Abstract
Purpose
To determine whether smoking, in any form, is a risk factor in the development of cervical cancer (CC) among urban Chinese women.
Methods
We ascertained retrospectively the smoking habits of 1,865 women (aged 35+) who had died from CC (cases) and 48,781 who had died from causes unrelated to smoking (controls) in 24 cities using data from a large national survey of smoking and mortality in 1989–1991. We assessed the risk of smoking on CC mortality with and without considering passive smoke exposure from a spouse using a proportional mortality study design.
Results
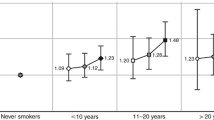
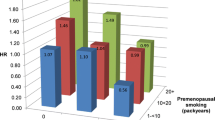
Overall, there was a 51.0 % excess risk of death from CC among smokers. When the spouse’s exposure was further considered, the RR (95 % CI) for exposed versus unexposed women was 1.28 (1.04–1.57) for passive smokers, 1.49 (1.02–2.20) for active smokers, and 1.69 (1.27–2.26) for women with both exposures (all p < 0.001). Significant dose–response associations were observed between smoking and CC for all categories of exposure. For example, individuals with both smoking exposure had the highest risk of CC mortality with moderate [RR = 1.67 (1.18–2.38)] and high [RR = 1.88 (1.04–3.41)] daily cigarette consumption, and they also had the highest risk with ≤15 years exposure [RR = 1.73 (1.19–2.52)] and >15 years exposure [RR = 1.95 (1.15–3.32)], compared with the active and passive groups (p for trend <0.001).
Conclusions
Younger trend of CC death and the rapid increase in smoking among young women may have a profound impact on future incidence of CC. Our findings emphasize the need for preventive efforts among both women and men in China.



Similar content being viewed by others
References
Liang J (2002) To meet global challenges and opportunities to prevent cervical cancer. Chin J Obstet Gynecol 37:129–131
He J, Chen WQ (2013) Chinese cancer registry annual report, 2012. Military Medical Science Press, Beijing
Zhao F, Hu S, Zhang S et al (2010) Cervical cancer mortality in 2004–2005 and changes during last 30 years in China. Chin J Prev Med 44:409–413
Walboomers JM, Jacobs MV, Manos MM et al (1999) Human papillomavirus is a necessary cause of invasive cervical cancer worldwide. J Pathol 189:12–19
Jensen KE, Schmiedel S, Frederiksen K, Norrild B, Iftner T, Kjær SK (2012) Risk for cervical intraepithelial neoplasia grade 3 or worse in relation to smoking among women with persistent human papillomavirus infection. Cancer Epidemiol Biomark Prev 21(11):1949–1955
Plummer M, Herrero R, Franceschi S, Meijer CJLM, Snijders P, Bosch FX et al (2003) Smoking and cervical cancer: pooled analysis of the IARC multi-centric case–control study. Cancer Causes Control 14:805–814
International Agency for Research on Cancer (1986) IARC Monographs programme on the evaluation of the carcinogenic risk of chemicals to humans. Preamble. IARC Monogr Eval Carcinog Risk Chem Hum 39:13–32
International Agency for Research on Cancer (2004) IARC monographs on the evaluation of carcinogenic risks to humans. Vol. 83: tobacco smoke and involuntary smoking. Iarc, Lyon
Trimble CL, Genkinger JM, Burke AE (2005) Active and passive cigarette smoking and the risk of cervical neoplasia. Obstet Gynecol 105(1):174–181
Zhou Q et al (2011) Influencing factors for cervical cancer of Chinese married women, a meta-analysis. China Oncol 21:125–129
Jia Y et al (2012) Case-control study of diet in patients with cervical cancer or precancerosis in wufeng, a high incidence region in China. Asian Pac J Cancer Prev 13:5299–5302
Liu B-Q et al (1998) Emerging tobacco hazards in China: 1. Retrospective proportional mortality study of one million deaths. BMJ 317:1411–1422
Yang GH (ed) (1997) Report on the 1996 nationwide survey of smoking prevalence. China Science and Technology Press, Beijing
Deng J, Gao YT (1985) The prevalence of smoking habit among 110 000 adult residents in urban Shanghai [in Chinese]. Chin J Prev Med 5:271–274
Yang GH, Ma JM, Liu N, Zhou LN (2005) 2002 survey of active and passive smoking of Chinese population. Chin J Prev Med 26:77–83
Xu T, Li W, Hu P (2010) Survey of smoking and passive smoking status among Chinese adults in 11 provinces. Chin J Prev Contrib Chronic Dis 18:229–230
Fonseca-Moutinho JA (2011) Smoking and cervical cancer. ISRN Obstet Gynecol 2011:847684
Lacey JV et al (2001) Associations between smoking and adenocarcinomas and squamous cell carcinomas of the uterine cervix (United States). Cancer Causes Control 12:153–161
Hildesheim A et al (2001) HPV co-factors related to the development of cervical cancer: results from a population-based study in Costa Rica. Br J Cancer 84:1219
Natphopsuk S, Settheetham-Ishida W, Sinawat S, Pientong C, Yuenyao P, Ishida T (2012) Risk factors for cervical cancer in Northeastern Thailand: detailed analyses of sexual and smoking behavior. Asian Pasic J Cancer Prev 13:5489–5495
Chen Zhu (2008) The report of the third national retrospective sampling survey of death causes. Peking Union Medical College Press, Beijing
Capps NP, Stewart A, Burns C (2009) The interplay between secondhand cigarette smoke, genetics, and cervical cancer: a review of the literature. Biol Res Nurs 10:392–399
Jones CJ et al (1991) Elevated nicotine levels in cervical lavages from passive smokers. Am J Public Health 81:378–379
Seccareccia F et al (2003) Serum cotinine as a marker of environmental tobacco smoke exposure in epidemiological studies: the experience of the MATISS project. Eur J Epidemiol 18:487–492
Matt G et al (2004) Households contaminated by environmental tobacco smoke: sources of infant exposures. Tob Control 13:29–37
McCann MF et al (1992) Nicotine and cotinine in the cervical mucus of smokers, passive smokers, and nonsmokers. Cancer Epidemiol Biomark Prev 1:125–129
Poppe W et al (1995) Tobacco smoking and the uterine cervix: cotinine in blood, urine and cervical fluid. Gynecol Obstet Invest 39:110–114
Szarewski A et al (1996) Effect of smoking cessation on cervical lesion size. Lancet 347:941–943
Prokopczyk B, Cox JE, Hoffmann D (1997) Identification of tobacco-specific carcinogen in the cervical mucus of smokers and nonsmokers. J Natl Cancer Inst 89:868–873
Eppel W et al (2000) The influence of cotinine on interleukin 6 expression in smokers with cervical preneoplasia. Acta Obstet Gynecol Scand 79:1105–1111
Szarewski A et al (2001) The effect of stopping smoking on cervical Langerhans’ cells and lymphocytes. BJOG 108:295–303
Sun Hongwei, Zhang Chong (2013) The Chang trend in Chinese married status in the past decades. J Sichuan Univ Sci Eng 28:11–17
Zhang R (2012) Study on HPV type distribution/smoking and cervical cancer and validation of a new screening method. Doctoral thesis, Cancer Institute and Hospital, Chinese Academy of Medical Sciences, Beijing. http://med.wanfangdata.com.cn/Paper/Detail/DegreePaper_Y2123298
Zhao FH, Lin MJ, Chen F, Hu SY, Zhang R, Belinson J, Sellors J, Franceschi S, Qiao YL, Castle P (2010) Performance of high-risk human papillomavirus DNA testing as a primary screen for cervical cancer: a pooled analysis of individual patient data from 17 population-based studies from China. Lancet Oncol 11:1160–1171
Bosch FX, Lorincz A, Munoz N, Meijer CJLM, Shah KV (2002) The causal relation between human papillomavirus and cervical cancer[J]. J Clin Pathol 55:244–265
Acknowledgments
We thank Cancer Research UK, the UK Medical Research Council, the US National Institutes of Health, the Chinese Ministry of Health for supporting the original survey. We thank Professor Richard Peto, who gave us great support for the project. The thousands of doctors, nurses, and other field workers who conducted the surveys, the local governments for their cooperation, and the million interviewees are greatly acknowledged.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Jingmei Jiang and Haiyu Pang have contributed equally to this work (joint first authors).
Rights and permissions
About this article
Cite this article
Jiang, J., Pang, H., Liu, B. et al. Effects of active, passive, and combined smoking on cervical cancer mortality: a nationwide proportional mortality study in Chinese urban women. Cancer Causes Control 26, 983–991 (2015). https://doi.org/10.1007/s10552-015-0580-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10552-015-0580-x