Abstract
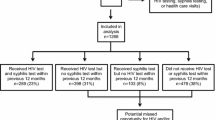
HIV testing is the first step to the fulfillment of Treat as Prevention (TasP) and reaching the 90-90-90 goal in HIV control. However, there are still a large number of Men who have Sex with Men (MSM) have never been tested for HIV before, and little is known about the HIV incidence and care linkage among this population. A Mixed method was used to recruit MSM who had never tested for HIV before from January 2012 to December 2014 in Shenyang, China. Potential MSM participants were invited to attend the enrollment for HIV and syphilis testing at a general hospital-based voluntary counseling and test (VCT). HIV confirmed positive subjects were further tested by BED HIV-1 capture enzyme immunoassay (BED-CEIA) to determine the HIV incidence. Syphilis was screened by the rapid plasma reagent test (RPR) and confirmed by Treponema pallidum particle assay (TPPA). All the HIV positive subjects were referred to the local Center for Disease Control and Prevention (CDC) and clinics for HIV primary care and follow-ups. In total 646 HIV first-time-testers of MSM (FMSM) attended this study, 73.4% (474/646) were aged under 31-year-old and 57.3% (370/646) and used the Internet as their major cruising avenue for seeking male sexual partners. The average prevalence of HIV and current syphilis infection was 10.8% (70/646) and 11.0% (71/646), respectively. The HIV incidence was 10.3 (95% confidence interval [CI] 6.1–14.5)/100PY. Multivariate logistic analysis showed that factors such as use of the Internet as the major cruising avenue (adjusted OR [AOR] 2.7, 95% CI 0.9–7.6) and having a current syphilis infection (AOR 4.2, 95% CI 1.8–12.2) were independent correlates of a recent HIV infection. Of the 95 HIV screening test positive FMSM, 73.7% (70/95) returned and be confirmed positive, 92.9% (65/70) of confirmed patients were linked to care. Among those retained and underwent CD4+ T cell test, 76.3% (42/55) started HIV antiretroviral therapy. Among the unconfirmed, 84.0% (21/25) were non-local migrants. The HIV incidence of FMSM in Shenyang was high. Future HIV testing program needs to keep on expanding among the MSM who have never been tested for HIV yet. The Internet-based campaigns and syphilis testing and treatment could represent an opportunity to get access to this hard-to-reach population and link them to HIV care. Future linkage to HIV care of this population should underscore the usage of HIV rapid diagnostic tests to prevent lost at early steps of linkage.


Similar content being viewed by others
References
Cohen MS, Chen YQ, McCauley M, et al. Prevention of HIV-1 infection with early antiretroviral therapy. N Engl J Med. 2011;365(6):493–505.
Gardner EM, McLees MP, Steiner JF, Del Rio C, Burman WJ. The spectrum of engagement in HIV care and its relevance to test-and-treat strategies for prevention of HIV infection. Clin Infectious Dis. 2011;52(6):793–800.
UNAIDS. AIDS by the numbers 2016. Availabe at http://www.aidsdatahub.org/sites/default/files/highlight-reference/document/UNAIDS_AIDS_by_the_numbers_2016.pdf. Accessed 14 Mar 2017
McLaughlin K. HIV infections are spiking among young gay Chinese. Science. 2017;355(6332):1359.
Zhang BCLX, Shi TX. A primary extimation of the number of population and HIV prevalence in homosexual and bisexual men in China. Chin J AIDS STD. 2002;8(8):197–9.
Zou H, Hu N, Xin Q, Beck J. HIV testing among men who have sex with men in China: a systematic review and meta-analysis. AIDS Behav. 2012;16(7):1717–28.
Qin Q, Tang W, Ge L, Li DM, Mahapatra T, Wang LY, et al. Changing trend of HIV, syphilis and Hepatitis C among men who have sex with men in China. Sci Rep. 2016;. doi:10.1038/srep31081.
Bai X, Xu J, Yang J, Yang B, Yu M, Gao Y, et al. HIV prevalence and high-risk sexual behaviours among MSM repeat and first-time testers in China: implications for HIV prevention. J Int AIDS Soc. 2014;17:18848.
Liu Y, Qian HZ, Ruan Y, Wu P, Osborn CY, Jia Y, et al. Frequent HIV testing: impact on HIV risk among chinese men who have sex with men. J Acquir Immune Defic Syndr. 2016;72(4):452–61.
Gao L, Zhang L, Jin Q. Meta-analysis: prevalence of HIV infection and syphilis among MSM in China. Sex Transm Infect. 2009;85(5):354–8.
Chow EP, Wilson DP, Zhang L. HIV and syphilis co-infection increasing among men who have sex with men in China: a systematic review and meta-analysis. PLoS ONE. 2011;6(8):e22768.
Wu Z, Xu J, Liu E, Mao Y, Xiao Y, Sun X, et al. HIV and syphilis prevalence among men who have sex with men: a cross-sectional survey of 61 cities in China. Clin Infect Dis. 2013;57(2):298–309.
Zhou Y, Li D, Lu D, Ruan Y, Qi X, Gao G. Prevalence of HIV and syphilis infection among men who have sex with men in China: a meta-analysis. Biomed Res Int. 2014;. doi:10.1155/2014/620431.
Peterman TA, Su J, Bernstein KT, Weinstock H. Syphilis in the United States: on the rise? Expert Rev Anti-Infect Ther. 2015;13(2):161–8.
Pan S, Xu J-J, Han X-X, Zhang J, Hu Q-H, Chu Z-X, et al. Internet-based sex-seeking behavior promotes HIV infection risk: a 6-year serial cross-sectional survey to MSM in Shenyang, China. Biomed Res Int. 2016;. doi:10.1155/2016/2860346.
Communique of the National Bureau of Statistics of People’s Republic of China on Major Figures of the 2010 Population Census. Available at http://www.stats.gov.cn/enGliSH/. Accessed 15 Mar 2017.
Xiao Y, Sun JP, Li CM, Lu F, Allen KL, Vermund SH, et al. Prevalence and correlates of HIV and syphilis infections among men who have sex with men in seven provinces in China with historically low hiv prevalence. JAIDS. 2010;. doi:10.1097/QAI.0b013e3181c7db43.
Xu JJ, Zhang M, Brown K, Reilly K, Wang HL, Hu QH, et al. Syphilis and HIV seroconversion among a 12-month prospective cohort of men who have sex with men in Shenyang, China. Sex Transmitted Dis. 2010;37(7):432–9.
Yang X, Zhang Y, Wang X, Fang R Gu Y, Tan X (2013) Analysis of characteristics of 936 HIV voluntary testing and counseling visitors in Shenyang. Practical Prevent Med 3.
China Center of Disease Control and Prevention. Update on the AIDS/STD epidemic in China and main response in control and prevention in December, 2015. Chin J AIDS STD. 2016;22(2):69.
Parekh BS, Kennedy MS, Dobbs T, et al. Quantitative detection of increasing HIV type 1 antibodies after seroconversion: a simple assay for detecting recent HIV infection and estimating incidence. AIDS Res Hum Retroviruses. 2002;18(4):295–307.
Hargrove JW, Humphrey JH, Mutasa K, Parekh BS, McDougal JS, Ntozini R. Improved HIV-1 incidence estimates using the BED capture enzyme immunoassay. AIDS (London, England). 2008;22(4):511–8.
Xu J, Wang H, Jiang Y, et al. Application of the BED capture enzyme immunoassay for HIV incidence estimation among female sex workers in Kaiyuan City, China, 2006-2007. Int J Infect Dis. 2010;14(7):e608–12.
Li SW, Zhang XY, Li XX, Wang MJ, Li DL, Ruan YH, et al. Detection of recent HIV-1 infections among men who have sex with men in Beijing during 2005–2006. Chin Med J. 2008;121(12):1105–8.
Chen Q, Li Y, Su X, Hao M, Lu H, He X. Epidemiological analysis on recent infected HIV-1 patients among newly reported HIV cases in Beijing, from 2009 to 2011. Chin J Epidemiol. 2014;35(1):53–6.
Han M, Feng LG, Yan J, Shen S, Ling H, Ding XB, et al. Surveillance on HIV-1 incidence among men who have sex with men in Chongqing, China, 2006–2008. Chin J Epidemiol. 2009;30(9):878–81.
Center for Disease Control and Prevention. Interim recommendations for the use of the BED capture enzyme immunoassay for incidence estimation and surveillance. Atlanta, GA. 2006. Availabe at https://www.cdc.gov/globalAIDS/docs/surveillance/Interim%20Recommendations%20for%20the%20use%20of%20the%20BED%20capture%20enzyme%20immunoassay%20for%20incidence%20estimation%20and%20surveillance%20Approved%20November%2021%202006%20(2).pdf. Accessed 14 Mar 2017.
UNAIDS (2006) Reference Group on estimates, modelling and projections–statement on the use of the BED assay for the estimation of HIV-1 incidence for surveillance or epidemic monitoring. Weekly Epidemiol Rec 81(4):40.
McFarland W, Busch MP, Kellogg TA, et al. Detection of early HIV infection and estimation of incidence using a sensitive/less-sensitive enzyme immunoassay testing strategy at anonymous counseling and testing sites in San Francisco. JAIDS. 1999;22(5):484–9.
Stall R, Duran L, Wisniewski SR, Friedman MS, Marshal MP, McFarland W, et al. Running in place: implications of HIV incidence estimates among urban men who have sex with men in the United States and other industrialized countries. AIDS Behav. 2009;13(4):615–29.
Li HM, Peng RR, Li J, et al. HIV incidence among men who have sex with men in China: a meta-analysis of published studies. PLoS ONE. 2011;6(8):e23431.
Yang L, Yang C, Jiang Y, Luo H, Chen M, Chen H, et al. The survey on HIV-1 incidence among drug users and men who have sex with men in Yunnan, China. Chin J Dermatovenereol. 2015;29(8):817–9.
Xu JJ, Zhang M, Brown K, et al. Syphilis and HIV seroconversion among a 12-month prospective cohort of men who have sex with men in Shenyang, China. Sex Transm Dis. 2010;37(7):432–9.
Patel P, Borkowf CB, Brooks JT, Lasry A, Lansky A, Mermin J. Estimating per-act HIV transmission risk: a systematic review. AIDS (London, England). 2014;28(10):1509–19.
Marcus U, Gassowski M, Drewes J. HIV risk perception and testing behaviours among men having sex with men (MSM) reporting potential transmission risks in the previous 12 months from a large online sample of MSM living in Germany. BMC Public Health. 2016;. doi:10.1186/s12889-016-3759-5.
Shang H, Xu J, Han X, Spero Li J, Arledge KC, Zhang L. HIV prevention: bring safe sex to China. Nature. 2012;485(7400):576–7.
Lipsitz MC, Segura ER, Castro JL, Smith E, Medrano C, Clark JL, et al. Bringing testing to the people—benefits of mobile unit HIV/syphilis testing in Lima, Peru, 2007–2009. Int J STD AIDS. 2014;25(5):325–31.
Young SD, Cumberland WG, Nianogo R, Menacho LA, Galea JT, Coates T. The HOPE social media intervention for global HIV prevention in Peru: a cluster randomised controlled trial. The lancet HIV. 2015;2(1):e27–32.
Swendeman D, Rotheram-Borus MJ. Innovation in sexually transmitted disease and HIV prevention: internet and mobile phone delivery vehicles for global diffusion. Curr Opin Psychiatr. 2010;23(2):139–44.
Liu C, Mao J, Wong T, Tang W, Tso LS, Tang S, et al. Comparing the effectiveness of a crowdsourced video and a social marketing video in promoting condom use among Chinese men who have sex with men: a study protocol. BMJ Open. 2016;6(10):e010755.
Burchell AN, Allen VG, Gardner SL, Moravan V, Tan DH, Grewal R, et al. High incidence of diagnosis with syphilis co-infection among men who have sex with men in an HIV cohort in Ontario, Canada. BMC Infect Dis. 2015;20(15):356.
Jansen K, Thamm M, Bock CT, Scheufele R, Kucherer C, Muenstermann D, et al. High prevalence and high incidence of coinfection with Hepatitis B, Hepatitis C, and syphilis and low rate of effective vaccination against Hepatitis B in HIV-positive men who have sex with men with known date of HIV seroconversion in Germany. PLoS ONE. 2015;10(11):e0142515.
Guidelines for the management of sexually transmitted infections. World Health Organization. 2003.
Bien CH, Muessig KE, Lee R, Lo EJ, Yang LG, Yang B, et al. HIV and syphilis testing preferences among men who have sex with men in South China: a qualitative analysis to inform sexual health services. PLoS ONE. 2015;. doi:10.1371/journal.pone.0124161.
Zhang N, Bussell S, Wang G, Zhu X, Yang X, Huang T, et al. Disparities in HIV care along the path from infection to viral suppression: a cross-sectional study of HIV/AIDS patient records in 2013, Shandong Province, China. Clin Infect Dis. 2016;63(1):115–21.
Hall HI, Frazier EL, Rhodes P, et al. Differences in human immunodeficiency virus care and treatment among subpopulations in the United States. JAMA Int Med. 2013;173(14):1337–44.
Qin QQ, Guo W, Wang LY, et al. The characteristics of HIV-positive men who have sex with men in China and predictors of their migration, 2008–2015. Chin J Prev Med. 2016;50(11):938–42.
Parekh BS, Kalou MB, Alemnji G, Ou CY, Gershy-Damet GM, Nkengasong JN. Scaling up HIV rapid testing in developing countries: comprehensive approach for implementing quality assurance. Am J Clin Pathol. 2010;134(4):573–84.
Acknowledgements
The authors thank the “Sunshine” NGOs in Shenyang for their help with recruitment of the participants and the Shenyang CDC for profound cooperation in this study. We also thank all of the MSM participants. The study was supported by the Mega-Projects of national science research for the 12th Five-Year Plan (2012ZX10001-006). Thanks to Dr. Ewen MacDonald from University of Eastern Finland for proofreading this manuscript.
Funding
This study was funded by the Mega-Project of National Science Research for the 12th-Five-Year Plan (2012ZX10001-006).
Author information
Authors and Affiliations
Contributions
Conceived and designed the experiments: JJX, JZ; performed the study and experiments: JZ, SP, HY, XM, ZXC, QHH; analyzed the data: JZ, JJX; contributed reagents/materials/analysis tools: YJJ, WQG; interpretation of data and study findings: JZ, JJX, WS; drafted the study report: JZ, JJX, NW, HS. All authors reviewed and approved the final report.
Corresponding authors
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Zhang, J., Xu, Jj., Song, W. et al. HIV Incidence and Care Linkage among MSM First-Time-Testers in Shenyang, China 2012–2014. AIDS Behav 22, 711–721 (2018). https://doi.org/10.1007/s10461-017-1840-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10461-017-1840-4