Abstract
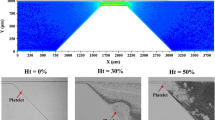
This paper presents dynamic flow experiments with fluorescently labeled platelets to allow for spatial observation of wall attachment in inter-strut spacings, to investigate their relationship to flow patterns. Human blood with fluorescently labeled platelets was circulated through an in vitro system that produced physiologic pulsatile flow in a parallel plate flow chamber that contained three different stent designs that feature completely recirculating flow, partially recirculating flow (intermediate strut spacing), and completely reattached flow. Highly resolved spatial distribution of platelets was obtained by imaging fluorescently labeled platelets between the struts. Platelet deposition was higher in areas where flow is directed towards the wall, and lower in areas where flow is directed away from the wall. Flow detachment and reattachment points exhibited very low platelet deposition. Platelet deposition within intermediate strut spacing continued to increase throughout the experimental period, indicating that the deposition rate had not plateaued unlike other strut spacings. The spatial uniformity and temporal increase in platelet deposition for the intermediate strut spacing confirms and helps explain our previous finding that platelet deposition was highest with this strut spacing. Further experimental investigations will include more complex three-dimensional geometries.
Similar content being viewed by others
References
Berry, J. L., A. Santamarina, J. E. Moore Jr., S. Roychowdhury, and W. D. Routh. Experimental and computational flow evaluation of coronary stents. Ann. Biomed. Eng. 28:386–398, 2000.
Bluestein, D., L. Niu, R. T. Schoephoerster, and M. K.Dewanjee. Fluid mechanics of Arterial Stenosis: Relationship to the development of mural thrombus. Ann. Biomed. Eng. 25:344–356, 1997.
Bluestein, D., L. Niu, R. T. Schoephoerster, and M. K. Dewanjee. Steady flow in an Aneurysm model: Correlation between fluid dynamics and blood platelet deposition. J. Biomech. Engg. 118:280–286, 1996.
Carlier, S. G., L. C. A. van Damme, C. P. Blommerde, J. J. Wentzel, G. van Langehove, S. Verheye, M. M. Kockx, M. W. M. Knaapen, C. Cheng, F. Gijsen, D. J. Duncker, N. Stergiopulos, C. J. Slager, P. W. Serruys, and R. Krams. Augmentation of wall shear stress inhibits neointimal hyperplasia after stent implantation: Inhibition through reduction of inflammation? Circulation 107:2741–2746, 2003.
Cejna, M., S. Thurnher, H. Illiasch, W. Horvath, P. Waldenberger, K. Hornik, and J. Lammer. PTA versus Palmaz stent placement in femoropopliteal artery obstructions: A multicenter prospective randomized study. J. Vasc. Interv. Radiol. Jan 12(1):23–31, 2001.
Crewe, K. H., and I. A. Feuerstein. Platelet adhesion to fibrinogen-coated glass at an abrupt tubular expansion viewed with fluorescent-video microscopy. Biorheology 23(5):443–452, 1986.
David, T., S. Thomas, and P. G. Walker. Platelet deposition in stagnation point flow: An analytical study and computational simulation. Med. Eng. Phys. 23(5):299–312, 2001.
Eigenthaler, M., U. R. Schwarz, B. Schinke, and A. Kobsar. Activated platelets induce migration, proliferation, and gene expression in human vascular endothelial cells. J. Thromb. Haemost. 1(1):12–18, July, 2003, PO164.
Gijsen, J. H., R. M. Oortman, J. J. Wentzel, J. C. H. Schuurbiers, K. Tanabe, M. Degertekin, J. M. Ligthart, A. Thury, P. J. de Feyter, P. W. Serruys, and C. J. Slager. Usefulness of shear stress pattern in predicting neointima distribution in Sirolimus-eluting stents in coronary arteries. Am. J. Cardiol. 92:1325–1328, 2003.
Grenacher, L., T. Saam, A. Geier, S. Muller-Hulsbeck, M. Cejna, G. W. Kauffmann, and G. M. Richter. PTA versus Palmaz stent placement in femoropopliteal artery stenoses: Results of a multicenter prospective randomized study (REFSA). Rofo. 176(9):1302–1310, 2004.
He, Y., N. Duraiswamy, A. O. Frank, and J. E. Moore Jr. Blood flow in stented arteries: A parametric comparison of strut design patterns in 3D. J. Biomech. Eng. 127(4):637–647, 2005.
Hideto, M., M. Sugimoto, T. Mizuno, S. Tsuji, S. Miyata, M. Matsuda, and A. Yoshioka. Distinct and concerted functions of von Willebrand factor and fibrinogen in mural thrombus growth under high shear flow. Blood 100(10):3604–3610, 2002.
Jeong, M. H., W. G. Owen, M. E. Staab, S. S. Srivatsa, G. Sangiorgi, M. Stewart, D. R. Holmes Jr., and R. S. Schwartz. Porcine model of stent thrombosis: Platelets are the primary component of acute stent closure. Cathet. Cardiovasc. Diagn. 38(1):38–43, 1996.
Karino, T., and H. L. Goldsmith. Adhesion of human platelets to collagen on the wall distal to a tubular expansion. Microvasc. Res. 17:238–262, 1979.
Kastrati, A. J., J. Mehilli, J. Dirschinger, J. Pache, K. Ulm, H. Schuhlen, M. Seyfarth, C. Schmitt, R. Blasini, F. J. Neumann, and A. Schomig. Restenosis after coronary placement of various stent types. Am. J. Cardiol. 87:34–39, 2001.
Lau, K. W., A Johan, U. Sigwart, and J. S. Hung. A stent is not just a stent: Stent construction and design do matter in its clinical performance. Singapore Med. J. 45(7):305–312, 2004.
Longest, P. W., and C. Kleinstreuer. Comparison of blood particle deposition models for non-parallel flow domains. J. Biomech. 36(3): 421–430, 2003.
Morice, M. C., P. W. Serruys, J. E. Sousa, J. Fajadet, E. Ban Hayashi, M. Perin, A. Colombo, G. Schuler, P. Barragan, G. Guagliumi, F. Molnar, and R. Falotico. A randomized comparison of a sirolimus-eluting stent with a standard stent for coronary revascularization. N. Engl. J. Med. 349:1315–1323, 2002.
Pache, A., J. Kastrati, H. Mehilli, H. Schuhlen, F. Dotzer, J. Hausleiter, M. Fleckenstein, F. J. Neumann, U. Sattelberger, C. Schmitt, M. Muller, J. Dirschinger, and A. Schomig. Intracoronary stenting and angiographic results: Strut thickness effect on restenosis outcome (ISAR-STEREO-2) trial. J. Am. Coll. Cardiol. 41(8):1283–1288, 2003.
Robaina, S., B. Jayachandran, Y. He, A. Frank, M. Moreno, J. E. Moore Jr., and R. T. Schoephoerster. Platelet adhesion to stimulated stented surfaces. J. Endovascular. Ther. 10:978–986, 2003.
Rogers, C., and E. R. Edelman. Endovascular stent design dictates experimental restenosis and thrombosis. Circulation 91:2995–3001, 1995.
Rolland, P. H., C. Mekkaoui, V. Vidal, J. L. Berry, J. E. Moore Jr., M. Moreno, P. Amabile, and J. M. Bartoli. Compliance matching stent placement in the carotid artery of the swine promotes optimal blood flow and attenuates restenosis. Eur. J. Vasc. Endovasc. Surg. 28:431–438, 2004.
Tominaga, R., H. E. Kambic, H. Emoto, H. Harasaki, C. Sutton, and J. Hollman. Effects of design geometry of intravascular endoprostheses on stenosis rate in normal rabbits. Am. Heart. J. 123:21–28, 1992.
Virmani, R., F. D. Kolodgie, A. Farb, and A. Lafont. Drug eluting stents: Are human and animal studies comparable? Heart 89:133–138, 2003.
Weyrich, A. S., S. M. Prescott, and G. A. Zimmerman. Platelets, endothelial cells, inflammatory chemokines, and restenosis: Complex signaling in the vascular play book. Circulation. 106(12):1433–1435, 2002.
He, Y. Computational analysis of blood flow in a stented chamber under physiologic flow conditions. Master's Thesis, Florida International University 2002.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Duraiswamy, N., Jayachandran, B., Byrne, J. et al. Spatial Distribution of Platelet Deposition in Stented Arterial Models Under Physiologic Flow. Ann Biomed Eng 33, 1767–1777 (2005). https://doi.org/10.1007/s10439-005-7598-2
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/s10439-005-7598-2