Abstract
Background
Modifying multiple behavior risks is a promising approach to reduce cancer risk. Primary prevention advices of the European Code against Cancer were included in an educational intervention (EI) using social cognitive theories for motivating families with cancer experiences to adopt six cancer prevention behaviors.
Methods
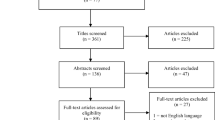
A randomized clinical controlled trial recruited 3,031 patients from Primary Care among cancer patients’ relatives. The experimental group (EG) received four EI, one EI every six months, focused on tobacco, alcohol, diet, weight, sun and work, and based on social cognitive models. The impact of the first three EI was calculated measuring at baseline and 18 months later: (a) The percentage of people with each risk behavior; (b) The score reached in a Total Cancer Behavioral Risk (TCBR) indicator; (c) The Odds Ratios at the post-test.
Results
Five risk behaviors decreased significantly more (p < 0.01) in the EG than in the CG: Smoking (OR = 0.662), drinking (OR = 0.504), diet (OR = 0.542), weight (OR = 0.698), and sun (OR = 0.389). The TCBR indicator also decreased an average of nearly 5 points (28.42 vs. 23.82), significantly more (p < 0.001) in the EG.
Conclusion
Families with cancer experiences changed five cancer risk behaviors when approached in Primary Care with interventions based on social cognitive models.


Similar content being viewed by others
References
Martínez C, Peris R, Sánchez MJ (2002) Epidemiología descriptiva del cáncer en España. Tercer libro blanco de la Oncología en España. FESEO. Ergon, Madrid, pp 1–32
Instituto Nacional de Estadística (2004) INEbase; Defunciones según causa de muerte [online], Madrid. Available from: http://www.ine/inebase/menu3_soc.htm (Accessed 20 September 2006)
Boyle P, Veronesi U, Tubiana M et al (1995) European School of Oncology advisory report to the European Commission for the ‘Europe against cancer programme’ European code against cancer. Eur J Cancer 31(9):1395–1405 (Special Paper)
Boyle P, Autier P, Bartelink H et al (2003) European code against cancer and scientific justification: third version (2003). Ann Oncol 14(7):973–1005
Boyle P, d’Onofrio A, Maisonneuve P et al (2003) Measuring progress against cancer in Europe: has the 15% decline targeted for 2000 come about? Ann Oncol 4(8):1312–1325
Rodríguez F, Gutierrez-Fisac J (2000) El estado de salud y sus determinantes: evaluación de los objetivos 1 a 12. In: Álvarez C, Peiró S (eds) Informe SESPAS 2000: La salud pública ante los desafíos de un nuevo siglo. Escuela Andaluza de Salud Pública, Granada, pp 43–50
Tomatis L (2000) Etiologic evidence and primary prevention of cancer. Drug Metab Rev 32(2):129–137
Rimer BK (2000) Cancer control research 2001. Cancer Causes Control 11(3):257–270
Audrain J, Rimer B, Cella D et al (1999) The impact of a brief coping skills intervention on adherence to breast self-examination among first-degree relatives of newly diagnosed breast cancer patients. Psychooncology 8(3):220–229
Ryan EL, Skinner CS (1999) Risk beliefs and interest in counseling: focus group interviews among first-degree relatives of breast cancer patients. J Cancer Educ 4(2):9–103
Weston R (1999) Intervention and prevention. Eur J Cancer Prev 8(5):373–375
Halverson PK, Mays GP, Rimer BK, Lerman C, Audrain J, Kaluzny AD (1999) Adoption of a health education intervention for family members of breast cancer patients. Am J Prev Med 18(3):189–198
De Vries H, Mudde A, Leijs I et al (2003) The European Smoking Prevention Framework Approach (EFSA): an example of integral prevention. Health Educ Res 18(5):611–626
De Vries H, Lezwijn J, Hol M, Honing C (2005) Skin cancer prevention: behaviour and motives of Dutch adolescents. Eur J Cancer Prev 14(1):39–50
De Vries H, Mesters I, Van de Steeg H, Honing C (2005) The general public’s information needs and perceptions regarding hereditary cancer: an application of the integrated change model. Patient Educ Couns 56(2):154–165
Brug J, Lechner L, De Vries H (1995) Psychosocial determinants of fruit and vegetable consumption. Appetite 25(3):285–296
Oostveen T, Knibbe R, de Vries H (1996) Social influences on young adults’ alcohol consumption: norms, modeling, pressure, socializing, and conformity. Addict Behav 21(2):187–197
Van Wechem SN, Van Assema P, Brug J (1997) Results of a community-based campaign to reduce fat intake. Nutr Health 11(3):207–218
De Vries H, Mudde AN (1998) Predicting stage transitions for smoking cessation applying the attitude-social influence-efficacy model. Psychol Health 13:369–385
De Vries H, Lechner L (2000) Motives for protective against carcinogenic substances in the workplace: a pilot study among Dutch workers. J Occup Environ Med 42(1):88–95
Lopez ML, Herrero P, Comas A et al (2004) Impact of cigarette advertising on smoking behaviour in Spanish adolescents as measured using recognition of billboard advertising. Eur J Public Health 14(4):428–432
Ajzen I (1991) The theory of planned behavior. Organ Behav Hum Decis Process 50 (2):179–211
Bandura A (1977) Self-efficacy—toward a unifying theory of behavioral change. Psychol Rev 84 (2):191–215
Prochaska JO, DiClemente CC (1982) Transtheorical therapy—toward a more integrative model of change. Psycother Theory Res Pract 19 (3):276–288
Glasgow RE, Goldstein MG, Ockene JK, Pronk NP (2004) Translating what we have learned into practice. Principles and hypotheses for interventions addressing multiple behaviors in primary care. Am J Prev Med 27(2 Suppl):88–101
Curry SJ (2004) Toward a public policy agenda for addressing multiple health risk behaviors in primary care. Am J Prev Med 27(2 Suppl):106–108
Pronk NP, Peek CJ, Goldstein MG (2004) Addressing multiple behavioral risk factors in primary care. A synthesis of current knowledge and stakeholder dialogue sessions. Am J Prev Med 27(2 Suppl):4–17
Gotay CC (2005) Behavior and cancer prevention. J Clin Oncol 23(2):301–310
Emmons KM, Stoddard AM, Gutheil C, Suarez EG, Lobb R, Fletcher R (2003) Cancer prevention for working class, multi-ethnic populations through health centers: the healthy directions study. Cancer Causes Control 14(8):727–737
Goldstein MG, Whitlock EP, DePue J (2004) Planning committee of the addressing multiple behavioral risk factors in primary care project. Multiple behavioral risk factor interventions in primary care Summary of research evidence. Am J Prev Med 27(2 Suppl):61–79
Prochaska JO, Velicer WF, Redding C et al (2005) Stage-based expert systems to guide a population of primary care patients to quit smoking, eat healthier, prevent skin cancer, and receive regular mammograms. Prev Med 41(2), 406–416
Emmons KM, McBride CM, Puleo E et al (2005) Project PREVENT: a randomized trial to reduce multiple behavioral risk factors for colon cancer. Cancer Epidem Biomar 14(6):1453–1459
Thompson B, Coronado G, Chen L, Islas I (2006) Celebremos la salud! a community randomized trial of cancer prevention (United States). Cancer Causes Control 7(5):733–746
Ostroff J, Ross S, Steinglass P, Ronis-Tobin V, Singh B (2004) Interest in and barriers to participation in multiple family groups among head and neck cancer survivors and their primary family caregivers. Fam Process 43(2):195–208
Rector TS, Venus PJ, Laine AJ (1999) Impact of mailing information about nonurgent care on emergency department visits by Medicaid beneficiaries enrolled in managed care. Am J Manag Care. 5(12):1505–1512
Wahlberg AC, Cedersund E, Wredling R (2003) Telephone nurses’ experience of problems with telephone advice in Sweden. J Clin Nurs 12(1):37–45
Carney PA, Harwood BG, Greene MA, Goodrich ME (2005) Impact of a telephone counseling intervention on transitions in stage of change and adherence to interval mammography screening (United States). Cancer Causes Control 16(7):799–807
Pieterse ME, Seydel ER, DeVries H, Mudde AN, Kok GJ (2001) Effectiveness of a minimal contact smoking cessation program for Dutch general practitioners: a randomized controlled trial. Prev Med 32(2):182–190
Bolman C, De Vries H, Van Breukelen G (2002) A minimal-contact intervention for cardiac inpatients: long-term effects on smoking cessation. Prev Med 35(2):181–192
Prochaska JO, Velicer WF (1997) The transtheoretical model of health change. Am J Health Promot 12(1):38–48
López ML, García-Cueto E, Fernández JM. Del Valle MO, Cueto A (2003) Validation of a questionnaire to evaluate the attitude towards primary prevention advice from the European Code against cancer. Eur J Cancer Prev 12(2):157–164
López ML, Comas A, Del Valle MO, López S, García JB, Cueto-Espinar A (2004) Psychosocial factors associated with cancer behavioural risk in relatives of cancer patients. Eur J Cancer Prev 13(2):105–111
Carrel AL, Clark RR, Peterson SE, Nemeth BA, Sullivan J, Allen DB (2005) Improvement of fitness, body composition, and insulin sensitivity in overweight children in a school-based exercise program: a randomized, controlled study. Arch Pediat Adol Med 159(10):963–968
Powers AR, Struempler BJ, Guarino A, Parmer SM (2005) Effects of a nutrition education program on the dietary behavior and nutrition knowledge of second-grade and third-grade students. J School Health 75(4):129–133
Rothman RL, Malone R, Bryant B et al (2005) A randomized trial of a primary care-based disease management program to improve cardiovascular risk factors and glycated hemoglobin levels in patients with diabetes. Am J Med 118(3):76–284
Dijkstra A, De Vries H (2000) Subtypes of precontemplating smokers defined by different long-term plans to change their smoking behavior. Health Educ Res 15(4):423–434
Ma J, Betts NM, Horacek T, Georgiou C, White A, Nitzke S (2002) The importance of decisional balance and self-efficacy in relation to stages of change for fruit and vegetable intakes by young adults. Am J Health Promot 16(3):157–166
Brunswick N, Wardle J, Jarvis MJ (2001) Public awareness of warning signs for cancer in Britain. Cancer Causes Control 12(1):33–37
Cohen M (2002) First-degree relatives of breast-cancer patients: cognitive perceptions, coping, and adherence to breast self-examination. Behav Med 28(1):15–22
Abroms L, Jorgensen CM, Southwell BG, Geller AC, Emmons KM (2003) Gender differences in young adults’ beliefs about sunscreen use. Health Educ Behav 30(1):29–43
Hadley DW, Jenkins J, Dimond E et al (2003) Genetic counseling and testing in families with hereditary nonpolyposis colorectal cancer. Arch Intern Med 163(5):573–582
Gonzalez CA, Navarro C, Martinez C et al (2004) The European prospective investigation about cancer and nutrition (EPIC). Rev Esp Salud Publica 78(2):167–176
Milch CE, Edmunson JM, Beshansky JR, Griffith JL, Selker HP (2004) Smoking cessation in primary care: a clinical effectiveness trial of two simple interventions. Prev Med 38(3):284–294
Kapur N, Hunt I, Lunt M, McBeth J, Creed F, Macfarlane G (2005) Primary care consultation predictors in men and women: a cohort study. Brit J Gen Pract 55(511):108–113
Vedsted P, Christensen MB (2005) Frequent attenders in general practice care: a literature review with special reference to methodological considerations. Public Health 119(2):118–137
Weinstock MA, Rossi JS, Redding CA, Maddock JE, Cottrill SD (2000) Sun protection behaviors and stages of change for the primary prevention of skin cancers among beachgoers in southeastern New England. Ann Behav Med 22(4):286–293
Baker AH, Wardle J (2003) Sex differences in fruit and vegetable intake in older adults. Appetite 40(3):269–275
Slattery ML, Kinney AY, Levin TR (2004) Factors associated with colorectal cancer screening in a population-based study: the impact of gender, health care source, and time. Prev Med 38(3):276–283
Nicholson FB, Korman MG (2005) Acceptance of flexible sigmoidoscopy and colonoscopy for screening and surveillance in colorectal cancer prevention. J Med Screen 12(2):89–95
McCann TJ, Criqui MH, Kashani IA et al (1997) A randomized trial of cardiovascular risk factor reduction: patterns of attrition after randomization and during follow-up. J Cardiovasc Risk 4(1):41–46
Acknowledgments
FIS 01/0311 and FICYT FC-02-PC-SPV01-14 grants supported this research. The authors wish to acknowledge: the contribution of the professionals, patients and sanitary authorities of the Principality of Asturias and Cantabria regions; the financial support of the RTICCC and ‘Obra Social Cajastur’.
Author information
Authors and Affiliations
Consortia
Corresponding author
Additional information
From Primary Care centers: Alonso Cortina, Mª Aurora; Alonso Montes, Flor; Álvarez González, Esperanza; Álvarez Gutiérrez, Lourdes; Blanco Diego, Julia; Blas Gutiérrez, Aurora de; Brun Gurpegui, Elisa; Cabañeros Vicente, Juan José; Cadaya Gabás, Mª Nieves; Castañeda García, Esperanza; Chamizo Vega, Carmen; Díez Lamadrid, Mª Josefa; Dorado Campos, Ofelia; Elena Sinobas, Pilar; Esparza Girón, Miguel; Fernández Prieto, Teresa; García Fernández, Ana Margarita; García Mata, Montserrat; Gonzalvo Rodríguez, Covadonga; Hermosa de la Llama, Mª Concepción; Lago García, Carmen Mª; Marín Ortega, Dolores; Plaza Verdesoto, Mª Fernanda; Sáiz Berzosa, Angélica; Sánchez Valles, Emma Rosa; Torre Arrarte, Begoña de la; Zumalacárregui Rodríguez, Mª Jesús. From the University of Oviedo: Martínez Canteli, Alejandra; Miguélez López, Ruth.
Rights and permissions
About this article
Cite this article
López, M.L., Iglesias, J.M., del Valle, M.O. et al. Impact of a primary care intervention on smoking, drinking, diet, weight, sun exposure, and work risk in families with cancer experience. Cancer Causes Control 18, 525–535 (2007). https://doi.org/10.1007/s10552-007-0124-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10552-007-0124-0