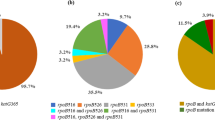
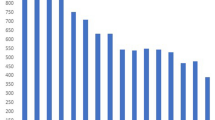
DNA sequencing analysis was used to investigate genetic alterations in the rpoB, katG, and inhA regulatory region and embB in 66 Mycobacterium tuberculosis isolates recovered from Central China. Of the 36 multidrug-resistant isolates, 33 (92%) had mutations in the amplified region of rpoB. The most frequent mutation (58%, 19/36) was S531L (TCG→TTG). At least one mutation was found in the katG and inhA regulatory region in 83% (30/36) of the multidrug-resistant isolates, and mutations at katG codon 315 were identified in 78% (28/36). Alterations at embB306 may not confer resistance to EMB, and embB306 mutants were more frequently accompanied by rpoB mutations (100%, 16/16) than by katG 315 mutations (75%, 12/16). Our results show that geographic variation in the molecular genetic mechanism is responsible for drug resistance in multidrug-resistant M. tuberculosis. This observation will facilitate the development of a rapid molecular drug resistance screening approach for drug-resistant M. tuberculosis.
Similar content being viewed by others
REFERENCES
Banerjee, A., Dubnau, E., Quemard, A., Balasubramanian, V., Um, K. S., Wilson, T., Collins, D., de Lisle, G., and Jacobs W. R., Jr. (1994). inhA, a gene encoding a target for isoniazid and ethionamide in Mycobacterium tuberculosis. Science 263:227–230.
Caugant, D. A., Sandven, P., Eng, J., Jeque, J. T., and Tonjum, T. (1995). Detection of rifampin resistance among isolates of Mycobacterium tuberculosis from Mozambique. Microb. Drug Resist. 1:321–326.
Chaves, F., Alonso-Sanz, M., Rebollo, M. J., Tercero, J. C., Jimenez, M. S., and Noriega, A. R. (2000). rpoB mutations as an epidemiologic marker in rifampin-resistant Mycobacterium tuberculosis. Int. J. Tuberc. Lung. Dis. 4:765–770.
Coll, P., Aragon, L. M., Alcaide, F., Espasa, M., Garrigo, M., Gonzalez, J., Manterola, J. M., Orus, P., and Salvado, M. (2005). Molecular analysis of isoniazid and rifampin resistance in Mycobacterium tuberculosis isolates recovered from Barcelona. Microb. Drug Resist. 11:107–114.
Dye, C., Scheele, S., Dolin, P., Pathania, V., and Raviglione, M. C. (1999). Global burden of tuberculosis: Estimated incidence, prevalence, and mortality by country. WHO global surveillance and monitoring project. JAMA 282:677–686.
Goble, M., Iseman, M. D., Madsen, L. A., Waite, D., Ackerson, L., and Horsburgh C. R., Jr. (1993). Treatment of 171 patients with pulmonary tuberculosis resistant to isoniazid and rifampin. N. Engl. J. Med. 328:527–532.
Herrera, L., Valverde, A., Saiz, P., Porterob, J. L., Jiménez, M. S. (2004). Molecular characterization of isoniazid-resistant Mycobacterium tuberculosis clinical strains isolated in the Philippines. Intern. J. Antimicrob. Agents 23:572–576.
Hillemann, D., Kubica, T., Rüsch-Gerde, S., Niemann, S. (2005). Disequilibrium in distribution of resistance mutations among Beijing and non-Beijing Mycobacterium tuberculosis strains isolated from patients resident in Germany. Antimicrob. Agents Chemother. 49:1229–1231.
Hazbon, M. H., Bobadilla del Valle, M., Guerrero, M. I., Varma-Basil, M., Filliol, I., Cavatore, M., Colangeli, R., Safi, H., Billman-Jacobe, H., Lavender, C., Fyfe, J., Garcia-Garcia, L., Davidow, A., Brimacombe, M., Leon, C. I., Porras, T., Bose, M., Chaves, F., Eisenach, K. D., Sifuentes-Osornio, J., Ponce de Leon, A., Cave, M. D., and Alland, D. (2005). Role of embB codon 306 mutations in Mycobacterium tuberculosis revisited: A novel association with broad drug resistance and IS6110 clustering rather than ethambutol resistance. Antimicrob. Agents Chemother. 49:3794–3802.
Jin, D. J., and Gross, C. A. (1988). Mapping and sequencing of mutations in the Ecsherichia coli rpoB gene that lead to rifampicin esistance. J. Mol. Biol. 202:45–58.
Kapur, V., Li, L. L., Iordanescu, S., Hamrick, M. R., Wanger, A., Kreiswirth, B. N., and Musser, J. M. (1994). Characterization by automated DNA sequencing of mutations in the gene (rpoB) encoding the RNA polymerase ß subunit in rifampin-resistant Mycobacterium tuberculosis strains from New York City and Texas. J. Clin. Microbiol. 32:1095–1098.
Khoo, K. H., Douglas E., Azadi P., Inamine J. M., Besra G. S., Mikusova K., Brennan P. J., and Chatterjee D. (1996). Truncated structural variants of lipoarabinomannan in ethambutol drug-resistant strains of Mycobacterium smegmatis: Inhibition of arabinan biosynthesis by ethambutol. J. Biol. Chem. 271:28682–28690.
Khoo, K. H., Tang J. B., and Chatterjee D. (2001). Variation in mannose-capped terminal arabinan motifs of lipoarabinomannans from clinical isolates of Mycobacterium tuberculosis and Mycobacterium avium complex. J. Biol. Chem. 276:3863–3871.
Lee, A. S., Othman, S. N., Ho, Y. M., and Wong, S. Y. (2004). Novel mutations within the embB gene in ethambutol-susceptible clinical isolates of Mycobacterium tuberculosis. Antimicrob. Agents Chemother. 48:4447–4449.
Mokrousov, I., Otten T., Vyshnevskiy B., and Narvskaya O. (2002). Detection of embB306 mutations in ethambutol-susceptible clinical isolates of Mycobacterium tuberculosis from northwestern Russia: Implications for genotypic resistance testing. J. Clin. Microbiol. 40:3810–3813.
Parsons, L. M., Salfinger, M., Clobridge, A., Dormandy, J., Mirabello, L., Polletta, V. L., Sanic, A., Sinyavskiy, O., Larsen, S. C., Driscoll, J., Zickas, G., and Taber, H. W. (2005). Phenotypic and molecular characterization of Mycobacterium tuberculosis isolates resistant to both isoniazid and ethambutol. Antimicrob. Agents Chemother. 49:2218–2225.
Peng, Y. L., Wang, G. B., Zhang, S. L., Wu, X. Q., Gao, S. Y., Zhang, L., and Sun, Z. Q. (2000). Detection of the rpsL mutation for streptomycin-resistant Mycobacterium uberculosis. Chin. J. Lab. Med. 23:148–149.
Qian, L., Abe, C., Lin, T. P., Yu, M. C., Cho, S. N., Wang, S., and Douglas, J. T. (2002). rpoB genotypes of Mycobacterium tuberculosis Beijing family isolates from East Asian countries. J. Clin. Microbiol. 40:1091–1094.
Ramaswamy, S., and Musser, J. M. (1998). Molecular genetic basis of antimicrobial agent resistance in Mycobacterium tuberculosis: 1998 update. Tuber. Lung Dis. 79:3–29.
Rinder, H., Dobner, P., Feldmann, K., Rifai, M., Bretzel, G., Rüsch-Gerdes, S., and Loscher, T. (1997). Disequilibria in the distribution of rpoB alleles in rifampicin-resistant M. tuberculosis isolates from Germany and Sierra Leone. Microb. Drug Resist. 3:195–197.
Rinder, H., Mieskes, K. T., Tortoli, E., Richter, E., Casal, M., Vaquero, M., Cambau, E., Feldmann, K., Loscher, T. (2001). Detection of embB codon 306 mutations in ethambutol resistant Mycobacterium tuberculosis directly from sputum samples: A low-cost, rapid approach. Mol. Cell. Probes. 15:37–42.
Suarez, P. G., Floyd, K., Portocarrero, J., Alarcon, E., Rapiti, E., Ramos, G., Bonilla, C., Sabogal, I., Aranda, I., Dye, C., Raviglione, M., and Espinal, M. A. (2002). Feasibility and cost-effectiveness of standardised second-line drug treatment for chronic tuberculosis patients: A national cohort study in Peru. Lancet 359:1980–1989.
Telenti, A., Honoré, N., Bernasconi, C., March, J., Ortega, A., Heym, B., Takiff, H. E., and Cole, S. T. (1997). Genotypic assessment of isoniazid and rifampin resistance in Mycobacterium tuberculosis: A blind study at reference laboratory level. J. Clin. Microbiol. 35:719–723.
Zhang, S. L., Wu, X. Q., and Zu, Y. (2000). Detection of katG mutations in isoniazid-resistant Mycobacterium tuberculosis strains by polymerase chain reaction-single strand conformational polymorphism. Chin. J. Health Lab Tech. 10:185–187.
ACKNOWLEDGMENTS
This study was supported by Grant No. 971200100 from Henan Key Scientific and Technological Project, China. We thank Zhan-Qiang Sun for excellent technical assistance in identification of Mycobacteria, and also thank Bing-Xiang Tang for helpful suggestions.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zhang, SL., Qi, H., Qiu, DL. et al. Genotypic Analysis of Multidrug-Resistant Mycobacterium tuberculosis Isolates Recovered From Central China. Biochem Genet 45, 281–290 (2007). https://doi.org/10.1007/s10528-006-9074-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10528-006-9074-6