Abstract
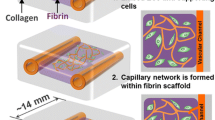
The lack of a simple and effective method to integrate vascular network with engineered scaffolds and tissue constructs remains one of the biggest challenges in true 3D tissue engineering. Here, we detail the use of a commercially available, low-cost, open-source 3D printer modified with a microfluidic print-head in order to develop a method for the generation of instantly perfusable vascular network integrated with gel scaffolds seeded with cells. The print-head features an integrated coaxial nozzle that allows the fabrication of hollow, calcium-polymerized alginate tubes that can be easily patterned using 3D printing techniques. The diameter of the hollow channel can be precisely controlled and varied between 500 μm – 2 mm by changing applied flow rates or print-head speed. These channels are integrated into gel layers with a thickness of 800 μm – 2.5 mm. The structural rigidity of these constructs allows the fabrication of multi-layered structures without causing the collapse of hollow channels in lower layers. The 3D printing method was fully characterized at a range of operating speeds (0–40 m/min) and corresponding flow rates (1–30 mL/min) were identified to produce precise definition. This microfluidic design also allows the incorporation of a wide range of scaffold materials as well as biological constituents such as cells, growth factors, and ECM material. Media perfusion of the channels causes a significant viability increase in the bulk of cell-laden structures over the long-term. With this setup, gel constructs with embedded arrays of hollow channels can be created and used as a potential substitute for blood vessel networks.











Similar content being viewed by others
References
A. Atala et al., Tissue-engineered autologous bladders for patients needing cystoplasty. Lancet 367(9518), 1241–1246 (2006)
R. Attalla, & Selvaganapathy, P., 3D Printing of Gels with Integrated Vascular Channels for Cell Culture using a Microfluidic Printhead. In 18th International Conference on Miniaturized Systems for Chemistry and Life Sciences. (2014)
H. Bae et al., Building vascular networks. Sci. Transl. Med. 4(160), 160 ps23 (2012)
S. Baiguera, D. Ribatti, Endothelialization approaches for viable engineered tissues. Angiogenesis 16(1), 1–14 (2013)
T. Barnes et al., Assessment of the elasticity of erythrocytes in different physiological fluids by laser traps. Optics and Photonics Journal 03(02), 211–216 (2013)
T. a. Becker, D. R. Kipke, Flow properties of liquid calcium alginate polymer injected through medical microcatheters for endovascular embolization. J. Biomed. Mater. Res. 61(4), 533–540 (2002)
H. Bernstein (ed.), Tissue engineering in regenerative medicine (Springer, New York, 2011)
L. E. Bertassoni et al., Hydrogel bioprinted microchannel networks for vascularization of tissue engineering constructs. Lab Chip 14(13), 2202–2211 (2014)
J. Berthier, P. Silberzan (eds.), Microfluidics for biotechnology 2nd ed (Artech House, Norwood, 2010)
S. Beyer, T. Mohamed, & K. Walus, A Microfluidics Based 3D Bioprinter with On-The-Fly Multimaterial Switching capability. In 17th International Conference on Miniaturized Systems for Chemistry and Life Sciences. (2013)
T. Boland et al., Cell and organ printing 2: fusion of cell aggregates in three-dimensional gels. Anat. Rec. A Discov. Mol. Cel.l Evol Biol 272(2), 497–502 (2003)
T. Boland et al., Application of inkjet printing to tissue engineering. Biotechnol. J. 1(9), 910–917 (2006)
P.-T. Brun, et al., Liquid ropes: a geometrical model for thin viscous jets instabilities, (2014) 2–6
O. Cakmak et al., Microcantilever based disposable viscosity sensor for serum and blood plasma measurements. Methods 63(3), 225–232 (2013)
P. Cheetham, K. Blunt, C. Bucke, Physical studies on cell immobilization using calcium alginate gels. Biotechnol. Bioeng. XXI(1979), 2155–2168 (1979)
Y. Chisti, Hydrodynamic damage to animal cells. Crit. Rev. Biotechnol. 21(2), 67–110 (2001)
J. O. Cruickshank, Low-Reynolds-number instabilities in stagnating jet flows. J. Fluid Mech. 193(−1), 111 (1988)
J. O. Cruickshank, B. R. Munson, Viscous fluid buckling of plane and axisymmetric jets. J. Fluid Mech. 113((−1), 221 (1981)
I. Fernandez Farrés, I. T. Norton, Formation kinetics and rheology of alginate fluid gels produced by in-situ calcium release. Food Hydrocoll. 40, 76–84 (2014)
C. Fidkowski et al., Endothelialized microvasculature based on a biodegradable elastomer. Tissue Eng. 11(1–2), 302–309 (2005)
Q. Gao et al., Coaxial nozzle-assisted 3D bioprinting with built-in microchannels for nutrients delivery. Biomaterials 61, 203–215 (2015)
A. Haug, O. Smidsrod, Determination of intrinsic viscosity of alginates. Acta Chem. Scand. 16(7), 1569–1578 (1962)
L. A. Hockaday et al., Rapid 3D printing of anatomically accurate and mechanically heterogeneous aortic valve hydrogel scaffolds. Biofabrication 4(3), 035005 (2012)
K. Jakab et al., Three-dimensional tissue constructs built by bioprinting. Biorheology 43(3–4), 509–513 (2006)
K. Jakab et al., Tissue engineering by self-assembly of cells printed into topologically defined structures. Tissue Eng. A 14(3), 413–421 (2008)
A. Jeanes, J. E. Pittsley, F. R. Senti, Polysaccharide B-1459: a new hydrocolloid polyelectrolyte produced from glucose by bacterial fermentation. J. Appl. Polym. Sci. 5(17), 519–526 (1961)
S. Kim et al., Engineering of functional, perfusable 3D microvascular networks on a chip. Lab Chip 13(8), 1489–1500 (2013)
R. Kohn, Ion binding on polyuronates-alginate and pectin. Biochem. J. 126(2), 371–397 (1972)
C. K. Kuo, P. X. Ma, Ionically crosslinked alginate hydrogels as scaffolds for tissue engineering: part 1. Structure, gelation rate and mechanical properties. Biomaterials 22(6), 511–521 (2001)
K. Y. Lee, D. J. Mooney, Alginate: properties and biomedical applications. Progress in Pol ymer Science (Oxford) 37(1), 106–126 (2012)
K. H. Lee et al., Synthesis of cell-laden alginate hollow fibers using microfluidic chips and microvascularized tissue-engineering applications. Small 5(11), 1264–1268 (2009)
W. Lee et al., On-demand three-dimensional freeform fabrication of multi-layered hydrogel scaffold with fluidic channels. Biotechnol. Bioeng. 105(6), 1178–1186 (2010)
V. K. Lee, D. Y. Kim, et al., Creating perfused functional vascular channels using 3D bio-printing technology. Biomaterials 35(28), 8092–8102 (2014a)
V. K. Lee, A. M. Lanzi, et al., Generation of multi-scale vascular network system within 3D hydrogel using 3D Bio-printing technology. Cell. Mol. Bioeng. 7(3), 460–472 (2014b)
M. A. LeRoux, F. Guilak, L. A. Setton, Compressive and shear properties of alginate gel: effects\nof sodium ions and alginate concentration. J. Biomed. Mater. Res. 47, 46–53 (1999)
T. Majmudar, et al., Nonlinear dynamics of coiling in viscoelastic jets. (2010)
M. S. Mannoor et al., 3D printed bionic ears. Nano Lett. 13(6), 2634–2639 (2013)
G. Matsumura et al., First evidence that bone marrow cells contribute to the construction of tissue-engineered vascular autografts in vivo. Circulation 108(14), 1729–1734 (2003)
A. B. Metzner, J. C. Reed, Flow of Non-newtonian fluids-correlation of the laminar, transition, and turbulent-flow regions. AICHE J. 4, 434–440 (1955)
J. S. Miller et al., Rapid casting of patterned vascular networks for perfusable engineered three-dimensional tissues. Nat. Mater. 11(9), 768–774 (2012)
V. Mironov et al., Organ printing: tissue spheroids as building blocks. Biomaterials 30(12), 2164–2174 (2009)
S. Moe et al., Calcium alginate gel fibers : influence of alginate source and gel structure on fiber strength. J. Appl. Polym. Sci. 51(10), 1771–1775 (1994)
M. Nakamura et al., Biocompatible inkjet printing technique for designed seeding of individual living cells. Tissue Eng. 11(11–12), 1658–1666 (2005)
V. W. Ostwald, Ueber die rechnerische darstellung des strukturgebietes der viskosit it. Kolloid-Zeitschrift 47(2), 176–187 (1928)
L. Pan et al., Viability and differentiation of neural precursors on hyaluronic acid hydrogel scaffold. J. Neurosci. Res. 87(14), 3207–3220 (2009)
J. L. Platt, New directions for organ transplantation. Nature 392(6679 Suppl), 11–17 (1998)
M. Radisic et al., Cardiac tissue engineering using perfusion bioreactor systems. Nat. Protoc. 3(4), 719–738 (2008)
D. Rees, Shapely polysaccharides. Biochem. J. 126(2), 257–273 (1972)
S. J. Shin et al., “On the fly” continuous generation of alginate fibers using a microfluidic device. Langmuir 23(17), 9104–9108 (2007)
B. Subramanian et al., Tissue-engineered three-dimensional in vitro models for normal and diseased kidney. Tissue Eng. A 16(9), 2821–2831 (2010)
C. Tropea, A. Yarin, J. Foss (eds.), Springer handbook of experimental fluid mechanics (Springer Science & Business Media, Berlin, 2007)
C. Wang et al., Endothelial cell sensing of flow direction. Arterioscler. Thromb. Vasc. Biol. 33(9), 2130–2136 (2013)
T. Xu et al., Hybrid printing of mechanically and biologically improved constructs for cartilage tissue engineering applications. Biofabrication 5(1), 015001 (2013)
Y. Yu et al., Evaluation of cell viability and functionality in vessel-like bioprintable cell-laden tubular channels. J. Biomech. Eng. 135(9), 91011 (2013)
I. Zein et al., Fused deposition modeling of novel scaffold architectures for tissue engineering applications. Biomaterials 23(4), 1169–1185 (2002)
Y. Zhang et al., Characterization of printable cellular micro-fluidic channels for tissue engineering. Biofabrication 5(2), 025004 (2013)
Y. Zhang et al., In vitro study of directly bioprinted perfusable vasculature conduits. Biomater. Sci. 3(1), 134–143 (2015)
Acknowledgments
This work has been supported by the NSERC Discovery grant, Canada Research Chairs Program, and Ontario Ministry of Innovation Early Researchers Award. The authors would also like to thank the Biointerfaces Institute for equipment support and the Electron Microscopy Facility for assistance with imaging techniques.
Author information
Authors and Affiliations
Corresponding author
Electronic Supplementary Material
ESM 1
(DOCX 61 kb)
Rights and permissions
About this article
Cite this article
Attalla, R., Ling, C. & Selvaganapathy, P. Fabrication and characterization of gels with integrated channels using 3D printing with microfluidic nozzle for tissue engineering applications. Biomed Microdevices 18, 17 (2016). https://doi.org/10.1007/s10544-016-0042-6
Published:
DOI: https://doi.org/10.1007/s10544-016-0042-6