Abstract
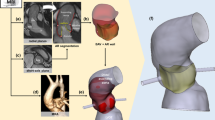
Bicuspid aortic valve (BAV) is the most common congenital heart disease. Calcific aortic valve disease (CAVD) accounts for the majority of aortic stenosis (AS) cases. Half of the patients diagnosed with AS have a BAV, which has an accelerated progression rate. This study aims to develop a computational modeling approach of both the calcification progression in BAV, and its biomechanical response incorporating fluid-structure interaction (FSI) simulations during the disease progression. The calcification is patient-specifically reconstructed from Micro-CT images of excised calcified BAV leaflets, and processed with a novel reverse calcification technique that predicts prior states of CAVD using a density-based criterion, resulting in a multilayered calcified structure. Four progressive multilayered calcified BAV models were generated: healthy, mild, moderate, and severe, and were modeled by FSI simulations during the full cardiac cycle. A valve apparatus model, composed of the excised calcified BAV leaflets, was tested in an in-vitro pulse duplicator, to validate the severe model. The healthy model was validated against echocardiography scans. Progressive AS was characterized by higher systolic jet flow velocities (2.08, 2.3, 3.37, and 3.85 m s−1), which induced intense vortices surrounding the jet, coupled with irregular recirculation backflow patterns that elevated viscous shear stresses on the leaflets. This study shed light on the fluid-structure mechanism that drives CAVD progression in BAV patients.








Similar content being viewed by others
References
Aksenov, A., A. Dyadkin, and V. Pokhilko. Overcoming of barrier between CAD and CFD by modified finite volume method. Asme-Publications-Pvp. 377:79–83, 1998.
Balachandran, K., P. Sucosky, H. Jo, and A. P. Yoganathan. Elevated cyclic stretch alters matrix remodeling in aortic valve cusps: implications for degenerative aortic valve disease. Am. J. Physiol. Circ. Physiol. 296:H756–H764, 2009.
Beppu, S., S. Suzuki, H. Matsuda, F. Ohmori, S. Nagata, and K. Miyatake. Rapidity of progression of aortic stenosis in patients with congenital bicuspid aortic valves. Am. J. Cardiol. 71:322–327, 1993.
Bouchareb, R., M. C. Boulanger, D. Fournier, P. Pibarot, Y. Messaddeq, and P. Mathieu. Mechanical strain induces the production of spheroid mineralized microparticles in the aortic valve through a RhoA/ROCK-dependent mechanism. J. Mol. Cell. Cardiol. 67:49–59, 2014.
Braverman, A. C., H. Güven, M. A. Beardslee, M. Makan, A. M. Kates, and M. R. Moon. The bicuspid aortic valve. Curr. Probl. Cardiol. 30:470–522, 2005.
Cao, K., S. K. Atkins, A. McNally, J. Liu, and P. Sucosky. Simulations of morphotype-dependent hemodynamics in non-dilated bicuspid aortic valve aortas. J. Biomech. 2016. https://doi.org/10.1016/j.jbiomech.2016.11.024.
Cao, K., and P. Sucosky. Computational comparison of regional stress and deformation characteristics in tricuspid and bicuspid aortic valve leaflets. Int. J. Numer. Method. Biomed. Eng. 33:1–21, 2017.
Ebenstein, D. M., D. Coughlin, J. Chapman, C. Li, and L. A. Pruitt. Nanomechanical properties of calcification, fibrous tissue, and hematoma from atherosclerotic plaques. J. Biomed. Mater. Res. A 91:1028–1037, 2009.
Emendi, M., F. Sturla, R. P. Ghosh, M. Bianchi, F. Piatti, F. R. Pluchinotta, D. Giese, M. Lombardi, A. Redaelli, and D. Bluestein. Patient-specific bicuspid aortic valve biomechanics: a magnetic resonance imaging integrated fluid-structure interaction approach. Ann. Biomed. Eng. 2020. https://doi.org/10.1007/s10439-020-02571-4.
Fisher, C. I., J. Chen, and W. D. Merryman. Calcific nodule morphogenesis by heart valve interstitial cells is strain dependent. Biomech. Model. Mechanobiol. 12:5–17, 2013.
Freeman, R. V., and C. M. Otto. Spectrum of calcific aortic valve disease: pathogenesis, disease progression, and treatment strategies. Circulation. 111:3316–3326, 2005.
Gundiah, N., K. Kam, P. B. Matthews, J. Guccione, H. A. Dwyer, D. Saloner, T. a M. Chuter, T. S. Guy, M. B. Ratcliffe, and E. E. Tseng. Asymmetric mechanical properties of porcine aortic sinuses. Ann. Thorac. Surg. 85:1631–1638, 2008.
Haj-Ali, R., G. Marom, S. Ben Zekry, M. Rosenfeld, and E. Raanani. A general three-dimensional parametric geometry of the native aortic valve and root for biomechanical modeling. J. Biomech. 45:2392–7, 2012.
Halevi, R., A. Hamdan, G. Marom, K. Lavon, S. Ben-Zekry, E. Raanani, D. Bluestein, and R. Haj-Ali. Fluid–structure interaction modeling of calcific aortic valve disease using patient-specific three-dimensional calcification scans. Med. Biol. Eng. Comput. 54:1683–1694, 2016.
Halevi, R., A. Hamdan, G. Marom, M. Mega, E. Raanani, and R. Haj-Ali. Progressive aortic valve calcification: three-dimensional visualization and biomechanical analysis. J. Biomech. 48:489–497, 2015.
Harloff, A., A. Nussbaumer, S. Bauer, A. F. Stalder, A. Frydrychowicz, C. Weiller, J. Hennig, and M. Markl. In vivo assessment of wall shear stress in the atherosclerotic aorta using flow-sensitive 4D MRI. Magn. Reson. Med. 63:1529–1536, 2010.
Hart, J. De, F. P. T. Baaijens, G. W. M. Peters, and P. J. G. Schreurs. A computational fluid-structure interaction analysis of a fiber-reinforced stentless aortic valve. J. Biomech. 36:699–712, 2003.
Katayama, S., N. Umetani, T. Hisada, and S. Sugiura. Bicuspid aortic valves undergo excessive strain during opening: a simulation study. J. Thorac. Cardiovasc. Surg. 145:1570–1576, 2013.
Kazik, H. B., H. S. Kandail, J. F. LaDisa Jr, and J. Lincoln. Molecular and mechanical mechanisms of calcification pathology induced by bicuspid aortic valve abnormalities. Front. Cardiovasc. Med. 8:1–13, 2021.
Kebed, K., D. Sun, K. Addetia, V. Mor-Avi, N. Markuzon, and R. M. Lang. Measurement errors in serial echocardiographic assessments of aortic valve stenosis severity. Int. J. Cardiovasc. Imaging. 36:471–479, 2020.
Lavon, K., G. Marom, M. Bianchi, R. Halevi, A. Hamdan, A. Morany, E. Raanani, D. Bluestein, and R. Haj-Ali. Biomechanical modeling of transcatheter aortic valve replacement in a stenotic bicuspid aortic valve: deployments and paravalvular leakage. Med. Biol. Eng. Comput. 57:2129–2143, 2019.
Lavon, K., R. Halevi, G. Marom, S. Ben Zekry, A. Hamdan, H. J. Schäfers, E. Raanani, and R. Haj-Ali. Fluid-structure interaction models of bicuspid aortic valves: the effects of non-fused cusp angles. J. Biomech. Eng. 140:031010-031010-7, 2018.
Lee, J. H., A. D. Rygg, E. M. Kolahdouz, S. Rossi, S. M. Retta, N. Duraiswamy, L. N. Scotten, B. A. Craven, and B. E. Griffith. Fluid-structure interaction models of bioprosthetic heart valve dynamics in an experimental pulse duplicator. Ann. Biomed. Eng. 48:1475–1490, 2020.
Luraghi, G., F. Migliavacca, C. Chiastra, A. Rossi, B. Reimers, G. G. Stefanini, and J. F. Rodriguez Matas. Does clinical data quality affect fluid-structure interaction simulations of patient-specific stenotic aortic valve models? J. Biomech. 94:202–210, 2019.
Marom, G., R. Haj-Ali, E. Raanani, H.-J. Schäfers, and M. Rosenfeld. A fluid-structure interaction model of the aortic valve with coaptation and compliant aortic root. Med. Biol. Eng. Comput. 50:173–182, 2012.
Marom, G., H.-S. Kim, M. Rosenfeld, E. Raanani, and R. Haj-Ali. Fully coupled fluid-structure interaction model of congenital bicuspid aortic valves: effect of asymmetry on hemodynamics. Med. Biol. Eng. Comput. 51:839–848, 2013.
Martin, C., and W. Sun. Biomechanical characterization of aortic valve tissue in humans and common animal models. J. Biomed. Mater. Res. A 100 A:1591–1599, 2012.
Mega, M., G. Marom, R. Halevi, A. Hamdan, D. Bluestein, and R. Haj-Ali. Imaging analysis of collagen fiber networks in cusps of porcine aortic valves: effect of their local distribution and alignment on valve functionality. Comput. Methods Biomech. Biomed. Engin. 19:1002–1008, 2016.
Merryman, W.D. Mechano-potential etiologies of aortic valve disease. 43:1–14, 2011.
Missirlis, Y. F., and M. Chong. Aortic valve mechanics–Part I: material properties of natural porcine aortic valves. J. Bioeng. 2:287–300, 1978.
Mohler, E. R., F. Gannon, C. Reynolds, R. Zimmerman, M. G. Keane, and F. S. Kaplan. Bone formation and inflammation in cardiac valves. Circulation. 103:1522–1528, 2001.
Nishimura, R., A. C. M. Otto, R. O. Bonow, B. a Carabello, J. P. Erwin, R. a Guyton, P. T. O’Gara, C. E. Ruiz, N. J. Skubas, P. Sorajja, T. M. Sundt, and J. D. Thomas. AHA/ACC guideline for the management of patients with valvular heart disease: executive summary: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. J. Am. Coll. Cardiol. 63(2438–88):2014, 2014.
Oliveira, D. M. C. de, N. Abdullah, N. C. Green, and D. M. Espino. Biomechanical assessment of bicuspid aortic valve phenotypes: a fluid-structure interaction modelling approach. Cardiovasc. Eng. Technol. 11:431–447, 2020.
Sun, L., N. M. Rajamannan, and P. Sucosky. Defining the role of fluid shear stress in the expression of early signaling markers for calcific aortic valve disease. PLoS ONE 8:e84433, 2013.
Wang, S. H., L. P. Lee, and J. S. Lee. A linear relation between the compressibility and density of blood. J. Acoust. Soc. Am. 109:390–396, 2001.
Weinberg, E. J., F. J. Schoen, and M. R. K. Mofrad. A computational model of aging and calcification in the aortic heart valve. PLoS ONE. 4:1–10, 2009.
Weinberg, E. J., P. J. Mack, F. J. Schoen, G. García-Cardeña, and M. R. Kaazempur Mofrad. Hemodynamic environments from opposing sides of human aortic valve leaflets evoke distinct endothelial phenotypes in vitro. Cardiovasc. Eng. 10:5–11, 2010.
Yap, C. H., N. Saikrishnan, and A. P. Yoganathan. Experimental measurement of dynamic fluid shear stress on the ventricular surface of the aortic valve leaflet. Biomech. Model. Mechanobiol. 11:231–244, 2012.
Yoganathan, A. P., K. B. Chandran, and F. Sotiropoulos. Flow in prosthetic heart valves: state-of-the-art and future directions. Ann. Biomed. Eng. 33:1689–1694, 2005.
Zhang, R., and Y. Zhang. An experimental study of pulsatile flow in a compliant aortic root model under varied cardiac outputs. Fluids. 3:71, 2018.
Acknowledgments
This work is supported by NIH-NIBIB BRP U03EB026414 grant. Author RHA acknowledges the support of the Nathan Cummings Chair of Mechanics. Author AM acknowledges the support of the Planning and Budgeting Committee – Israeli Council for Higher Education.
Conflicts of Interest
Authors KL and RH are employees of Edwards Lifesciences Ltd. Author DB has an equity interest in Polynova Cardiovascular Inc. All other authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
Associate Editor Stefan M. Duma oversaw the review of this article.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file1 (MP4 3789 kb)
Rights and permissions
About this article
Cite this article
Lavon, K., Morany, A., Halevi, R. et al. Progressive Calcification in Bicuspid Valves: A Coupled Hemodynamics and Multiscale Structural Computations. Ann Biomed Eng 49, 3310–3322 (2021). https://doi.org/10.1007/s10439-021-02877-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10439-021-02877-x