders: Alberta Health, Alberta Cancer Foundation, Canadian Partnership Against Cancer and Health Canada, and substantial in kind funding from Alberta Health Services. Cancer registry data was obtained through linkage with Surveillance & Reporting, Cancer Research & Analytics, Cancer Care Alberta. The views expressed herein represent the views of the author(s) and not of the data sources or any of its funders. The views expressed herein represent the views of the author(s) and not of the data sources or any of its funders.
Funding
Dr. Darren R. Brenner is supported by the Armstrong Investigatorship in Molecular Epidemiology from the Cumming School of Medicine at the University of Calgary and a Canadian Institutes of Health Research Grant (#397332). Dylan O’Sullivan was supported by an Ontario Graduate Scholarship and a Chen-Aronson Fellowship in Causes of Cancer.
Author information
Authors and Affiliations
Contributions
DRB: Conception and design. DRB, RBB, DEO and JP: Development of methodology. DRB, CMF, RM, EW, MLQ, and JP: Acquisition of data (provided animals, acquired and managed patients, provided facilities, etc.). JP, RBB, DEO and DRB: Analysis and interpretation of data (e.g., statistical analysis, biostatistics, computational analysis). JP, RBB, DEO and DRB, NEM, YR, CMF, RM, EW, and MLQ: Writing, review, and/or revision of the manuscript. JP, RBB: Administrative, technical, or material support (i.e., reporting or organizing data, constructing databases). DRB: Study supervision.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no potential conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Pader, J., Basmadjian, R.B., O’Sullivan, D.E. et al. Examining the etiology of early-onset breast cancer in the Canadian Partnership for Tomorrow’s Health (CanPath). Cancer Causes Control 32, 1117–1128 (2021). https://doi.org/10.1007/s10552-021-01460-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10552-021-01460-y