Abstract
Utilizing interviews with students and a key administrator, analyses of academic schedules, and observations of courses, labs, and small groups, this study examines if and how elements of the explicit preclinical curriculum may have deleterious effects on medical students’ humanitarian attributes, namely empathy. Findings from this case-study of a medical school in the United States suggest that the lack of frequent formal testing in the psycho-social aspects of patient care during the preclinical years, as well as a general reduction in curriculum hours devoted to teaching the social aspects of medicine, may serve as mechanisms behind the diminution of medical students’ levels of empathy and other positive attributes as found by previous research. Following the basic tenets of the Testing Effect and the assumption that assessment drives learning, it is argued that a feasible way to maintain and potentially cultivate these traits among medical students, without saturating an overwhelmed medical curriculum, would be to install periodic, formally graded exams into preclinical curriculums that evaluate empathy and the psycho-social aspects of care.

Similar content being viewed by others
Notes
County SOM, County University, and all names presented in this work are pseudonyms.
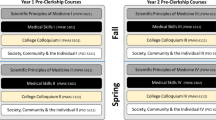
The alterations and new emphases of the curriculum will be explained in the pages to follow.
The argument presented in this paper does not state that current curriculum of County SOM, or other medical education institutions, is wrong or lacking, it is understood that clinical knowledge is imperative. Rather, this argument focuses on the structure of assessment of students’ skills as it currently exists in formal medical education.
References
Becker, H., Geer, B., Hughs, E., & Strauss, A. (1961). Boys in white. New Brunswick, NJ: Transaction Books.
Cantillon, P. (2008). Do not adjust your set: The benefits and challenges of test-enhanced learning. Medical Education, 42, 954–956.
Case, G., & Brauner, D. (2010). The doctor as performer: A proposal for change based on a performance studies program. Academic Medicine, 85, 159–163.
Colliver, J., Conlee, M., Verhulst, S., & Dorsey, K. (2010). Reports of the decline of empathy during medical education are greatly exaggerate: A reexamination of the research. Academic Medicine, 85(4), 588–593.
Colliver, J., & Swartz, M. (1997). Assessing clinical performance with standardized patients. JAMA, 278(9), 790–791.
Conrad, P. (1988). Learning to doctor: Reflections on recent accounts of the medical school years. Journal of Health and Social Behavior, 29, 323–332.
Coombs, R. (1978). Mastering medicine. New York, NY: The Free Press.
Course Bulletins are not included in the reference section to protect the anonymity of the medical school studied.
DasGupta, S., & Charon, R. (2004). Personal illness narratives: Using reflective writing to teach empathy. Academic Medicine, 79(4), 351–356.
Davis, M. (1996). Empathy: A social psychological approach. New York, NY: Westview Press, Inc.
Diseker, R., & Michielutte, R. (1981). An analysis of empathy in medical students before and following clinical experience. Journal of Medical Education, 56, 1004–1010.
Epstein, R., & Hundert, E. (2002). Defining and assessing professional competence. JAMA, 287(2), 226–235.
Frederiksen, N. (1984). The real test bias: Influences of testing on teaching and learning. American Psychologist, 39(3), 193–202.
Glick, S. (1993). The empathic physician: Nature and nuture. In H. Spiro, M. G. McCrea-Curnen, E. Peschel, & D. St. James (Eds.), Empathy and the practice of medicine (pp. 85–102). New Haven, CT: Yale University Press.
Hafferty, F. (1988). Cadaver stories and the emotional socialization of medical students. Journal of Health and Social Behavior, 29, 344–356.
Hafferty, F., & Franks, R. (1994). The hidden curriculum, ethics, teaching, and the structure of medical education. Academic Medicine, 69(11), 861–871.
Haidet, P., Dains, J., Paterniti, D., Chang, T., Tsang, E., & Rogers, J. (2001). Medical students’ attitudes toward patient-centered care and standardized patients’ perceptions of humanism: A link between attitudes and outcomes. Academic Medicine, 76(10), S42–S44.
Halpern, J. (2003). What is clinical empathy? Journal of General Internal Medicine, 18, 670–674.
Hanna, M., & Fins, J. (2006). Power and communication: Why simulation training ought to be complemented by experiential and humanistic learning. Academic Medicine, 81(3), 265–270.
Hochberg, M., Kalet, A., Zabar, S., Kachur, E., Gillespie, C., & Berman, (2010). Can professionalism be taught? Encouraging evidence. American Journal of Surgery, 199(1), 86–93.
Hojat, M., Gonnella, J., Mangione, S., Nasca, T., & Magee, M. (2003). Physician empathy in medical education and practice: Experience with the jefferson scale of physician empathy. Seminars in Integrative Medicine, 1(1), 25–41.
Hojat, M., Mangione, S., Nasca, T., Rattner, S., Erdmann, J., Gonnella, J., et al. (2004). An empirical study of decline in empathy in medical students. Medical Education, 38, 934–941.
Hojat, M., Vergare, M., Maxwell, K., Brainard, G., Herrine, S., Isenberg, G., et al. (2009). The devil is in the third year: A longitudinal study of erosion of empathy in medical school. Academic Medicine, 84(9), 1182–1191.
Hornblow, A., Kidson, M., & Ironsides, W. (1988). Empathic process: Perception by medical students of patients’ anxiety and depression. Medical Education, 22, 15–18.
Horowitz, C., Suchman, A., Branch, W., & Frankel, R. (2003). What do doctors find meaningful about their work? Annals of Internal Medicine, 138(9), 772–776.
Klass, P. (1987). A not entirely benign procedure. New York, NY: G. P. Putnam’s Sons.
Konner, M. (1987). Becoming a doctor. New York, NY: Penguin Books.
Kramer, D., Ber, R., & Moore, M. (1989). Increasing empathy among medical students. Medical Education, 23, 168–173.
Kumagai, A. (2008). A conceptual framework for the use of illness narratives in medical education. Academic Medicine, 83(7), 653–658.
Kvale, S., & Brickman, S. (2009). Interviews (2nd ed.). Thousand Oaks, CA: Sage Publications.
Lancaster, T., Hart, R., & Gardner, S. (2002). Literature and medicine: Evaluating a special study module using the nominal group technique. Medical Education, 36, 1071–1076.
Larsen, D., Butler, A., & Roediger, H., I. I. I. (2008). Test-enhanced learning in medical education. Medical Education, 42, 959–966.
Larson, E., & Yao, H. (2005). Clinical empathy as emotional labor in the patient-physician relationship. JAMA, 293(9), 1100–1106.
Le, T., Bhushan, V., Rao, D., & Grimm, L. (2008). First aid for the USMLE Step 1 2008. New York, NY: McGraw Hill.
LeBaron, C. (1981). Gentle vengeance. New York, NY: Richard Marek Publishers.
Lofland, J., Snow, D., Anderson, L., & Lofland, L. (2006). Analyzing social settings: A guide to qualitative observation and analysis. Belmont, CA: Thomson-Wadsworth.
Marcus, E. (1999). Empathy, humanism, and the professionalization process of medical education. Academic Medicine, 74(11), 1211–1215.
McDaniel, M., Anderson, J., Derbish, M., & Morrisette, N. (2007). Testing the testing effect in the classroom. European Journal of Cognitive Psychology, 19(4/5), 494–513.
Mehrabian, A. (2000). Manual for the Balanced Emotional Empathy Scale (BEES). Available from Albert Mehrabian, 1130 Alta Mesa Road, Monterey, CA 93940.
Merton, R. (1957). Some preliminaries to a sociology of medical education. In R. K. Merton, G. G. Reader, & P. L. Kendall (Eds.), The student-physician: Introductory studies in the sociology of medical education (pp. 3–79). Cambridge, MA: Harvard University Press.
Michalec, B. (2010). An assessment of medical school stressors on preclinical students’ levels of clinical empathy. Current Psychology, 29(3), 210–221.
Plano-Clark, V., & Creswell, J. (2008). The mixed methods reader. Los Angeles, CA: Sage Publications.
Robbins, J., Bertakis, K., Helms, J., Azari, R., Callahan, E., & Creten, D. (1993). The influence of physician practice behaviors on patient satisfaction. Family Medicine, 25(1), 17–20.
Roberts, W., & Strayer, J. (1996). Empathy, emotional expressiveness, and prosocial behavior. Child Development, 67, 449–470.
Saunders, P., Tractenberg, R., Chateriji, R., Amri, H., Harazduk, N., Gordon, J., et al. (2007). Promoting self-awareness and reflection through an experiential Mind-Body Skills course for first year medical students. Medical Teacher, 29, 778–784.
Spiro, H. (1993). What is empathy and can it be taught? In H. Spiro, M. G. McCrea-Curnen, E. Peschel, & D. St. James (Eds.), Empathy and the practice of medicine (pp. 7–14). New Haven, CT: Yale University Press.
Szmuilowicz, E., el-Jawahri, A., Chiapetta, L., Kamdar, M., & Block, S. (2010). Improving residents’ end-of-life communication skills with a short retreat: A randomized controlled trial. Journal of Palliative Medicine, 13(4), 439–452.
Teherani, A., Hauer, K., & O’Sullivan, P. (2008). Can simulations measure empathy? Considerations on how to assess behavioral empathy via simulations. Patient Education and Counseling, 71, 148–152.
Wear, D. (1998). On white coats and professional development: The formal and the hidden curricula. Annals of Internal Medicine, 129, 734–737.
Wear, D., & Castellani, B. (2000). The development of professionalism: Curriculum matters. Academic Medicine, 75(6), 602–611.
Wear, D., & Varley, J. (2008). Rituals of verification: The role of simulation in developing and evaluating empathic communication. Patient Education and Counseling, 71, 153–156.
Whitemore, P., Burstein, A., Loucks, S., & Schoenfeld, L. (1985). A longitudinal study of personality changes in medical students. Journal of Medical Education, 60, 404–405.
Wolf, T., Balson, P., Faucett, J., & Randall, H. (1989). A retrospective study of attitude change during medical education. Medical Education, 23, 19–23.
Wood, T. (2009). Assessment not only drives learning, it may also help learning. Medical Education, 43, 5–6.
Zillman, D., & Cantor, J. (1977). Affective responses to the emotions of protagonist. Journal of Experimental Social Psychology, 13, 155–165.
Zraick, R., Allen, R., & Johnson, S. (2003). The use of standardized patients to teach and test interpersonal and communication skills with students in speech-language pathology. Advances in Health Sciences Education, 8, 237–248.
Acknowledgments
The author would like to thank all students, faculty, and staff at County SOM for their participation in this study.
Conflict of interests
The author declared no conflicts of interest with respect to the authorship and/or publication of this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Michalec, B. Learning to cure, but learning to care?. Adv in Health Sci Educ 16, 109–130 (2011). https://doi.org/10.1007/s10459-010-9249-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10459-010-9249-0