Abstract
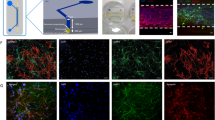
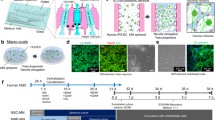
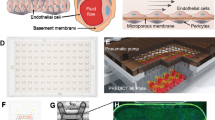
Angiogenesis plays a key role in the pathology of diseases such as cancer, diabetic retinopathy, and age-related macular degeneration. Understanding the driving forces of endothelial cell migration and organization, as well as the time frame of these processes, can elucidate mechanisms of action of important pathological pathways. Herein, we have developed an organ-specific microfluidic platform recapitulating the in vivo angiogenic microenvironment by co-culturing mouse primary brain endothelial cells with brain pericytes in a three-dimensional (3D) collagen scaffold. As a proof of concept, we show that this model can be used for studying the angiogenic process and further comparing the angiogenic properties between two different common inbred mouse strains, C57BL/6J and 129S1/SvlmJ. We further show that the newly discovered angiogenesis-regulating gene Padi2 promotes angiogenesis through Dll4/Notch1 signaling by an on-chip mechanistic study. Analysis of the interplay between primary endothelial cells and pericytes in a 3D microfluidic environment assists in the elucidation of the angiogenic response.







Similar content being viewed by others
Data availability
All data generated or analyzed during this study are included in this article (and its supplementary information files), and are available from the corresponding author upon request.
References
Craig LE, Spelman JP, Strandberg JD, Zink MC (1998) Endothelial cells from diverse tissues exhibit differences in growth and morphology. Microvasc Res 55(1):65–76. https://doi.org/10.1006/mvre.1997.2045
Blanco R, Gerhardt H (2013) VEGF and Notch in tip and stalk cell selection. Cold Spring Harbor Perspect Med 3(1):a006569. https://doi.org/10.1101/cshperspect.a006569
Vossenaar ER, Zendman AJ, van Venrooij WJ, Pruijn GJ (2003) PAD, a growing family of citrullinating enzymes: genes, features and involvement in disease. BioEssays 25(11):1106–1118. https://doi.org/10.1002/bies.10357
Ferrara N, Gerber HP, LeCouter J (2003) The biology of VEGF and its receptors. Nat Med 9(6):669–676. https://doi.org/10.1038/nm0603-669
Gerhardt H, Golding M, Fruttiger M, Ruhrberg C, Lundkvist A, Abramsson A, Jeltsch M, Mitchell C, Alitalo K, Shima D, Betsholtz C (2003) VEGF guides angiogenic sprouting utilizing endothelial tip cell filopodia. J Cell Biol 161(6):1163–1177. https://doi.org/10.1083/jcb.200302047
Lobov I, Mikhailova N (2018) The role of Dll4/Notch signaling in normal and pathological ocular angiogenesis: Dll4 controls blood vessel sprouting and vessel remodeling in normal and pathological conditions. J Ophthalmol 2018:3565292. https://doi.org/10.1155/2018/3565292
Kopan R, Ilagan MX (2009) The canonical Notch signaling pathway: unfolding the activation mechanism. Cell 137(2):216–233. https://doi.org/10.1016/j.cell.2009.03.045
Benedito R, Roca C, Sorensen I, Adams S, Gossler A, Fruttiger M, Adams RH (2009) The notch ligands Dll4 and Jagged1 have opposing effects on angiogenesis. Cell 137(6):1124–1135. https://doi.org/10.1016/j.cell.2009.03.025
Ziółkowska K, Kwapiszewski R, Brzózka Z (2011) Microfluidic devices as tools for mimicking the in vivo environment. New J Chem 35(5):979–990. https://doi.org/10.1039/C0NJ00709A
Bajaj P, Schweller RM, Khademhosseini A, West JL, Bashir R (2014) 3D biofabrication strategies for tissue engineering and regenerative medicine. Annu Rev Biomed Eng 16:247–276. https://doi.org/10.1146/annurev-bioeng-071813-105155
Bai J, Wang C (2020) Organoids and microphysiological systems: new tools for ophthalmic drug discovery. Front Pharmacol. https://doi.org/10.3389/fphar.2020.00407
Avendano A, Cortes-Medina M, Song JW (2019) Application of 3-D microfluidic models for studying mass transport properties of the tumor interstitial matrix. Front Bioeng Biotechnol 7:6. https://doi.org/10.3389/fbioe.2019.00006
Motherwell J, Murfee WL (2018) Modelling microvascular pathology. Nat Biomed Eng 2(6):349–350. https://doi.org/10.1038/s41551-018-0251-9
van Duinen V, Trietsch SJ, Joore J, Vulto P, Hankemeier T (2015) Microfluidic 3D cell culture: from tools to tissue models. Curr Opin Biotechnol 35:118–126. https://doi.org/10.1016/j.copbio.2015.05.002
Kamm RD, Bashir R, Arora N, Dar RD, Gillette MU, Griffith LG, Kemp ML, Kinlaw K, Levin M, Martin AC, McDevitt TC, Nerem RM, Powers MJ, Saif TA, Sharpe J, Takayama S, Takeuchi S, Weiss R, Ye K, Yevick HG, Zaman MH (2018) Perspective: the promise of multi-cellular engineered living systems. APL Bioeng 2(4):040901. https://doi.org/10.1063/1.5038337
Andrejecsk JW, Hughes CCW (2018) Engineering perfused microvascular networks into microphysiological systems platforms. Curr Opin Biomed Eng 5:74–81. https://doi.org/10.1016/j.cobme.2018.02.002
Haase K, Kamm RD (2017) Advances in on-chip vascularization. Regen Med 12(3):285–302. https://doi.org/10.2217/rme-2016-0152
Yeon JH, Ryu HR, Chung M, Hu QP, Jeon NL (2012) In vitro formation and characterization of a perfusable three-dimensional tubular capillary network in microfluidic devices. Lab Chip 12(16):2815–2822. https://doi.org/10.1039/C2LC40131B
van Duinen V, Zhu D, Ramakers C, van Zonneveld AJ, Vulto P, Hankemeier T (2019) Perfused 3D angiogenic sprouting in a high-throughput in vitro platform. Angiogenesis 22(1):157–165. https://doi.org/10.1007/s10456-018-9647-0
Zeinali S, Bichsel CA, Hobi N, Funke M, Marti TM, Schmid RA, Guenat OT, Geiser T (2018) Human microvasculature-on-a chip: anti-neovasculogenic effect of nintedanib in vitro. Angiogenesis 21(4):861–871. https://doi.org/10.1007/s10456-018-9631-8
Bai J, Adriani G, Dang TM, Tu TY, Penny HX, Wong SC, Kamm RD, Thiery JP (2015) Contact-dependent carcinoma aggregate dispersion by M2a macrophages via ICAM-1 and beta2 integrin interactions. Oncotarget 6(28):25295–25307. https://doi.org/10.18632/oncotarget.4716
Bai J, Tu TY, Kim C, Thiery JP, Kamm RD (2015) Identification of drugs as single agents or in combination to prevent carcinoma dissemination in a microfluidic 3D environment. Oncotarget 6(34):36603–36614. https://doi.org/10.18632/oncotarget.5464
Aref AR, Huang RY, Yu W, Chua KN, Sun W, Tu TY, Bai J, Sim WJ, Zervantonakis IK, Thiery JP, Kamm RD (2013) Screening therapeutic EMT blocking agents in a three-dimensional microenvironment. Integr Biol 5(2):381–389. https://doi.org/10.1039/c2ib20209c
Horbach S, Halffman W (2017) The ghosts of HeLa: How cell line misidentification contaminates the scientific literature. PLoS ONE 12(10):e0186281. https://doi.org/10.1371/journal.pone.0186281
Perez RA, Mestres G (2016) Role of pore size and morphology in musculo-skeletal tissue regeneration. Mater Sci Eng C 61:922–939. https://doi.org/10.1016/j.msec.2015.12.087
Rohan RM, Fernandez A, Udagawa T, Yuan J, D'Amato RJ (2000) Genetic heterogeneity of angiogenesis in mice. FASEB J 14(7):871–876
Khajavi M, Zhou Y, Birsner AE, Bazinet L, Rosa Di Sant A, Schiffer AJ, Rogers MS, Krishnaji ST, Hu B, Nguyen V, Zon L, D'Amato RJ (2017) Identification of Padi2 as a novel angiogenesis-regulating gene by genome association studies in mice. PLoS Genet 13(6):e1006848. https://doi.org/10.1371/journal.pgen.1006848
McElwee JL, Mohanan S, Griffith OL, Breuer HC, Anguish LJ, Cherrington BD, Palmer AM, Howe LR, Subramanian V, Causey CP, Thompson PR, Gray JW, Coonrod SA (2012) Identification of PADI2 as a potential breast cancer biomarker and therapeutic target. BMC Cancer 12:500. https://doi.org/10.1186/1471-2407-12-500
Koch MW, Metz LM, Kovalchuk O (2013) Epigenetic changes in patients with multiple sclerosis. Nat Rev Neurol 9(1):35–43. https://doi.org/10.1038/nrneurol.2012.226
Tigges U, Welser-Alves JV, Boroujerdi A, Milner R (2012) A novel and simple method for culturing pericytes from mouse brain. Microvasc Res 84(1):74–80. https://doi.org/10.1016/j.mvr.2012.03.008
Perriere N, Demeuse P, Garcia E, Regina A, Debray M, Andreux JP, Couvreur P, Scherrmann JM, Temsamani J, Couraud PO, Deli MA, Roux F (2005) Puromycin-based purification of rat brain capillary endothelial cell cultures. Effect on the expression of blood-brain barrier-specific properties. J Neurochem 93(2):279–289. https://doi.org/10.1111/j.1471-4159.2004.03020.x
Song JW, Munn LL (2011) Fluid forces control endothelial sprouting. Proc Natl Acad Sci USA 108(37):15342–15347. https://doi.org/10.1073/pnas.1105316108
Chen MB, Hajal C, Benjamin DC, Yu C, Azizgolshani H, Hynes RO, Kamm RD (2018) Inflamed neutrophils sequestered at entrapped tumor cells via chemotactic confinement promote tumor cell extravasation. Proc Natl Acad Sci USA 115(27):7022–7027. https://doi.org/10.1073/pnas.1715932115
Ludovica V. AS, Zdenko H., Rabih M. (2017) Mechanisms of histone modifications. In: Handbook of epigenetics (2nd edn). Academic Press, pp 25–46. https://doi.org/10.1016/B978-0-12-805388-1.00003-1
Thurston G, Kitajewski J (2008) VEGF and Delta-Notch: interacting signalling pathways in tumour angiogenesis. Br J Cancer 99(8):1204–1209. https://doi.org/10.1038/sj.bjc.6604484
Zhang X, Bolt M, Guertin MJ, Chen W, Zhang S, Cherrington BD, Slade DJ, Dreyton CJ, Subramanian V, Bicker KL, Thompson PR, Mancini MA, Lis JT, Coonrod SA (2012) Peptidylarginine deiminase 2-catalyzed histone H3 arginine 26 citrullination facilitates estrogen receptor alpha target gene activation. Proc Natl Acad Sci USA 109(33):13331–13336. https://doi.org/10.1073/pnas.1203280109
Falcao AM, Meijer M, Scaglione A, Rinwa P, Agirre E, Liang J, Larsen SC, Heskol A, Frawley R, Klingener M, Varas-Godoy M, Raposo A, Ernfors P, Castro DS, Nielsen ML, Casaccia P, Castelo-Branco G (2019) PAD2-mediated citrullination contributes to efficient oligodendrocyte differentiation and myelination. Cell Rep 27(4):1090–1102. https://doi.org/10.1016/j.celrep.2019.03.108
Ostergaard L, Engedal TS, Moreton F, Hansen MB, Wardlaw JM, Dalkara T, Markus HS, Muir KW (2016) Cerebral small vessel disease: capillary pathways to stroke and cognitive decline. J Cereb Blood Flow Metab 36(2):302–325. https://doi.org/10.1177/0271678X15606723
Bodnar RJ, Rodgers ME, Chen WC, Wells A (2013) Pericyte regulation of vascular remodeling through the CXC receptor 3. Arterioscler Thromb Vasc Biol 33(12):2818–2829. https://doi.org/10.1161/ATVBAHA.113.302012
Bergers G, Song S (2005) The role of pericytes in blood-vessel formation and maintenance. Neuro Oncol 7(4):452–464. https://doi.org/10.1215/S1152851705000232
Darrah E, Rosen A, Giles JT, Andrade F (2012) Peptidylarginine deiminase 2, 3 and 4 have distinct specificities against cellular substrates: novel insights into autoantigen selection in rheumatoid arthritis. Ann Rheum Dis 71(1):92–98. https://doi.org/10.1136/ard.2011.151712
Wang L, Song G, Zhang X, Feng T, Pan J, Chen W, Yang M, Bai X, Pang Y, Yu J, Han J, Han B (2017) PADI2-mediated citrullination promotes prostate cancer progression. Can Res 77(21):5755–5768. https://doi.org/10.1158/0008-5472.CAN-17-0150
Moscarello MA, Mastronardi FG, Wood DD (2007) The role of citrullinated proteins suggests a novel mechanism in the pathogenesis of multiple sclerosis. Neurochem Res 32(2):251–256. https://doi.org/10.1007/s11064-006-9144-5
Guarani V, Deflorian G, Franco CA, Kruger M, Phng LK, Bentley K, Toussaint L, Dequiedt F, Mostoslavsky R, Schmidt MHH, Zimmermann B, Brandes RP, Mione M, Westphal CH, Braun T, Zeiher AM, Gerhardt H, Dimmeler S, Potente M (2011) Acetylation-dependent regulation of endothelial Notch signalling by the SIRT1 deacetylase. Nature 473(7346):234–238. https://doi.org/10.1038/nature09917
Lobov IB, Renard RA, Papadopoulos N, Gale NW, Thurston G, Yancopoulos GD, Wiegand SJ (2007) Delta-like ligand 4 (Dll4) is induced by VEGF as a negative regulator of angiogenic sprouting. Proc Natl Acad Sci USA 104(9):3219–3224. https://doi.org/10.1073/pnas.0611206104
Bai J, Fu H, Bazinet L, Birsner AE, D'Amato RJ (2020) A method for developing novel 3D cornea-on-a-chip using primary murine corneal epithelial and endothelial cells. Front Pharmacol. https://doi.org/10.3389/fphar.2020.00453
Funding
This study was supported, in part, by the NIH National Eye Institute. Award Number R01EY012726-12 (to RJD).
Author information
Authors and Affiliations
Contributions
JB, RJD, MK, HJF, STK, and AEB contributed to the design and implementation of the research, JB, LFS, and LB performed the experiments, and JB, RJD, RDK, and MK contributed to the interpretation of the results and the preparation of the manuscript. All authors provided critical feedback and helped shape the research, analysis, and manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The author(s) declare(s) that there is no conflict of interest regarding the publication of this article.
Ethics approval
All animal studies were conducted in compliance with the protocols approved by the Institutional Animal Care and Use Committee of Boston Children’s Hospital (approval number 15-08-2998R for mouse experiments).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Bai, J., Khajavi, M., Sui, L. et al. Angiogenic responses in a 3D micro-engineered environment of primary endothelial cells and pericytes. Angiogenesis 24, 111–127 (2021). https://doi.org/10.1007/s10456-020-09746-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10456-020-09746-6