Abstract
Background
Microfinance interventions have the potential to improve HIV treatment outcomes, but the mechanisms through which they operate are not entirely clear.
Objectives
To construct a synthesizing conceptual framework for the impact of microfinance interventions on HIV treatment outcomes using evidence from our systematic review.
Methods
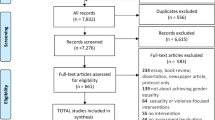
We conducted a systematic review by searching electronic databases and journals from 1996 to 2018 to assess the effects of microfinance interventions on HIV treatment outcomes, including adherence, retention, viral suppression, and CD4 cell count.
Results
All studies in the review showed improved adherence, retention, and viral suppression, but varied in CD4 cell count following participation in microfinance interventions—overall supporting microfinance’s positive role in improving HIV treatment outcomes. Our synthesizing conceptual framework identifies potential mechanisms through which microfinance impacts HIV treatment outcomes through hypothesized intermediate outcomes.
Conclusion
Greater emphasis should be placed on assessing the effect mechanisms and intermediate behaviors to generate a sound theoretical basis for microfinance interventions.
Resumen
Antecedentes
Las intervenciones de microfinanzas tienen el potencial de mejorar los resultados del tratamiento del VIH, pero los mecanismos a través de los cuales operan no están del todo claros.
Objetivos
Construir un marco conceptual de síntesis del impacto de las intervenciones de microfinanzas en los resultados del tratamiento del VIH utilizando evidencia de una revisión sistemática.
Métodos
Se llevó a cabo una revisión sistemática mediante búsquedas en bases de datos electrónicas y revistas desde 1996 hasta 2018 para evaluar los efectos de las intervenciones de microfinanzas en los resultados del tratamiento del VIH, incluida la adherencia, la retención, la supresión viral y el recuento de células CD4.
Resultados
Todos los estudios en la revisión mostraron una mejor adherencia, retención y supresión viral, pero variaron en el recuento de células CD4 luego de la participación en las intervenciones de microfinanzas, lo que respalda el papel positivo de las microfinanzas en la mejora de los resultados del tratamiento del VIH. El marco conceptual de síntesis propuesto identifica los mecanismos potenciales a través de los cuales las microfinanzas impactan los resultados del tratamiento del VIH a través de resultados intermedios hipotéticos.
Conclusión
Se debe poner mayor énfasis en evaluar los mecanismos de efecto y los comportamientos intermedios para generar una base teórica sólida para las intervenciones de microfinanzas.

Similar content being viewed by others
References
Gupta GR, Parkhurst JO, Ogden JA, Aggleton P, Mahal A. Structural approaches to HIV prevention. Lancet (London, England). 2008;372(9640):764–75. https://doi.org/10.1016/S0140-6736(08)60887-9.
Gitahi-Kamau NT, Kiarie JN, Mutai KK, Gatumia BW, Gatongi PM, Lakati A. Socio-economic determinants of disease progression among HIV infected adults in Kenya. BMC Public Health. 2015;15:733. https://doi.org/10.1186/s12889-015-2084-8.
Witte SS, Aira T, Tsai LC, et al. Efficacy of a savings-led microfinance intervention to reduce sexual risk for HIV among women engaged in sex work: a randomized clinical trial. Am J Public Health. 2015;105(3):e95–102. https://doi.org/10.2105/AJPH.2014.302291.
MacPherson E, Desmond N, Mwapasa V, Lalloo DG, Seeley J, Theobald S. Exploring the complexity of microfinance and HIV in fishing communities on the shores of Lake Malawi. Malawi-Liverpool-Wellcome Trust Clin Res Program. 2015;30096(3):414–36.
Swann M. AIDS Care Psychological and Socio-medical Aspects of AIDS/HIV Economic strengthening for retention in HIV care and adherence to antiretroviral therapy: a review of the evidence Economic strengthening for retention in HIV care and adherence to antiretroviral therapy: a review of the evidence. AIDS Care. 2018;30(S3):99–125. https://doi.org/10.1080/09540121.2018.1479030org/10.1080/09540121.2018.1479030.
Defining Adherence. 2003. http://www.who.int/chp/knowledge/publications/adherence_Section1.pdf. Accessed 30 Sept 2018.
Scientific Journals Related to HIV/AIDS. American Psychological Association. 2018. https://www.apa.org/pi/aids/resources/research/journals.aspx. Accessed 17 oCT 2018.
Arrivillaga M, Salcedo JP, Pérez M. The IMEA project: an intervention based on microfinance, entrepreneurship, and adherence to treatment for women with HIV/AIDS living in poverty. AIDS Educ Prev. 2014;26(5):398–410. https://doi.org/10.1521/aeap.2014.26.5.398.
Bezabih T, Weiser SD, Menbere MS, Negash A, Grede N. Comparison of treatment adherence outcome among PLHIV enrolled in economic strengthening program with community control. AIDS Care. 2018. https://doi.org/10.1080/09540121.2017.1371667.
Daigle GT, Jolly PE, Chamot EAM, et al. System-level factors as predictors of adherence to clinical appointment schedules in antiretroviral therapy in Cambodia. AIDS Care. 2015. https://doi.org/10.1080/09540121.2015.1024098
Muñoz M, Bayona J, Sanchez E, et al. Matching social support to individual needs: a community- based intervention to improve HIV treatment adherence in a resource-poor setting. AIDS Behav. 2010;15:1454–64. https://doi.org/10.1007/s10461-010-9697-9.
Weiser SD, Bukusi EA, Steinfeld RL, et al. Shamba Maisha: randomized controlled trial of an agricultural and finance intervention to improve HIV health outcomes. AIDS. 2015;29(14):1889–94. https://doi.org/10.1097/QAD.0000000000000781.
Petrovic K, Blank TO. The Andersen-Newman Behavioral Model of Health Service Use as a conceptual basis for understanding patient behavior within the patient-physician dyad: the influence of trust on adherence to statins in older people living with HIV and cardiovascular disease. Cogent Psychol. 2015;2:1038894. https://doi.org/10.1080/23311908.2015.1038894.
Weiser SD, Young SL, Cohen CR, et al. Conceptual framework for understanding the bidirectional links between food insecurity and HIV/AIDS. Am J Clin Nutr. 2011;94(6):1729S–39S. https://doi.org/10.3945/ajcn.111.012070.
Kenya Country Operational Plan (COP) 2018 Strategic Direction Summary. 2018. https://www.pepfar.gov/documents/organization/285861.pdf. Accessed 16 Feb 2019.
Ethiopia Country/Regional Operational Plan (COP/ROP) 2018 Strategic Direction Summary.; 2018. https://www.pepfar.gov/documents/organization/285863.pdf. Accessed 16 Feb 2019.
Strategic Direction Summary Cambodia Country Operational Plan. https://www.pepfar.gov/documents/organization/272005.pdf. Accessed 4 Sept 2018.
Vargas V. The New HIV/AIDS Program in Peru: The Role of Prioritizing and Budgeting for Results.; 2015. https://openknowledge.worldbank.org/bitstream/handle/10986/21497/942600WP00PUBL0IV0AIDS0Program0Peru.pdf?sequence=1&isAllowed=y. Accessed 4 Sept 2018.
MLHW Country Case Studies. http://www.who.int/workforcealliance/knowledge/resources/MLHWCountryCaseStudies_annex12_Peru.pdf. Accessed 4 Sept 2018.
HIV and AIDS Estimates Country Factsheets Colombia 2017. 2017.
Behavioral Economics and Social Policy Designing Innovative Solutions for Programs Supported by the Administration for Children and Families. 2014. http://www.acf.hhs.gov/programs/opre. Accessed 4 Sept 2018.
Prevent HIV, Test and Treat All: WHO Support for Country Impact. Geneva. 2016. http://apps.who.int/iris/bitstream/handle/10665/251713/WHOHIV?sequence=1. Accessed 1 Jan 2019.
Alonzo AA, Reynolds NR. Stigma, HIV and AIDS: an exploration and elaboration of a stigma trajectory. 1995. https://ac.els-cdn.com/0277953694003846/1-s2.0-0277953694003846-main.pdf?_tid=793d4d1d-1d00-434c-8365-d831014fe366&acdnat=1538531643_9d3961e1458c3d921f9deb6b784cd6c7. Accessed 2 Oct 2018.
Katz IT, Ryu AE, Onuegbu AG, et al. Impact of HIV-related stigma on treatment adherence: systematic review and meta-synthesis. J Int AIDS Soc. 2013. https://doi.org/10.7448/ias.16.3.18640.
Govindasamy D, Ford N, Kranzer K. Risk factors, barriers and facilitators for linkage to antiretroviral therapy care. AIDS. 2012;26(16):2059–67. https://doi.org/10.1097/QAD.0b013e3283578b9b.
Mullainathan S, Krishnan S. Psychology and economics: what it means for microfinance. 2008. www.financialaccess.orgwww.poverty-action.org. Accessed 25 July 2018.
Baird SJ, Garfein RS, Mcintosh CT, Özler B. Effect of a cash transfer programme for schooling on prevalence of HIV and herpes simplex type 2 in Malawi: a cluster randomised trial. Lancet. 2012;379:1320–9. https://doi.org/10.1016/S0140.
Weiser SD, Hatcher AM, Hufstedler LL, et al. Changes in health and antiretroviral adherence among HIV-infected adults in Kenya: qualitative longitudinal findings from a livelihood intervention. AIDS Behav. 2017;21(2):415–27. https://doi.org/10.1007/s10461-016-1551-2.
Gnauck K, Ruiz J, Kellett N, et al. Economic empowerment and AIDS-related stigma in rural Kenya: a double-edged sword? Cult Heal Sex An Int J Res Interv Care. 2013;15(7):851–65. https://doi.org/10.1080/13691058.2013.789127.
Kim JC, Watts CH, Hargreaves JR, et al. Understanding the impact of a microfinance-based intervention on women’s empowerment and the reduction of intimate partner violence in South Africa. Am J Public Health. 2007;97(10):1794–802. https://doi.org/10.2105/AJPH.2006.095521.
Bertrand M, Mullainathan S, Shafir E. A Behavioral-Economics View of Poverty. Am Econ Assoc Pap Proc. 2004;94(2):419–23. https://doi.org/10.1257/0002828041302019.
Ashraf N, Karlan D, Yin W. Tying Odysseus to the mast: evidence from a commitment savings product in the Philippines. Q J Econ. 2006;121:635–72.
Dworkin SL, Blankenship K. Microfinance and HIV/AIDS prevention: assessing its promise and limitations. AIDS Behav. 2009;13:462–9. https://doi.org/10.1007/s10461-009-9532-3.
Kodongo O, Kendi LG. Individual lending versus group lending: an evaluation with Kenya’s microfinance data. Rev Dev Financ. 2013;3:99–108. https://doi.org/10.1016/j.rdf.2013.05.001.
Holmes K, Winskell K, Hennink M, Chidiac S. Microfinance and HIV mitigation among people living with HIV in the era of anti-retroviral therapy: Emerging lessons from Côte d’Ivoire. Glob Public Health. 2010. https://doi.org/10.1080/17441692.2010.515235.
Hashemi SM, Schuler SR, Riley AP. Rural credit programs and women’s empowerment in Bangladesh. World Dev. 1996;24(4):635–53.
Morduch J. The Microfinance Promise. J Econ Lit. 1999;37:1569–614. https://doi.org/10.1257/jel.37.4.1569.
Pronyk PM, Kim JC, Makhubele MB, et al. Microfinance and HIV prevention—emerging lessons from rural South Africa. Small Enterp Dev. 2005;16(3):26–38.
Mohindra K, Haddad S, Narayana D. Can microcredit help improve the health of poor women? Some findings from a cross-sectional study in Kerala, India. Int J Equity Health. 2008;7:2. https://doi.org/10.1186/1475-9276-7-2.
Ahmed SM, Chowdhury M. Micro-Credit and Emotional Well-Being: Experience of Poor Rural Women from Matlab, Bangladesh. World Dev. 2001;29(11):1957–66.
Fernald LC, Hamad R, Karlan D, Ozer EJ, Zinman J. Small individual loans and mental health: a randomized controlled trial among South African adults. BMC Public Health. 2008. https://doi.org/10.1186/1471-2458-8-409.
Berg KM, Arnsten JH. Practical and conceptual challenges in measuring antiretroviral adherence. J Acquir Immune Defic Syndr. 2006;43(Suppl 1):S79–87. https://doi.org/10.1097/01.qai.0000248337.97814.66.
Acknowledgements
This paper was partially funded by the U.S. National Institutes of Health (NIH) Grants (R21-AI-118393; R34-MH-114664; K01MH099966; P2C-HD-041020). This work was facilitated by the Providence/Boston Center for AIDS Research, CFAR (P30-AI-042853).
Funding
This paper was partially funded by National Institutes of Health (NIH) Grants (R21-AI-118393; R34-MH-114664; K01MH099966).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical Approval
This review article does not contain any research with human participants or animals performed directly by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Nadkarni, S., Genberg, B. & Galárraga, O. Microfinance Interventions and HIV Treatment Outcomes: A Synthesizing Conceptual Framework and Systematic Review. AIDS Behav 23, 2238–2252 (2019). https://doi.org/10.1007/s10461-019-02443-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10461-019-02443-6