Abstract
Objectives
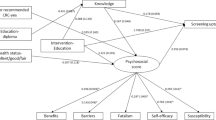
We examined the interrelationships between and contributions of background, cognitive, and environmental factors to colorectal cancer (CRC) screening adherence.
Methods
In this study, 2,416 average risk patients aged 50–75 from 24 Veterans Affairs medical facilities responded to a mailed survey with phone follow-up (response rate 81%). Survey data (attitudes, behaviors, demographics) were linked to facility (organizational complexity) and medical records data (diagnoses, screening history). Patients with a fecal occult blood test within 15 months, sigmoidoscopy or barium enema within 5.5 years, or colonoscopy within 11 years of the survey were considered adherent. Logistic regressions estimated the association between adherence and background, cognitive, and environmental factors. Deviance ratios examined interrelationships between factors. Population attributable risks (PAR) were used to identify intervention targets.
Results
The association of background factors with adherence was partially explained by cognitive and environmental factors. The association of environmental factors with adherence was partially explained by cognitive factors. Cognitive and environmental factors contributed equally to adherence. Factors with the highest PARs for non-adherence were age 50–64, less than two comorbidities, and lack of physician recommendation.
Conclusions
Efforts to increase physician screening recommendations for younger, healthy patients at facilities with the lowest screening rates may improve CRC adherence in this setting.


Similar content being viewed by others
References
American Cancer Society (2008) Cancer facts and figures 2008. American Cancer Society, Atlanta
Hardcastle JD, Chamberlain JO, Robinson MH et al (1996) Randomised controlled trial of faecal-occult-blood screening for colorectal cancer. Lancet 348:1472–1477
Kronborg O, Fenger C, Olsen J, Jorgensen OD, Sondergaard O (1996) Randomised study of screening for colorectal cancer with faecal-occult-blood test. Lancet 348:1467–1471
Mandel JS, Bond JH, Church TR et al (1993) Reducing mortality from colorectal cancer by screening for fecal occult blood. Minnesota Colon Cancer Control Study. N Engl J Med 328:1365–1371
Newcomb PA, Norfleet RG, Storer BE, Surawicz TS, Marcus PM (1992) Screening sigmoidoscopy and colorectal cancer mortality. J Natl Cancer Inst 84:1572–1575
Selby JV, Friedman GD, Quesenberry CP Jr, Weiss NS (1992) A case-control study of screening sigmoidoscopy and mortality from colorectal cancer. N Engl J Med 326:653–657
U.S. Preventive Services Task Force (2008) Screening for colorectal cancer: U.S. Preventive Services Task Force recommendation statement. Ann Int Med 149:627–637
U.S. Preventive Services Task Force (2002) Colorectal cancer screening guidelines. Agency for Healthcare Research and Quality, Rockville
U.S. Preventive Services Task Force (1996) US Preventive Services Task Force guide to clinical preventive services. Williams and Wilkins, Baltimore
Schroy PC (2002) Barriers to colorectal cancer screening: part 1—patient noncompliance. Med Gen Med 4(2)
Schroy PC (2002) Barriers to colorectal cancer screening: part 2—provider underutilization. Med Gen Med 4(3)
Subramanian S, Klosterman M, Amonkar MM, Hunt TL (2004) Adherence with colorectal cancer screening guidelines: a review. Prev Med 38:536–550
Rosenstock IM (2002) The health belief model: explaining health behavior through expectancies. In: Glanz K, Lewis FM, Rimer BK (eds) Health behavior and health education, theory, research, and practice. Jossey-Bass Publishers, San Francisco, pp 39–62
Ajzen I (2005) Attitudes, personality, and behavior. Open University Press/McGraw-Hill, Milton-Keynes
Bandura A (2000) Health promotion from the perspective of social cognitive theory. In: Abraham C, Norman P, Connor M (eds) Understanding and changing health behavior: from health beliefs to self-regulation. Harwood Academic Publishers, Amsterdam, pp 299–342
Partin MR, Grill J, Noorbaloochi S et al (2008) Validation of self-reported colorectal cancer screening behavior from a mixed-mode survey of veterans. Cancer Epidemiol Biomarkers Prev 17:768–776
Vernon SW, Meissner H, Klabunde C et al (2004) Measures for ascertaining use of colorectal cancer screening in behavioral, health services, and epidemiologic research. Cancer Epidemiol Biomarkers Prev 13:898–905
Vernon SW, Tiro JA, Vojvodic RW et al (2008) Reliability and validity of a questionnaire to measure colorectal cancer screening behaviors: does mode of survey administration matter? Cancer Epidemiol Biomarkers Prev 17:758–767
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40:373–383
Deyo RA, Cherkin DC, Ciol MA (1992) Adapting a clinical comorbidity index for use with ICD-9-CM administrative databases. J Clin Epidemiol 45:613–619
Manne S, Markowitz A, Winawer S et al (2002) Correlates of colorectal cancer screening compliance and stage of adoption among siblings of individuals with early onset colorectal cancer. Health Psychol 21:3–15
Rutten LF, Moser RP, Beckjord EB, Hesse BW, Croyle RT (2007) Cancer communication: health information national trends survey. NIH Pub. No. 07-6214. National Cancer Institute, Washington
Vernon SW, Myers RE, Tilley BC (1997) Development and validation of an instrument to measure factors related to colorectal cancer screening adherence. Cancer Epidemiol Biomarkers Prev 6:825–832
Sherbourne CD, Stewart AL (1991) The MOS social support survey. Soc Sci Med 32:705–714
Tiro JA, Vernon SW, Hyslop T, Myers RE (2005) Factorial validity and invariance of a survey measuring psychosocial correlates of colorectal cancer screening among African Americans and Caucasians. Cancer Epidemiol Biomarkers Prev 14:2855–2861
Stefos T, LaVellee N, Holden F (1992) Fairness in prospective payment: a clustering approach. Health Serv Res 27:239–261
Szabo CR (2005) 2005 Facility complexity model. Veterans Health Administration, NLB Human Resources Committee, Washington
Washington DL, Yano EM, Goldzweig C, Simon B (2006) VA emergency health care for women: condition-critical or stable? Women’s Health Issues 16:133–138
Yano EM, Soban LM, Parkerton PH, Etzioni DA (2007) Primary care practice organization influences colorectal cancer screening performance. Health Serv Res 42:1130–1149
Nelson D, Noorbaloochi S (2009) Dimension reduction summaries for balanced comparisons. J Stat Plan Inference 139(2):617–628
Noorbaloochi S, Nelson D (2008) Conditionally specified models and dimension reduction in the exponential families. J Multivar Anal 99:1574–1589
Little RJA, Rubin DB (2003) Statistical analysis with missing data. Wiley, New York
Rubin DB (1987) Multiple imputation for nonresponse in surveys. Wiley, New York
Zhang J, Yu KF (1998) What’s the relative risk? A method of correcting the odds ratio in cohort studies of common outcomes. JAMA 280:1690–1691
Partin MR, Slater JS (2003) Promoting repeat mammography use: insights from a systematic needs assessment. Health Educ Behav 30:97–112
Andersen RM (1995) Revisiting the behavioral model and access to medical care: does it matter? J Health Soc Behav 36:1–10
Honda K, Kagawa-Singer M (2006) Cognitive mediators linking social support networks to colorectal cancer screening adherence. J Behav Med 29:449–460
Power E, Jaarsveld CHM, McCaffery K, Miles A, Atkin W, Wardle J (2008) Understanding intentions and action in colorectal cancer screening. Ann Behav Med 35:285–294
Brenes GA, Paskett ED (2000) Predictors of stage of adoption for colorectal cancer screening. Prev Med 31:410–416
Kelly RB, Shank JC (1992) Adherence to screening flexible sigmoidoscopy in asymptomatic patients. Med Care 30:1029–1042
Lewis SF, Jensen NM (1996) Screening sigmoidoscopy. Factors associated with utilization. J Gen Intern Med 11:542–544
Lipkus IM, Rimer BK, Lyna PR, Pradhan AA, Conaway M, Woods-Powell CT (1996) Colorectal screening patterns and perceptions of risk among African–American users of a community health center. J Commun Health 21:409–427
Vernon SW (1997) Participation in colorectal cancer screening: a review. J Natl Cancer Inst 89:1406–1422
Weitzman ER, Zapka J, Estabrook B, Goins KV (2001) Risk and reluctance: understanding impediments to colorectal cancer screening. Prev Med 32:502–513
Zapka JG, Puleo E, Vickers-Lahti M, Luckmann R (2002) Healthcare system factors and colorectal cancer screening. Am J Preven Med 23:28–35
McQueen A, Vernon SW, Meissner HI, Klabunde CN, Rakowski W (2006) Are there gender differences in colorectal cancer test use prevalence and correlates? Cancer Epidemiol Biomarkers Prev 15:782–791
Bastani R, Maxwell AE, Bradford C (1996) Cross-sectional versus prospective predictors of screening mammography. Cancer Epidemiol Biomarkers Prev 5:845–848
McQueen A, Vernon SW, Myers RE, Watts BG, Lee ES, Tilley BC (2007) Correlates and predictors of colorectal cancer screening among male automotive workers. Cancer Epidemiol Biomarkers Prev 16:500–509
Acknowledgments
This project was supported by three grants from the United States’ Veterans Affairs Health Services Research & Development service: Investigator Initiated grant #IIR 04-042-2 (Partin); Career Development Award #RCD03-174 (Fisher); and Merit Review Entry Program award #MRP 04-412-1 (Burgess).
Author information
Authors and Affiliations
Corresponding author
Appendix
Appendix
The ratio statistic for examining whether background factors are mediated by cognitive and environmental factors was calculated as follows:
-
1.
A model including only the intercept was fit and its deviance, D(intercept), was computed.
-
2.
A model including the intercept and X (all measures of background factors) was fit and its deviance, D(intercept, X), was computed.
-
3.
We then computed the difference between these two deviances, DevDiff(X) = D(intercept) − D(intercept, X), which is a measure of the unadjusted association of X with Y.
-
4.
A model including the intercept and M (all measures of cognitive and environmental factors) was fit and its deviance, D(intercept, M) was computed.
-
5.
A model including the intercept, M, and X was fit, and its deviance, D(intercept, M, X), was computed.
-
6.
We then computed the difference between these two deviances, DevDiff (X|M) = D(intercept, M) − D(intercept, M, X), which is a measure of the conditional (adjusted) association of X with Y after adjusting for M.
-
7.
We then compute the ratio: \( {\frac{{{\text{DevDiff}}({\mathbf{X}}|{\mathbf{M}})}}{{{\text{DevDiff}}({\mathbf{X}})}}} \).
-
8.
To calculate a confidence interval for the ratio statistic, we used bootstrapping methods. Specifically, bootstrapping drawing n = 1,000 repeated samples of size = 2,416 with replacement were used to calculate the ratio for each sample. We then determined the mean and 2.5 and 97.5 percentiles of the resulting sampling distribution to obtain a point estimate and accompanying 95% CI for the ratio.
The ratio statistic for examining whether social environmental factors are mediated by cognitive factors was calculated as follows:
-
1.
A model including only the intercept was fit and its deviance, D(intercept), was computed.
-
2.
A model including the intercept and X (all measures of social environmental factors) was fit and its deviance, D(intercept, X), was computed.
-
3.
We then computed the difference between these two deviances, DevDiff(X) = D(intercept) − D(intercept, X), which is a measure of the unadjusted association of X with Y.
-
4.
A model including the intercept and M (all measures of cognitive factors) was fit and its deviance, D(intercept, M), was computed.
-
5.
A model including the intercept, M, and X was fit, and its deviance, D(intercept, M, X), was computed.
-
6.
We then computed the difference between these two deviances, DevDiff (X|M) = D(intercept, M) − D(intercept, M, X), which is a measure of the conditional (adjusted) association of X with Y after adjusting for M.
-
7.
We then compute the ratio: \( {\frac{{{\text{DevDiff}}({\mathbf{X}}|{\mathbf{M}})}}{{{\text{DevDiff}}({\mathbf{X}})}}} \).
-
8.
The same bootstrapping methods described earlier were used to calculate a confidence interval for this ratio statistic
The ratio statistic for examining whether medical environmental factors are mediated by cognitive factors was calculated as follows:
-
1.
A model including only the intercept was fit and its deviance, D(intercept), was computed.
-
2.
A model including the intercept and X (all measures of medical environmental factors) was fit and its deviance, D(intercept, X), was computed.
-
3.
We then computed the difference between these two deviances, DevDiff(X) = D(intercept) − D(intercept, X), which is a measure of the unadjusted association of X with Y.
-
4.
A model including the intercept and M (all measures of cognitive factors) was fit and its deviance, D(intercept, M) was computed.
-
5.
A model including the intercept, M, and X was fit, and its deviance, D(intercept, M, X), was computed.
-
6.
We then computed the difference between these two deviances, DevDiff (X|M) = D(intercept, M) − D(intercept, M, X), which is a measure of the conditional (adjusted) association of X with Y after adjusting for M.
-
7.
We then compute the ratio: \( {\frac{{{\text{DevDiff}}({\mathbf{X}}|{\mathbf{M}})}}{{{\text{DevDiff}}({\mathbf{X}})}}} \).
-
8.
The same bootstrapping methods described earlier were used to calculate a confidence interval for this ratio statistic
Steps involved in assessing whether environmental or cognitive factors had a greater association with adherence:
-
1.
A model including the intercept and the background factors was fit and its deviance, D(intercept, background), was computed.
-
2.
A model including the intercept, the background factors, and the cognitive factors was fit and its deviance, D(intercept, background, cognitive), was computed.
-
3.
A model including the intercept, the background factors, and the environmental factors was fit and its deviance, D(intercept, background, environmental), was computed.
-
4.
We then computed the following two deviance differences: DevDiff (cognitive|background) = D(intercept, background) − D(intercept, background, cognitive), a measure of the association of the cognitive factors on screening adherence adjusting for the background factors; and DevDiff (environmental|background) = D(intercept, background) − D(intercept, background, environmental), a measure of the association of the environmental factors with screening adherence adjusting for the background factors.
-
5.
\( {\frac{{{\text{DevDiff}}({\text{cognitive}}|{\text{background}})}}{{{\text{DevDiff}}({\text{environmental}}|{\text{background}})}}} \)We then computed the ratio of these measures of association:
-
6.
Bootstrapping methods as described earlier were then used to derive a point estimate and 95% confidence interval for the ratio.
Rights and permissions
About this article
Cite this article
Partin, M.R., Noorbaloochi, S., Grill, J. et al. The interrelationships between and contributions of background, cognitive, and environmental factors to colorectal cancer screening adherence. Cancer Causes Control 21, 1357–1368 (2010). https://doi.org/10.1007/s10552-010-9563-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10552-010-9563-0